Clear Sky Science · en
Identification and verification of SPP1 in anoikis as a prognostic biomarker for intestinal metaplasia and gastric cancer
Why this matters for stomach health
Gastric (stomach) cancer is one of the world’s deadliest cancers largely because it is usually discovered late. Before a full-blown tumor appears, the stomach lining often passes through a warning stage called intestinal metaplasia, where normal stomach cells begin to resemble those in the intestine. This study follows that entire journey—from healthy tissue, through intestinal metaplasia, to gastric cancer—to search for a single measurable signal in the tissue that could flag high risk early and help doctors predict which patients are most likely to fare poorly and might benefit from closer follow-up or new treatments.
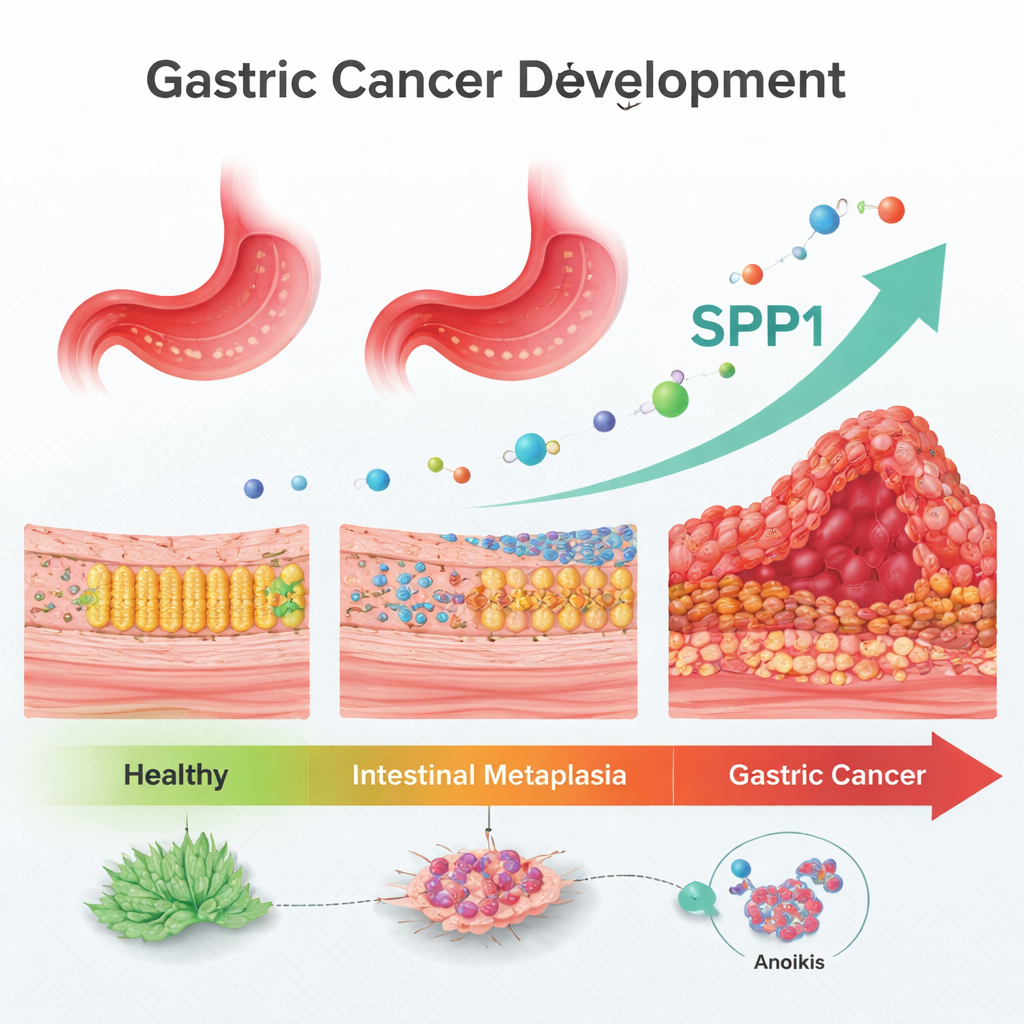
A stepping-stone on the road to cancer
Doctors have long known that intestinal metaplasia is a premalignant condition, but they lack reliable markers to tell who will actually progress to cancer. The researchers focused on a type of cell death called anoikis, which normally kills cells that detach from their proper place in a tissue. Cancer cells must learn to resist anoikis in order to move, survive in the bloodstream, and seed distant tumors. By mining large public gene databases from hundreds of patients, the team looked for genes linked to anoikis that change steadily across the “Correa cascade”: healthy stomach lining, intestinal metaplasia, and finally gastric cancer.
Zeroing in on a key warning molecule
Using advanced statistical tools and network analyses, the scientists repeatedly identified one standout gene: SPP1, which makes a protein also known as osteopontin. Across three independent datasets, SPP1 levels were consistently low in healthy stomach tissue, higher in intestinal metaplasia, and highest in gastric cancer. This stepwise pattern held up even after correcting for technical differences between studies. Further computer analyses of thousands of genes showed that high SPP1 tended to appear alongside changes in immune-related pathways and responses to environmental and chemical stress, suggesting that the molecule might be weaving together cell survival, chronic irritation, and the immune system during cancer development.
