Clear Sky Science · en
An epidemiological analysis of cranio-vertebral morphometrics other than tonsillar position in symptomatic, adult, female Chiari malformation type I
Why the shape of the skull base matters
Chiari malformation type I is a condition in which part of the brain at the back of the head bulges down toward the spine, often causing severe headaches, neck pain, and other neurological problems. Yet doctors have long puzzled over why some people with this downward bulge are desperately ill while others feel fine. This study looks beyond the usual measure of how far the brain has dropped, and instead asks a broader question: does the overall shape of the skull base and surrounding spaces help explain who develops symptomatic Chiari?
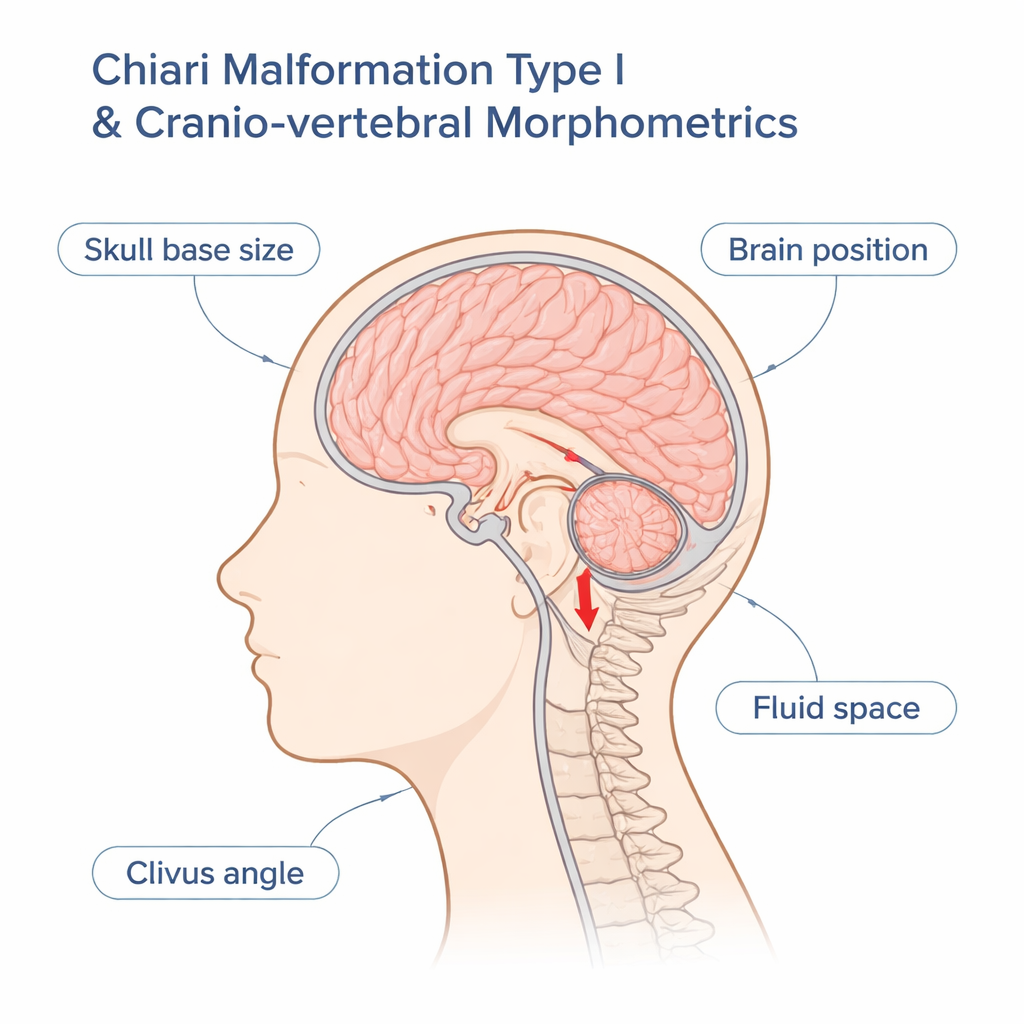
Looking past a single measurement
Traditionally, Chiari I has been defined by how many millimeters the cerebellar tonsils extend below a bony opening at the base of the skull. But research has shown that many people meet that definition on an MRI scan yet have no symptoms at all. At the same time, patients who are clearly disabled by Chiari can have only mild-looking changes on their scans. To untangle this, the authors studied a large group of 432 adult women with symptomatic Chiari I and 148 healthy women. Instead of focusing on tonsil position alone, they analyzed nine different size and angle measurements that describe the bony skull base, the position of the lower back part of the brain, and the space available for the fluid that bathes the brain and spinal cord.
How the study was set up
The researchers used existing MRI scans from two large projects: one that follows people with Chiari and one that follows healthy volunteers. For each participant, they measured features such as the length of key skull base bones, the area of the space at the back of the skull that houses the cerebellum, and the size of the fluid spaces in front of and behind the brainstem. They then asked two main questions. First, how much more likely is someone to have Chiari if a given measurement is unusually small or large compared with controls? Second, if you look at all nine measurements together, can you reliably tell who has symptomatic Chiari, even without looking at how far the tonsils have herniated?
Key shapes and spaces that stand out
Several clear patterns emerged. Women with Chiari tended to have a slightly smaller space at the back of the skull, shorter skull base bones, and tighter fluid spaces around the brainstem. Among all measurements, one stood out: the vertical position of a landmark deep inside the cerebellum, called the fastigium. In patients, this landmark sat noticeably closer to the opening at the base of the skull, even when the overall skull space was not dramatically smaller. Women whose fastigium lay far below the typical level were many times more likely to have Chiari than women with a typical value. Another important feature was the amount of fluid space in front of the brainstem. People with Chiari often had this front space squeezed, and the more it was reduced, the stronger the link to having the condition.
