Clear Sky Science · en
A multimodal retinal aging clock for biological age prediction and systemic health assessment via OCT and fundus imaging
Why the Eyes Can Reveal More Than Meets the Eye
The tiny blood vessels and nerve fibers at the back of the eye are among the few parts of the body where doctors can directly see living tissue. This study asks a provocative question: can routine eye scans reveal how “old” the body truly is—its biological age—and even hint at a person’s overall disease burden and risk of death more accurately than the number of candles on their last birthday cake?
Looking at Biological Age, Not Just Birthdays
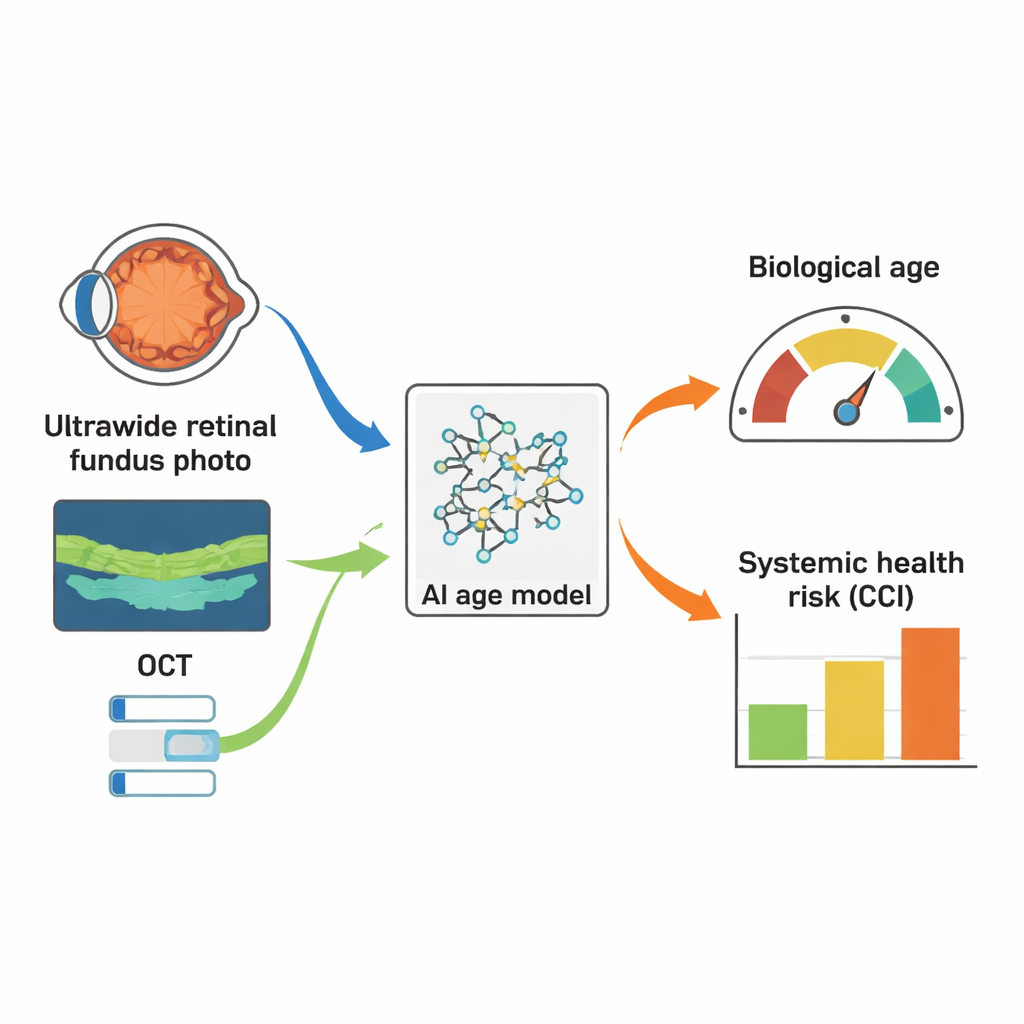
Chronological age is simply how long we have lived. Biological age reflects how worn or preserved our organs and tissues are. Two people who are 65 years old may have very different health outlooks, depending on how quickly their bodies have aged. Traditional biological clocks rely on blood tests that measure DNA or proteins, which can be costly and invasive. The authors explored a simpler alternative: using two common eye imaging tests—ultrawide-field fundus photographs and optical coherence tomography (OCT)—combined with artificial intelligence (AI) to estimate biological age from the retina, a window into the body’s vascular, nerve, and metabolic health.
Teaching an AI to Read Age in the Retina
The team trained a deep learning model on over 12,000 fundus images and 7,700 OCT scans from 2,467 patients. In the first experiment, the AI “age clock” was trained only on eyes without major structural disease and then tested on both healthy and diseased eyes. In the second experiment, the model was retrained on a broader mix of eyes, including four common conditions that deform the retina: age-related macular degeneration, diabetic retinopathy, epiretinal membrane, and pathologic or high myopia. In this second round, the AI also received each eye’s disease label. In both setups, the model’s goal was to predict age from images; the researchers then treated this predicted age as a biological age and asked how well it tracked overall illness.
Eye Age vs. Whole-Body Disease Burden
To link retinal age to general health, the authors used the Charlson Comorbidity Index (CCI), a widely used score that sums up a person’s serious long-term diseases and predicts their one-year risk of death. They compared how well chronological age versus AI-derived biological age correlated with CCI, and also built simple statistical models to see which better predicted CCI. Across both experiments, biological age from the retinal images generally captured comorbidity burden more strongly than chronological age, especially in eyes with structural disease. When disease labels were added in the second study, the model’s accuracy improved substantially: its average age error in the test set dropped to about six years, and biological age still tended to outperform birthdays for reflecting overall illness, particularly in patients whose retinas were visibly abnormal.
