Clear Sky Science · en
Evaluation of idiopathic olfactory dysfunction as a warning marker for early parkinson’s disease: a population-based cross-sectional study
Why losing your sense of smell matters
Most of us think of Parkinson’s disease as a disorder of shaking hands and stiff muscles. But long before these visible signs appear, the disease may be quietly affecting other parts of the body—especially the sense of smell. This study asked a simple question with big implications: can an otherwise unexplained loss of smell serve as an early warning flag for Parkinson’s, allowing doctors to spot at-risk people years sooner and intervene earlier?
Smell as an early warning signal
Researchers in Mashhad, Iran, focused on people with idiopathic olfactory disorder—smell loss that cannot be explained by allergies, sinus problems, head injury, or other obvious causes. Earlier work has shown that 70–90% of people with Parkinson’s have trouble smelling, often years before tremors begin. Because a smell test is cheap, quick, and painless, it offers an appealing way to screen large groups of people for hidden risk. The challenge is that smell problems are also common in the general population, so the team needed a way to separate harmless cases from those that might signal the early, or “prodromal,” phase of Parkinson’s.
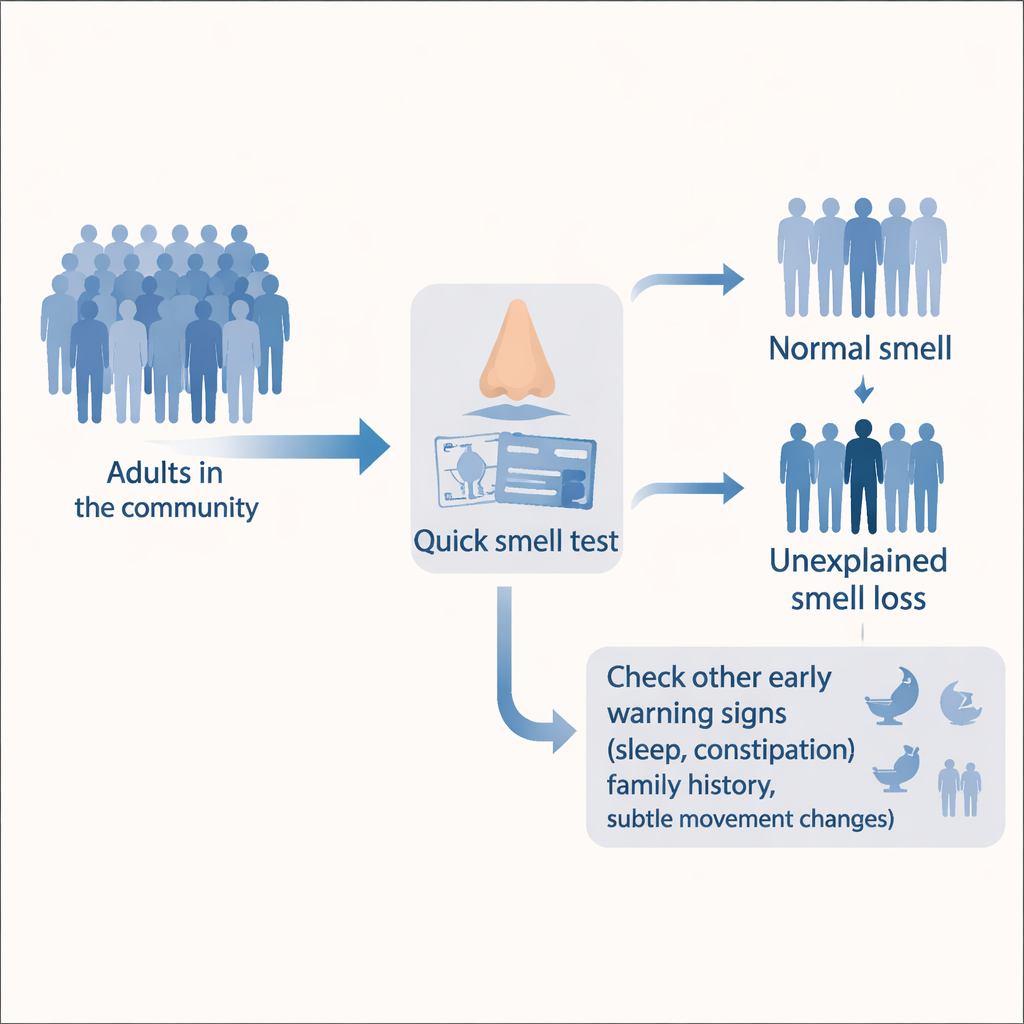
A two-step screening approach
The investigators used a stepwise design built for real-world clinics and community programs. First, 1,044 adults from an ongoing Persian Cohort Study took a rapid six-item smell test tailored to familiar Iranian odors. Next, anyone whose smell loss could be traced to known causes—such as chronic sinus disease, certain medications, or past head trauma—was excluded. This left 701 people, all with either normal smell or idiopathic smell loss. These participants were then evaluated using international research guidelines from the Movement Disorder Society, which combine age, lifestyle factors (like smoking, caffeine use, and pesticide exposure), and early symptoms (such as constipation, sleep problems, or subtle movement changes) into an overall probability score for being in the early phase of Parkinson’s.
Who had unexplained smell loss?
In this carefully filtered group, 13.6% had idiopathic smell problems. Smell scores tended to worsen with age: only a tiny fraction of adults under 50 had severe loss, while among those 50 and older, about a quarter met criteria for idiopathic dysfunction. Several everyday factors were linked to poorer smell performance. Men were more likely than women to have reduced smell. Regular exposure to pesticides and solvents, not using caffeine, current smoking, and constipation all showed clear associations with low smell scores. Together, these patterns support the idea that smell loss often clusters with other subtle changes long before a Parkinson’s diagnosis is made.
