Clear Sky Science · en
Patient-environment monitoring for smart healthcare in hospitals with cooperative power-data transfer
Why powering tiny hospital sensors matters
Modern hospitals increasingly rely on tiny wireless sensors to track patients’ vital signs and room conditions around the clock. These unobtrusive devices can spot early warning signs of trouble and help staff keep wards comfortable and safe. But there is a hidden weak link: most sensors run on small batteries. When those batteries run low, monitoring can quietly fail, and crucial health information may be lost. This paper explores how to keep such sensors running reliably by sending them power through the air and helping them pass their data along more efficiently.
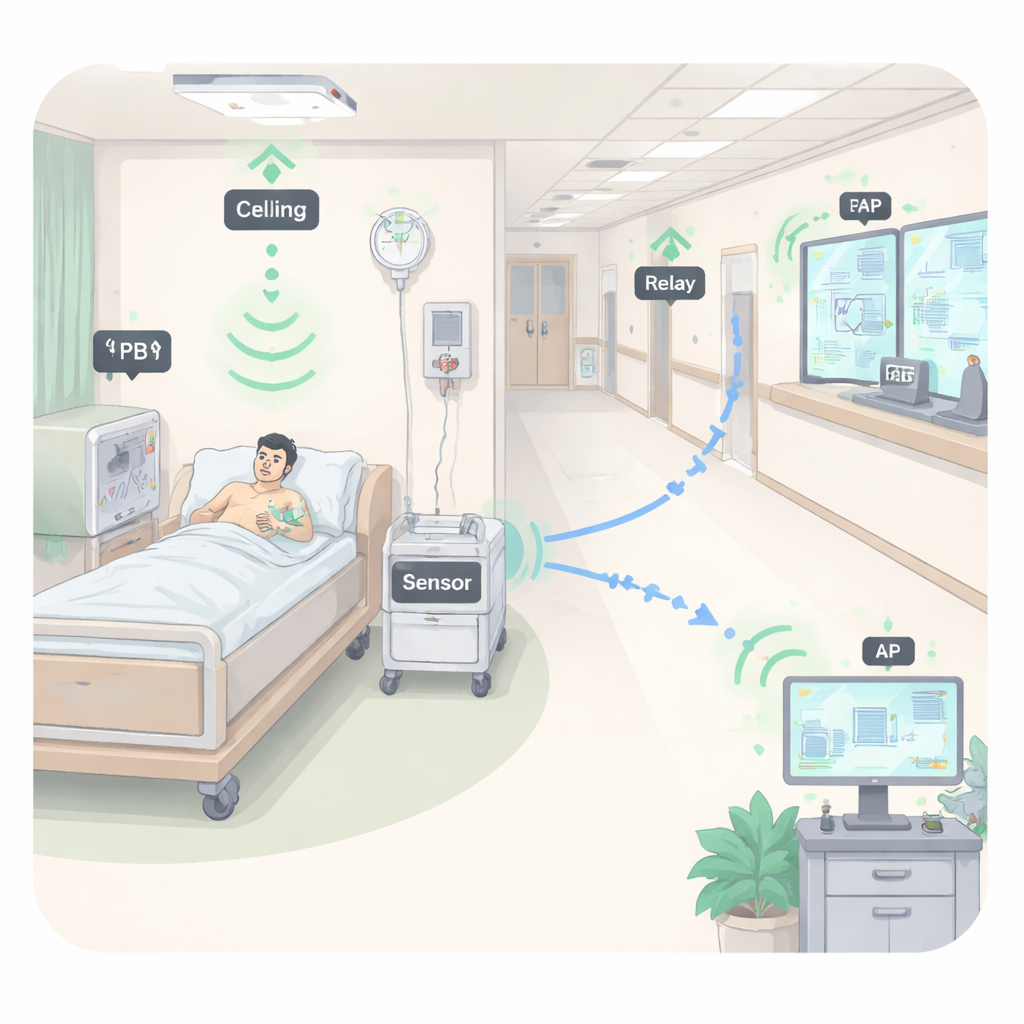
Hospitals filled with silent helpers
In smart healthcare systems, sensors may be worn on the body, implanted under the skin, or placed around beds and hallways. They continuously measure heart rate, breathing, motion, temperature, humidity, and other signals. Readings are sent wirelessly to access points, which forward them to hospital servers for analysis. If something looks wrong—a dangerous heart rhythm, a fall, or a sudden drop in room oxygen—the system can alert nurses immediately. When many sensors are scattered through a ward, however, routinely replacing or recharging batteries is impractical. If a sensor dies unnoticed, the monitoring gap can put patients at risk. The authors focus on how to make these networks “energy-sustainable” so they can run for long periods without human intervention.
Sending power through the air
Instead of relying solely on batteries, the study considers wireless power transfer: special devices called power beacons send out radio-frequency energy that nearby sensors harvest and convert into electricity. In a hospital, these beacons might be ceiling panels, bedside monitors, nursing carts, or even Wi‑Fi access points repurposed to add power signals. The sensor first spends part of each time cycle charging itself from the strongest available beacon. Then it uses the harvested energy to send its data. The authors use a realistic model of the charging electronics that captures how such circuits behave nonlinearly—they do not simply double the output when the incoming signal doubles, and they eventually saturate. This modeling helps predict how much useful power a sensor can expect under different conditions.
