Clear Sky Science · en
Two paired HPV-59 cervical cancer cell lines with distinct chemoradioresistant phenotypes
Why this research matters to patients
Cervical cancer remains one of the leading causes of cancer death in women, and many patients receive a combination of chemotherapy and radiation. Yet some tumors learn to survive these powerful treatments, coming back stronger and harder to cure. This study follows one young woman’s tumor over time and turns her cancer cells into two living laboratory models, created before and after therapy, to reveal how resistance to treatment can emerge and how future drugs might be tested more realistically.
Following one tumor through treatment
The researchers worked with 45 cervical tumor samples but were only able to grow long-lasting cultures from one patient: a 22-year-old woman with advanced squamous cell carcinoma of the cervix. From her, they established two permanent cell lines. The first, called AdMer35, came from a biopsy taken before she received chemoradiotherapy. The second, AdMer43, was created from a biopsy taken several months later, after two courses of radiation and chemotherapy with paclitaxel and carboplatin. Both cell lines kept the appearance of epithelial cells, the type that lines the cervix, and both carried DNA from the same high‑risk human papillomavirus strain, HPV‑59, a relatively rare type in existing research models. 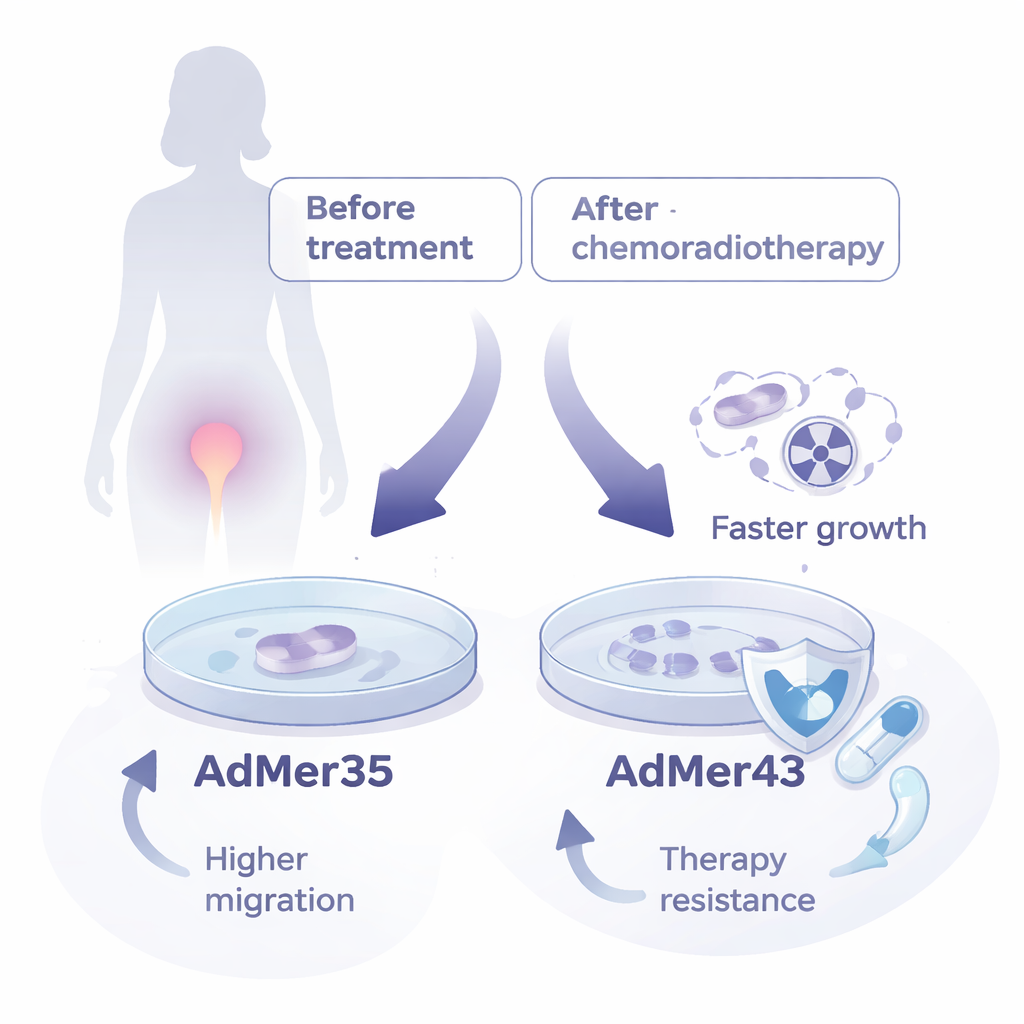
Same origin, different behaviors
Although AdMer35 and AdMer43 share a common patient and viral origin, they behave quite differently in the lab. AdMer43 divides more quickly, reaching higher growth levels than AdMer35 in real‑time monitoring tests, and shows stronger staining for Ki‑67, a protein linked with active cell proliferation. AdMer35, in contrast, migrates across surfaces faster, hinting at a greater ability to invade nearby tissues. Chromosome studies showed that the two lines have different abnormal chromosome counts, reflecting the genetic chaos typical of cancers but also underscoring that they represent distinct branches of the same tumor’s evolution.
How the cells handle radiation and drugs
The key question was how these sister lines respond to the treatments the patient actually received. When exposed to a clinically relevant dose of X‑rays, AdMer35 slowed its growth sharply over several days, showed an increase in cells pausing in the G2/M stage of the cell cycle—a checkpoint for DNA damage—and displayed more signs of programmed cell death. In contrast, AdMer43 kept proliferating almost as well as non‑irradiated cells, showed little or no cell‑cycle arrest, and only minimal apoptosis. A similar pattern appeared with chemotherapy: higher doses of carboplatin and paclitaxel were required to kill half of the AdMer43 cells compared with AdMer35, indicating reduced drug sensitivity. In essence, the post‑treatment line, AdMer43, had acquired a more durable, chemoradioresistant personality.
Testing tumor growth in animals
To see how these differences play out in a living organism, the scientists implanted both cell lines under the skin of immunodeficient mice. Both AdMer35 and AdMer43 formed tumors, proving that each line is capable of driving cancer growth. Tumors from AdMer35 generally grew larger and seemed more locally aggressive, consistent with this line’s strong migration ability in cell culture. AdMer43 tumors were smaller but showed a high fraction of cells positive for Ki‑67, indicating intense cell division, and contained more supporting connective tissue. Together, these features suggest that AdMer35 may be better at spreading through tissue, while AdMer43 excels at sustained proliferation once established. 
A new tool to study and outsmart resistance
For non‑specialists, the main takeaway is that the authors have built a rare “before‑and‑after” model of the same cervical cancer as it passes through real‑world therapy. AdMer35 represents the tumor as it initially presented; AdMer43 captures a later, more treatment‑hardened version that shrugs off radiation and standard drugs. Because both lines preserve the patient’s original HPV‑59 infection and tumor traits, they offer a powerful way to dissect how cancer cells adapt under therapeutic pressure and to test new combinations of treatments designed to prevent or overcome resistance. Ultimately, insights gained from such paired models could help clinicians keep cervical cancers from rebounding after therapy, improving long‑term survival for future patients.
Citation: Tatarnikova, I., Talyshev, V., Sen’kova, A. et al. Two paired HPV-59 cervical cancer cell lines with distinct chemoradioresistant phenotypes. Sci Rep 16, 7307 (2026). https://doi.org/10.1038/s41598-026-36260-4
Keywords: cervical cancer, chemoradioresistance, HPV-59, cancer cell lines, therapy resistance