Clear Sky Science · en
Comparison of clinical and inflammatory markers for dry eye disease following phacoemulsification and manual small incision cataract surgery (MSICS)
Why cataract surgery can leave eyes feeling dry
Cataract surgery is one of the most common and successful operations worldwide, restoring clear sight to millions each year. Yet many patients are surprised to find that, instead of instant comfort, their eyes feel gritty, watery, or sore afterward. This study explores why that happens, comparing two popular cataract techniques to see how each one affects the eye’s delicate surface and tear film in the weeks after surgery.
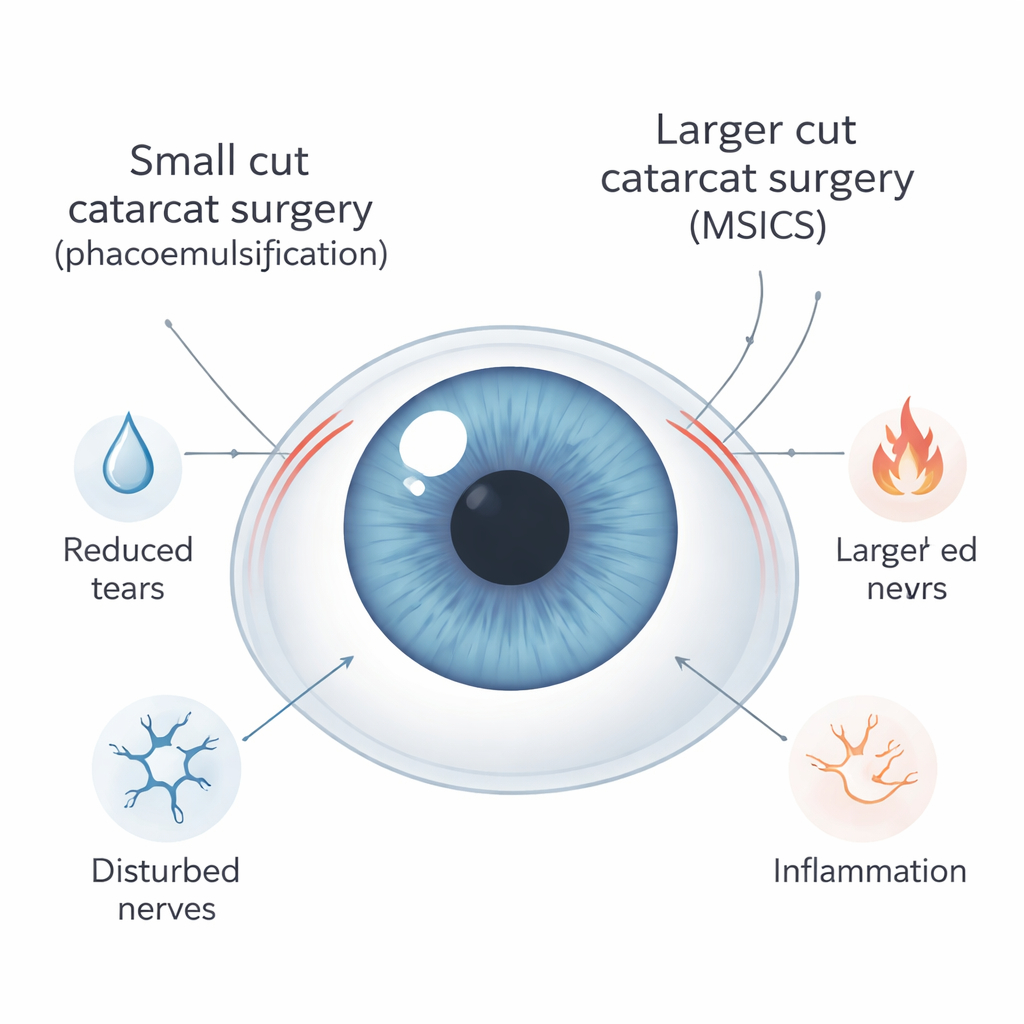
Two ways to remove a cloudy lens
The researchers focused on people over 40 with simple age-related cataracts, none of whom had dry eye disease before surgery. Half were treated with standard phacoemulsification, which uses ultrasound through a very small cut in the clear front window of the eye. The other half had manual small incision cataract surgery (MSICS), a technique widely used in busy or low-resource hospitals that relies on a larger cut but simpler instruments. In both groups, eye comfort and tear function were checked before surgery and then several times afterward, up to two months.
How the team measured eye comfort
To capture what patients felt, the team used a questionnaire that asks about stinging, light sensitivity, and how much these symptoms interfere with daily life. They also used simple clinic tests: a strip of paper to measure how many tears the eye produces, a dye to see how quickly the tear film breaks up between blinks, and a staining score to show how much the eye’s surface has been irritated. In addition, they examined the oil-producing glands in the eyelids—known as meibomian glands—that help keep tears from evaporating too quickly.
