Clear Sky Science · en
Obesity and risk of immune-mediated inflammatory diseases: a real-world propensity score-matched cohort study using electronic health records
Why Weight and the Immune System Matter
Most people know that extra body weight can strain the heart and raise the risk of diabetes. Far fewer realize that fat tissue also talks to the immune system. This study asks a simple but important question: does obesity make people more likely to develop autoimmune and other immune-related diseases, where the body mistakenly attacks its own tissues? Using millions of real-world medical records, the researchers traced how body mass index (BMI) relates to a wide range of these conditions.
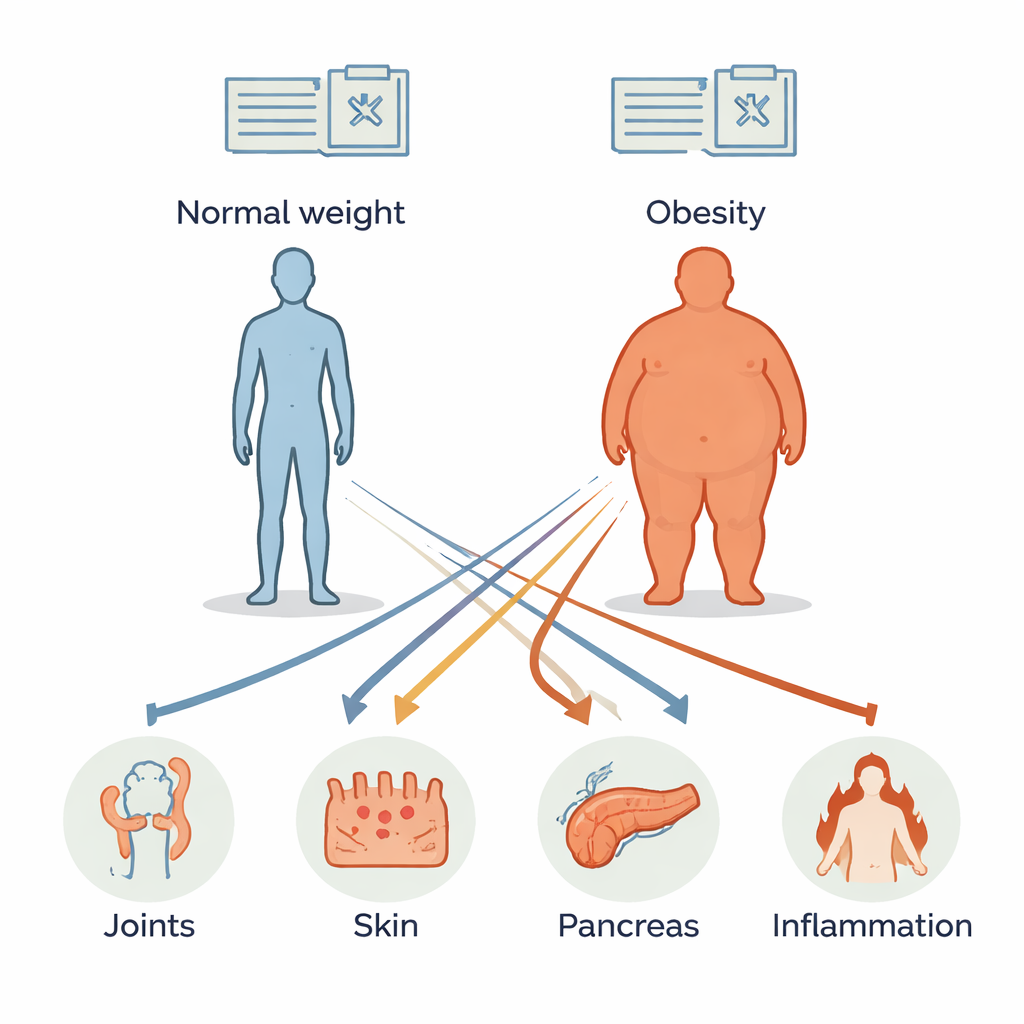
A Massive Look at Everyday Medical Records
Instead of running a traditional clinical trial, the team tapped into the TriNetX global research network, which pools anonymous electronic health records from more than 300 million patients across many hospitals. They focused on adults who had their BMI recorded between 2015 and 2019 and divided them into two groups: those with obesity (BMI of 30 or higher) and those without obesity (BMI between 18.5 and 29.9). To make the comparison fair, each person with obesity was matched to a similar person without obesity based on age, sex, race, other illnesses, and how often they saw doctors. This careful matching yielded nearly 700,000 people in each group—over 1.3 million in total—who were then followed for up to five years.
Tracking Who Developed Which Diseases
The researchers checked who went on to develop 15 different immune-mediated inflammatory diseases. These included joint and skin conditions like rheumatoid arthritis and psoriasis, gland disorders such as type 1 diabetes and thyroid disease, and whole-body or nerve-related conditions like lupus, sarcoidosis, and multiple sclerosis. They used standard diagnosis codes from routine care to mark when each disease first appeared and applied statistical models to estimate how much more (or less) likely people with obesity were to develop each condition compared with their matched peers.
Higher Risks for Some Diseases, Lower for Others
Obesity did not affect all immune-related diseases in the same way. People with obesity had noticeably higher risks of several conditions. The largest increases were seen in psoriatic arthritis, a painful joint disease linked to psoriasis, where risk was about three-quarters higher, and in type 1 diabetes, where risk was about 40% higher. Risks were also modestly higher for rheumatoid arthritis, psoriasis itself, lupus, sarcoidosis, and ankylosing spondylitis. Strikingly, two autoimmune diseases—Sjögren’s syndrome and systemic sclerosis—were actually less common in people with obesity. For several nerve-related conditions, such as multiple sclerosis and myasthenia gravis, there was no clear difference between weight groups.
