Clear Sky Science · en
Association between initial diastolic arterial pressure and gastrointestinal dysfunction during the first ICU week in septic shock patients
Why the gut matters in life‑threatening infections
When people land in an intensive care unit with septic shock, doctors fight to keep their blood pressure high enough to protect vital organs. Guidelines focus on a single number called mean arterial pressure, but this may not tell the whole story. This study asks a simple but important question for patients and families: does the lower part of blood pressure – the diastolic value shown in every blood pressure reading – influence how well the gut works, and even who survives, during the dangerous first week in the ICU?
Looking closely at blood pressure and the sickest patients
Researchers analyzed detailed records from nearly a decade of care at a major U.S. hospital, using the large public MIMIC‑IV intensive‑care database. They focused on 1,990 adults with septic shock who stayed in the ICU for at least a week and whose average blood pressure met current safety guidelines (mean arterial pressure of 65 mmHg or higher) during the first 24 hours. Within this group, they grouped patients by their average diastolic pressure: low (<55 mmHg), intermediate (55–65 mmHg), and high (≥65 mmHg). This design allowed them to ask whether differences in the “bottom number” of blood pressure, even when the usual target was met, were linked to problems in the digestive system.
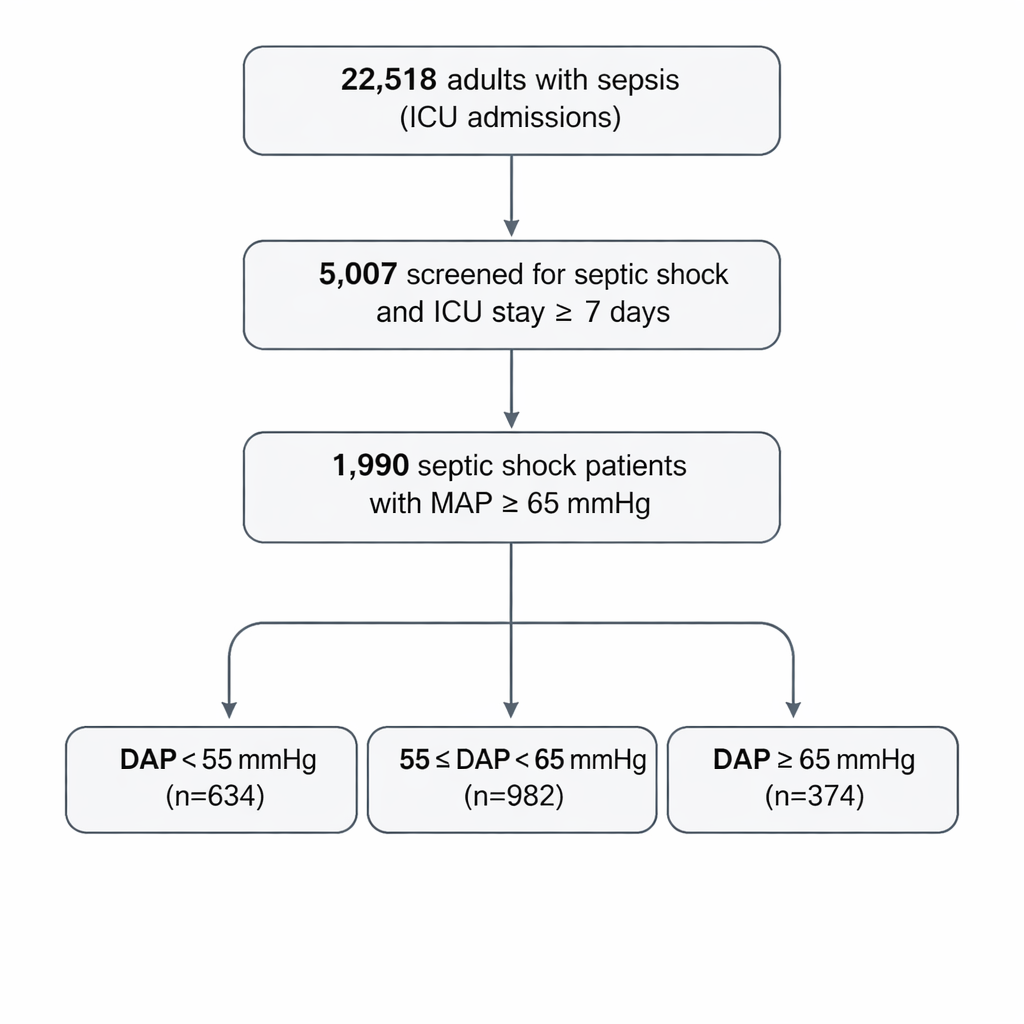
Tracking stomach and bowel trouble day by day
The team then examined how often patients developed gastrointestinal symptoms during their first seven days in the ICU. They looked for signs such as diarrhea, vomiting or regurgitation, a swollen abdomen, poor bowel sounds, large amounts of stomach contents that failed to move along, and bleeding anywhere in the digestive tract. Using bedside records and diagnostic codes, they counted not only whether each symptom appeared, but also how many different symptoms each person experienced. Having three or more distinct gut problems within the week was treated as a marker of serious digestive dysfunction.
Lower diastolic pressure, more gut injury
More than half of all patients had at least three digestive symptoms in that first week, underscoring how fragile the gut is during septic shock. But the burden was not evenly shared. Patients with the lowest diastolic pressures (<55 mmHg) were more likely to suffer from diarrhea and gastrointestinal bleeding, and these problems tended to last longer. In contrast, those whose diastolic pressure stayed at or above 65 mmHg had markedly fewer episodes of diarrhea (about 10% versus over 22% in the low‑pressure group) and less bleeding. Overall, they were less likely to accumulate three or more gut symptoms. When the researchers adjusted for age, other illnesses, and lab results, a diastolic pressure of at least 65 mmHg still appeared to protect against severe digestive problems.
Links to long‑term survival and kidney–gut signals
The differences in early gut health echoed in long‑term outcomes. Over 90 days, patients with very low diastolic pressure had a higher risk of death than those in the intermediate or high ranges, even though short‑term (28‑day) survival looked similar. Another signal came from blood urea nitrogen, a common lab test often used to assess kidney function and hydration. Higher values of this marker were independently tied to a greater chance of having multiple gut symptoms, hinting at a two‑way connection between stressed kidneys, toxin buildup, and a leaky or inflamed intestine in critically ill patients.
What this might mean for patients and care teams
This study does not prove that simply forcing the diastolic pressure higher will cure gut problems, and the authors caution against blindly raising drug doses to chase a number. Very strong blood‑vessel tightening can itself starve the gut of blood and strain the heart. Instead, their findings suggest that a low diastolic pressure should act as an early warning sign that the gut may be at risk, even when standard blood pressure goals appear to be met. In everyday terms, paying attention to the “bottom number” on the monitor could help ICU teams fine‑tune fluids, medications, and nutrition to better protect the digestive system – and possibly improve survival – in people battling septic shock.
Citation: Wang, Q., Zhang, G. Association between initial diastolic arterial pressure and gastrointestinal dysfunction during the first ICU week in septic shock patients. Sci Rep 16, 5649 (2026). https://doi.org/10.1038/s41598-026-36591-2
Keywords: septic shock, blood pressure, diastolic pressure, gut dysfunction, intensive care