Clear Sky Science · en
AI–assisted multimodal assessment for right ventricular function from echocardiography predicts mortality in patients with pulmonary hypertension and right heart failure
Why this matters for patients and families
Pulmonary hypertension and right-sided heart failure are often silent until they become life-threatening. Doctors can look at ultrasound images of the heart, but subtle early damage to the right ventricle is easy to miss and difficult to measure. This study shows how an artificial intelligence (AI) system can read these heart scans in more detail than a human can alone, helping doctors estimate a patient’s risk of dying in the hospital and over the next few years—and potentially intervene sooner.
A closer look at a stressed right heart
When pressure in the lung circulation stays high, the right side of the heart must pump against extra resistance. Over time, the right ventricle stretches, its muscle fibers weaken, and patients develop swelling, breathlessness, and low blood pressure. Standard echocardiography—the familiar heart ultrasound—can measure simple movements, such as how far a valve ring travels as the heart beats. But the right ventricle has a complex shape and does not squeeze uniformly, so these traditional measurements can miss early or patchy damage, especially in very sick patients.
Measuring how the heart muscle deforms
Modern ultrasound software can track tiny speckle patterns in the muscle wall from frame to frame, calculating how much each region shortens and lengthens with every heartbeat. This measure, called longitudinal strain, is especially important for the right ventricle. In this study, doctors focused on an average strain value taken from six standard segments of the right ventricle wall. Less negative numbers (meaning less shortening) reflect weaker muscle function. Among 586 adults hospitalized with pulmonary hypertension and right-sided heart failure, those who died had clearly worse strain values and higher pressures in the lung artery than survivors, confirming that this detailed motion measure captures real biological risk.
Teaching an AI to read the heart
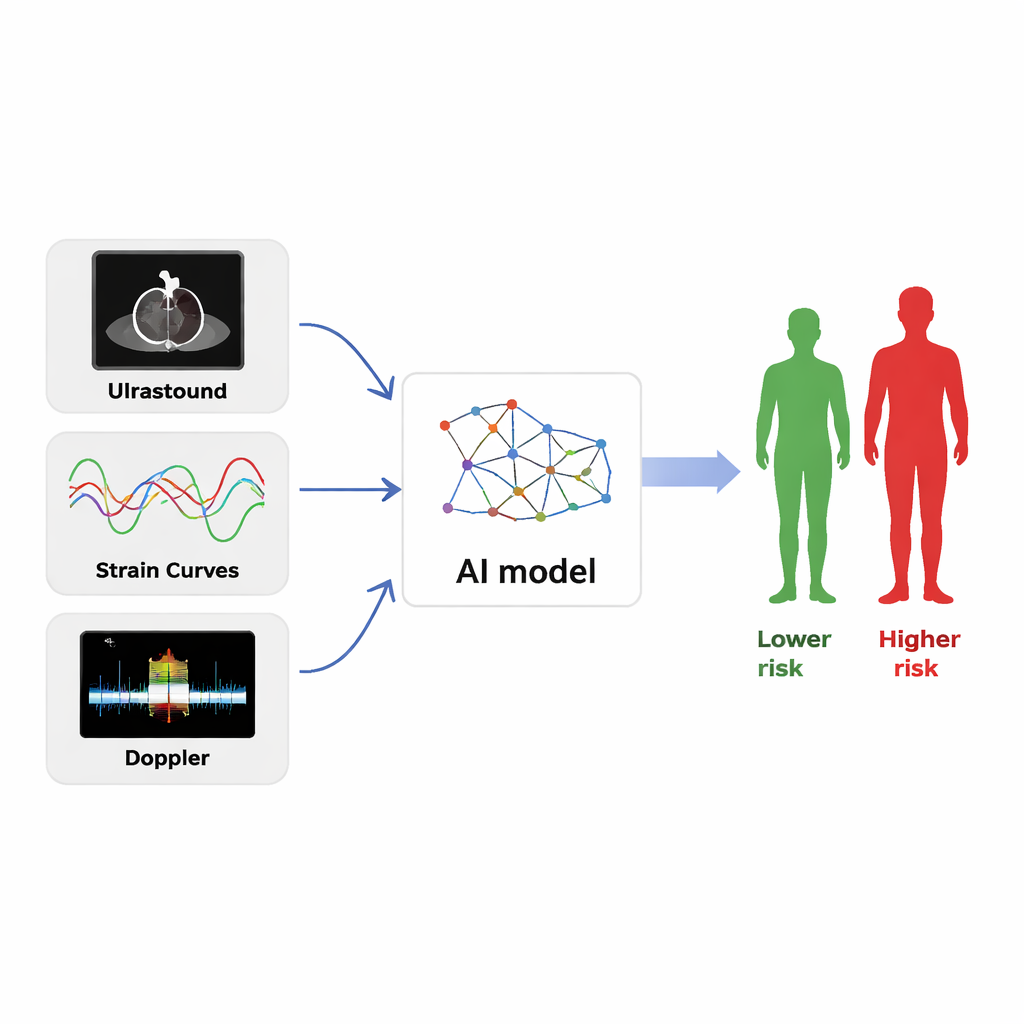
The research team built a deep-learning model that did not rely on a single number or image type. Instead, it analyzed three streams of information drawn from one heartbeat: the full strain curves over time, ultrasound video clips from two viewing angles, and Doppler traces that show the speed and direction of blood flow. Each stream was processed by its own specialized encoder, and a "cross-attention" module then taught the AI to align motion, structure, and flow patterns that belonged together. Clinical data and conventional ultrasound measurements were included as well. The system’s task was straightforward: for each patient, output the probability of death in the hospital and during long-term follow-up.
