Clear Sky Science · en
A transpupillary approach for crosslinking Guinea pig sclera using WST11 and near-infrared light
Why this eye research matters
More and more children and adults around the world are becoming nearsighted, or myopic, which raises the risk of serious eye diseases and even blindness later in life. One reason myopia can worsen is that the white outer coat of the eye, the sclera, gradually stretches and weakens, allowing the eye to grow too long. This study explores a new, needle‑thin, light‑based approach to stiffen and strengthen the sclera from the outside, potentially offering a future way to slow or prevent dangerous eye elongation without major surgery.
A new way to strengthen the eye wall
Existing approaches to reinforce the sclera have important drawbacks. Earlier light‑based methods used ultraviolet light and the vitamin riboflavin to create extra links in collagen, the main structural protein in the eye wall. While these methods can stiffen tissue, ultraviolet light does not penetrate deeply and can damage the delicate retina unless surgeons surgically expose the sclera from the outside. Chemical agents injected around the eye can also crosslink collagen but tend to spread beyond the target area and may cause high eye pressure, inflammation, or retinal harm. The researchers instead tested a drug called WST11, mixed with a thickening sugar polymer named dextran, and activated it with near‑infrared (NIR) light at a wavelength (753 nm) that can safely pass through the pupil and reach the back of the eye.
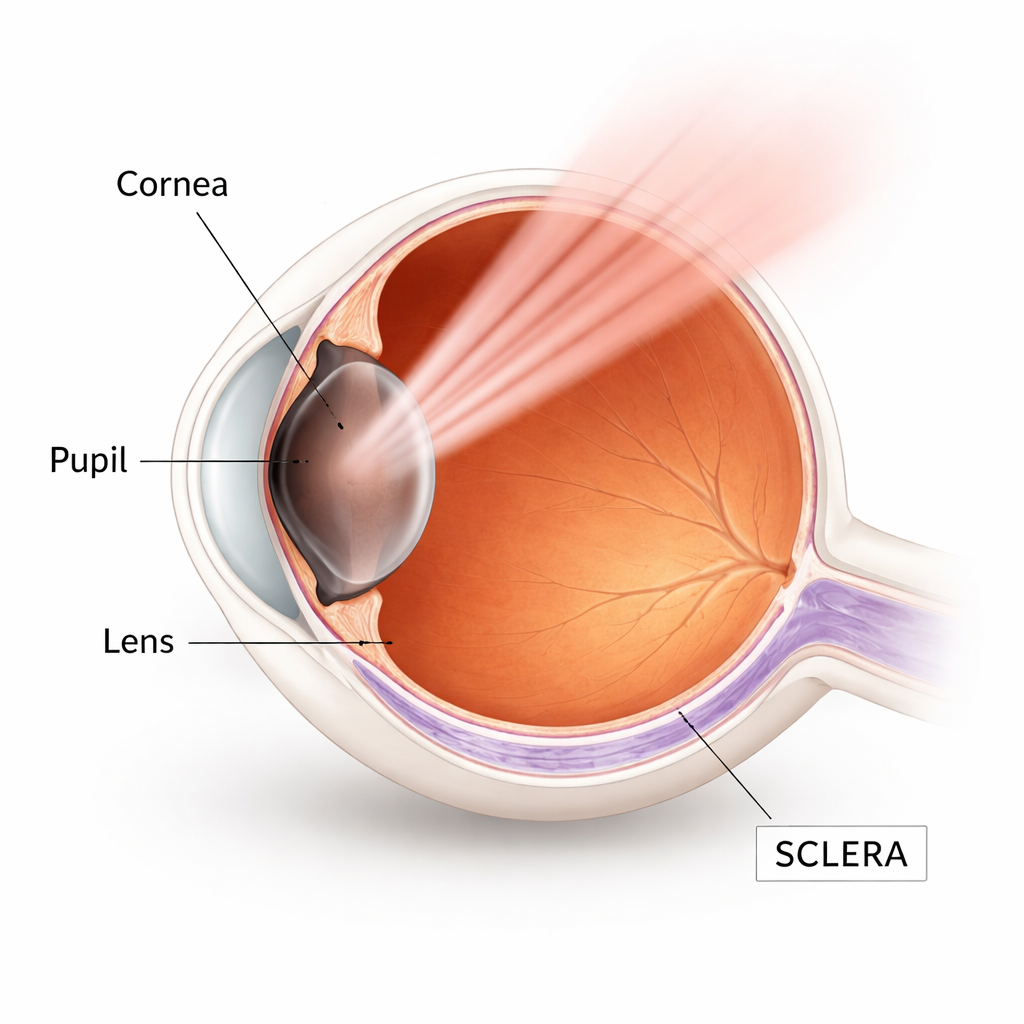
Keeping the treatment where it is needed
The first step was to make sure the drug stayed mainly in the sclera and did not seep into deeper, more sensitive layers like the retina. Using eyes from guinea pigs, a well‑established model for human myopia, the team soaked the back of the eye in WST11 solutions containing different amounts of dextran. Under a fluorescence microscope, they watched how far the purple‑glowing drug spread. Low dextran allowed WST11 to pass through the sclera and into the blood‑rich choroid, while higher dextran made the solution thicker and sharply slowed the drug’s movement. At 10% dextran and 30 minutes of exposure, most of the drug remained in the outer half of the sclera. Computer modeling of diffusion confirmed that these conditions would keep less than 1% of the peak drug concentration at the boundary with the choroid over this time, so this formulation was chosen for further tests.
