Clear Sky Science · en
Activation of LH orexin neurons and VTA dopamine neurons is involved in anesthesia/surgery-induced sleep–wake disorders and delirium-like behaviors in mice
Why surgery can unsettle sleep and thinking
Many people, especially older adults, notice that after surgery they sleep poorly and feel unusually confused or disoriented. Doctors call this combination of disturbed sleep and short-term confusion "postoperative delirium," and it can slow recovery and increase the risk of long-term problems. This study in mice asks a simple but important question: what is happening inside the brain after anesthesia and surgery that links broken sleep and delirium-like behavior—and could an existing sleep drug help?
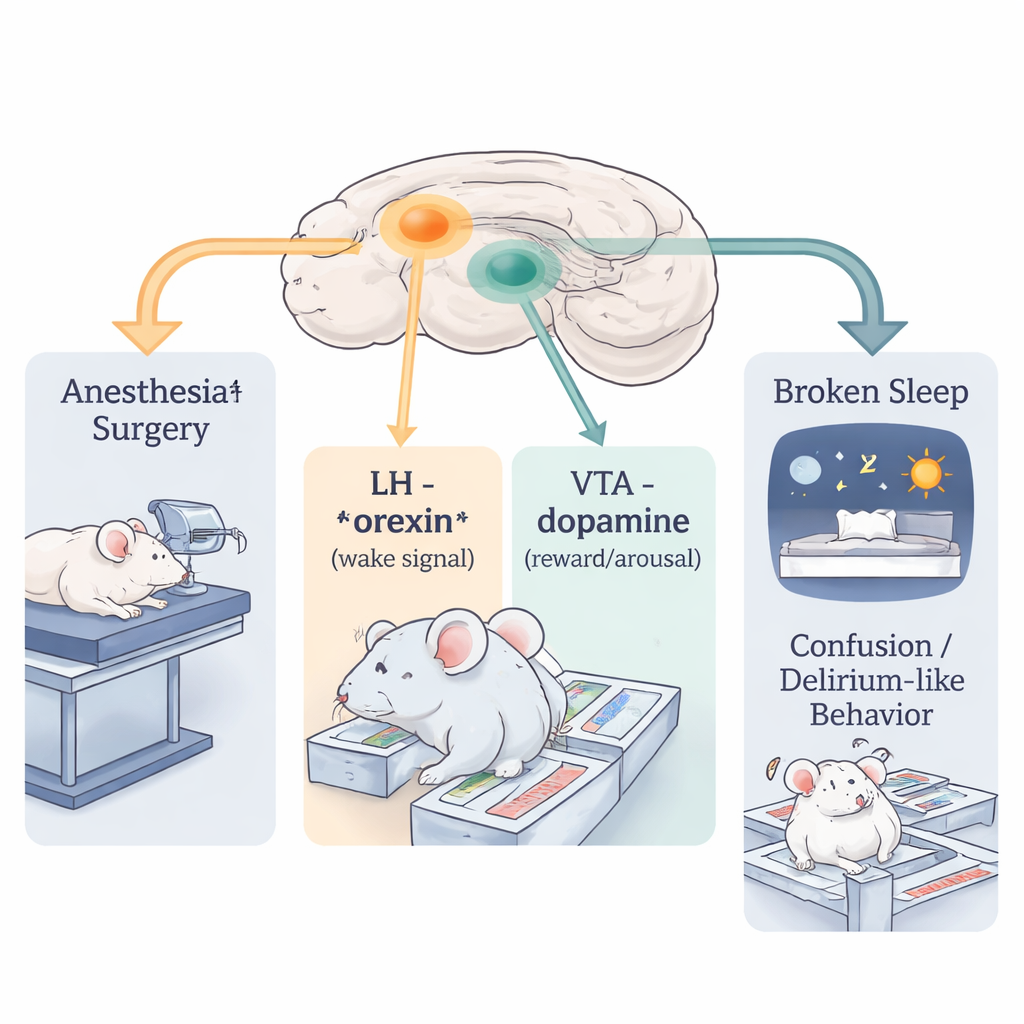
How the brain keeps us awake—or lets us sleep
Sleep and wakefulness are controlled by a network of brain areas that act a bit like a switchboard. One key region, the lateral hypothalamus, sends out a chemical messenger called orexin that strongly promotes wakefulness and alertness. Another region, the ventral tegmental area, is rich in dopamine-producing cells that support motivation, reward, and arousal. In healthy conditions these systems balance brain states so we cycle smoothly between restful sleep and refreshing wakefulness. When this balance is disturbed, people can feel wired but foggy, anxious, and cognitively impaired.
What anesthesia and surgery did in mice
The researchers used a standard abdominal surgery under the anesthetic sevoflurane in middle-aged mice, then measured behavior and brain activity. Compared with control mice, operated mice took longer to find buried food, avoided the center of an open arena, and performed worse in a Y-shaped maze, all signs of anxiety and delirium-like confusion. Brain recordings over 24 hours showed that these mice spent more time awake and less time in both deep non-REM sleep and dream-like REM sleep during the day, when mice usually sleep. Their sleep became fragmented, with many brief episodes and weaker slow brain waves that normally help restore the brain and support memory.