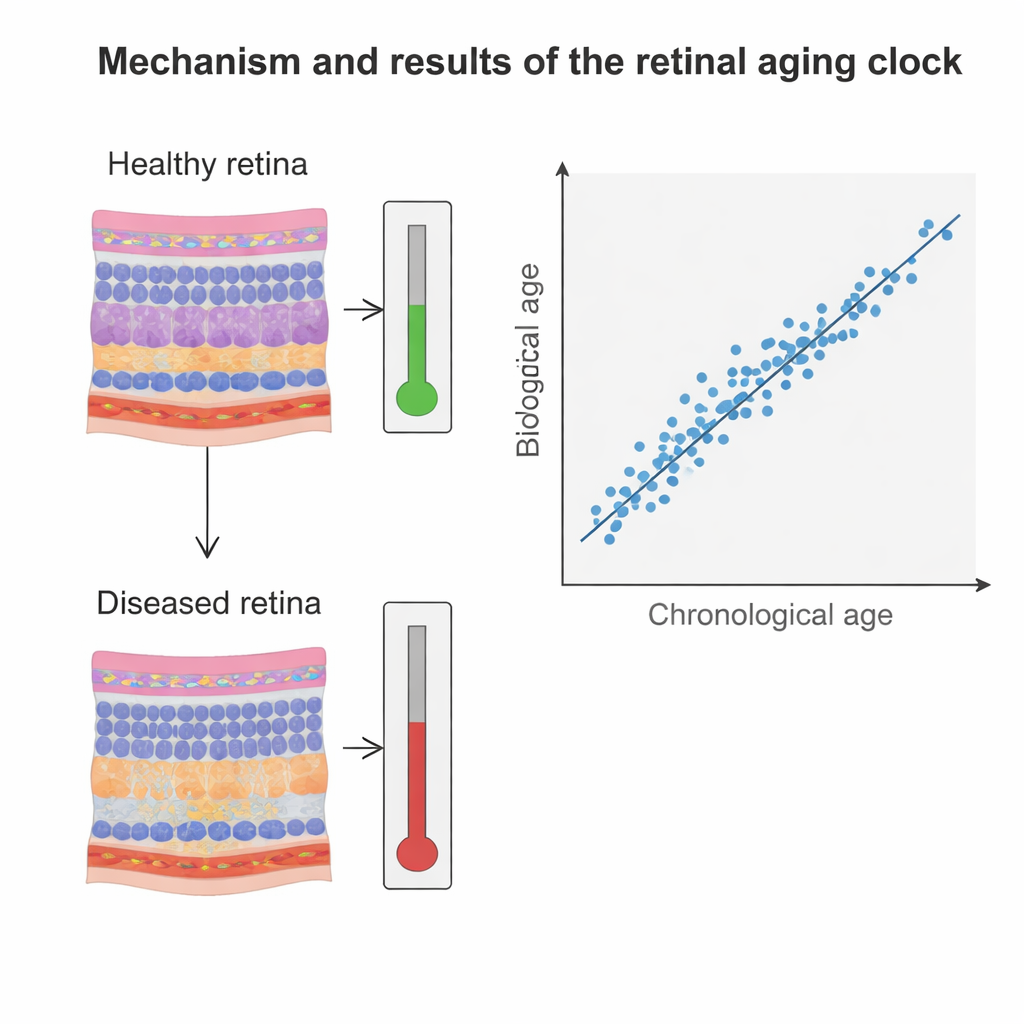
What the AI Actually Sees in the Eye
To peek inside the AI’s “thought process,” the researchers generated heatmaps showing which parts of each image most influenced its predictions. Rather than fixating on the central macula, the model consistently focused on the optic nerve head, the surrounding nerve fiber layer, and deeper vascular layers like the choroid. These are structures known to thin and stiffen with age and to be sensitive to pressure and blood flow changes. The AI’s attention patterns were similar across very different eye diseases, suggesting it had learned robust, anatomy-based indicators of aging rather than simply memorizing disease categories. Interestingly, when disease images were included in training, the model began to pay somewhat more attention to macular areas in conditions such as macular degeneration, hinting that disease-specific training helps it better recognize those patterns.
Limits, Caveats, and Future Possibilities
The study does have limitations. All data came from a single academic medical center, and many patients had low CCI scores, which blunts the ability to detect strong statistical links. The CCI itself is an older tool that may not fully capture modern patterns of chronic disease. Some correlations, particularly in macular degeneration, were weak or inconsistent. Yet despite a modest sample size compared with giant population biobanks, the model achieved competitive age-prediction accuracy and, crucially, tied retinal biological age to a validated measure of whole-body disease burden.
What This Means for Patients and Clinicians
For a layperson, the key message is that routine eye scans might someday do much more than check for glasses prescriptions or eye disease. By reading subtle changes in the retina’s nerves and blood vessels, AI could estimate how “old” the body truly is and flag people whose tissues are aging faster than their calendar years suggest. This retinal aging clock is not yet a bedside tool, but it points toward a future where a quick, noninvasive eye exam could contribute to early warning of hidden health risks, helping guide preventive care long before serious disease becomes obvious.
Citation: Ludwig, C.A., Salvi, A., Mesfin, Y. et al. A multimodal retinal aging clock for biological age prediction and systemic health assessment via OCT and fundus imaging. Sci Rep 16, 6465 (2026). https://doi.org/10.1038/s41598-026-36518-x
Keywords: retinal imaging, biological age, artificial intelligence, systemic health, eye disease