Clear Sky Science · en
Differential sensitivity of impedance plethysmography and photoplethysmography sensors to temperature-induced peripheral vasoconstriction
Why cooling your wrist matters to wearable tech
Many of us rely on smartwatches and fitness bands to track our heart and health. But what happens to these sensors when your hands get really cold, like when you hold an ice pack or walk on a winter day? This study explores how two common ways of measuring blood flow in the body respond to cold: an electrical method used in research tools and an optical method used in most wearables. Understanding their differences could lead to smarter, more reliable health trackers that work well in everyday conditions.
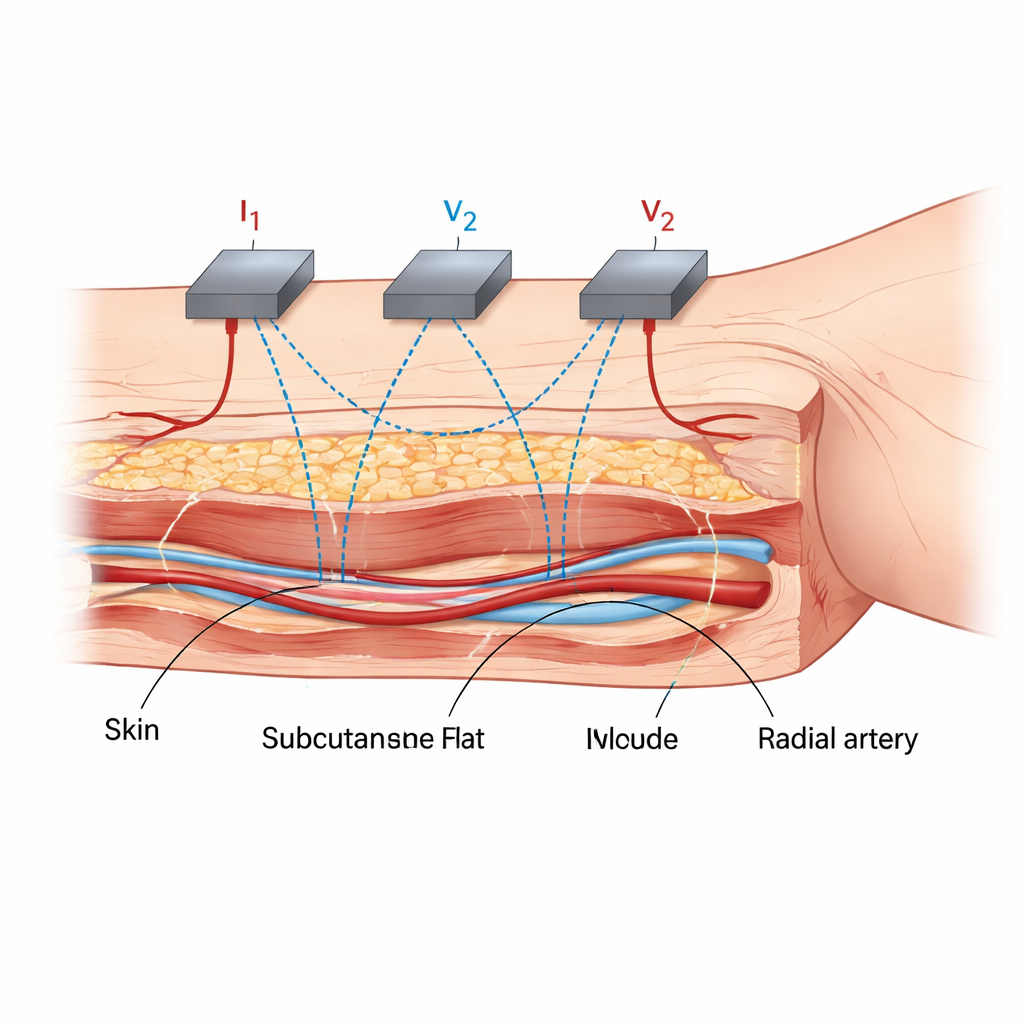
Two different ways to listen to your pulse
The researchers focused on two non-invasive sensing methods. One, called photoplethysmography, shines light into the skin and measures how the returning light changes with each heartbeat; this is the basis of the green or infrared LEDs you see blinking on the underside of many watches. The other, impedance plethysmography, sends a tiny, harmless electrical current through the arm using four skin electrodes and tracks how the electrical resistance changes as blood moves. While the light-based sensor is known to be very sensitive to shallow blood vessels near the surface, the electrical method is thought to pick up signals from deeper structures, but this has not been well tested in humans.
Putting ice to work as a natural test
To probe how deeply each sensor “looks” into the body, the team used a simple but powerful trick: cold. When skin is cooled, small vessels near the surface tighten, or constrict, which sharply reduces blood flow in those upper layers without necessarily changing blood pressure in the larger arteries. Twenty-one adult volunteers visited the lab and wore both types of sensors on the same spot over the radial artery in the forearm. On one trial, fake ice cubes were placed over a towel on their arm to mimic weight and pressure without cooling. On another, real ice cubes were used to create a strong drop in skin temperature while the volunteers stayed still and relaxed.