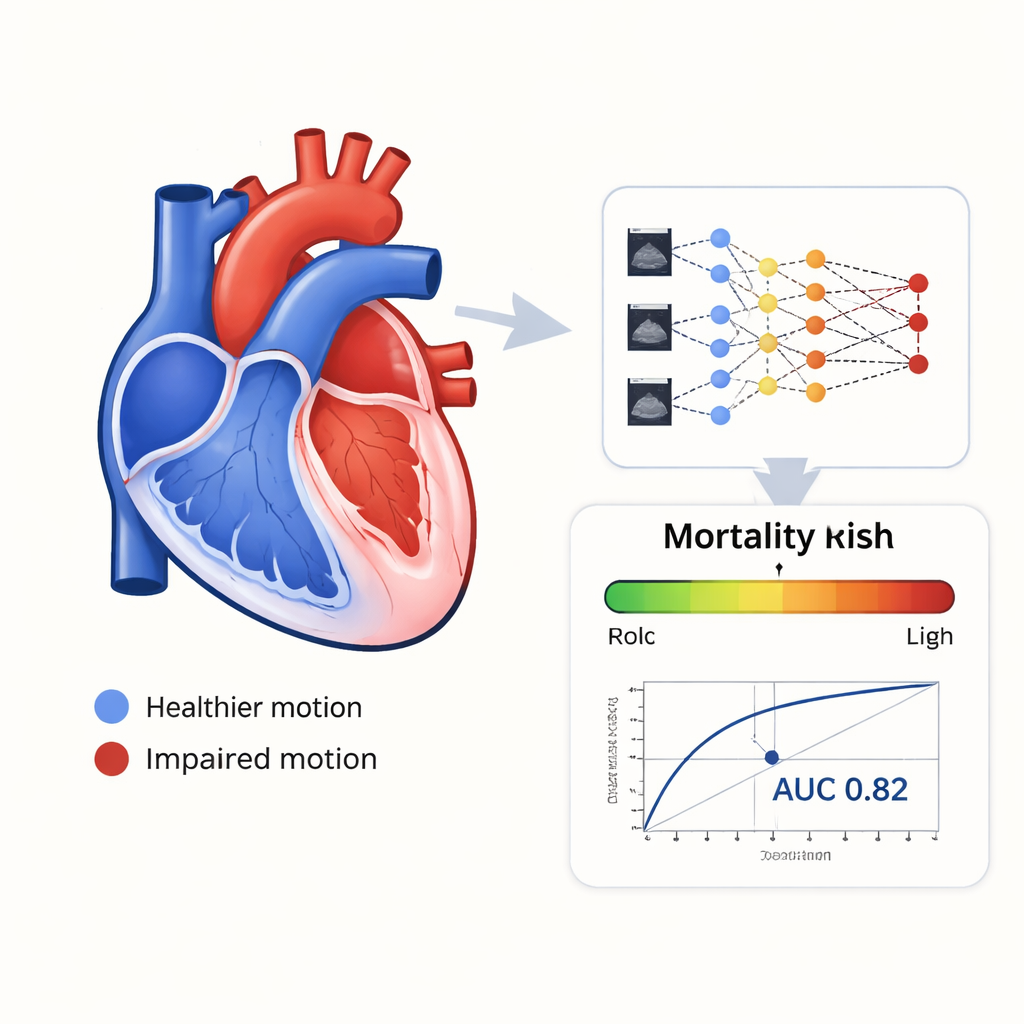
How well the AI predicted outcomes
The patients were randomly split into training, validation, and testing groups so that final performance could be checked on data the AI had never seen before. In the independent test set, the model reached an area under the receiver operating characteristic curve (AUC) of 0.823, meaning it correctly ranked higher-risk and lower-risk patients more than 8 times out of 10. It outperformed individual standard measurements, including lung artery pressure and average right ventricular strain when used alone. The AI system was also fast: it could analyze the necessary ultrasound information in about four minutes, compared with roughly twenty minutes for a sonographer to perform and interpret strain analysis manually.
What this could mean for care
For a patient lying in an intensive care bed with advanced pulmonary hypertension, knowing whether their right heart is failing quietly or holding steady can change treatment choices—such as when to intensify medications, consider advanced therapies, or plan closer follow-up. This study suggests that an AI assistant, plugged into routine heart ultrasound, can deliver a more precise and timely risk estimate than standard measures alone. While the approach still needs testing in other hospitals and with different ultrasound machines, it points toward a future in which detailed, automated analysis of heart motion helps doctors tailor care and potentially improve survival for people with severe right-sided heart disease.
Citation: Mou, H., Zhang, G., Xiu, L. et al. AI–assisted multimodal assessment for right ventricular function from echocardiography predicts mortality in patients with pulmonary hypertension and right heart failure. Sci Rep 16, 5323 (2026). https://doi.org/10.1038/s41598-026-36533-y
Keywords: pulmonary hypertension, right heart failure, echocardiography, artificial intelligence, risk prediction