Clear Sky Science · en
Machine learning integrating MRI and clinical features predicts early recurrence of hepatocellular carcinoma after resection
Why early cancer comeback matters
For people who undergo surgery to remove liver cancer, one of the biggest worries is whether the disease will come back quickly. Early return of hepatocellular carcinoma—the most common type of primary liver cancer—often signals an aggressive tumor and poorer survival. Doctors would like to know, even before surgery, which patients are most likely to face an early recurrence so they can tailor follow‑up scans and extra treatments. This study explores whether artificial intelligence (AI) can combine routine blood tests, MRI scans, and tissue findings to provide that early warning signal.
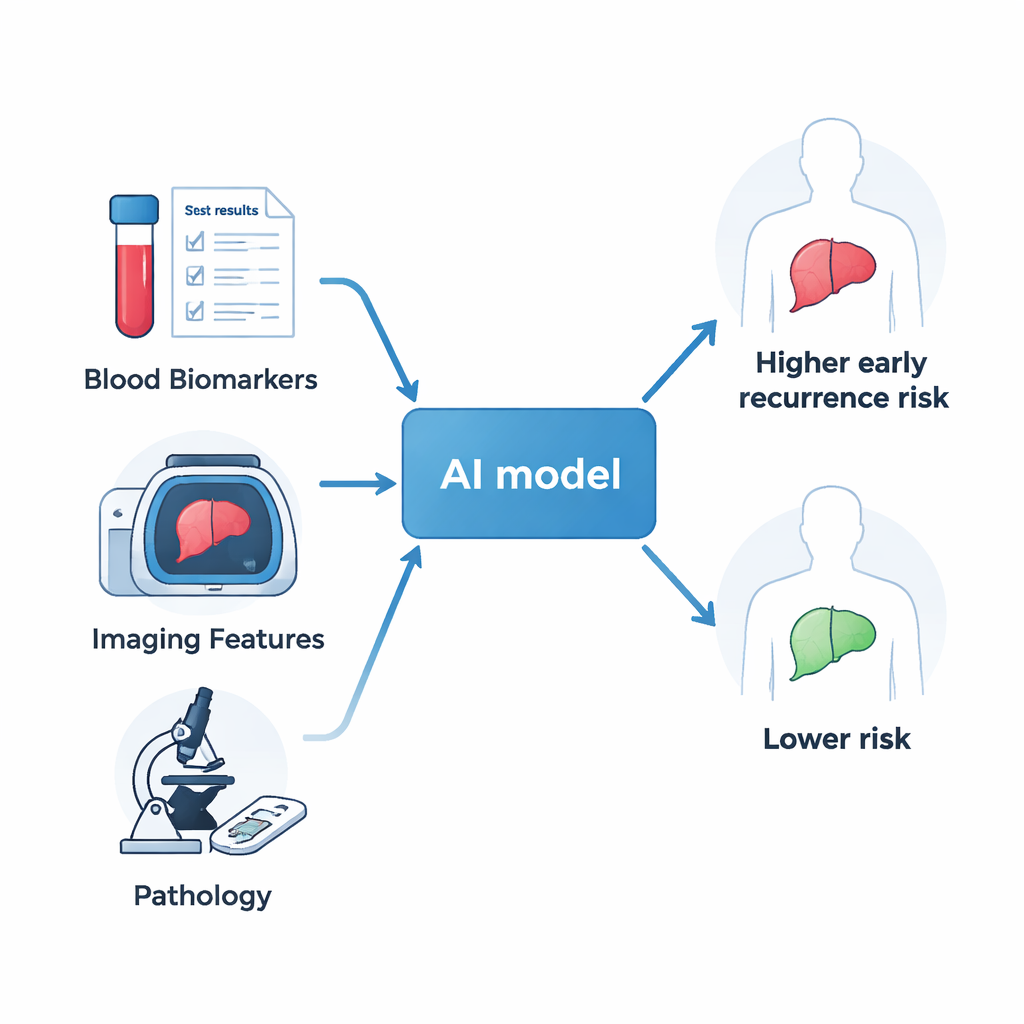
Bringing many clues together
The researchers analyzed 240 patients with liver cancer who had surgery at two hospitals in China. Before their operations, all patients had standard contrast‑enhanced MRI scans and common blood tests, and after surgery their tumors were examined under the microscope. Instead of looking at one factor at a time—such as tumor size or a single blood marker—the team fed dozens of these measurements into machine‑learning algorithms. These AI methods are designed to spot complex patterns and interactions that traditional statistical tools may miss, especially when the relationships are not simply “bigger is worse” or “higher is better.”
How the AI models were built
To avoid overloading the system, the investigators first trimmed down the long list of candidate features. They removed measurements that were almost duplicates of each other and then used a statistical technique called LASSO to select 14 of the most informative factors. With these, they trained several tree‑based machine‑learning models—ExtraTrees, XGBoost, LightGBM, and GradientBoosting—to predict whether a patient would see the cancer return within two years of surgery. The models were tuned on data from one hospital and then tested on an independent group of patients from the second hospital, a tougher check that better reflects real‑world use.
How well the models performed
Three of the AI models—ExtraTrees, XGBoost, and LightGBM—showed strong ability to distinguish between patients with and without early recurrence. In the training group, their performance scores (measured by the area under the ROC curve, or AUC) ranged from about 0.82 to 0.98, where 1.0 is perfect and 0.5 is no better than chance. In the external test group, the AUCs were a bit lower, around 0.76 to 0.79, but still indicated useful predictive power. Decision‑curve analysis, a method that estimates whether a model would actually help doctors make better choices, suggested that using these AI tools could provide more benefit than treating all patients the same way or relying on chance. Overall, the models appeared reasonably accurate and clinically meaningful.