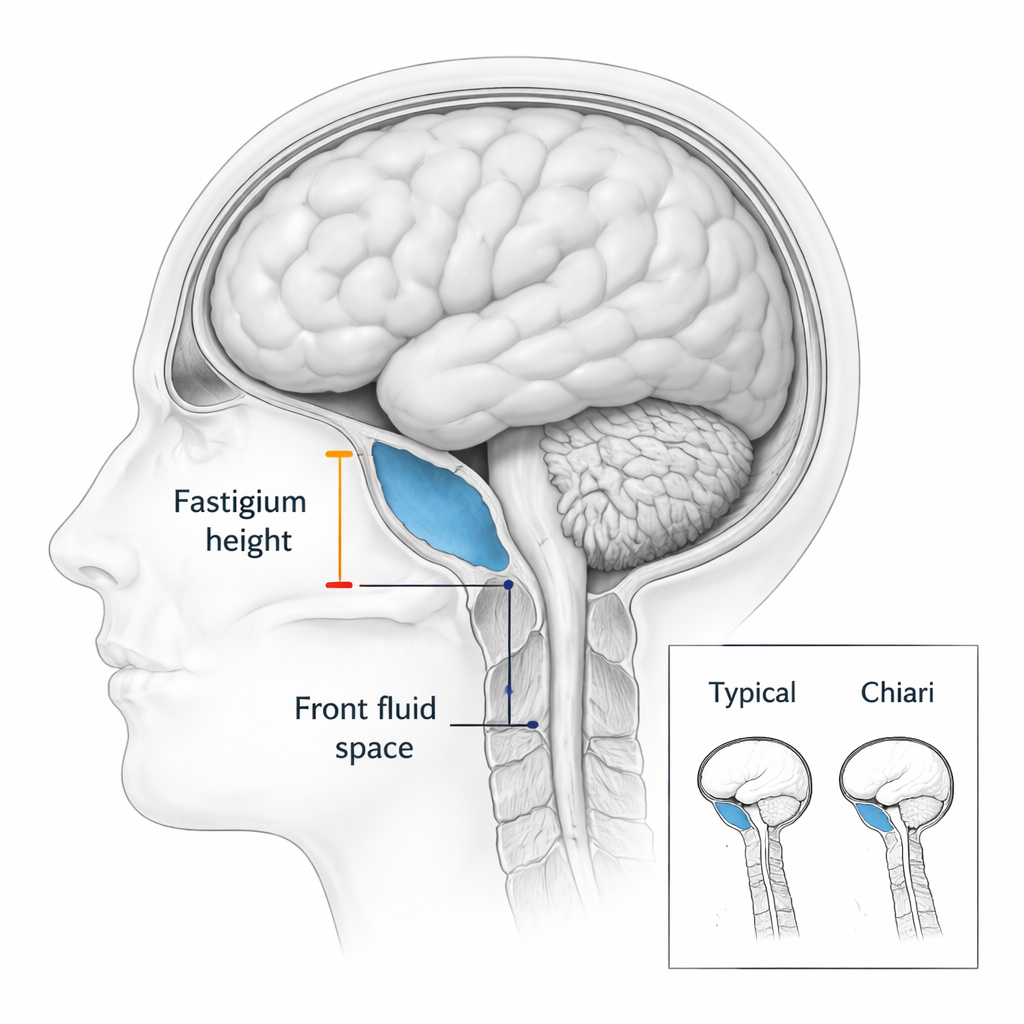
Pattern recognition in brain and bone
When the team combined the measurements in a statistical model, six of the nine features—particularly fastigium height and the front fluid space—helped distinguish patients from healthy controls. Using only these shape measures and not the tonsil herniation itself, the model correctly labeled about 87% of the Chiari cases and about 81% of all participants overall. Most women with Chiari had at least three measurements that were more than one standard unit away from the typical control value, underscoring that their skull base and nearby structures often deviate from the norm in several subtle ways rather than through a single dramatic abnormality.
Symptoms are more than structure alone
Surprisingly, having more abnormal measurements did not mean worse symptoms. Patients with relatively mild-looking anatomy could be just as disabled, and just as likely to need surgery or develop fluid-filled cavities in the spinal cord, as those with more extreme shapes. This suggests that other factors—such as how brain fluid pulses with each heartbeat, how flexible the covering of the brain and spinal cord is, how the body responds to long-term stress, and even past injuries—may strongly influence how sick a person becomes, beyond what static MRI pictures reveal.
What this means for patients
For people living with Chiari I, this study reinforces that the condition is about more than a simple measurement of how far the brain has dropped. Many patients share a cluster of subtle shape differences in the skull base, the back of the brain, and the nearby fluid spaces, especially a lower position of the cerebellar fastigium and a narrowed front fluid channel. These features make Chiari more likely, but they do not by themselves dictate how much pain or disability a person will experience. In practice, this means that understanding and treating Chiari will require looking at both anatomy and how the nervous system and whole body respond over time—not just a single number on the scan.
Citation: Labuda, R., Klinge, P., Bhadelia, R. et al. An epidemiological analysis of cranio-vertebral morphometrics other than tonsillar position in symptomatic, adult, female Chiari malformation type I. Sci Rep 16, 5330 (2026). https://doi.org/10.1038/s41598-026-36412-6
Keywords: Chiari malformation type I, skull base anatomy, cerebrospinal fluid space, brain MRI, neurological pain