Clear Sky Science · en
The predictors of treatment adherence among hypertensive patients with cost-free access
Why skipping pills still matters when medicine is free
High blood pressure is often called the “silent killer” because it quietly damages the heart, brain and kidneys for years before any symptoms appear. Many people assume that if medicines are free, patients will take them as prescribed and stay healthy. This study from Ghana challenges that belief by showing that even when cost is removed, most workers with high blood pressure still do not take their medication regularly, putting their health and livelihoods at risk.
A closer look at workers with free heart medicine
The research focused on staff and family members of the Volta River Authority, a major employer in Ghana that covers the full cost of blood pressure drugs for its workers. Because money should not be an obstacle here, this group offers a powerful way to study other reasons why people stick with, or abandon, long-term treatment. The team surveyed 253 adults who had been diagnosed with high blood pressure for at least six months and were receiving free medicines at the company hospital’s hypertension clinic. Participants filled out a detailed questionnaire about their backgrounds, daily routines, side effects and how faithfully they took their pills.
When almost everyone falls off track
To judge how well people followed their treatment, the researchers used an eight-question checklist about everyday behaviors, such as forgetting doses, stopping pills when feeling better or worse, and finding the routine inconvenient. Only those who answered correctly on more than three-quarters of the items were counted as “adherent.” The result was startling: just 11.1 percent of patients met this standard, while 88.9 percent showed low adherence. In other words, nearly nine out of ten people with free access to medicine were not taking it as advised, leaving them vulnerable to strokes, heart attacks and other preventable complications.
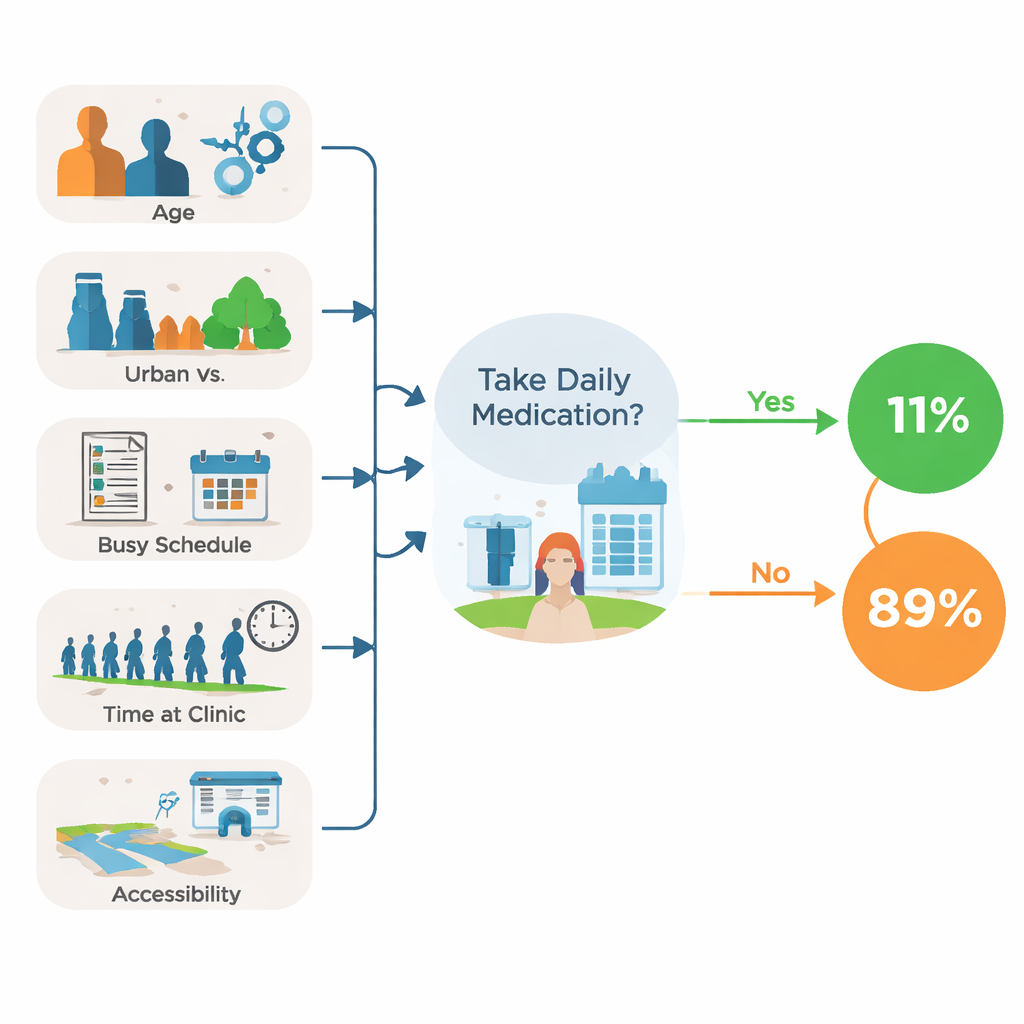
Life pressures, not price tags, drive many choices
The team then explored which factors were most closely linked with skipping treatment. Age, sex, place of residence, work demands, clinic experience and ease of reaching care all played a role. Younger adults in their twenties and people living in urban areas were more likely to take their medicines properly than older patients and those in rural settings, possibly because city dwellers and younger workers have better access to health information and services. Men, however, were less likely than women to follow their pill schedules. A packed workday and long waiting times at the clinic strongly discouraged adherence, suggesting that even free drugs are hard to use when refilling them requires hours away from job and family. In contrast, people who reported that the clinic was easy to reach were much more likely to stay on track with their treatment.
How the numbers were untangled
Because only a small fraction of patients were taking their medicine correctly, the researchers needed a statistical tool that could handle such unbalanced outcomes. They compared two related approaches for predicting adherence from multiple factors at once. While both methods showed that non-cost barriers mattered, a technique called the complementary log–log model captured the patterns in the data better than standard logistic regression. This means that when success (in this case, good adherence) is rare, more specialized tools can give clearer insight into which groups are at highest risk of falling behind on treatment.
What this means for everyday health
For non-specialists, the message is plain: making medicine free is necessary but not sufficient to keep blood pressure under control. In this Ghanaian workforce, most patients still missed doses or stopped pills, despite not paying out of pocket. Practical obstacles—busy schedules, long queues, difficult travel—and personal factors like gender and age strongly shaped behavior. The authors conclude that employers and health services must redesign care around patients’ lives, for example by shortening clinic waits, improving access in rural areas, addressing side effects and providing regular education and support. Only by tackling these real-world barriers, alongside reducing costs, can we expect more people to take their daily pills and avoid the silent damage of uncontrolled high blood pressure.
Citation: Nyande, F.K., Konlan, K.D., Asiamah, L.S. et al. The predictors of treatment adherence among hypertensive patients with cost-free access. Sci Rep 16, 6658 (2026). https://doi.org/10.1038/s41598-026-36702-z
Keywords: hypertension, medication adherence, Ghana, workplace health, chronic disease management