Clear Sky Science · en
Association of a five-metabolite and early-symptom profile with Parkinson’s disease and its clinical progression
Why blood tests for Parkinson’s could change everything
Parkinson’s disease is best known for shaking and slowed movement, but by the time these symptoms appear, much of the damage in the brain is already done. This study asks a simple, high-stakes question: can a small blood sample and a few early non-motor symptoms reveal who has Parkinson’s and how far it has progressed? If such a test proves reliable, it could open the door to earlier diagnosis, closer monitoring, and eventually treatments that start before disabling motor problems take hold.
Looking for chemical fingerprints in the blood
The researchers focused on tiny molecules in the blood called metabolites—products of how our cells and gut microbes process food and energy. They recruited 60 people: 20 healthy adults, 20 with intermediate Parkinson’s, and 20 with more advanced disease. From each person, they drew blood and used a highly precise technique to measure the absolute amounts of 144 different metabolites, including amino acids, fatty acid breakdown products, and membrane fats. Unlike many previous studies that only compare relative levels, this approach yields exact concentrations, making it easier for future labs and clinics to reproduce the findings.
Patterns that track disease stages
When the team analyzed all 144 metabolites together, they found that the overall chemical profile of people with Parkinson’s clearly differed from that of healthy controls. Many of these molecules changed systematically as the disease advanced. Some, such as glycine and certain membrane lipids, tended to rise from healthy to intermediate to advanced Parkinson’s. Others, including several gut-derived compounds and fatty acid transport molecules, fell as the disease progressed. Using statistical tools, the researchers narrowed this long list down to the metabolites that differed most strongly even after accounting for age and sex.
A five-molecule blood panel
From this refined set, the authors used a genetic algorithm—a type of computer search method—to find the smallest combination of metabolites that best separated the three groups. They landed on five key molecules: glutamine, butyric acid, indoleacetic acid, a specific phosphatidylcholine (PC aa C40:2), and an acylcarnitine (C12:1). Together, these five markers captured several major biological themes in Parkinson’s: changes in brain-related amino acid handling (glutamine), disruptions in gut microbe products that influence inflammation and the gut barrier (butyric acid and indoleacetic acid), altered cell membrane fats (PC aa C40:2), and impaired energy production in mitochondria (C12:1). In computer models, this five-metabolite panel distinguished healthy people from Parkinson’s patients with high accuracy and also gave useful information about whether a patient was in an intermediate or more advanced stage.
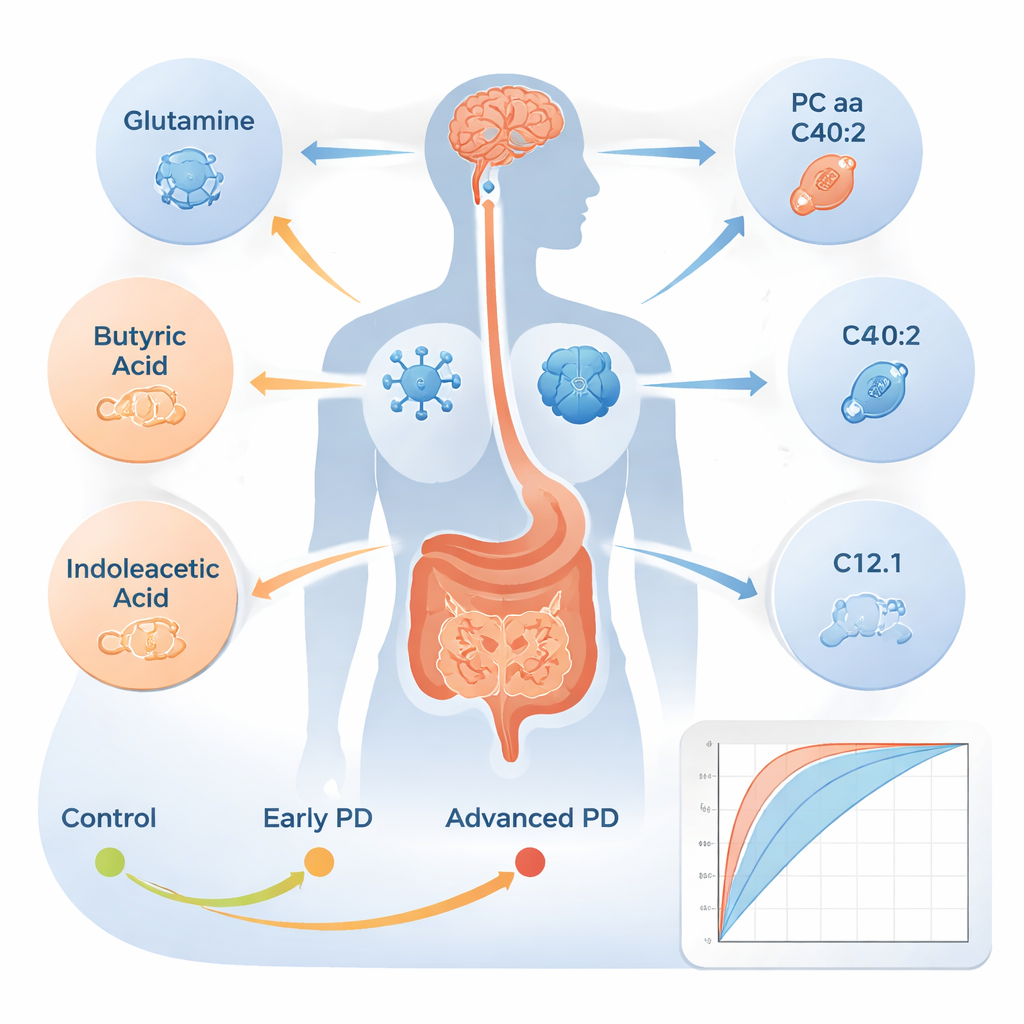
Adding early non-motor symptoms to the mix
Parkinson’s does not start with tremors alone. Many patients first develop problems such as drooling, a sleep disorder in which they act out dreams (REM sleep behavior disorder), and depression. These non-motor features match early spread of the disease along the body’s nerve pathways. The researchers built additional models that combined the five blood metabolites with these three symptoms plus age. This combined profile did an even better job at telling healthy people from those with early Parkinson’s and separating intermediate from advanced disease. In other words, a brief clinical interview and a small plasma sample together provided a rich snapshot of how far Parkinson’s had progressed in each person.
What this could mean for patients
To a layperson, the key message is that Parkinson’s disease leaves a measurable trail in the blood long before and alongside obvious motor symptoms. This study identifies a compact set of five blood chemicals, plus a trio of early symptoms, that together reflect changes in the gut, the brain’s energy systems, and nerve cell membranes as the disease advances. The work is still exploratory and involved only 60 people, so much larger, independent studies are needed before any routine test can be offered in clinics or for screening people without symptoms. Yet it provides a promising blueprint: a single blood draw and short interview might one day help doctors detect Parkinson’s earlier, stage it more precisely, and track how it responds to future disease-slowing treatments.
Citation: Oropeza Valdez, J.J., Elizalde-Díaz, J.P., Antonio, O.R. et al. Association of a five-metabolite and early-symptom profile with Parkinson’s disease and its clinical progression. Sci Rep 16, 5885 (2026). https://doi.org/10.1038/s41598-026-36756-z
Keywords: Parkinson’s disease, metabolomics, biomarkers, gut-brain axis, early diagnosis