Patterns by Age, Sex, and Amount of Weight
The links between obesity and disease also varied across different types of people. Middle-aged adults showed the strongest ties between obesity and joint diseases like rheumatoid and psoriatic arthritis, while younger adults with obesity were more likely to develop type 1 diabetes and autoimmune thyroid problems. Women with obesity tended to have higher risks than men for some conditions, including rheumatoid arthritis, psoriatic arthritis, and type 1 diabetes. When the team split BMI into finer categories—from overweight to severe obesity—they saw that risks for rheumatoid arthritis and psoriasis rose in a stepwise fashion as BMI increased, suggesting a dose–response effect: the higher the BMI, the greater the risk.
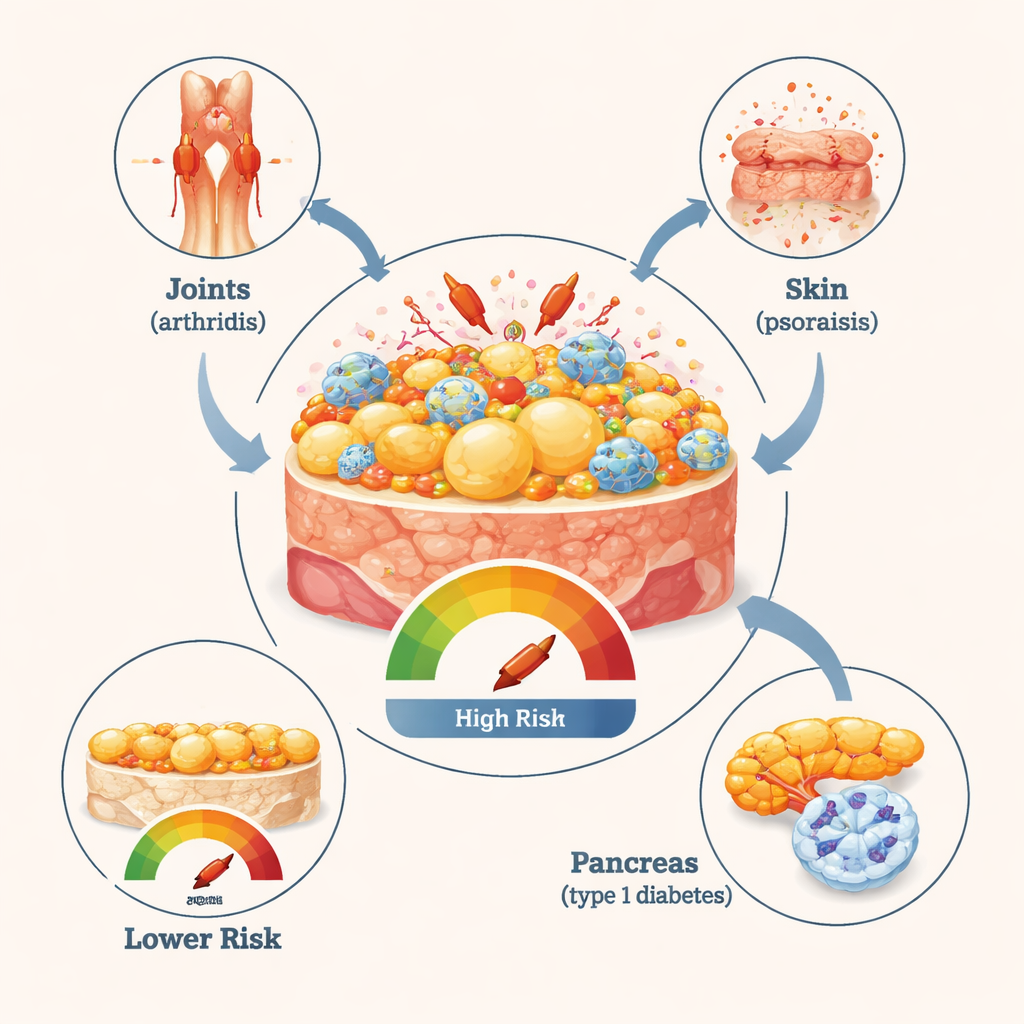
What This Means for Health and Prevention
To a lay reader, the takeaway is that body fat is not just a passive energy store; it actively shapes the immune system. Extra fat tissue can release inflammatory molecules and alter immune cells in ways that appear to make certain autoimmune diseases more likely, especially psoriasis, psoriatic arthritis, rheumatoid arthritis, and type 1 diabetes. At the same time, the fact that some diseases were less common or unchanged reminds us that obesity does not raise the risk of every immune condition and that different diseases may follow different biological pathways. While this study cannot prove cause and effect, its size and careful design strongly support obesity as a modifiable risk factor for several autoimmune illnesses. That means strategies that prevent or reduce obesity may not only protect the heart and metabolism but could also help lower the chances of some immune-related diseases.
Citation: Lin, YJ., Hsu, WH., Lai, CC. et al. Obesity and risk of immune-mediated inflammatory diseases: a real-world propensity score-matched cohort study using electronic health records. Sci Rep 16, 5332 (2026). https://doi.org/10.1038/s41598-026-36400-w
Keywords: obesity, autoimmune diseases, inflammation, electronic health records, rheumatoid arthritis