Clear Sky Science · en
Resting-state brain function and its modulation by intranasal oxytocin in antisocial personality disorder with and without psychopathy
Why this research matters for understanding violent behavior
Why do some people with a history of serious violence seem cold and calculating, while others are hot-headed and impulsive? And could a simple nasal spray ever help shift the brain patterns behind such behavior? This study looks inside the resting brain of men with antisocial personality disorder, with and without psychopathy, to see how their brain activity differs from non-offenders and how it responds to oxytocin, a hormone often linked to trust, bonding, and social connection.
Looking at the brain at rest
Rather than asking participants to perform tasks in a scanner, the researchers focused on what the brain is doing in a quiet, resting state. They recruited three groups of men: violent offenders with antisocial personality disorder and high psychopathic traits, violent offenders with antisocial personality disorder but lower psychopathic traits, and healthy men with no criminal record. Using a non-invasive MRI technique that measures blood flow in different brain regions, they compared how active various areas were when participants simply lay still in the scanner. They also used a rigorous double-blind, placebo-controlled crossover design, giving each man both a dose of intranasal oxytocin and a placebo spray on different days, then comparing the brain scans.
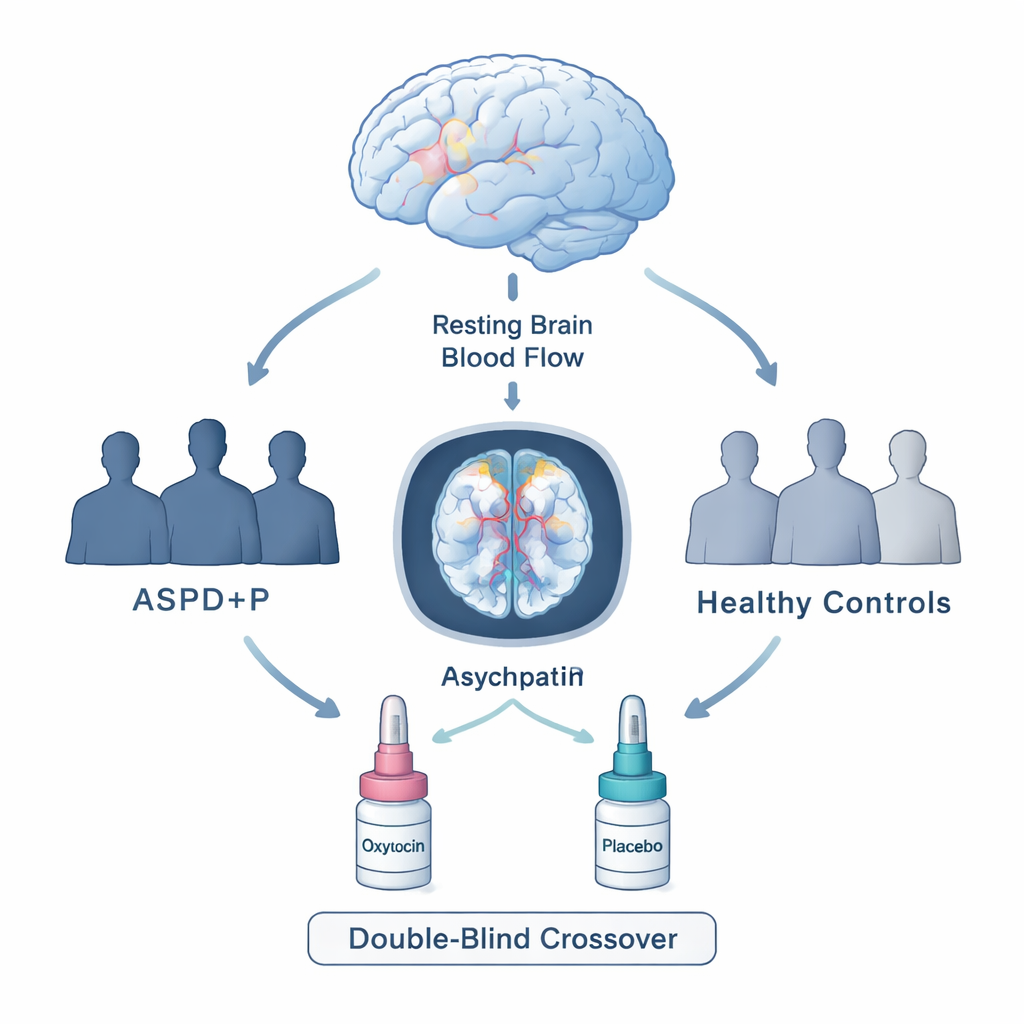
Shared brain changes in antisocial men
The study found that both groups of antisocial men showed lower blood flow in several key regions in the front and side of the brain compared with non-offenders. These frontotemporal areas are important for controlling impulses, learning from punishment, making flexible decisions, and interpreting other people’s signals. Lower activity at rest in these regions may make it harder for people to adjust their behavior when rules change or when their actions hurt others. These findings align with earlier work showing structural and functional changes in similar regions among people with serious antisocial behavior, but the current study used a more precise and reliable blood flow measure and carefully defined clinical groups.
What sets psychopathy apart
Despite these shared patterns, the group with psychopathy stood out in one important way. Men with antisocial personality disorder and high psychopathic traits showed higher blood flow in a cluster of regions at the back and middle of the brain that form the core of the brain’s "default mode" network, including the posterior cingulate and precuneus. In healthy people, this network is especially active at rest and supports functions such as self-reflection, imagining others’ minds, and recalling personal memories. In psychopathy, this region has long been suspected to work differently. The elevated resting activity seen here may reflect altered network wiring, possible compensation for other deficits, or difficulty turning this inward-focused system down when attention should shift outward to tasks or social cues.
