Clear Sky Science · en
Effects of DRG pulsed radiofrequency parameters on the clinical outcome for battered sensory never syndrome: a prospective, triple-blind, randomized controlled trial
Why Back and Leg Pain After Surgery Still Matters
Many people hope that back surgery will finally end their years of pain. Yet a surprising number continue to live with burning, shooting pain down the leg even after technically “successful” operations. This study looks at a newer, needle-based treatment that targets tiny nerve clusters along the spine using carefully controlled bursts of radio waves. The researchers asked a simple but crucial question: which settings for this treatment give patients the most relief while staying safe?
A Hidden Cause of Stubborn Nerve Pain
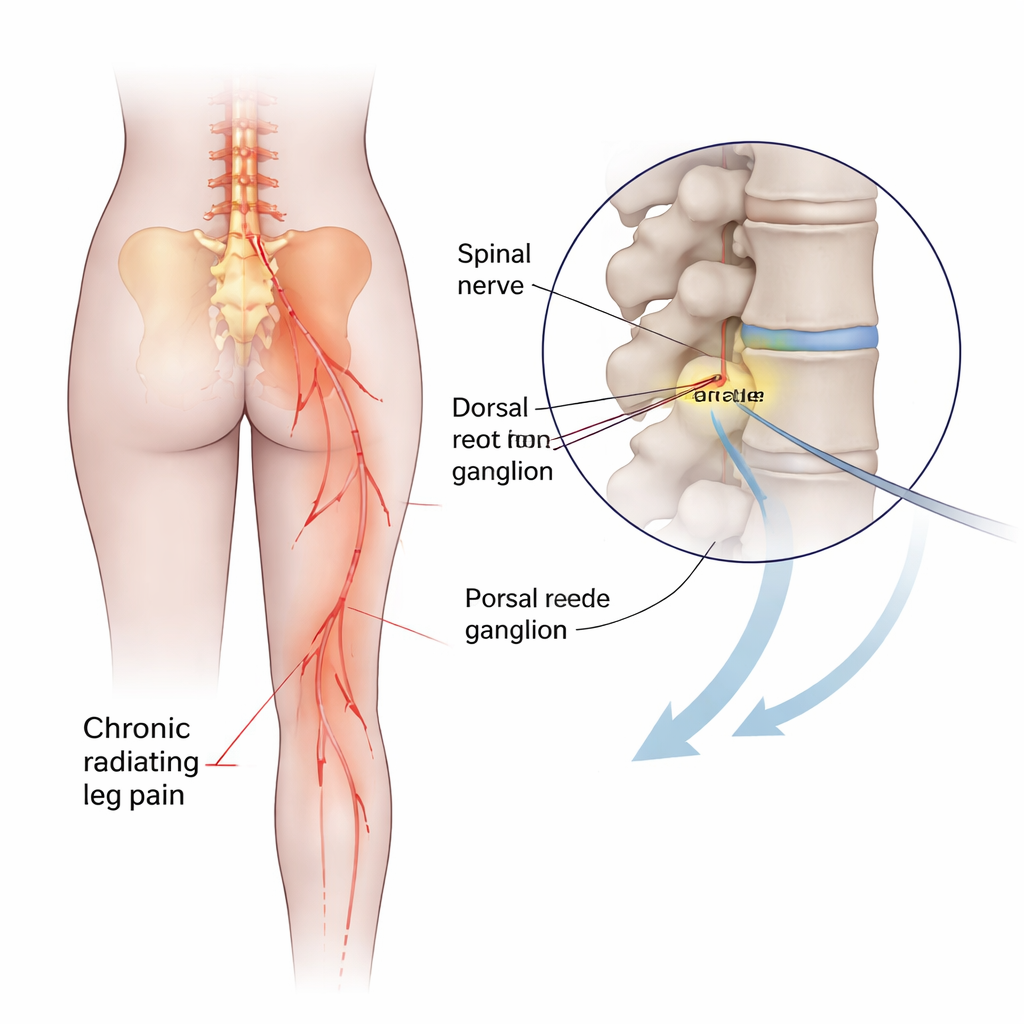
The team focused on a condition called battered sensory nerve syndrome (BSNS). In this disorder, the sensory roots and small nerve hubs (dorsal root ganglia) near the spine are chronically irritated or compressed. Patients, most of them older adults, feel burning or stabbing pain, oversensitivity to touch, tingling, and leg pain that may worsen when they move. Many had already undergone spine surgery, yet their scans no longer showed a clear target to fix. Traditional options such as more surgery or long-term pain pills often bring only partial relief and can add new problems like medication side effects, anxiety, depression, and poor sleep.
A Needle, Gentle Pulses, and Carefully Set Heat
Pulsed radiofrequency (PRF) is a minimally invasive technique in which a thin needle is guided under X-ray to the affected nerve root’s ganglion. Instead of burning the nerve, the device delivers very brief, high-voltage electrical pulses. These create a strong electric field and only mild, short bursts of heat, aiming to “reset” how the nerve transmits pain signals rather than destroying it. For BSNS, doctors already knew that using higher voltages can help, but the best temperature and treatment time were unclear. To answer this, the researchers randomly assigned 60 patients to one of four settings, all at high voltage but with two temperatures (42 °C or 55 °C) and two time lengths (3 or 12 minutes). Neither the patients, the treating doctors, nor the people measuring outcomes knew who was in which group.