Overactive wake signals and dopamine after surgery
To see which brain circuits were involved, the team examined markers of recent neural activity in regions that promote sleep and wakefulness. After anesthesia and surgery, sleep-promoting areas in the preoptic region were quieter, while wake-promoting zones in the lateral hypothalamus and a nearby anxiety-related region became more active. Orexin-producing nerve cells in the lateral hypothalamus fired more and released more orexin A. At the same time, dopamine-producing neurons in the ventral tegmental area were more active, showed higher levels of the enzyme needed to make dopamine, and the midbrain contained more dopamine overall. Together, these findings suggest that surgery pushes the brain into an over-aroused, dopamine-rich state that keeps animals awake yet mentally impaired.
Testing a sleep medicine as a possible fix
The scientists next asked whether dialing down orexin signaling could calm this overactive circuit. They gave some mice suvorexant, an approved insomnia drug that blocks both main orexin receptors, for two weeks before surgery. In mice that then underwent anesthesia and surgery, suvorexant reduced activation of dopamine neurons in the ventral tegmental area, lowered dopamine-related protein levels, and brought dopamine concentrations closer to normal. Behaviorally, these mice found food faster, spent more time exploring the center of the open field, and performed better in the Y-maze than untreated surgery mice. Their daytime sleep also improved, with more non-REM sleep and less wakefulness, while not greatly disturbing normal animals that received the drug without surgery.
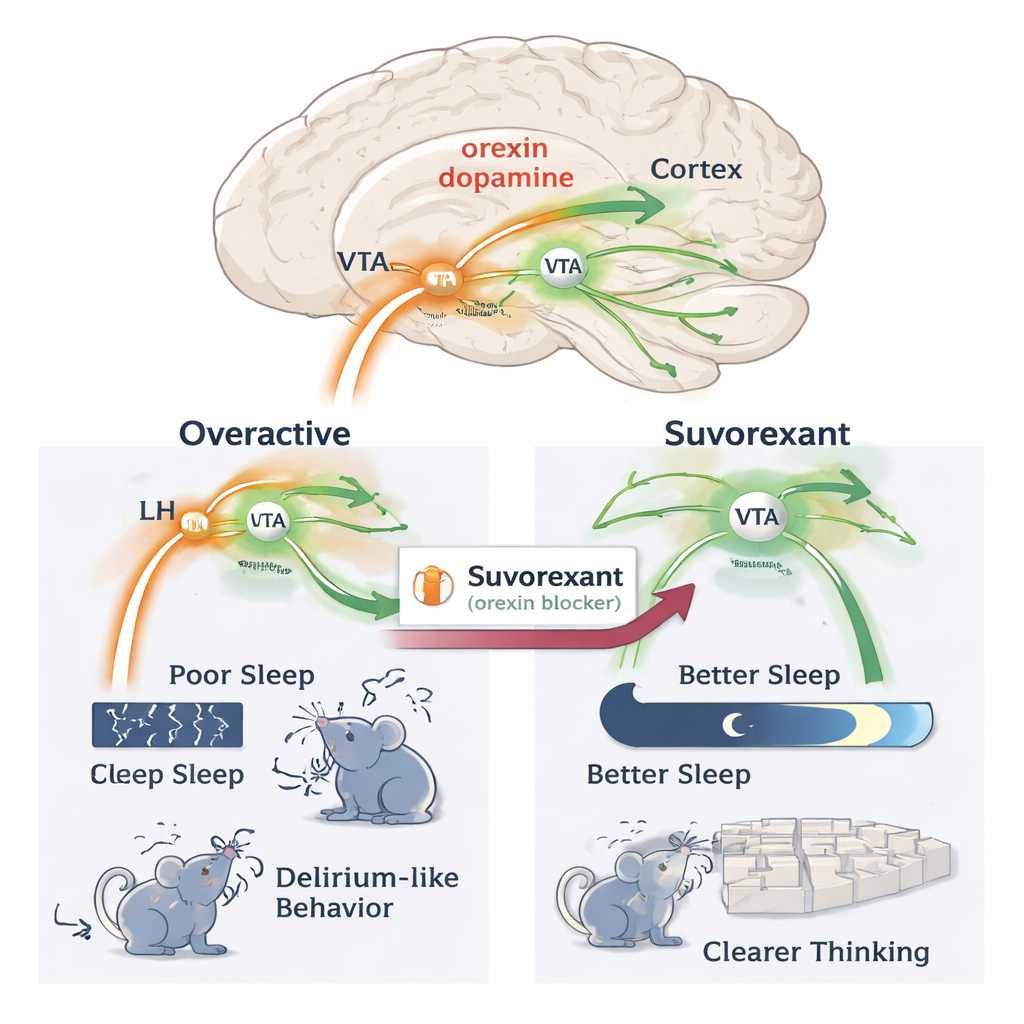
What this could mean for patients
In plain terms, this work supports the idea that surgery and anesthesia can flip the brain’s arousal systems into an overdrive state powered by orexin and dopamine. That state seems to fragment sleep and foster delirium-like confusion. By blocking orexin, suvorexant dampened this over-arousal and helped restore both sleep and behavior in mice. While animal findings do not directly translate to people, the study highlights the orexin–dopamine pathway as a promising target for preventing or treating postoperative sleep problems and delirium, using drugs that are already in clinical use for insomnia.
Citation: Han, S., He, K., Cao, L. et al. Activation of LH orexin neurons and VTA dopamine neurons is involved in anesthesia/surgery-induced sleep–wake disorders and delirium-like behaviors in mice. Sci Rep 16, 6035 (2026). https://doi.org/10.1038/s41598-026-36688-8
Keywords: postoperative delirium, sleep disturbances, orexin, dopamine, suvorexant