Clear Sky Science · en
Evaluation of dECM hydrogel-NAP on 3D organotypic human corneal epithelium in diabetic keratopathy model
Why this matters for people with diabetes
People with diabetes often worry about damage to the retina, but the very front of the eye—the clear cornea—is also at risk. In a condition called diabetic keratopathy, the surface of the eye becomes fragile, slow to heal, and more vulnerable to infection and vision loss. This study explores a new gel-based treatment, built from natural tissue and a protective peptide, that could help the cornea heal better and stay clear in people with diabetes.
A damaged eye surface in diabetes
The cornea is the transparent “window” that lets light enter the eye. Its outermost layer, the epithelium, must remain smooth, intact, and quickly repair any tiny scratches from blinking or dust. In diabetes, high blood sugar triggers stress and inflammation in these cells, causing them to die more readily and weakening the barrier that keeps germs and fluid out. Over time, this can lead to poor wound healing, recurrent erosions, pain, scarring, and blurred vision. Current treatments mostly soothe symptoms with eye drops or bandage lenses, but they do little to correct the underlying cellular damage.
A smart gel built from natural tissue
The researchers tested a new material called a decellularized extracellular matrix (dECM) hydrogel, made from bovine pericardium (the membrane around a cow’s heart). All living cells are removed, leaving behind a natural scaffold rich in collagen and other molecules that living cells like to attach to. They then enriched this gel with a tiny fragment of a protective brain protein, known as NAP, which has already shown antioxidant and cell-protecting effects in the eye and nervous system. The team first checked that the gel stayed transparent enough for vision and that it was not toxic to human and rabbit corneal cells grown in the lab. At a low concentration, the gel remained almost as clear as the human cornea and actually improved cell growth, especially when combined with NAP.
Helping corneal cells close wounds
To test whether the gel could speed healing, the scientists created small scratches in lab-grown corneal cell layers—an in vitro stand‑in for a superficial corneal wound. Cells growing on the NAP-enriched dECM hydrogel migrated into the scratch more quickly and closed the gap faster than untreated cells or cells exposed to the gel or NAP alone. Importantly, the gel did not distort normal cell shape or organization over several days of culture, suggesting that it offers a friendly surface that supports repair without harming the cells.
Rebuilding a diabetic-like cornea in 3D
Because a flat cell sheet cannot fully mimic the eye, the researchers built a three-dimensional “organotypic” human corneal epithelium—essentially, a miniature, layered corneal surface grown at an air–liquid interface. Under normal sugar levels, this model developed multiple organized layers, expressed typical corneal markers, and showed electrical resistance similar to that measured in living human corneas, indicating a tight, functional barrier. When exposed to high glucose levels that resemble those found in people with diabetes, the tissue thinned, lost key barrier proteins, and showed more signs of cell death and fewer dividing cells. Adding the dECM hydrogel enriched with NAP largely reversed these changes: the layers thickened again, barrier strength recovered, a tight-junction protein called ZO‑1 reappeared in the right locations, cell survival improved, and markers of programmed cell death dropped.
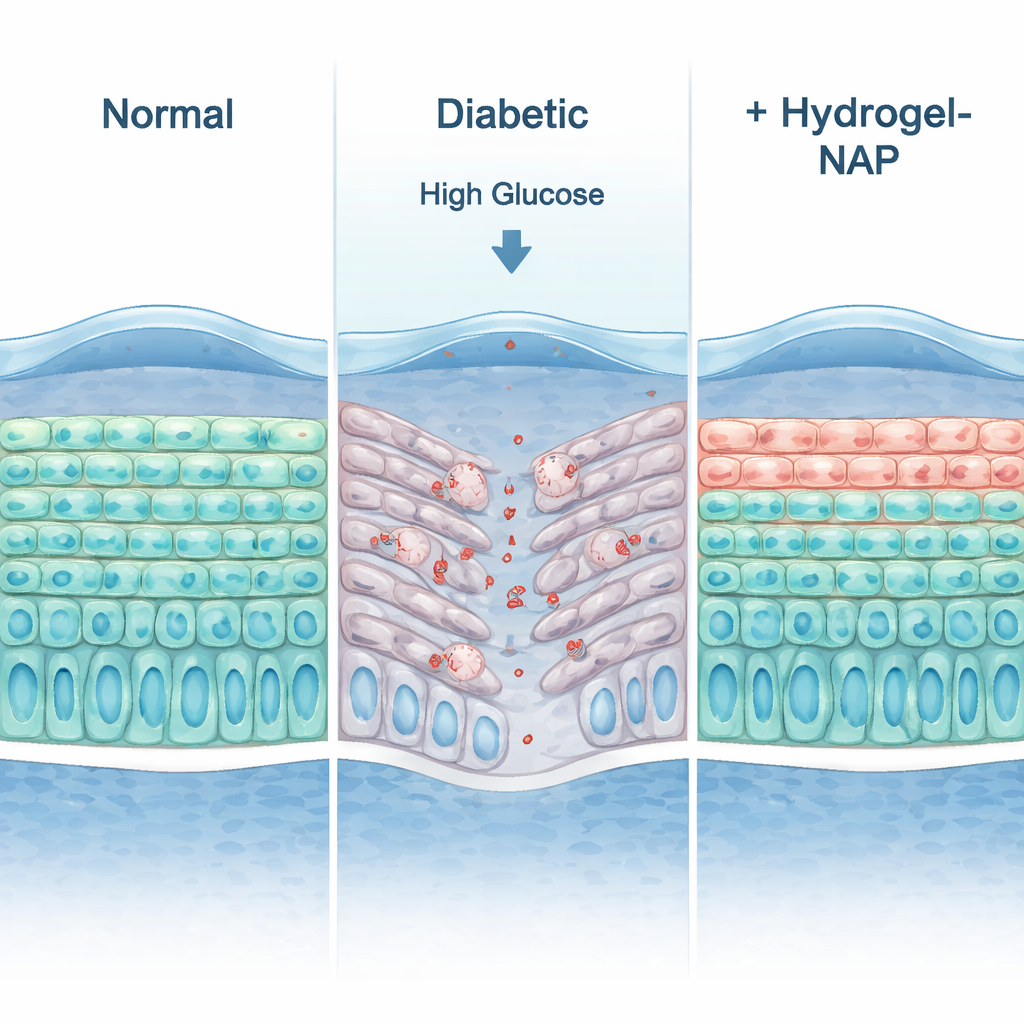
What this could mean for future eye care
For a layperson, the takeaway is that this natural, transparent gel acts like a smart bandage for the diabetic cornea. In a realistic lab model, it helped rebuild a strong, multilayered surface, reduced cell death, and supported healing under damaging high-sugar conditions. While these results are still preclinical and more work is needed in full‑thickness corneal models and animal studies, the approach could one day translate into eye drops, bioactive contact lenses, or post‑surgical treatments specifically designed to protect and repair the corneas of people living with diabetes.
Citation: Casarella, S., Palmeri, N., D’Amico, A.G. et al. Evaluation of dECM hydrogel-NAP on 3D organotypic human corneal epithelium in diabetic keratopathy model. Sci Rep 16, 5221 (2026). https://doi.org/10.1038/s41598-026-36316-5
Keywords: diabetic keratopathy, corneal healing, tissue-engineered hydrogel, NAP peptide, ocular surface regeneration