Clear Sky Science · en
Increased cervical spinal cord signal intensity corresponds to specific cerebellar and cerebral functional changes in degenerative cervical myelopathy patients
Neck Problems That Reach All the Way to the Brain
Many people develop wear-and-tear changes in the neck that slowly squeeze the spinal cord, a condition called degenerative cervical myelopathy. It can cause clumsy hands, trouble walking, and even bladder problems. Doctors can see damage in the cord on MRI scans as bright spots, but these images do not fully explain why some patients bounce back after surgery while others do not. This study asks a simple but important question: do those bright spots in the neck line up with hidden changes in the brain and cerebellum that help determine recovery?
Bright Spots on MRI and What They Really Mean
On standard MRI scans, many patients show areas of increased signal intensity—bright regions inside the spinal cord. A newer system, called Ax-CCM, sorts these patterns into several types. One particular kind, a fuzzy focal bright spot known as type 2, has been linked to worse outcomes after surgery and is thought to reflect ongoing, active injury rather than old, healed damage. However, these images mainly reveal structure, not function. They do not show how well the spinal cord and brain are actually working, which ultimately governs how much function a person can regain.
Peeking at Brain Activity in Resting Patients
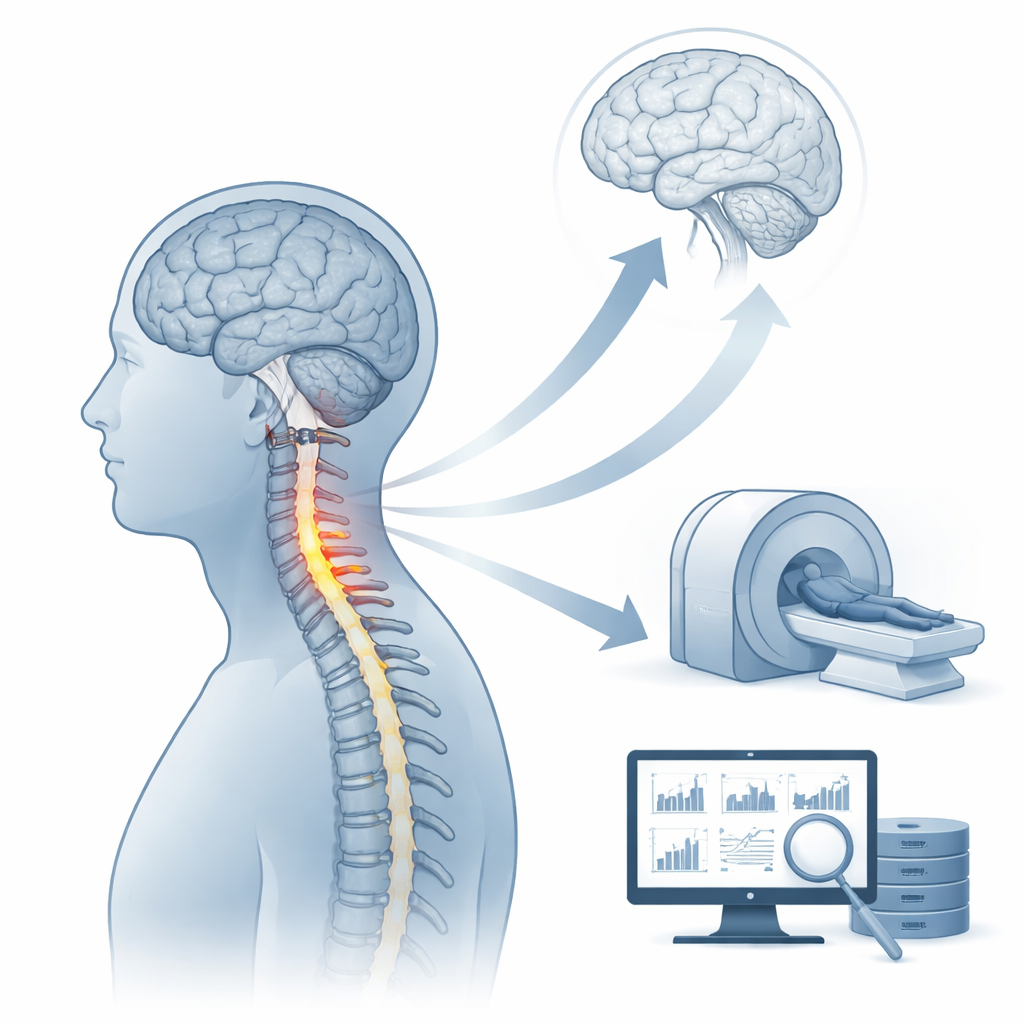
To explore this, the researchers studied 54 patients with degenerative cervical myelopathy and 50 healthy volunteers using resting-state functional MRI, which tracks natural fluctuations in blood flow as a stand-in for brain activity. They focused on a measure called the amplitude of low-frequency fluctuation, or ALFF, which captures how strongly different brain areas "pulse" at rest. Patients were divided into two groups: those with the worrisome type 2 bright spots, and those with all other patterns. The team compared brain activity among these two patient groups and the healthy controls, and then asked whether these brain signals could help predict how well patients recovered after spinal cord decompression surgery.