Testing how much stronger the sclera becomes
To find the best light dose, the researchers then illuminated treated scleral samples with various NIR light powers and times and measured how easily the tissue shrank when gently heated. Collagen that has been crosslinked holds its shape to a higher temperature, so the key number was the temperature at which 50% shrinkage occurred. Across many combinations, all WST11‑plus‑NIR treatments increased this temperature compared with untreated eyes, meaning the tissue had become more heat‑resistant and therefore more strongly crosslinked. A relatively gentle setting—10 milliwatts per square centimeter for 30 minutes after a 30‑minute drug soak—produced one of the largest increases, about 6.8 °C, and also raised the mechanical stiffness (Young’s modulus) in standard pulling tests. Notably, eyes from older guinea pigs (about five to six months) showed a larger strengthening effect than those from younger animals, hinting that tissue maturity influences how well the treatment works.
Moving from the lab bench into living eyes
Next, the team tried to mimic how the treatment might be delivered in patients. In one series of experiments, they shone NIR light through the pupil of intact, drug‑soaked eyes and found that this “transpupillary” route stiffened the equatorial sclera (the region around the mid‑eye) just as well as direct exposure to bare scleral pieces. A simple physical model suggested that roughly 40% of the incoming NIR light should still be available at the back surface of the guinea pig sclera, enough to trigger crosslinking. Finally, in live anesthetized animals, the drug mixture was injected around the eye near either the equator or the very back, allowed to sit for 30 minutes, and then activated by NIR light entering through the pupil. In both regions, the treated sclera showed significantly higher thermal stability than tissue from untreated fellow eyes, demonstrating that this minimally invasive approach can work in vivo. Some mild strengthening also occurred in control eyes exposed only to light and saline, raising the possibility that NIR light alone may trigger beneficial remodeling.
