Clear Sky Science · en
Preprocedural vascular sheath insertion reduces hospital mortality in high risk PCI patients
Why this matters for people with heart disease
When a heart artery is badly blocked, doctors can open it with a procedure called PCI, threading tiny tools through blood vessels to restore blood flow. For people who are especially fragile, this life-saving procedure can also be very risky, sometimes leading to sudden heart failure or brain injury. This study asks a simple but important question: if doctors quietly prepare an extra "emergency access" to the blood vessels before starting the high‑risk procedure, can they step in faster when trouble strikes—and does that preparation actually save lives?
A safety backup before the crisis
In high‑risk PCI, patients already have weakened hearts or very complex blockages, so even brief drops in blood pressure can be dangerous. Doctors can support circulation with machines that pump or oxygenate blood outside the body, but setting these up in a rush is slow and technically demanding. The idea tested here is straightforward: before PCI begins, the team places small tubes (called sheaths) into a major artery and vein in the groin. These tubes are like ready‑made ports, allowing rapid connection to heart‑support machines if the patient suddenly crashes. 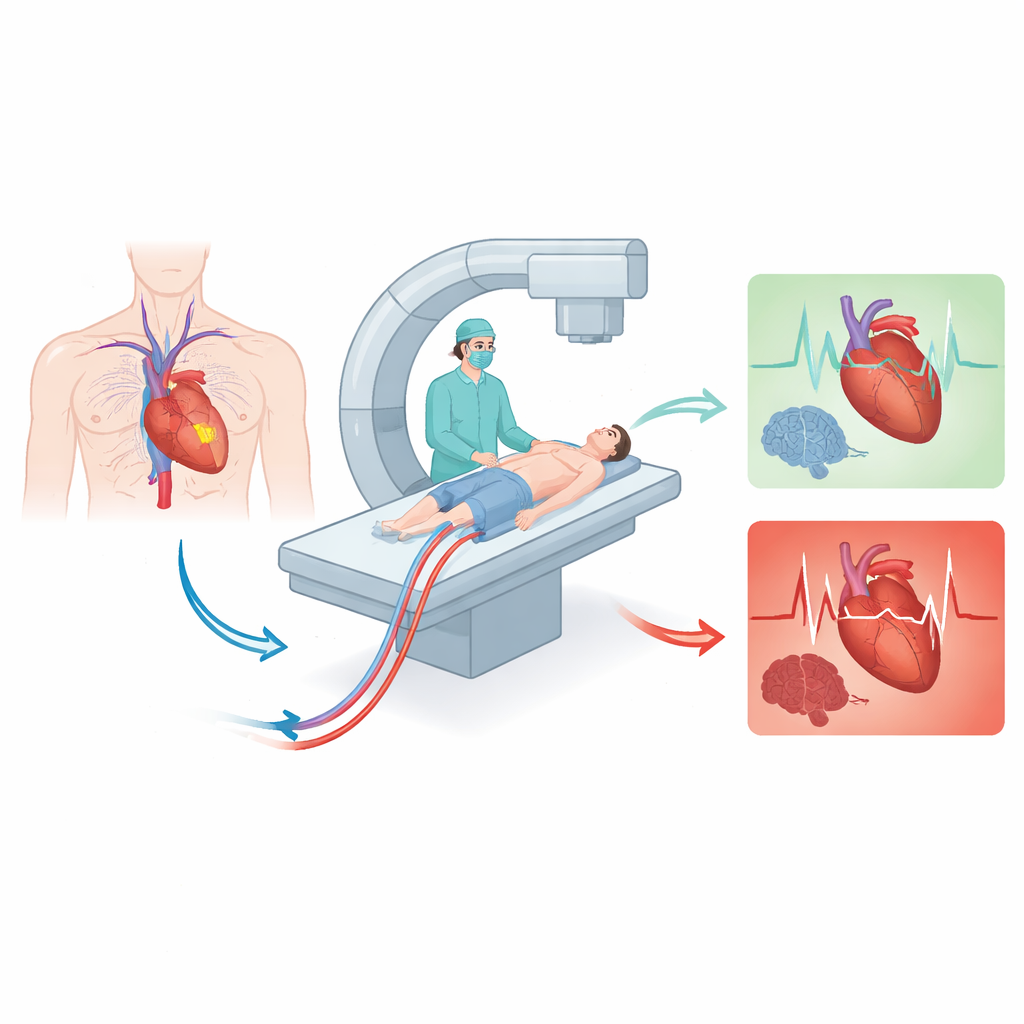
How the researchers tested the idea
Doctors at two large hospitals in China reviewed records from 443 people who underwent high‑risk PCI between 2018 and 2022. Some patients had these groin sheaths placed in advance, while others did not and would need fresh needle punctures if emergency support was required. Because the study was not a randomized trial, the team used a matching method to pair each patient who received pre‑inserted sheaths with a similar patient who did not, balancing factors such as age, other illnesses, heart function, and type of blockage. This approach helps mimic the fairness of a randomized study and reduces the chance that differences in outcomes are driven only by who doctors originally chose for the new strategy.
