Clear Sky Science · en
Unique perspectives about men’s awareness of BRCA1/2 genetic testing in primary care
Why this matters for you and your family
Many people have heard of the “breast cancer genes” BRCA1 and BRCA2, but they are often thought of as a women’s issue. This study shows that men can carry these same genes, face higher risks of cancers such as prostate and colon cancer, and yet often remain in the dark about their own risk. Understanding how much men know—and don’t know—about these genes and cancer screening can help improve early detection, protect families, and potentially save lives.
Hidden genes, hidden risks
BRCA1 and BRCA2 are inherited genes that can run silently through families, passed down equally from mothers or fathers to sons and daughters. When a person carries a harmful change in one of these genes, their chances of developing certain cancers rise—but so do their chances of catching cancer early if they are screened. While women with BRCA mutations are often linked to breast and ovarian cancer, men who carry these genes are at higher risk for prostate, colon, and even male breast cancer. Despite this, men are tested far less often than women, and their family histories—especially on the father’s side—are not always carefully recorded.
What the researchers set out to learn
The researchers surveyed 234 Jewish and Muslim men in Israel who had never had cancer and did not know if they carried a BRCA1/2 mutation. They wanted to understand four things: whether the men knew anything about BRCA1/2; how serious they believed cancer to be; how likely they thought men in general—and they themselves—were to develop prostate or colon cancer; and where they usually got their health information. The men completed questionnaires available in English, Hebrew, or Arabic, and the answers were analyzed to see how background factors like age, religion, and education were linked to awareness of BRCA.
Big fears about cancer, but low sense of personal risk
The survey revealed a striking disconnect. Nearly seven in ten men reported having a family history of cancer, and almost all (over 90%) said cancer is a serious or very serious disease. Yet when asked specifically about prostate cancer, just over half thought men in general faced a high risk, while only about one in five felt that they personally were at high risk. A similar gap appeared for colon cancer. This pattern suggests that many men can recognize cancer as a major public health problem, but still believe “it is unlikely to happen to me,” a mindset that can delay screening or testing even when there is family history.
Low awareness of BRCA and who knows more
