Clear Sky Science · en
Platelet count has a U-shaped association with all-cause mortality in COPD patients
Why Blood Platelets Matter in Lung Disease
Chronic obstructive pulmonary disease (COPD) is a long‑lasting lung condition that makes breathing difficult and often leads to repeated hospital stays. Doctors are eager to find simple tests that can flag which patients are in greater danger of dying or being readmitted to the hospital. This study asked whether a basic blood test—the platelet count—could help do just that in people hospitalized for sudden flare‑ups of COPD.
A Common Blood Test Under the Microscope
Platelets are tiny cell fragments in the blood best known for helping it clot after an injury. But they also take part in inflammation, a body‑wide process that is central to COPD. Because platelet counts are measured routinely in hospitals, they are an attractive candidate marker: cheap, fast, and already familiar to every clinician. Earlier research hinted that very high or very low platelet counts might spell trouble in various illnesses and even in the general population, but the exact risk pattern in COPD—especially during acute flare‑ups—was not well defined.
Following Patients Through and Beyond the Hospital
The researchers reviewed records from a single hospital in southwest China, identifying 853 adults admitted between 2019 and 2023 for acute exacerbations of COPD, meaning a sudden worsening of symptoms such as shortness of breath and coughing. Each person’s platelet count on the day of admission was recorded and grouped as low, normal, or high. Patients were then followed for a median of four years to see who died from any cause and who had to come back to the hospital for another COPD flare‑up. Statistical methods were used to account for age, other illnesses, and medications, so that the specific relationship between platelets and outcomes could be teased out. 
A Surprising U‑Shaped Risk Curve
When the team compared outcomes across the three platelet groups, a clear pattern emerged. Patients whose platelet counts fell in the normal range had the best long‑term survival and the lowest chance of being readmitted. Those with either low or high counts did significantly worse. Over five years, about 81 percent of patients with normal platelets were still alive, compared with 68 percent in the low‑platelet group and 59 percent in the high‑platelet group. More sophisticated analyses treating platelet count as a continuous measure showed a U‑shaped curve: risk declined as platelet counts approached roughly 200 billion cells per liter of blood, then climbed again as counts fell below or rose above that level. The same U‑shape appeared for both death and hospital readmission.
What Might Be Happening Inside the Body
The study cannot prove cause and effect, but it offers clues to possible mechanisms. High platelet counts may reflect an overactive inflammatory state or a tendency to form small clots in blood vessels of the lungs and elsewhere, both of which can worsen COPD and strain the heart. On the other end of the spectrum, very low platelet counts may signal severe underlying illness, a fragile clotting system, or side effects of medications and infections, leaving patients vulnerable to complications. The authors note that the lungs themselves are an important factory for platelets, so disturbed lung function in COPD could feed back into abnormal platelet production and behavior. 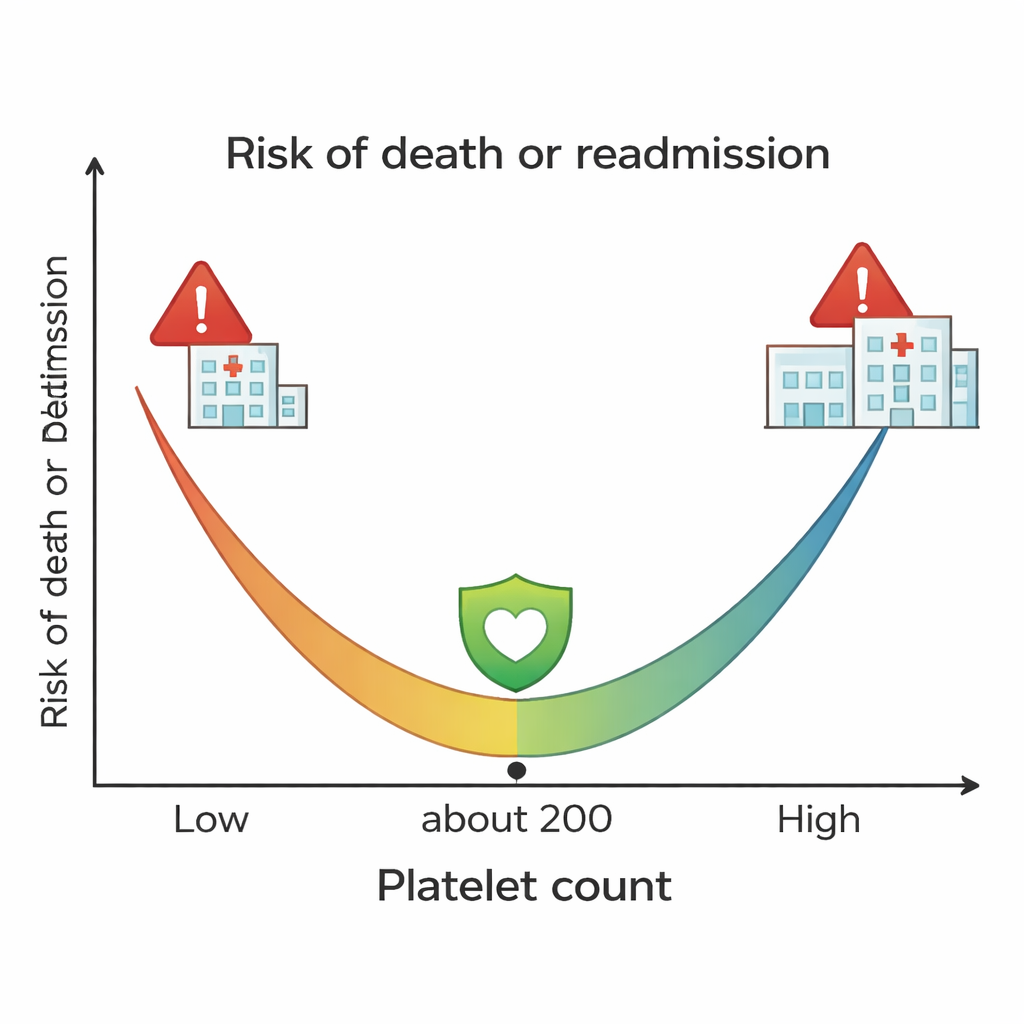
What This Means for Patients and Clinicians
For people living with COPD, the findings suggest that something as routine as a platelet count may carry valuable warning information. A count that is far below or above the usual range—especially outside a zone near 200 billion platelets per liter—could flag a higher chance of death or future hospital stays after a flare‑up. The study does not yet tell doctors to change treatments based solely on platelets, and it cannot say whether correcting low or high counts would improve outcomes. But it points to a simple tool that might help doctors sort patients by risk and decide who needs closer follow‑up or more intensive care.
Citation: Ran, J., Ran, Y., Ran, Y. et al. Platelet count has a U-shaped association with all-cause mortality in COPD patients. Sci Rep 16, 5341 (2026). https://doi.org/10.1038/s41598-026-36268-w
Keywords: COPD, platelet count, hospital readmission, mortality risk, inflammation