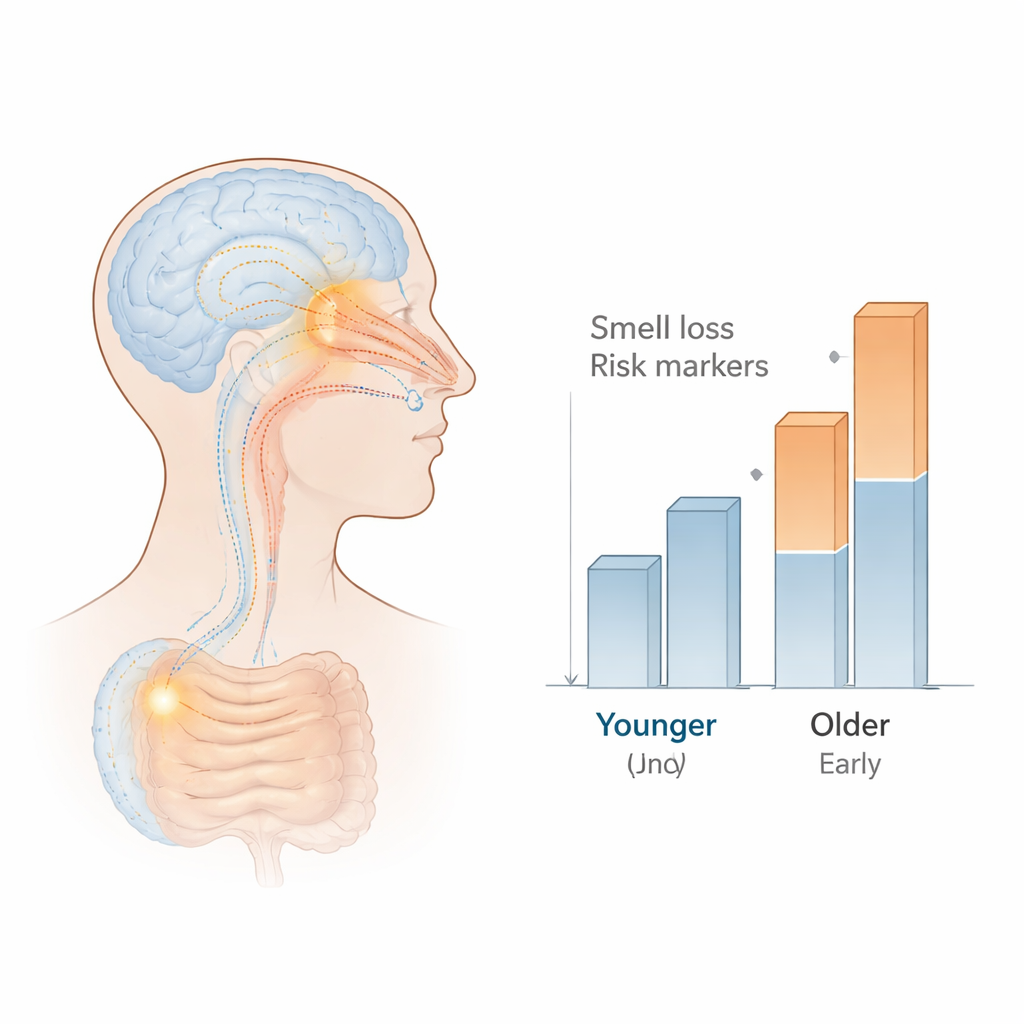
Finding the rare high‑risk individual
When the team applied the formal Parkinson’s risk calculator, almost everyone—despite some having idiopathic smell loss—fell below the threshold for “probable prodromal Parkinson’s disease.” One person, however, stood out. This 60‑year‑old man had complete loss of smell and several additional warning signs, including constipation, poor sleep, exposure to pesticides and solvents, and a family history of Parkinson’s. His calculated risk score was more than ten times higher than the cutoff used to define probable early Parkinson’s. At the time of screening, he had only very subtle movement changes, not enough for a full diagnosis. On follow-up, his symptoms progressed, and he was formally diagnosed with early Parkinson’s disease—confirming that the two-step approach had successfully flagged a true prodromal case.
What this means for patients and clinics
For the average person with unexplained smell loss, this study does not mean that Parkinson’s is inevitable. Most participants with idiopathic smell problems did not meet the criteria for being in the high-probability, prodromal phase of the disease. Instead, the work shows how smell testing can be used as a first “filter” to find a smaller group who deserve closer attention. In settings with limited resources, a quick smell test followed by a structured checklist of other risk factors could help doctors identify the rare individuals who should see a specialist quickly, while simply monitoring others over time. The authors conclude that idiopathic smell loss is best viewed as an enrichment marker: on its own it rarely proves that Parkinson’s is coming, but in combination with age and other early symptoms, it can spotlight those most likely to be on the road toward the disease—and who may benefit most from early, targeted care.
Citation: Vedadi, Z., Miandehi, E.E., Akbari, M. et al. Evaluation of idiopathic olfactory dysfunction as a warning marker for early parkinson’s disease: a population-based cross-sectional study. Sci Rep 16, 6329 (2026). https://doi.org/10.1038/s41598-026-36736-3
Keywords: Parkinson’s disease, smell loss, early diagnosis, prodromal markers, olfactory testing