How oxytocin affected different antisocial brains
Oxytocin is often discussed as a "social" hormone because of its role in bonding and empathy. Earlier studies suggested it can temporarily normalize some brain responses to emotional faces in psychopathic offenders. In this resting-state study, however, oxytocin did not change activity in the two regions the team had expected—the amygdala and anterior insula—or in the default mode network. Instead, its effects were highly specific and differed by subgroup. Only the antisocial group without psychopathy showed a clear response: after oxytocin, they had reduced blood flow in a deep brain region on the left side known as the basal ganglia, which helps govern habits, learning from rewards and punishments, and choosing actions.
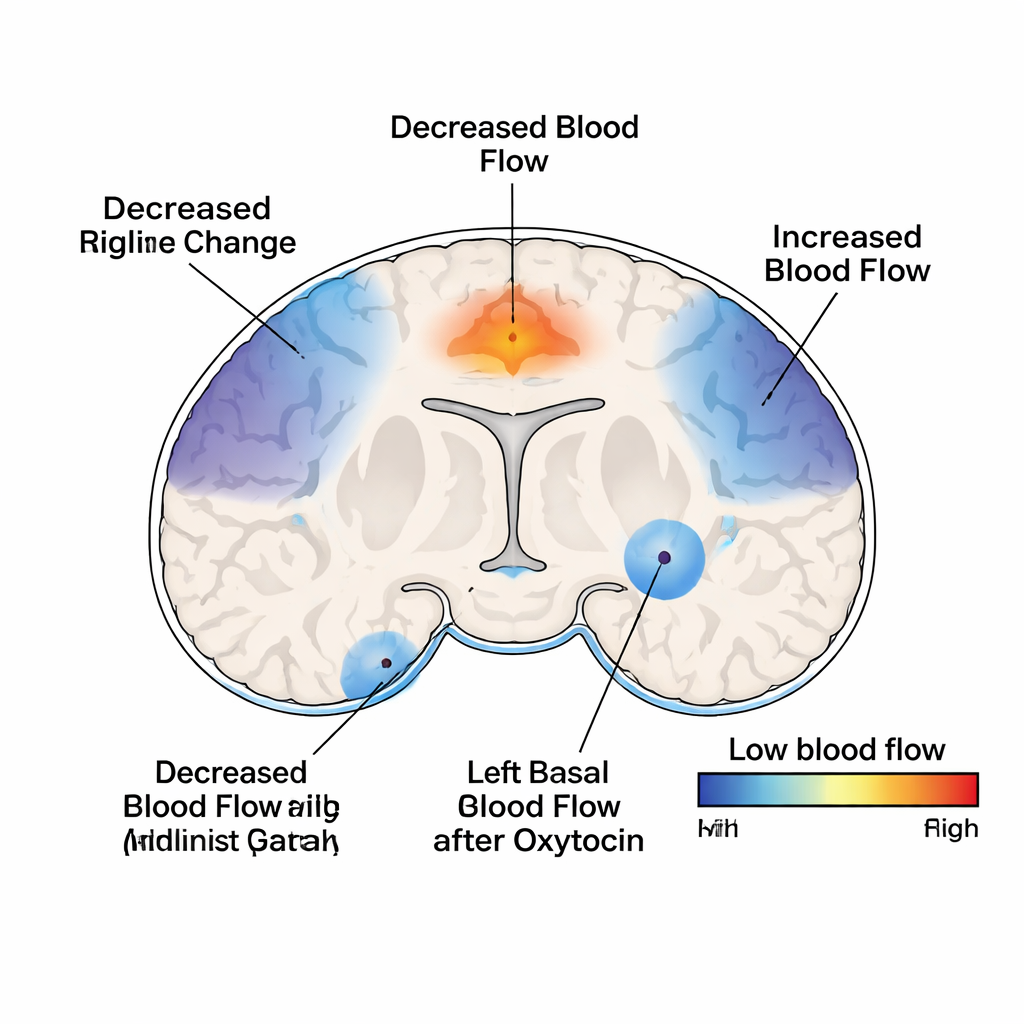
What this could mean for future treatments
The selective oxytocin effect in the non-psychopathic antisocial group suggests that brain chemistry and treatment sensitivity may differ meaningfully between antisocial individuals with and without psychopathy. Because the basal ganglia shape how people learn from consequences and form habits, changing activity here might, in principle, influence how someone with antisocial personality disorder responds to rewards, punishments, or rehabilitation programs. At the same time, the lack of detectable oxytocin effects in the psychopathic group at the measured time point warns against assuming that one biological intervention will work equally well for all forms of serious antisocial behavior. Overall, the study supports the idea that antisocial personality disorder is not a single biological entity and that tailoring future treatments—including pharmacological approaches like oxytocin—will likely require taking psychopathic traits and underlying brain differences into account.
Citation: Griem, J., Martins, D., Tully, J. et al. Resting-state brain function and its modulation by intranasal oxytocin in antisocial personality disorder with and without psychopathy. Sci Rep 16, 6207 (2026). https://doi.org/10.1038/s41598-026-36661-5
Keywords: antisocial personality disorder, psychopathy, oxytocin, brain blood flow, resting-state MRI