What happened to patients with and without preplaced sheaths
After matching, 220 patients were compared in two equal groups. The differences were striking: only about 1 in 22 patients with pre‑inserted sheaths died in the hospital, versus about 1 in 6 in the standard‑care group. The risk of leaving the hospital with serious brain problems was also cut by more than half in the sheath group. At the same time, there was no clear increase in leg complications, such as bleeding or poor blood flow, despite the extra tubes in the groin. Interestingly, the overall use of heart‑support machines was similar in both groups, but when they were needed, the team could connect them much faster—cutting hookup time by roughly 10 to 15 minutes—because the access ports were already in place. 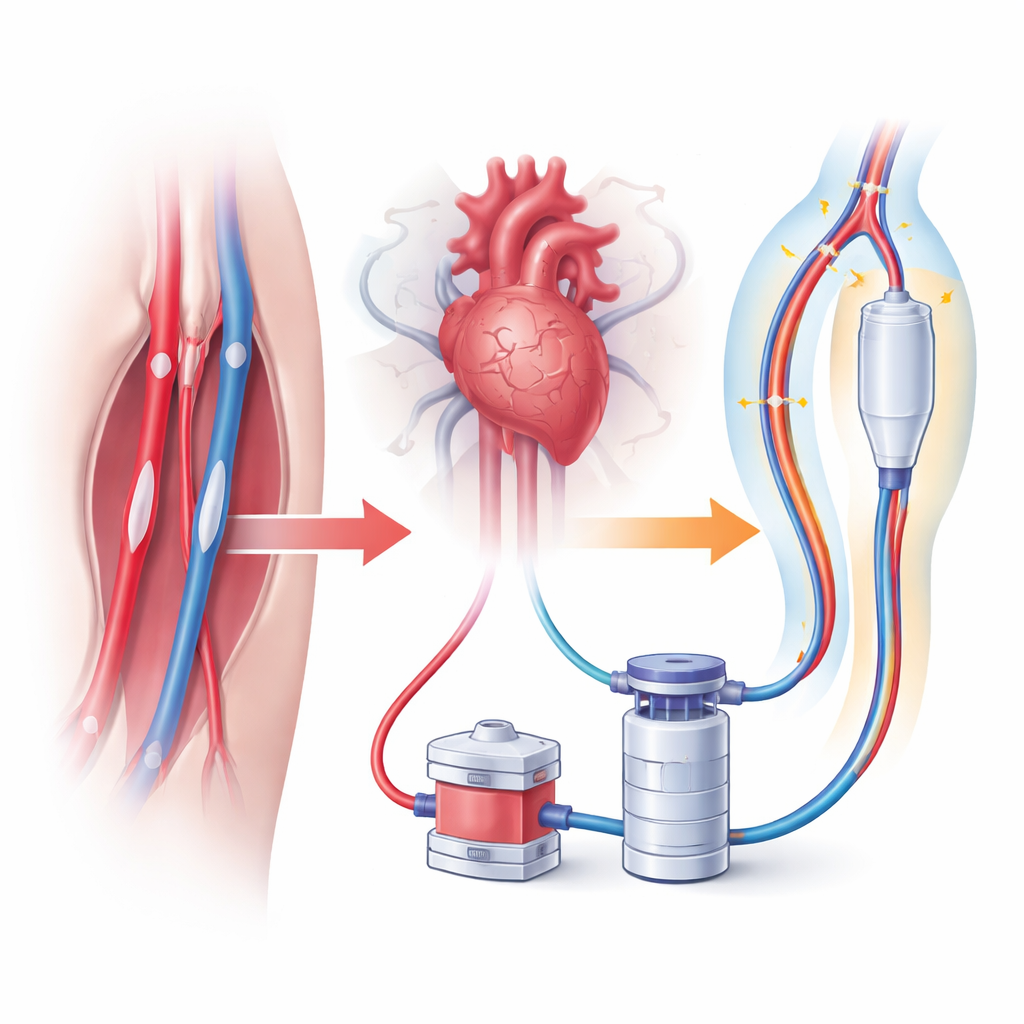
Why faster action may protect the brain and the heart
The human brain and heart can tolerate only short periods of poor blood flow before damage becomes permanent. In emergencies during PCI, every minute spent trying to gain access to blood vessels and connect bulky machines is a minute of low oxygen and unstable circulation. By placing sheaths in advance, medical teams can start support quickly without interrupting chest compressions or juggling extra steps under pressure. The study suggests that this faster response likely explains both the lower death rate and better brain outcomes, even though the same kinds of machines were used in both groups.
What this means going forward
For people facing a very risky heart‑artery procedure, quietly adding an "emergency on‑ramp" to the bloodstream before anything goes wrong may offer a powerful layer of protection. This study found that pre‑inserting vascular sheaths was linked to fewer deaths and less severe brain injury, without a noticeable rise in serious side effects. The work stops short of proving cause and effect—because it was observational, not a randomized trial—and it did not follow patients after they left the hospital. Still, the findings strongly support the idea that planning ahead for the worst, by preparing rapid access to heart‑support machines, can turn a dangerous scramble into a controlled rescue, and may become an important part of care for the sickest heart patients.
Citation: Sun, B., Liu, C., Zhou, M. et al. Preprocedural vascular sheath insertion reduces hospital mortality in high risk PCI patients. Sci Rep 16, 8790 (2026). https://doi.org/10.1038/s41598-026-36613-z
Keywords: high-risk PCI, vascular sheath, mechanical circulatory support, coronary artery disease, in-hospital mortality