Clear Sky Science · en
Glymphatic system impairment in type II diabetes mellitus adults
Why brain “cleaning” matters in diabetes
Type 2 diabetes is usually discussed in terms of blood sugar and heart health, but it also quietly affects the brain. Many people with diabetes report poor sleep and subtle thinking problems years before any diagnosis of dementia. This study asks a timely question: does diabetes interfere with the brain’s own “night shift” cleaning crew—the system that washes away waste while we sleep—and could that help explain higher risks of memory loss and Alzheimer’s disease in these patients?
The brain’s overnight wash cycle
Over the past decade, researchers have identified a network of tiny channels that move fluid through the brain, rinsing out toxic by-products such as amyloid and tau proteins that are linked to Alzheimer’s disease. This network, nicknamed the glymphatic system, is most active during deep, restful sleep. In animals, aging, high blood pressure, and metabolic problems can all slow this cleaning flow. Yet, until now, no one had directly examined how this system behaves in adults living with type 2 diabetes, even though they often struggle with disturbed sleep and face higher risks of cognitive decline.
Peering into the brain’s drainage pipes
To probe this hidden plumbing, the researchers recruited 78 adults with type 2 diabetes and 106 similar adults without diabetes. Everyone completed detailed questionnaires about sleep quality and daytime sleepiness and took a brief but comprehensive thinking test called the Montreal Cognitive Assessment. They then underwent advanced MRI scans. From these scans, the team calculated a measure called the DTI-ALPS index, which tracks how water moves along small spaces surrounding blood vessels—key highways for the brain’s waste-carrying fluid. Although indirect, this index has been repeatedly linked to how well the glymphatic system is working.
Diabetes, poorer sleep, and a sluggish brain rinse
Compared with healthy volunteers, adults with diabetes slept worse and felt sleepier during the day. They reported more sleep disturbances, lower sleep efficiency, and more daytime dysfunction. On the thinking test, the diabetes group scored lower overall, with clear weaknesses in visuospatial skills, attention, and language, even though many still tested above the usual dementia threshold. Crucially, their DTI-ALPS values were significantly reduced, pointing to impaired brain waste clearance. Subtle changes in how water diffused through key fiber pathways in the brain accompanied these lower scores, hinting at early microscopic tissue changes. These differences persisted even after accounting for age, sex, body weight, sleepiness, and thinking-test performance.
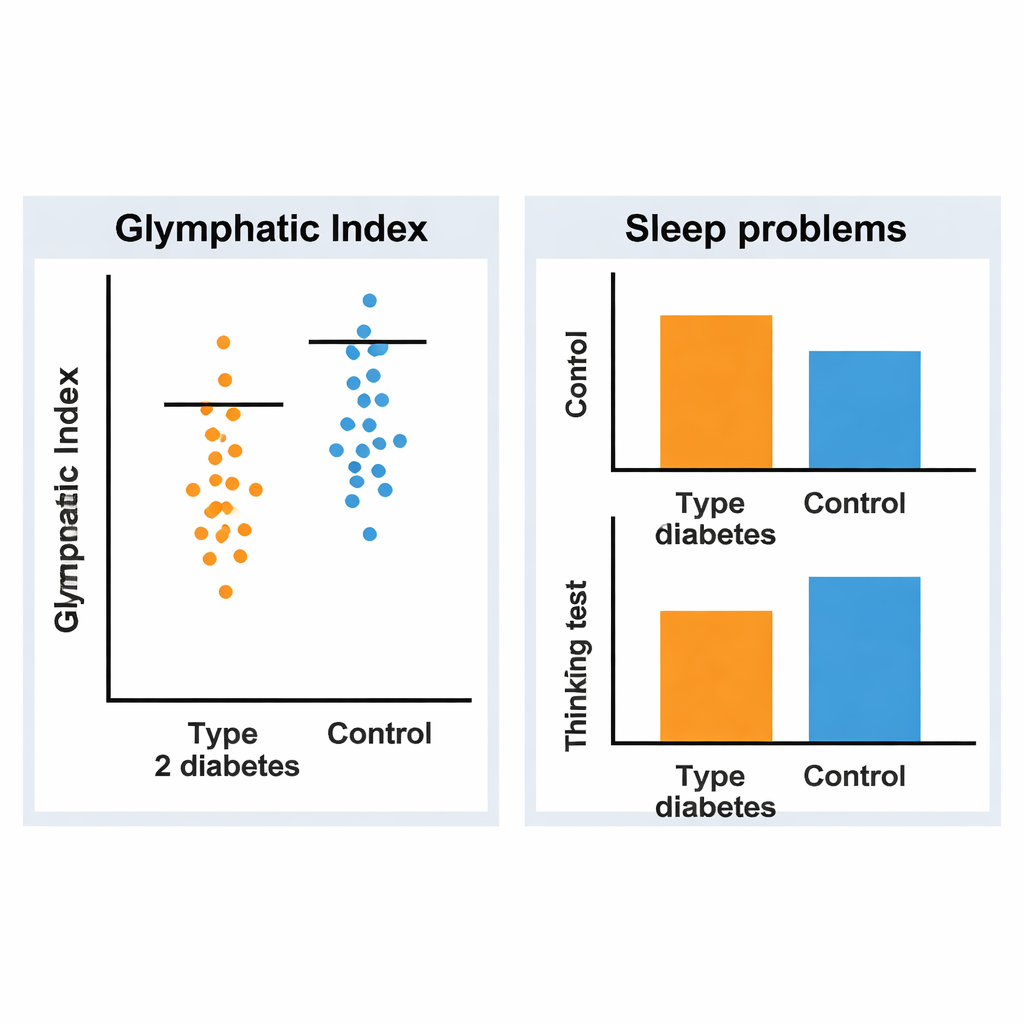
A complex tangle of metabolism, sleep, and memory
Interestingly, within the diabetes group, the strength of the brain-cleaning measure did not line up neatly with how bad someone’s sleep complaints or blood sugar readings were. That suggests the problem is not driven by any single factor. Instead, long-term high blood sugar, low-grade inflammation, subtle blood vessel damage, and disturbed sleep may together burden the glymphatic system and brain tissue. The authors point to animal work showing that diabetes can weaken water channels that help push fluid through the brain and to other studies linking diabetes with heightened brain inflammation. All of these processes could slow waste clearance and set the stage for neurodegeneration.
What this means for people with diabetes
For a lay reader, the takeaway is both sobering and hopeful. The study provides imaging evidence that, even before dementia appears, adults with type 2 diabetes may already have a less efficient brain “cleaning” system, worse sleep, and early thinking changes. This combination could help explain why diabetes raises the risk of Alzheimer’s disease. At the same time, the findings highlight new opportunities. Because the glymphatic system is most active during good-quality sleep, strategies that improve sleep—such as cognitive-behavioral therapy, healthier routines, treatment of sleep apnea, and careful management of diabetes-related risk factors—may help protect the brain. Future research will need to test whether targeting this hidden cleaning network can slow or prevent memory decline in people living with type 2 diabetes.
Citation: Roy, B., Lubera, V., Singh, K.R. et al. Glymphatic system impairment in type II diabetes mellitus adults. Sci Rep 16, 7286 (2026). https://doi.org/10.1038/s41598-026-36573-4
Keywords: type 2 diabetes, brain waste clearance, sleep and cognition, glymphatic system, Alzheimer’s risk