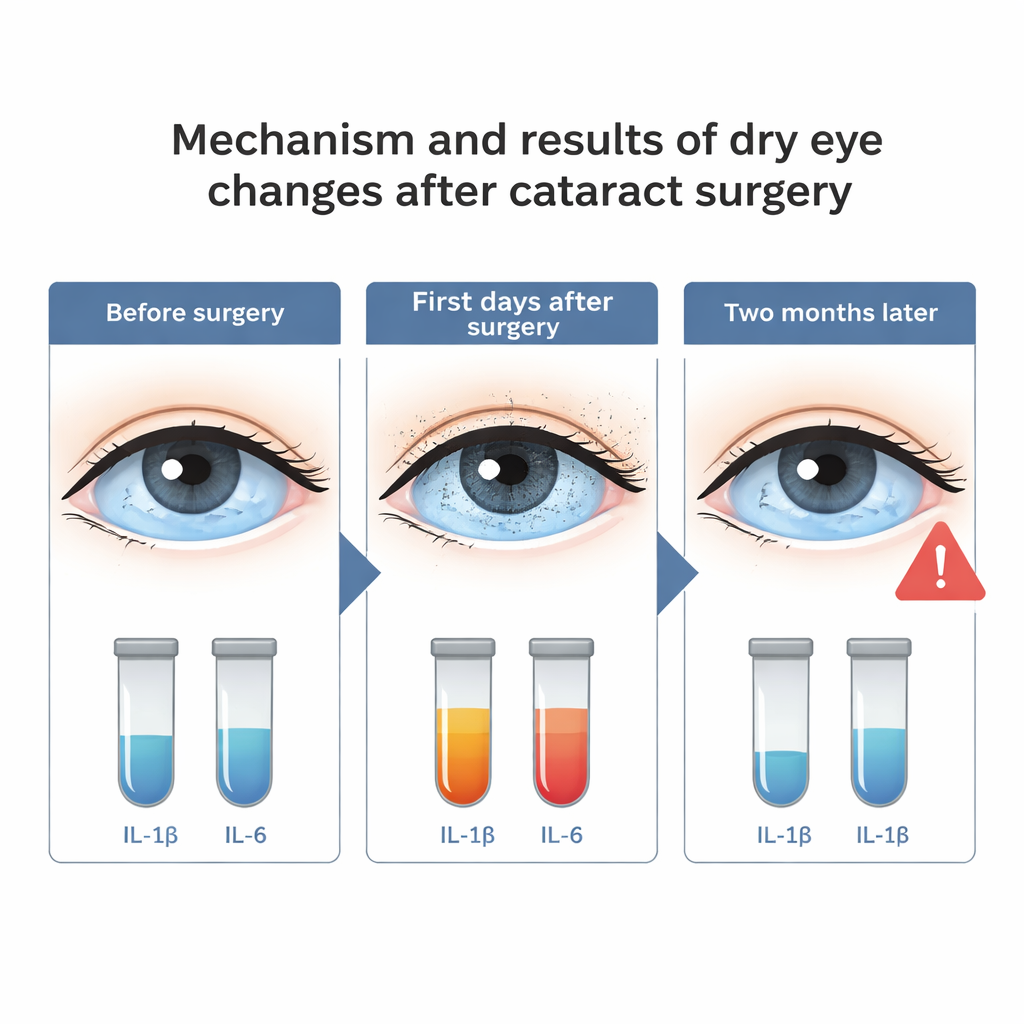
Inflammation hidden in the tears
Beyond what doctors can see at the slit lamp, the team looked for chemical signals of inflammation in the tears. They measured two molecules, interleukin‑1 beta (IL‑1β) and interleukin‑6 (IL‑6), which rise when tissues are irritated or injured. Tear samples were collected just before surgery, the day after, three weeks later, and again at two months. In both surgical groups, levels of these markers spiked sharply right after surgery, then gradually settled down. IL‑6 largely returned to its starting level by two months, but IL‑1β stayed higher than before surgery, suggesting a lingering low-grade irritation.
What differed between the two surgical styles
Both techniques clearly disturbed the eye surface in the short term. On the first day after surgery, patients in each group reported worse dryness symptoms, produced fewer tears, and showed more surface staining. These measures slowly improved but, even at two months, many values had not fully returned to pre-surgery levels. When the two operations were compared, some patterns stood out. The tear film in MSICS patients broke up more quickly at every visit, hinting that the larger incision and greater disturbance of corneal nerves may destabilize the tear layer more. On the other hand, the quality of eyelid oil seemed worse in the phacoemulsification group, and their inflammatory markers in tears—especially IL‑1β—tended to be higher at the two‑month mark.
What this means for patients and surgeons
For people planning cataract surgery, these findings underline that dry, uncomfortable eyes are not unusual afterward, even when the operation goes smoothly. Both small‑cut and larger‑cut techniques can temporarily upset the balance of tears, eyelid oils, and microscopic inflammation on the eye’s surface. The study suggests that simple office tests and attention to eyelid gland health are usually enough to track these changes and guide treatment. With lubricating drops and, when needed, anti‑inflammatory medicines, most patients can expect their eyes to feel steadily better over the weeks following surgery, even if subtle signs of irritation linger longer beneath the surface.
Citation: Behera, G., Ramachandar, H., Rajappa, M. et al. Comparison of clinical and inflammatory markers for dry eye disease following phacoemulsification and manual small incision cataract surgery (MSICS). Sci Rep 16, 5734 (2026). https://doi.org/10.1038/s41598-026-36738-1
Keywords: cataract surgery, dry eye, phacoemulsification, MSICS, tear inflammation