Clear Sky Science · en
Baseline serum oxytocin and OXTR rs53576 genotype are not predictive of escitalopram response in generalized anxiety disorder
Why this study matters for people with chronic worry
Many people with generalized anxiety disorder live with constant, exhausting worry and often try several medications before finding any relief. Scientists hoped that a hormone called oxytocin, sometimes nicknamed the “bonding hormone,” and a related gene might help predict who will benefit from a common anxiety medicine, escitalopram. This study tested whether a simple blood test and a gene test could guide more personalized treatment for anxiety.
A closer look at worry, hormones, and genes
Generalized anxiety disorder (GAD) is marked by persistent, hard-to-control worry about everyday things. Escitalopram, a selective serotonin reuptake inhibitor (SSRI), is a standard first-line medication, but people’s responses vary widely. The researchers focused on oxytocin, a hormone involved in stress relief, social bonding, and emotional regulation, and on a specific variation in the oxytocin receptor gene, called OXTR rs53576. Previous work suggested that people with one version of this gene (the AA type) tend to be more stress-sensitive, while those carrying a G variant may be more resilient. The team asked: do baseline oxytocin levels and this gene variant help predict who will respond better to escitalopram?
Who took part and what the team measured
The study followed 60 adults experiencing their first episode of GAD who had not recently taken psychiatric medication, along with 60 healthy people of the same age and sex for comparison. All participants gave a fasting blood sample so the team could measure oxytocin levels and determine which version of the OXTR rs53576 gene they carried. The patients then took escitalopram for eight weeks, starting at 10 mg per day, with the option to increase to 20 mg. Trained clinicians, unaware of the lab results, rated anxiety using a standard questionnaire at the start and again at weeks 2, 4, and 8. A “treatment response” meant at least a 50 percent drop in anxiety scores.
What they discovered about anxiety and oxytocin
Compared with healthy volunteers, people with GAD started out with significantly higher oxytocin levels in their blood and were far more likely to have the AA version of the oxytocin receptor gene. Both higher oxytocin and the AA genotype were linked to more severe anxiety symptoms at the beginning of the study, even after accounting for age and sex. This pattern may reflect a stressed system trying, but failing, to compensate: the body may release more oxytocin to counter chronic worry, while a less favorable receptor version makes that signal less effective. In other words, the oxytocin system clearly looked “off balance” in people with GAD.
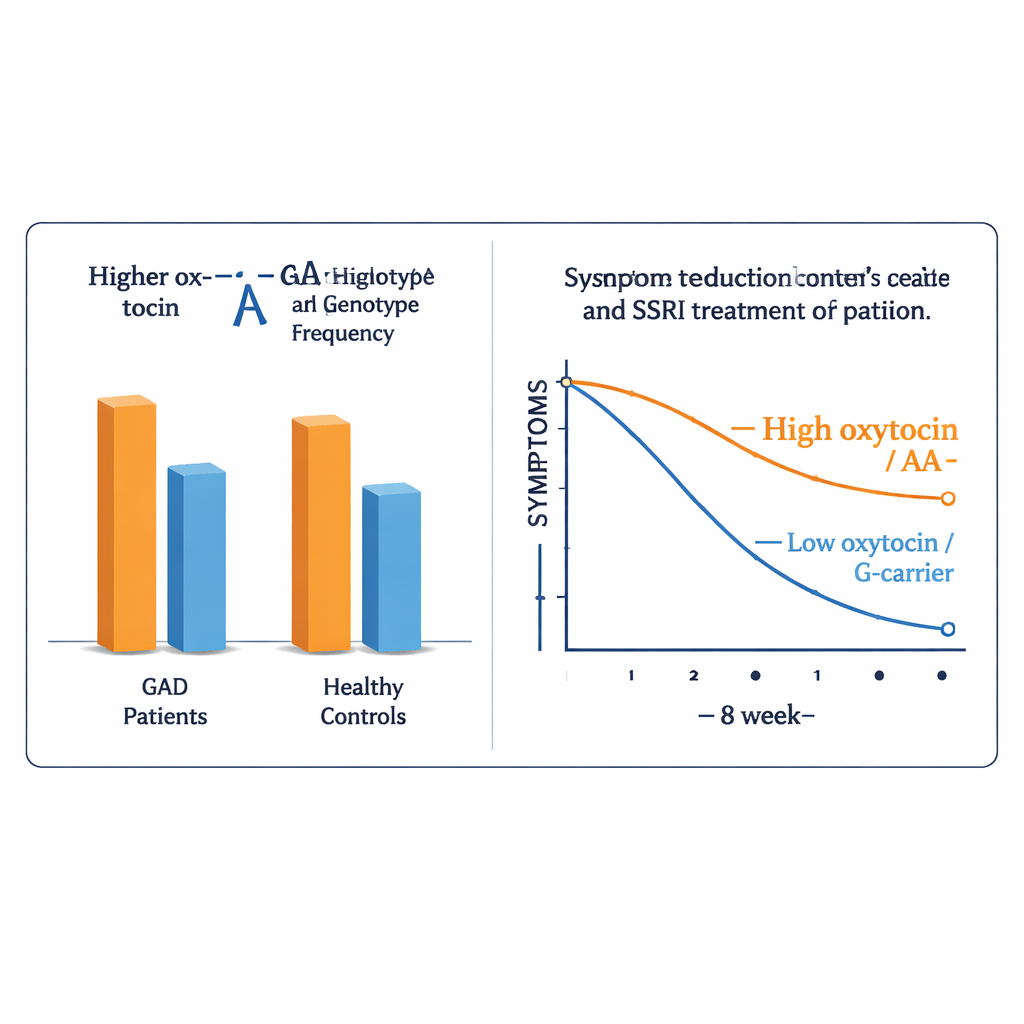
What happened once treatment began
After eight weeks of escitalopram, more than three-quarters of the patients showed a strong reduction in anxiety. However, when the researchers compared those who improved with those who did not, they found no meaningful differences in starting oxytocin levels or in their OXTR gene type at weeks 2, 4, or 8. Whether a patient had high or low oxytocin, or the AA or G-carrying gene version, their chances of benefiting from escitalopram were essentially the same. Even when the team looked at different medication doses, these biological measures still did not help explain who responded and who did not.
What this means for people seeking better treatments
For patients and clinicians hoping for a quick blood or gene test to choose the best anxiety medicine, this study brings a clear message: although oxytocin biology is linked to having generalized anxiety and to how severe it feels at the outset, it does not tell us who will get better on escitalopram in the short term. The findings narrow the search for useful predictors, suggesting that we should look beyond baseline oxytocin and this single gene variant when designing personalized treatment plans. Future work may focus on how oxytocin changes over time, other kinds of therapies, or combinations of many genes to better match each person with the treatment most likely to ease their chronic worry.
Citation: Xue, L., Ni, H. & Xu, S. Baseline serum oxytocin and OXTR rs53576 genotype are not predictive of escitalopram response in generalized anxiety disorder. Sci Rep 16, 7458 (2026). https://doi.org/10.1038/s41598-026-36366-9
Keywords: generalized anxiety disorder, oxytocin, escitalopram, biomarkers, personalized psychiatry