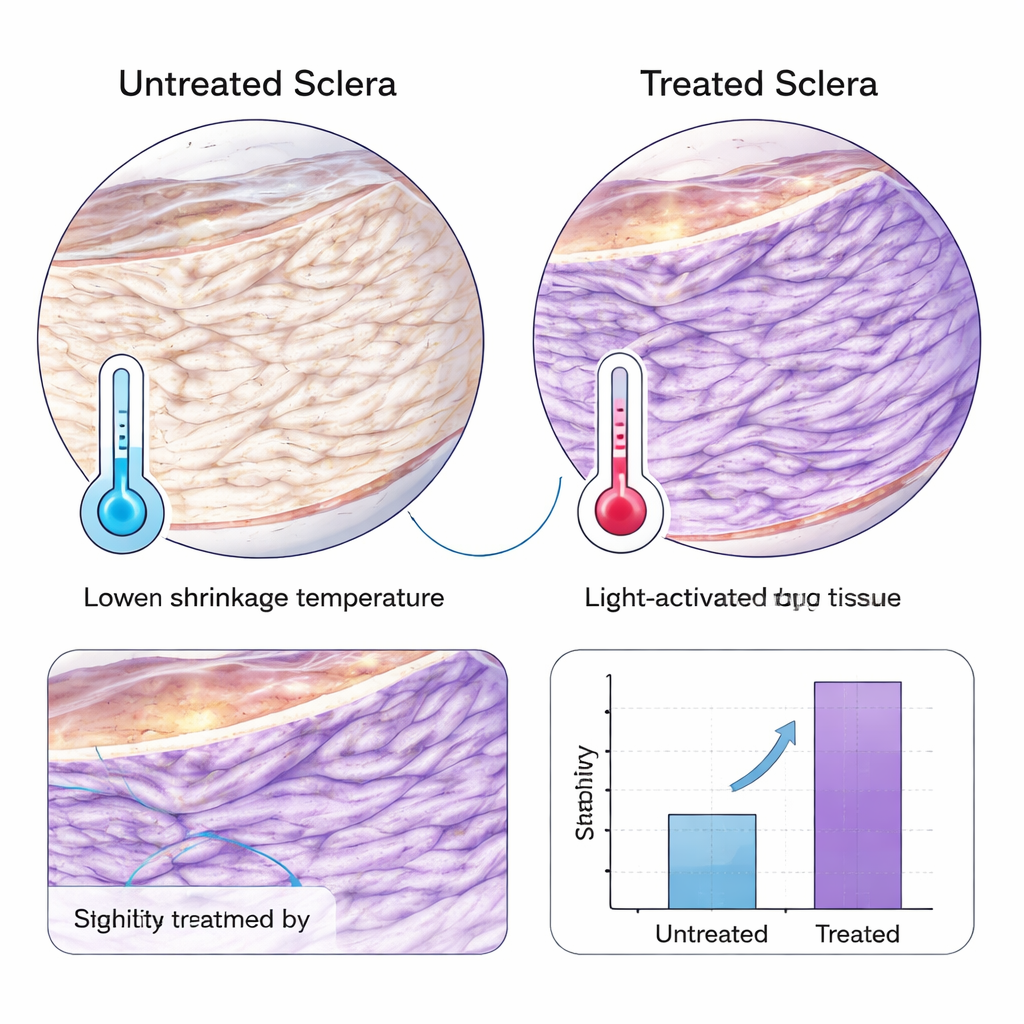
What this could mean for people with worsening myopia
Overall, the study shows that a carefully formulated WST11 and dextran solution, activated by safe levels of near‑infrared light directed through the pupil, can selectively stiffen the sclera in guinea pigs without obvious spread of the drug into deeper tissues. The method strengthened both side and back regions of the eye wall and appeared more effective in more mature eyes, suggesting that future treatments might be tailored by age. While many questions remain—especially about long‑term safety, ideal dosing in human‑sized eyes, and real‑world impact on myopia progression—this work offers a promising blueprint for a noninvasive procedure that directly targets the weak outer shell of the eye, aiming to keep it from stretching and protect vision over a lifetime.
Citation: Vogels, D.H.J., Abdulla, Y., Myles, W. et al. A transpupillary approach for crosslinking Guinea pig sclera using WST11 and near-infrared light. Sci Rep 16, 6098 (2026). https://doi.org/10.1038/s41598-026-36438-w
Keywords: myopia control, scleral crosslinking, near infrared light, WST11 treatment, guinea pig eye model