Clear Sky Science · en
Body mass index and metabolic dysfunction associated steatotic liver disease remission among Chinese adults in a retrospective cohort study
Why Liver Fat and Body Weight Matter to You
Many people live for years with extra fat in their liver without realizing it. This condition, now called metabolic dysfunction-associated steatotic liver disease (MASLD), is tied to common problems like high blood pressure, diabetes, and high cholesterol. Doctors know that carrying extra body weight raises the risk of MASLD, but far less is known about what helps the liver recover once the disease has started. This study followed thousands of Chinese adults with MASLD to ask a simple but important question: how does body weight affect the chances that fatty liver will actually go away?
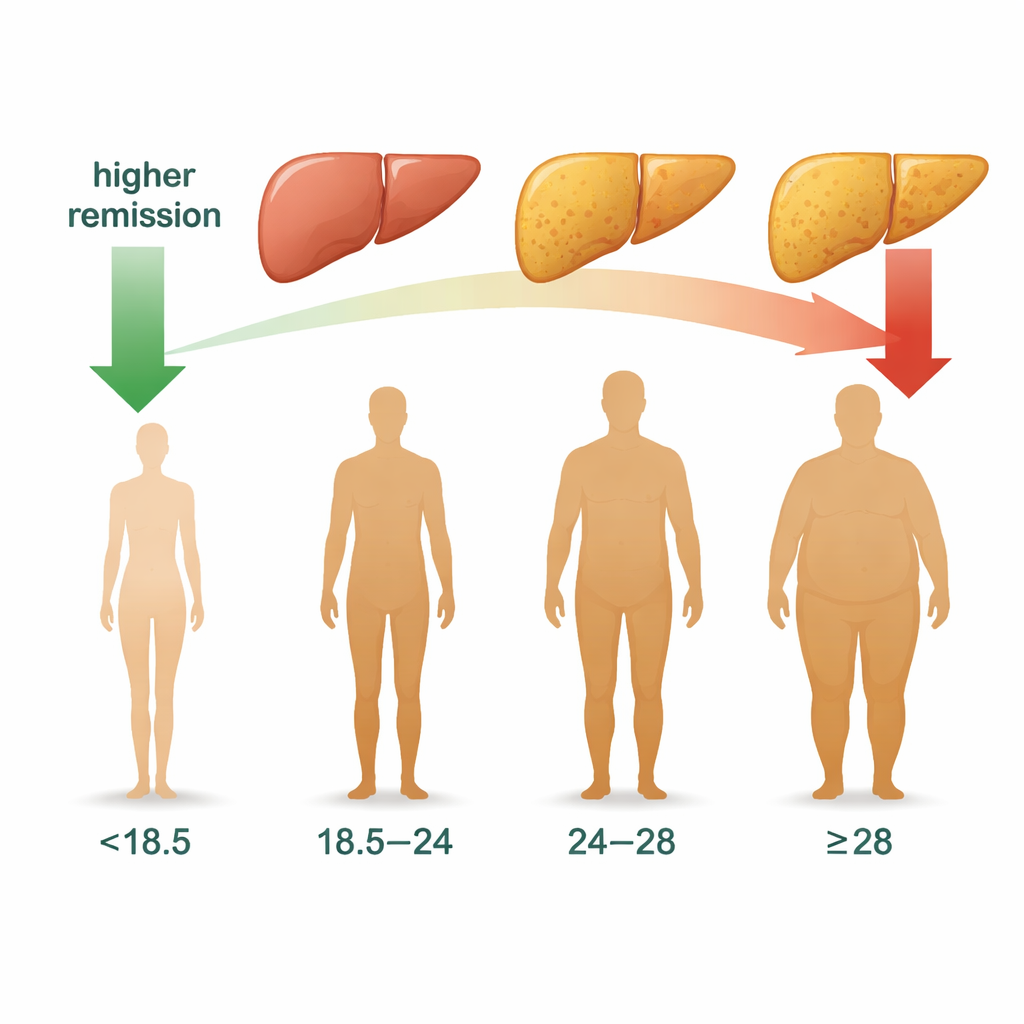
A Common Condition With Real Health Risks
MASLD happens when excess fat builds up in liver cells in people who do not drink heavily but who often have other metabolic issues such as high blood pressure, abnormal blood fats, or elevated blood sugar. It is now one of the most common liver disorders worldwide and can progress from simple fat build-up to inflammation, scarring, and serious liver disease. The encouraging news is that in some people the liver can return to normal, a process called remission. Remission is more than just a nicer-looking scan: past research suggests it lowers the risk of diabetes, high blood pressure, and heart disease. Understanding who is most likely to experience remission can shape advice on lifestyle changes and medical care.
How the Study Was Done
Researchers analyzed records from a health checkup program at a hospital in Shenzhen, China. They focused on 2,890 adults who had MASLD in 2018 and returned for at least one follow-up visit through 2023. Everyone had yearly measurements of height, weight, waist size, blood pressure, blood fats, and blood sugar, as well as liver ultrasound scans. Body mass index (BMI) was used as a standard measure of overall body size, and participants were grouped as underweight, normal weight, overweight, or obese using Chinese guidelines. MASLD remission meant that liver fat disappeared on ultrasound and the person no longer met the criteria for MASLD at follow-up.