Different Neck Lesions, Different Brain Signatures
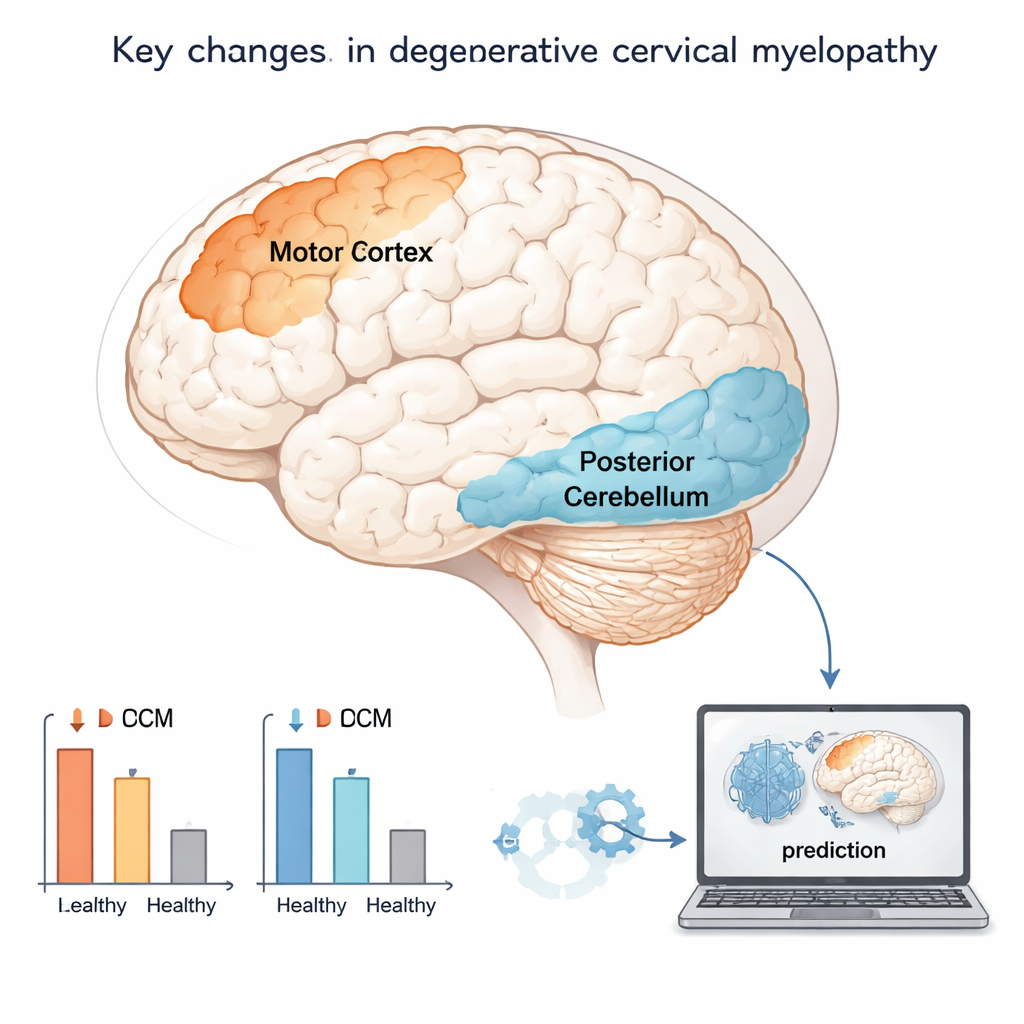
The team found that patients with type 2 lesions had especially reduced activity in a region of the back of the cerebellum, a structure critical for coordinating movement and balance. Lower activity here was tied to poorer recovery after surgery, particularly in the type 2 group, suggesting that cerebellar dysfunction marks a more advanced or actively damaging stage of disease. By contrast, patients with other lesion types showed stronger changes in the precentral gyrus, the brain’s primary motor area that controls voluntary movement. Both patient groups also showed reduced activity in a frontal region involved in higher-level control of movement and planning when compared to healthy people. Together, these findings support the idea that the brain reorganizes differently depending on the pattern of spinal cord damage seen on MRI.
Using Brain Signals to Forecast Recovery
The researchers next built computer models to see whether these functional brain measures could help forecast how patients would do after surgery. They tested three versions: one that used only basic clinical information such as age, smoking status, disease duration, and pre-surgery scores; a second that added the MRI lesion type; and a third that added the brain activity measures from the motor cortex and cerebellum. All models could predict recovery to some degree, but including the brain data gave a modest improvement in accuracy and lowered the prediction error. This suggests that MRI of the brain can capture aspects of spinal cord function—and its capacity to rebound—that structural images of the neck alone miss.
What This Means for Patients and Their Doctors
For patients, the message is that neck problems can quietly reshape how the brain and cerebellum work, and those changes matter for recovery. A certain kind of bright spot in the spinal cord, the fuzzy focal type 2 lesion, appears to go hand in hand with more serious disruption in the cerebellum and a tougher road back after surgery. For doctors, combining traditional scans of the neck with functional brain imaging and machine learning may eventually provide a more personalized forecast: who is likely to recover well, who may need closer follow-up, and who might benefit from added rehabilitation targeting balance and coordination. While larger studies are still needed, this work points toward a future in which treating spinal cord disease means looking beyond the neck to the entire nervous system.
Citation: Li, L., Sun, Z., Wang, Y. et al. Increased cervical spinal cord signal intensity corresponds to specific cerebellar and cerebral functional changes in degenerative cervical myelopathy patients. Sci Rep 16, 5992 (2026). https://doi.org/10.1038/s41598-026-36384-7
Keywords: degenerative cervical myelopathy, spinal cord MRI, functional brain imaging, cerebellum, surgical prognosis