What Changed for Patients Over a Year
The team followed 52 patients for up to 12 months, tracking pain scores, daily function, mood, sleep, and use of pain medications. Across all four groups, patients reported clear drops in pain intensity and disability, along with less anxiety and depression. Many reduced or stopped medications such as nerve pain drugs and anti-inflammatory pills. Importantly, there were no serious complications: no nerve damage, infections, or bleeding. Even when the temperature was raised to 55 °C, patients mainly felt a brief, tolerable warmth in the painful area, and heart rate and blood pressure remained stable during the procedure.
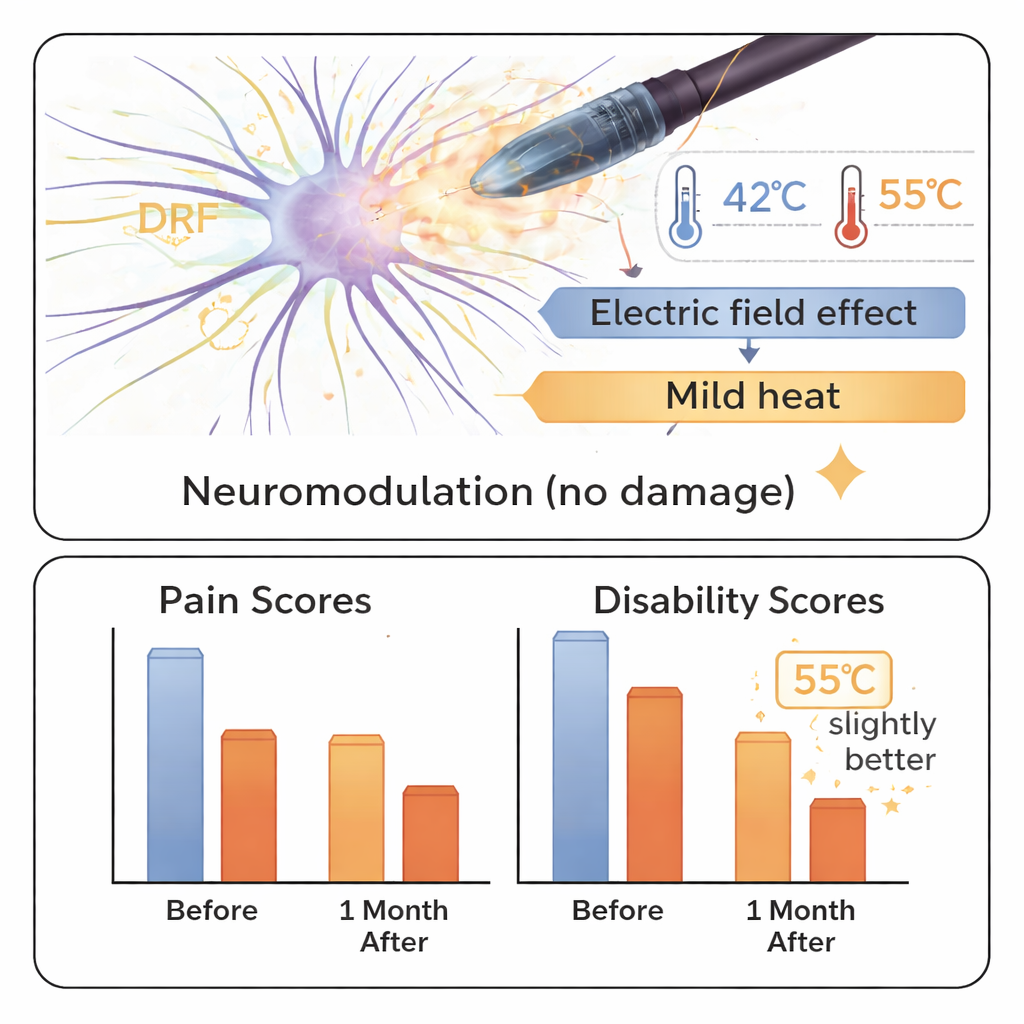
Hotter Worked Faster, Longer Did Not
When the researchers looked more closely at temperature and time, a pattern emerged. Patients treated at the higher 55 °C setting had better pain relief and greater improvement in physical function one month after treatment than those treated at 42 °C. A larger share of these patients achieved at least a 50% drop in both pain scores and disability. In contrast, stretching the treatment from 3 minutes to 12 minutes did not make a meaningful difference. The authors suggest that once the nerve has been exposed to a strong enough electric field, extra minutes may add little benefit, perhaps because the nerve has already adapted to the stimulation.
What This Means for People Living With Post‑Surgical Back Pain
For patients with stubborn nerve pain after back surgery, this study offers practical hope. A high-voltage PRF procedure targeted to the spinal nerve ganglion can significantly reduce pain and improve mobility for at least a year, without the nerve-destroying heat of traditional radiofrequency treatments. Using a slightly higher temperature of 55 °C appears to give quicker and stronger early relief, while keeping the treatment short avoids needless time in the operating room. Although larger, multi-center trials are still needed, these findings help refine how doctors can use PRF to ease chronic back- and leg-related nerve pain in a safer, more effective way.
Citation: Wang, Q., Hu, R., Han, R. et al. Effects of DRG pulsed radiofrequency parameters on the clinical outcome for battered sensory never syndrome: a prospective, triple-blind, randomized controlled trial. Sci Rep 16, 5777 (2026). https://doi.org/10.1038/s41598-026-36277-9
Keywords: chronic low back pain, nerve root pain, pulsed radiofrequency, dorsal root ganglion, failed back surgery