What the Researchers Found
Over a median of almost three years, 17% of participants saw their MASLD go into remission. But this average hid big differences by body weight. Underweight people had the highest remission rate, while obese people had the lowest. For every one-unit increase in BMI (for example, from 22 to 23), the chance of remission fell by about 3–4%, even after taking into account age, sex, blood pressure, cholesterol, blood sugar, alcohol use, smoking, physical activity, and several medications. The researchers also found that waist size—an indicator of belly fat—explained nearly 40% of the link between BMI and remission, suggesting that where fat is stored matters as much as how much there is.
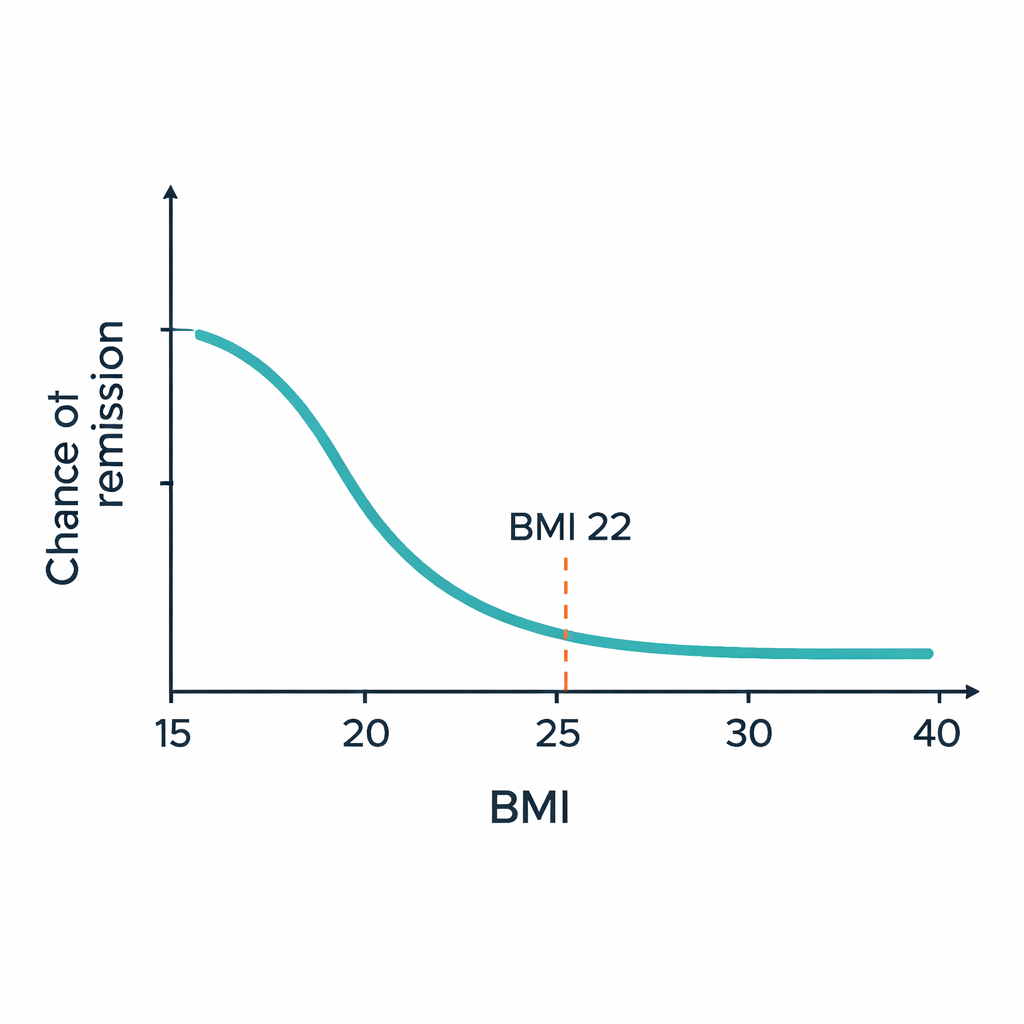
A Hidden Turning Point in Body Weight
When the team looked more closely, the relationship between BMI and liver recovery turned out to be curved rather than straight. Using a statistical method that allows for bends in the line, they identified a key threshold at a BMI of about 22. Below this level, even small increases in BMI were linked to a clear drop in remission chances. Above this level, however, further increases in BMI did not significantly change the odds of getting better—the risk seemed to have already “flattened out.” People with BMI above 22 tended to have higher blood pressure, worse blood fats, higher blood sugar, and more sedentary lifestyles, all of which may blunt the impact of additional weight gain.
What This Means for Everyday Health
For people already living with MASLD, this study suggests that lower body weight—especially less belly fat—gives the liver a better chance to clear out excess fat and recover. The findings highlight BMI around 22 as a rough tipping point: below it, changes in weight appear especially important for liver health, while above it, other metabolic problems may also need aggressive attention. Although this research cannot prove cause and effect and was done in one Chinese hospital, it supports practical advice: healthy eating, more physical activity, and careful management of blood pressure, blood sugar, and blood fats are central to helping fatty livers heal. Future multi-center studies will be needed to confirm these patterns in other populations.
Citation: Zhang, J., Guo, Y., Li, B. et al. Body mass index and metabolic dysfunction associated steatotic liver disease remission among Chinese adults in a retrospective cohort study. Sci Rep 16, 6883 (2026). https://doi.org/10.1038/s41598-026-36612-0
Keywords: fatty liver, body mass index, obesity, metabolic health, liver remission