Clues from the body’s defense cells
The team next examined how SPP1 relates to the immune cells that infiltrate tumors. In bulk tumor samples, higher SPP1 was tied to shifts in the balance of immune cells, including increases in certain macrophages and T cells that can either attack tumors or be turned off by them. Single-cell RNA sequencing—reading gene activity one cell at a time—revealed that SPP1 was strongly switched on in tumor-associated macrophages and other cells in the tumor environment. Signals involving SPP1 and a partner receptor called CD44 appeared to link these macrophages to helper T cells, hinting that this pathway may help create an immune “neighborhood” that favors tumor survival rather than clearance. Although these links are correlative, they point to SPP1 as a potential player in how gastric tumors evade immune attack.
From big data to real tissues and cells
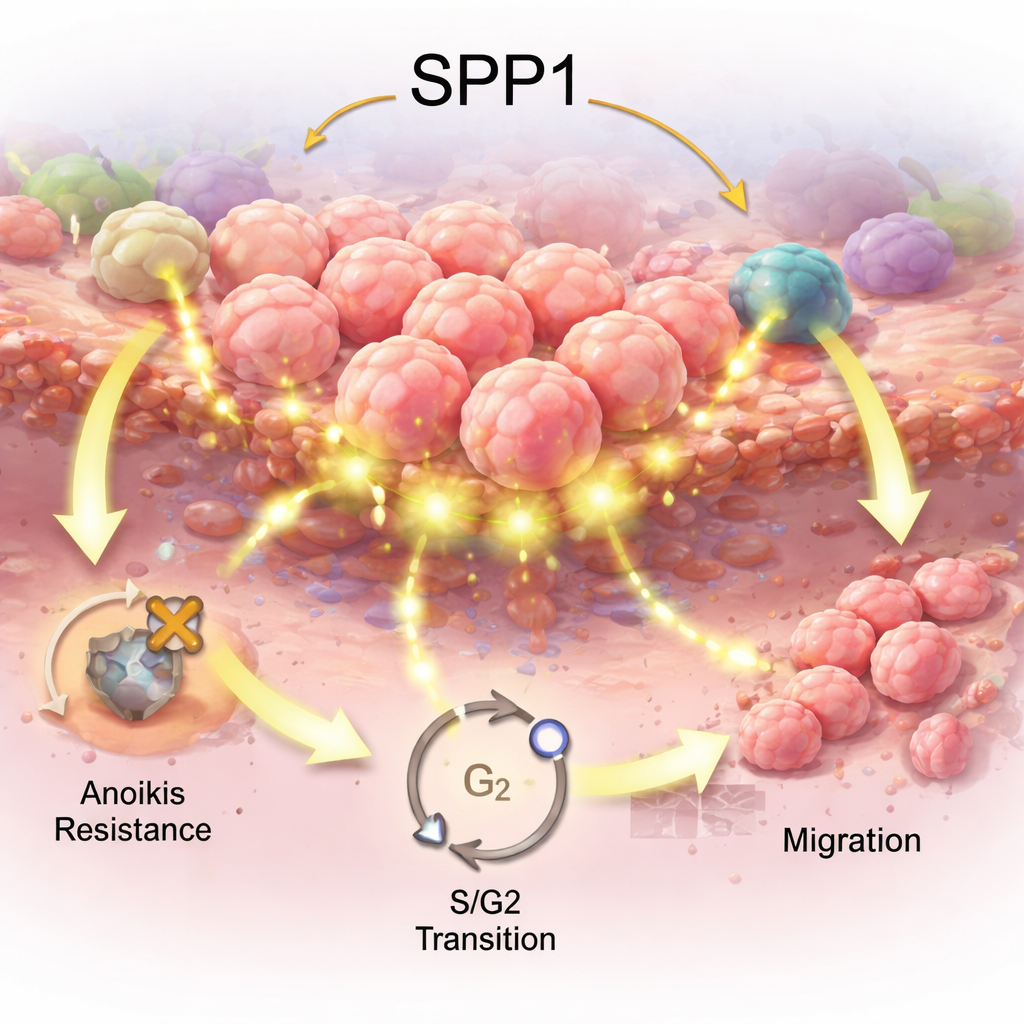
To check that the computer findings matched reality, the researchers measured SPP1 in 32 human stomach tissue samples. Both gene and protein tests showed the same trend: lowest levels in normal tissue, higher in intestinal metaplasia, and highest in gastric cancer. Patients whose tumors expressed more SPP1 had substantially worse overall survival, and statistical models suggested that SPP1 helped predict one-, three-, and five-year outcomes. In cell culture, turning down SPP1 in a gastric cancer cell line slowed cell growth, reduced their ability to migrate, increased programmed cell death, and caused cells to stall in a critical phase of the cell cycle. These experiments support the idea that SPP1 actively helps cancer cells resist dying and continue dividing.
What this could mean for patients
For non-specialists, the takeaway is that SPP1 behaves like a rising alarm bell along the path from a “risky but not yet cancerous” stomach lining to full cancer. High levels of this molecule mark tissues that are more likely to progress and patients who are more likely to have poor outcomes. Although more work is needed—especially larger patient studies and animal experiments—monitoring SPP1 in biopsies from intestinal metaplasia could one day help doctors decide who needs tighter surveillance or earlier treatment. In established gastric cancer, drugs that block SPP1 or its key partners might weaken the tumor’s defenses, both by making cancer cells more vulnerable to cell death and by reshaping the surrounding immune cells to fight the disease more effectively.
Citation: Wu, K., Ye, Y., Pei, B. et al. Identification and verification of SPP1 in anoikis as a prognostic biomarker for intestinal metaplasia and gastric cancer. Sci Rep 16, 5842 (2026). https://doi.org/10.1038/s41598-026-36714-9
Keywords: gastric cancer, intestinal metaplasia, biomarkers, osteopontin SPP1, tumor microenvironment