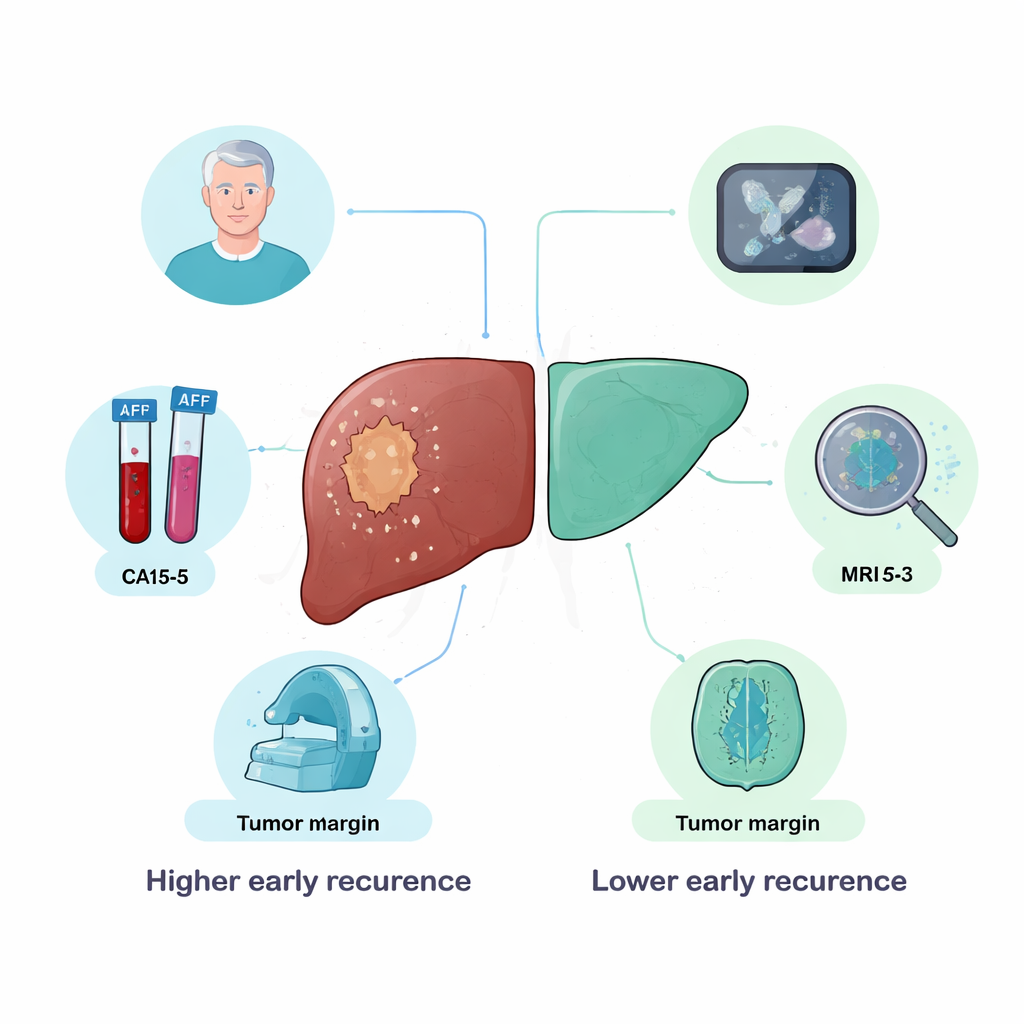
What drove the predictions
By examining which inputs the models relied on most, the study offers insight into what seems to matter for early relapse. Two blood markers—AFP, long used in liver cancer care, and CA15‑3, more familiar from breast cancer—consistently ranked among the most influential features. MRI signs of an irregular, non‑smooth tumor margin were strongly tied to early recurrence, echoing prior work linking jagged tumor outlines to more invasive behavior and hidden spread within the liver. Age also played a role, with younger patients surprisingly more likely to have early recurrence, probably reflecting more aggressive tumor biology in this group. Microscopic features such as small clusters of cancer cells in tiny blood vessels further supported the AI’s risk estimates.
What this means for patients and doctors
For a person facing liver cancer surgery, the models described in this study do not replace a doctor’s judgment, but they could offer an extra layer of guidance. By combining information that is already collected in routine care—blood tests, MRI findings, and standard pathology—the AI tools can flag patients at higher risk of early relapse. Those individuals might benefit from closer imaging follow‑up, more frequent blood checks, or consideration of additional treatments after surgery. Because the study was retrospective and limited to two centers in one region, the authors emphasize that larger, forward‑looking trials are needed before such models become standard. Still, the work points toward a future where AI helps doctors personalize surveillance and therapy, with the goal of catching returning liver cancer earlier and improving long‑term outcomes.
Citation: Feng, L., Luo, N., Ruan, F. et al. Machine learning integrating MRI and clinical features predicts early recurrence of hepatocellular carcinoma after resection. Sci Rep 16, 5653 (2026). https://doi.org/10.1038/s41598-026-36261-3
Keywords: liver cancer, machine learning, MRI, tumor recurrence, blood biomarkers