Getting a helping hand from relay nodes
Simply powering the sensor is not enough if it must send data over a long, weak radio path to a distant access point. To address this, the paper introduces relay nodes: devices with stable power supplies placed between the sensor and the access point. The sensor sends its data over a short hop to one relay, which then forwards it on. Shorter hops require less transmit power and are more robust to signal fading inside buildings. The researchers compare two ways of choosing relays. In the “best relay” strategy, the network quickly checks which relay offers the strongest overall path and uses that one. In the “random relay” strategy, a helper is chosen without channel measurements, which is simpler but less effective. They pair each relay strategy with either the best or a random power beacon choice, creating four combinations to test.
Finding the sweet spot for time and placement
Using a mix of mathematical analysis and large computer simulations, the authors study how often the system fails to deliver data—its outage probability—under different settings. They vary how much time in each cycle is spent charging versus sending data, how the time is split between the sensor and the relay, how many beacons and relays exist, and where the relays are placed along the line between the sensor and the access point. The results reveal clear trade-offs: giving too much time to charging leaves too little for sending data, while too little charging starves the sensor of energy. There is an optimal middle ground. Adding more power beacons helps only if the system actually chooses the best one; random choice sees little benefit. By contrast, adding more relays greatly improves reliability when the best relay is selected, but barely changes performance if relays are picked at random.
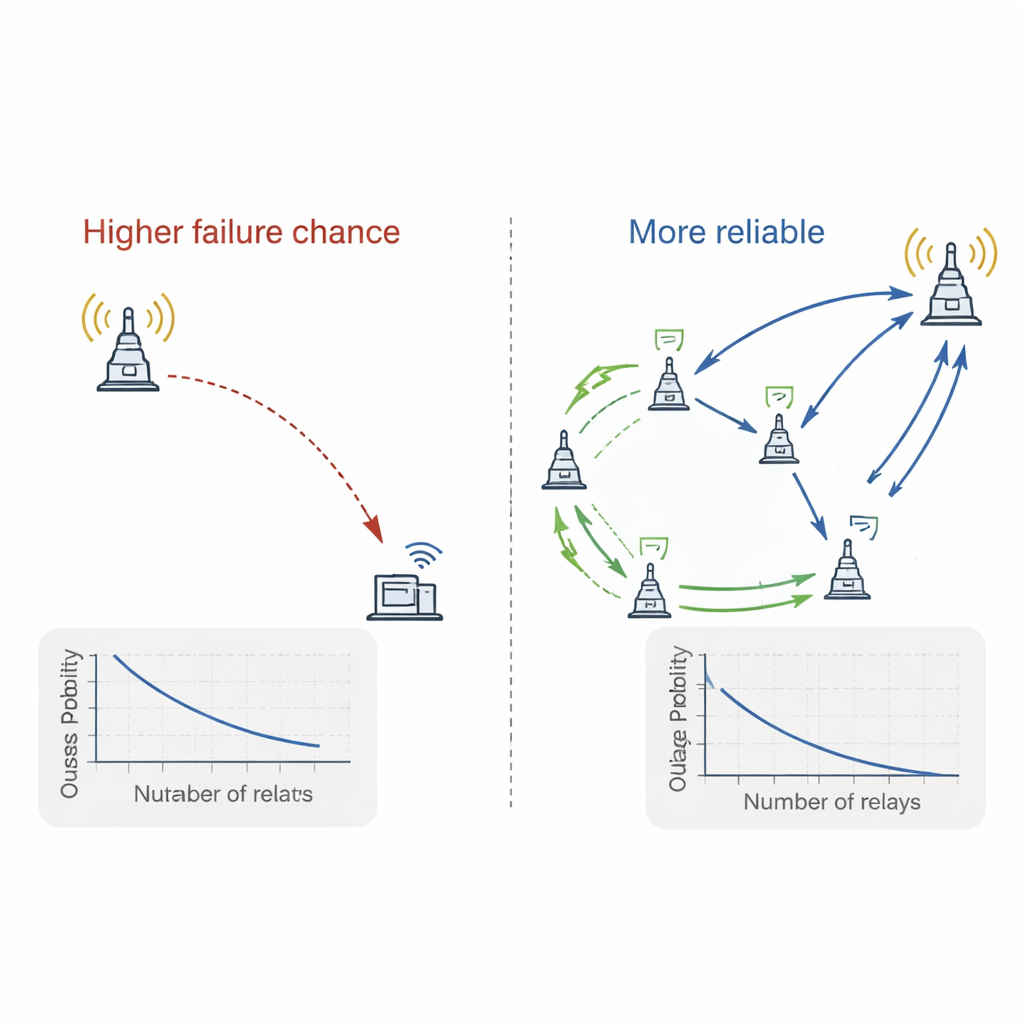
What this means for future smart hospitals
The key takeaway in everyday terms is that to build dependable, battery-light monitoring in hospitals, it is more important to choose a good helper device to pass along data than to obsess over which charger to use. Carefully placing and selecting relay nodes can sharply reduce the chances that a health reading is lost, while smart use of wireless power keeps sensors running without constant battery swaps. With these ideas, hospitals could move toward always-on, low-maintenance monitoring that quietly watches over patients, flags problems early, and supports more personalized, preventive care without adding to staff workload.
Citation: Li, J., Zhai, C. Patient-environment monitoring for smart healthcare in hospitals with cooperative power-data transfer. Sci Rep 16, 5794 (2026). https://doi.org/10.1038/s41598-026-36580-5
Keywords: smart healthcare, wireless power transfer, patient monitoring, sensor networks, hospital Internet of Things