Clear Sky Science · en
Differences in red blood cell fatty acid profiles by type 2 diabetes status in early-stage chronic kidney disease
Why Fats in Blood Cells Matter for Kidneys
Chronic kidney disease and type 2 diabetes are two of the most common long-term illnesses worldwide, and they often occur together. Both conditions quietly damage blood vessels and organs over many years before symptoms appear. This research asks a deceptively simple question with big implications: can the types of fats stored in the membranes of our red blood cells reveal early trouble in the kidneys, and do these fat patterns look different in people with and without type 2 diabetes? Understanding this could open the door to earlier detection and more tailored dietary advice for those at risk.
Looking Inside Red Blood Cells
The study focused on the fatty acids that make up the outer membrane of red blood cells. These fats change slowly over time and therefore act as a longer-term record of diet and internal metabolism than a single blood test for cholesterol or glucose. The researchers examined a large group of 893 adults from 16 low-resource communities in Cape Town, South Africa. All participants either already had type 2 diabetes or were considered at high risk for it, based on a simple screening score using age, waist size, and blood pressure. The team measured kidney function, indicators of diabetes, and then used laboratory techniques to separate and quantify many different fatty acids in the red blood cell membranes.
Early Kidney Disease in the Community
Among these adults, about one in four had chronic kidney disease, mostly at very early stages, and a bit more than one in three had type 2 diabetes. Around one in six people were living with both conditions at the same time. Those with both kidney disease and diabetes tended to be older and, interestingly, weighed less and had smaller waistlines than some of their peers without diabetes, reflecting the complex ways in which long-term illness can affect body size. When the researchers looked at blood tests, they found that people with diabetes and kidney disease had more disturbed glucose levels, triglycerides, and kidney filtration measures, confirming that these were metabolically vulnerable groups.
Good and Bad Fat Patterns
The core of the study compared the detailed fat patterns in red blood cells across four groups: people with neither disease, with kidney disease alone, with diabetes alone, and with both. Overall, red blood cell membranes contained mostly saturated fats, followed by polyunsaturated fats and then monounsaturated fats. People with diabetes (with or without kidney disease) had lower levels of certain saturated and monounsaturated fats but higher levels of others, including the omega-3 fat docosahexaenoic acid. Most importantly, higher levels of polyunsaturated fats—especially linoleic acid and total omega-6 fats, along with overall polyunsaturated fats—were linked to better kidney function and lower odds of having chronic kidney disease. In contrast, a higher “lipogenic index,” an indicator of how strongly the body is channelling metabolism toward making certain saturated fats, was linked to worse kidney health.
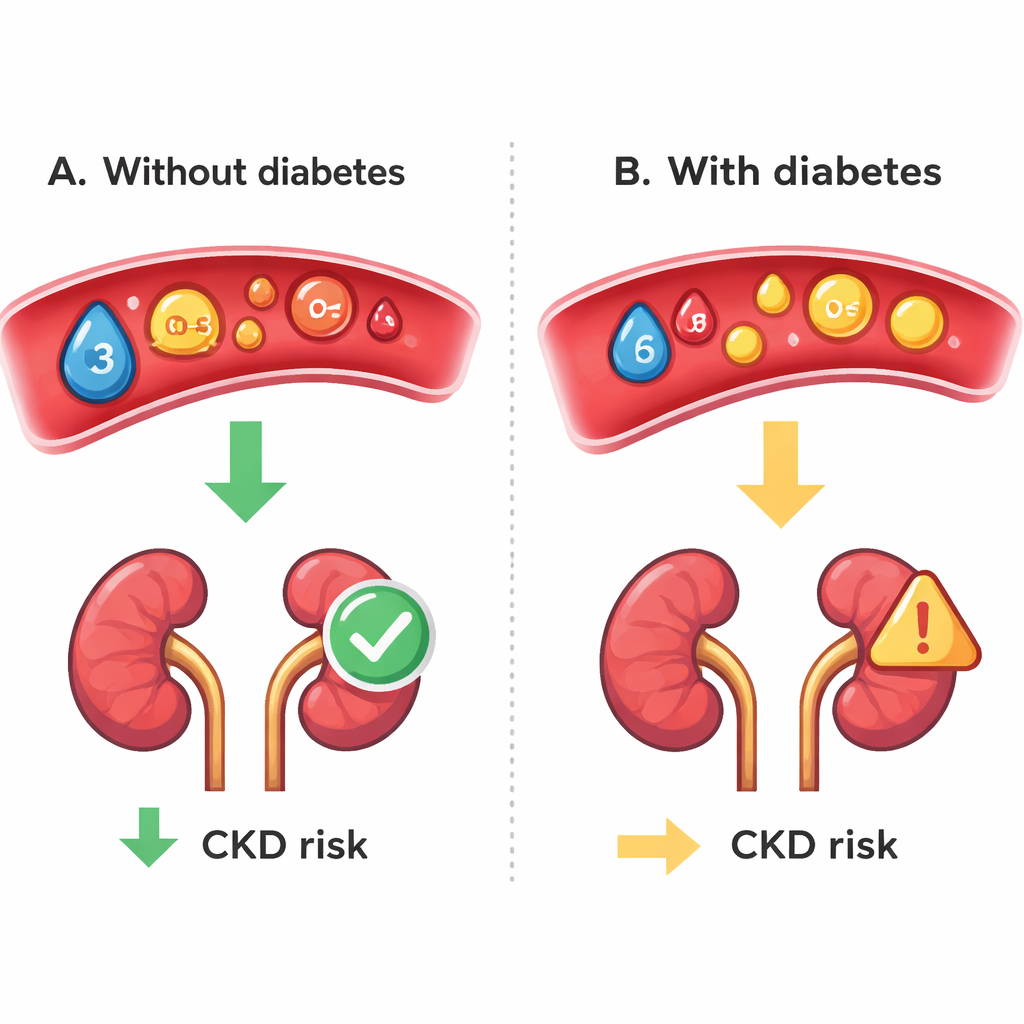
Diabetes Changes the Protective Effect
A striking finding was that the apparent protective effect of polyunsaturated fats was not the same for everyone. When the researchers separated people with and without type 2 diabetes, they found that higher levels of omega-6 and total polyunsaturated fats were associated with a lower chance of chronic kidney disease only in those without diabetes. Among people with diabetes, these higher levels no longer clearly reduced kidney disease risk. The authors suggest that in diabetes, long-standing high blood sugar, inflammation, and disordered fat handling may blunt the usual benefits of these healthier fats. In other words, the same fat pattern that looks helpful in one group may be less effective once diabetes has reshaped the body’s chemistry.
What This Means for Everyday Health
For a lay reader, the message is that the quality of fats built into our red blood cells—and ultimately into our organs—may give early warning of kidney stress, especially before full-blown disease appears. Diets that include a balanced intake of omega-6 and omega-3 polyunsaturated fats, from foods such as vegetable oils, nuts, seeds, and oily fish, are likely to support better kidney and metabolic health. However, once type 2 diabetes is established, these fats may not offer the same level of protection, underscoring the importance of prevention and early management. The study suggests that detailed fat profiles in red blood cells could one day complement existing tests to help doctors identify at-risk individuals sooner and to personalise dietary and treatment strategies for preserving kidney function.
Citation: George, C., Hill, J., Nqebelele, N.U. et al. Differences in red blood cell fatty acid profiles by type 2 diabetes status in early-stage chronic kidney disease. Sci Rep 16, 6127 (2026). https://doi.org/10.1038/s41598-026-36504-3
Keywords: chronic kidney disease, type 2 diabetes, red blood cell fatty acids, polyunsaturated fats, metabolic health