Knowledge about BRCA1/2 itself was even more limited. More than half of the men—58%—said they did not know what BRCA1/2 was at all, so they could not say whether anyone in their family carried these genes. When the researchers grouped men who answered “yes” or “no” about family BRCA history into a single “I know what BRCA is” category, they found that education level was the only factor strongly tied to awareness. Men with more years of schooling were more likely to say they knew about BRCA, but even in this relatively well-educated sample, overall awareness was still low. Other factors, such as age, religion, and how religious they were, did not significantly change whether men knew about BRCA.
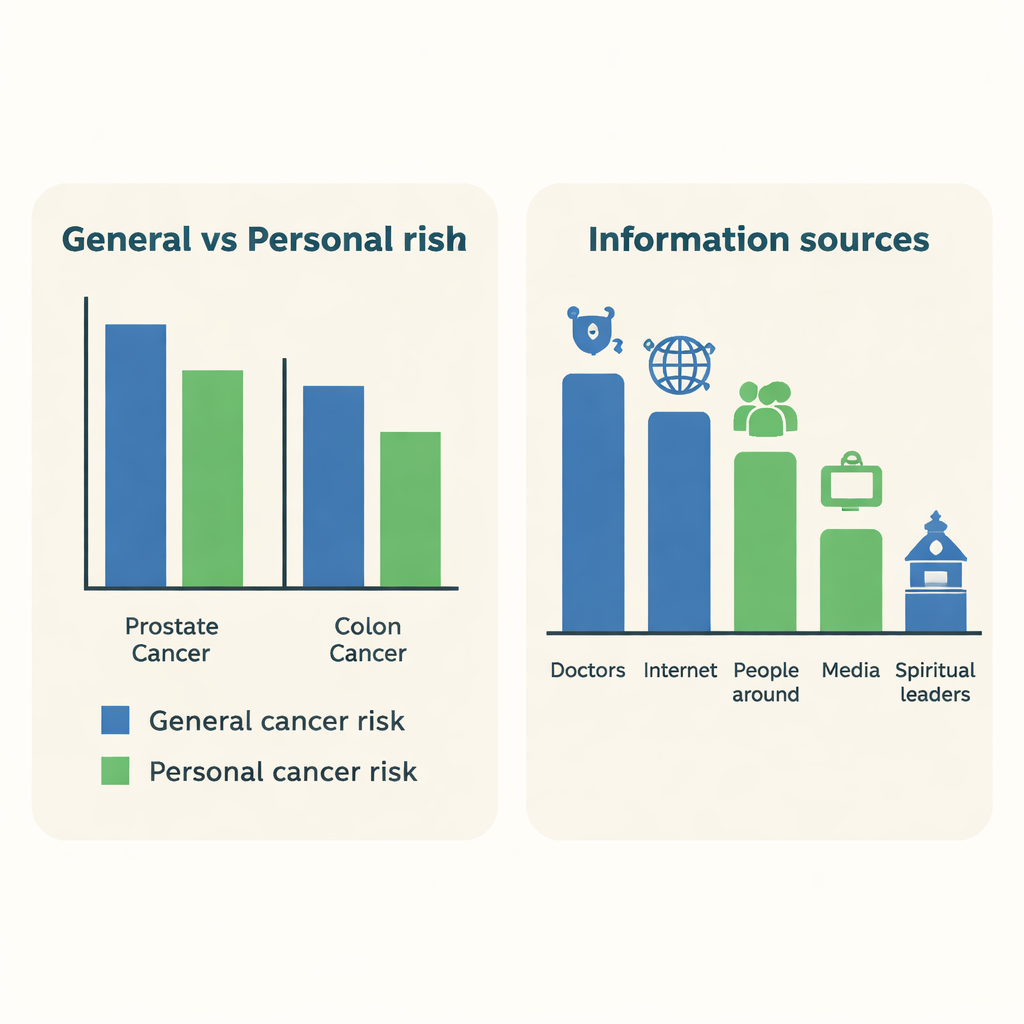
Who men listen to about health
The men were also asked where they turn for information about cancer. An overwhelming 97% said they were likely or very likely to trust doctors, nurses, and other health professionals. The internet and people around them—such as friends and family—were also common sources, while radio, television, and newspapers were used to a lesser degree. Spiritual leaders, despite nearly half the sample describing themselves as religious, were the least used source for cancer information. These patterns send a clear message: for most men, primary care providers are the main gateway to learning about cancer risk and genetic testing.
What this means for everyday care
The findings point to a major missed opportunity. Men rely heavily on their primary care clinicians, yet many do not understand that genes like BRCA1/2 can affect them or their children. At the same time, existing guidelines and practice have historically focused more on women’s cancer risks, leaving men under-tested and under-informed. The authors argue that primary care providers should routinely ask about both maternal and paternal cancer histories, consider hereditary risks for men as well as women, and refer at-risk patients for genetic counseling and testing when needed.
Takeaway for men and families
For a layperson, the message is simple: cancer-related genes are not just a women’s issue, and they can quietly pass through fathers as well as mothers. Many men in this study did not know what BRCA1/2 was or how it might affect their own cancer risk or that of their children. Because men overwhelmingly trust their doctors for health information, primary care visits are a crucial moment to ask about family cancer history and talk about genetic testing. By recognizing that men can be important carriers of hereditary risk, families can move from unknowing to proactive screening and earlier, potentially life-saving care.
Citation: Andrews, C.S., Ibrahim, I., Baruch, Y.B. et al. Unique perspectives about men’s awareness of BRCA1/2 genetic testing in primary care. Sci Rep 16, 5892 (2026). https://doi.org/10.1038/s41598-026-36554-7
Keywords: BRCA genes, men’s cancer risk, genetic testing, prostate cancer, primary care