Clear Sky Science · en
Cardiac autonomic function in bronchiectasis and age and gender-matched healthy participants: case–control study
When Lung Disease Reaches the Heart
Most people think of bronchiectasis as a lung problem: damaged airways, chronic cough, and frequent infections. But this study asks a bigger question with everyday consequences—does this long‑standing lung disease quietly strain the heart’s control system, raising future risks for fatigue, poor exercise tolerance, and even heart trouble? Understanding that hidden link could change how doctors monitor and protect patients living with bronchiectasis.
A Quiet Communication Network in Trouble
The heart does not beat on its own schedule. It is constantly guided by the autonomic nervous system, a built‑in control network that speeds the heart up when we are active or stressed and slows it down when we rest. One way to measure how well this system works is heart rate variability, or HRV—tiny, natural changes in the time between heartbeats. Higher and more flexible variability is usually a sign of a healthier, more adaptable heart. The researchers wanted to know whether people with bronchiectasis, a chronic condition in which the airways become widened and scarred, show signs of disrupted autonomic control compared with similar people who do not have lung disease.
Comparing Patients and Healthy Neighbors
The team carried out a case–control study in India, enrolling 60 adults with confirmed bronchiectasis and 60 healthy adults matched by age and sex. Everyone had a normal body‑mass range and no major illnesses such as heart disease, high blood pressure, diabetes, or cancer that might cloud the results. In a quiet, temperature‑controlled room, participants rested lying down before wearing a chest strap heart monitor for a five‑minute recording. From those recordings, specialized software calculated several HRV measures that reflect how strongly the “accelerator” (sympathetic nerves) and “brake” (parasympathetic nerves) of the heart are working.
Signs of a Stressed Heart Control System
Compared with their healthy counterparts, people with bronchiectasis had a faster resting heart rate, slightly lower oxygen levels, and a lower average body weight. More importantly, they showed clear differences in HRV. Overall variability was reduced, and two key measures—called low‑frequency and high‑frequency power—were lower in the bronchiectasis group. High‑frequency power is closely linked to the calming, parasympathetic branch, so its drop suggests weaker “rest and recover” signals to the heart. At the same time, the ratio of low‑ to high‑frequency power was higher, pointing to a shift toward sympathetic, stress‑like activity even while at rest. Taken together, these patterns suggest that the heart in bronchiectasis patients is being nudged into a more strained, less flexible state.
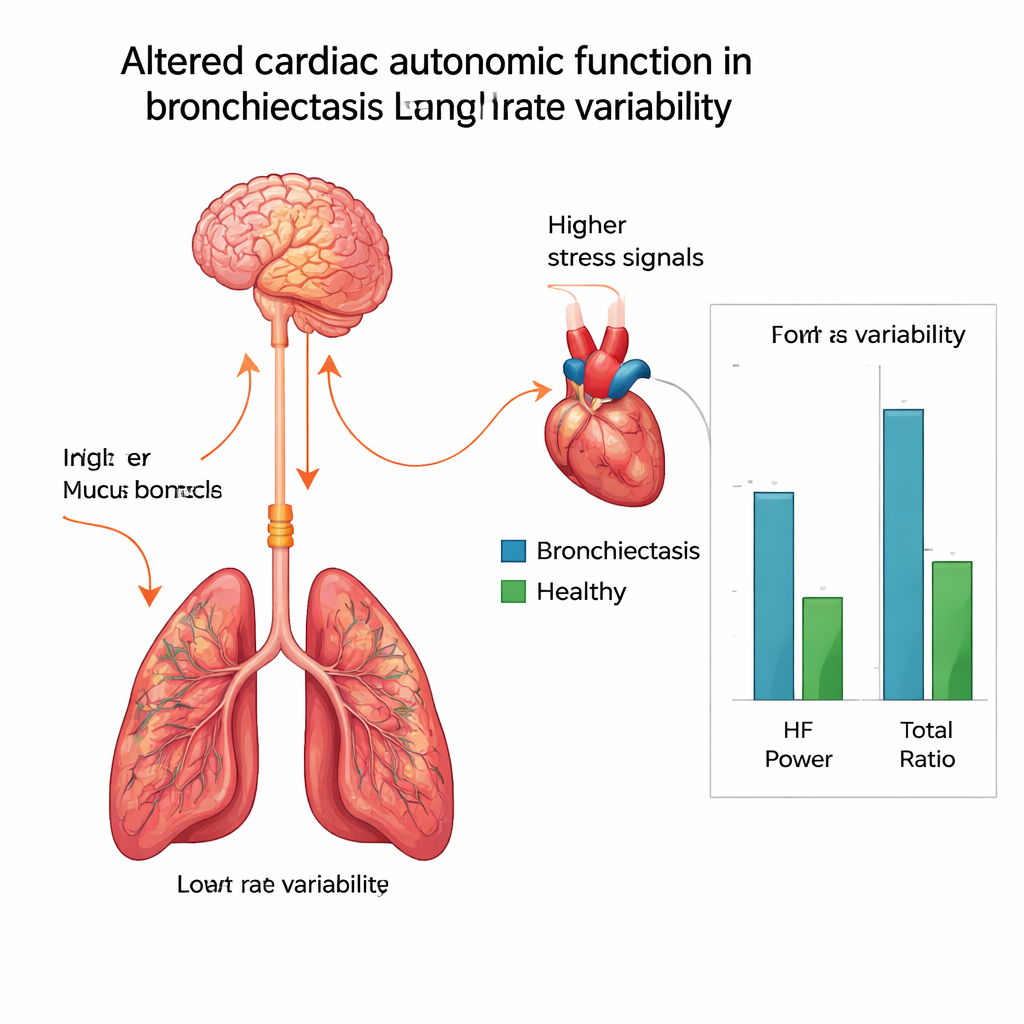
Why Chronic Lung Damage Reaches the Heart
The authors propose several reasons why a lung disease might unsettle the heart’s control system. Persistent airway inflammation can release chemical signals into the bloodstream that act on nerves and blood vessels. Even mild drops in blood oxygen, extra effort spent breathing, and long‑term use of certain inhaled drugs may all stimulate the body’s stress responses. Over months and years, this background strain could tip the balance toward sympathetic dominance and lower HRV. The study also notes that real‑world patients often have overlapping breathing problems such as asthma or chronic obstructive lung disease, which may further alter autonomic control. Although the researchers carefully excluded many other illnesses, they acknowledge that differences in medications, mental health, and recovery from recent flare‑ups could also play a role.
What This Means for Patients and Care
For non‑specialists, the message is straightforward: bronchiectasis affects more than the lungs. This study shows that even in a relatively stable phase of the disease, many patients already display a heart rhythm pattern associated with higher cardiovascular risk in other conditions. Because HRV can be measured non‑invasively with modern heart monitors, it may become a useful early warning sign to flag patients who would benefit from closer heart check‑ups, exercise‑based rehabilitation, and better control of inflammation and breathing symptoms. While more research is needed to untangle the exact causes and to test targeted treatments, the work highlights that protecting heart health should be a routine part of caring for people with long‑standing bronchiectasis.
Citation: Dinesh, D., Vaishali, K., Bhat, A. et al. Cardiac autonomic function in bronchiectasis and age and gender-matched healthy participants: case–control study. Sci Rep 16, 7032 (2026). https://doi.org/10.1038/s41598-026-36722-9
Keywords: bronchiectasis, heart rate variability, autonomic nervous system, chronic lung disease, cardiovascular risk