What changed in the signals—and what did not
The cold stimulus did exactly what it was supposed to do: it cooled the skin above the sensors by more than 13 degrees Celsius on average, while blood pressure remained stable and heart rate slowed slightly as people relaxed. The light-based sensor showed a clear effect of this cooling. Its pulse signal dropped by about 40 percent in size, meaning the light detected much less of the usual rise and fall in superficial blood volume. In contrast, the electrical sensor’s pulse signal stayed almost the same before and after cooling. Detailed timing features—such as how long it took the pulse wave to travel from the heart’s electrical beat to the wrist—also stayed largely unchanged in both sensors, matching the observation that overall blood pressure did not shift.
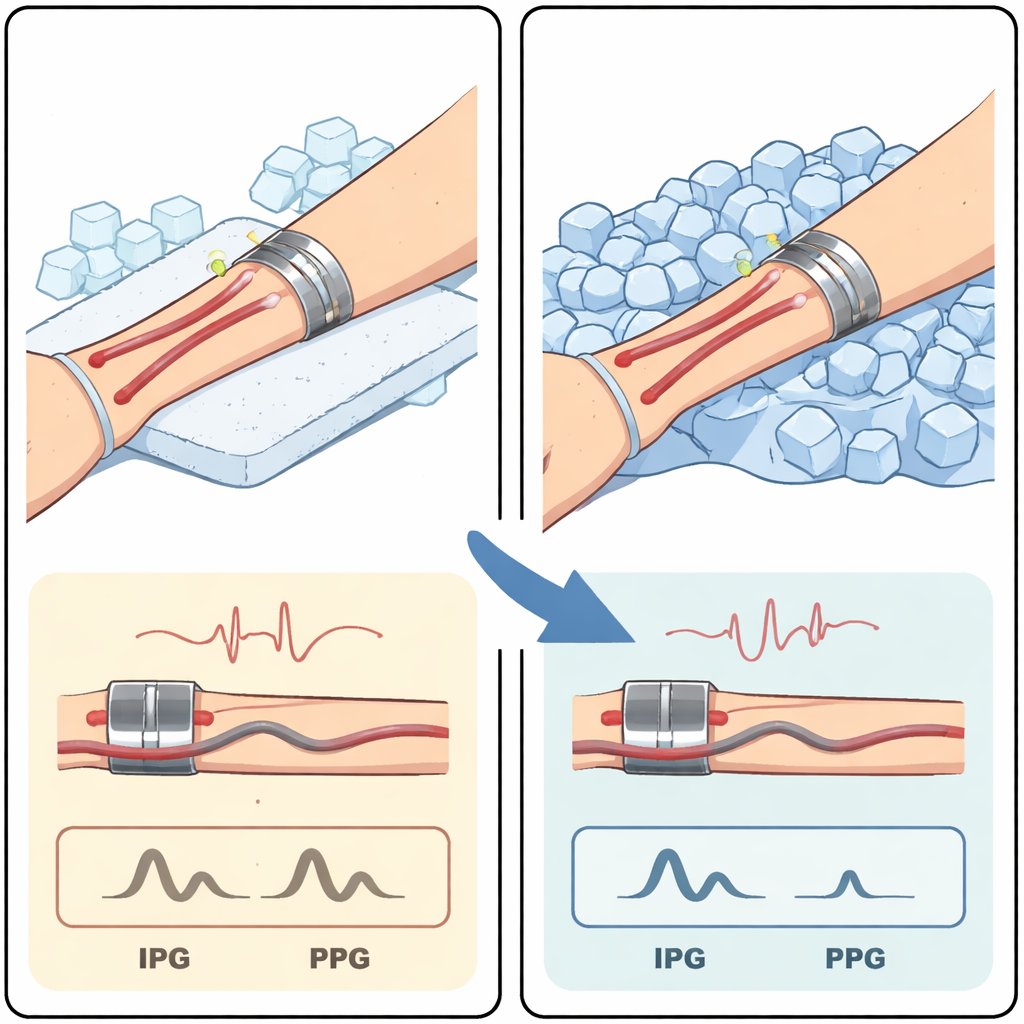
Clues about where these sensors are looking
The opposite reactions of the two sensors to cold offer an important clue. If the electrical method were mainly sensing the same shallow vessels as the light-based one, its signal should have shrunk when those vessels constricted. Instead, it remained steady, even while the optical signal dropped. This strongly suggests that the electrical measurements are influenced more by deeper blood vessels, such as the radial artery under the skin, which are less affected by brief local cooling. Previous computer simulations of current flow in the forearm support this idea, showing that much of the electrical path passes through deeper tissues rather than just the thin layer of capillaries at the surface.
What this means for future wearables
For non-experts, the bottom line is that not all pulse sensors on the body are seeing the same thing. Light-based sensors are excellent for tracking changes in shallow blood flow but can be thrown off when the skin gets cold or blood vessels tighten. Electrical sensors, on the other hand, seem to stay steady under those same conditions, hinting that they may be better suited to monitoring deeper blood flow and heart-related activity. Combining both approaches in future wearable devices could make them more robust in everyday life, allowing your watch or band to keep delivering accurate insights about your heart and circulation whether your hands are warm, cold, or somewhere in between.
Citation: Jung, S., Thomson, S., Pantelopoulos, A. et al. Differential sensitivity of impedance plethysmography and photoplethysmography sensors to temperature-induced peripheral vasoconstriction. Sci Rep 16, 6828 (2026). https://doi.org/10.1038/s41598-026-36563-6
Keywords: wearable sensors, blood flow, cold exposure, pulse monitoring, smartwatch accuracy