Clear Sky Science · en
Functional competency of a novel 2-ply vacuum-pressed biological scaffold for entire posterior mitral valve reconstruction
Why fixing a tiny heart valve matters
The mitral valve is a small but vital gateway that lets blood flow in one direction through the heart. When it leaks badly, people can become short of breath, tired, and at risk of heart failure. Surgeons usually try to repair this valve instead of replacing it with an artificial one, because keeping as much natural tissue as possible tends to give better long‑term results. But when the back part of the valve is badly damaged, repair can be very difficult. This study explores a new kind of soft biological patch that might let surgeons rebuild that damaged section while preserving the rest of the patient’s own valve.
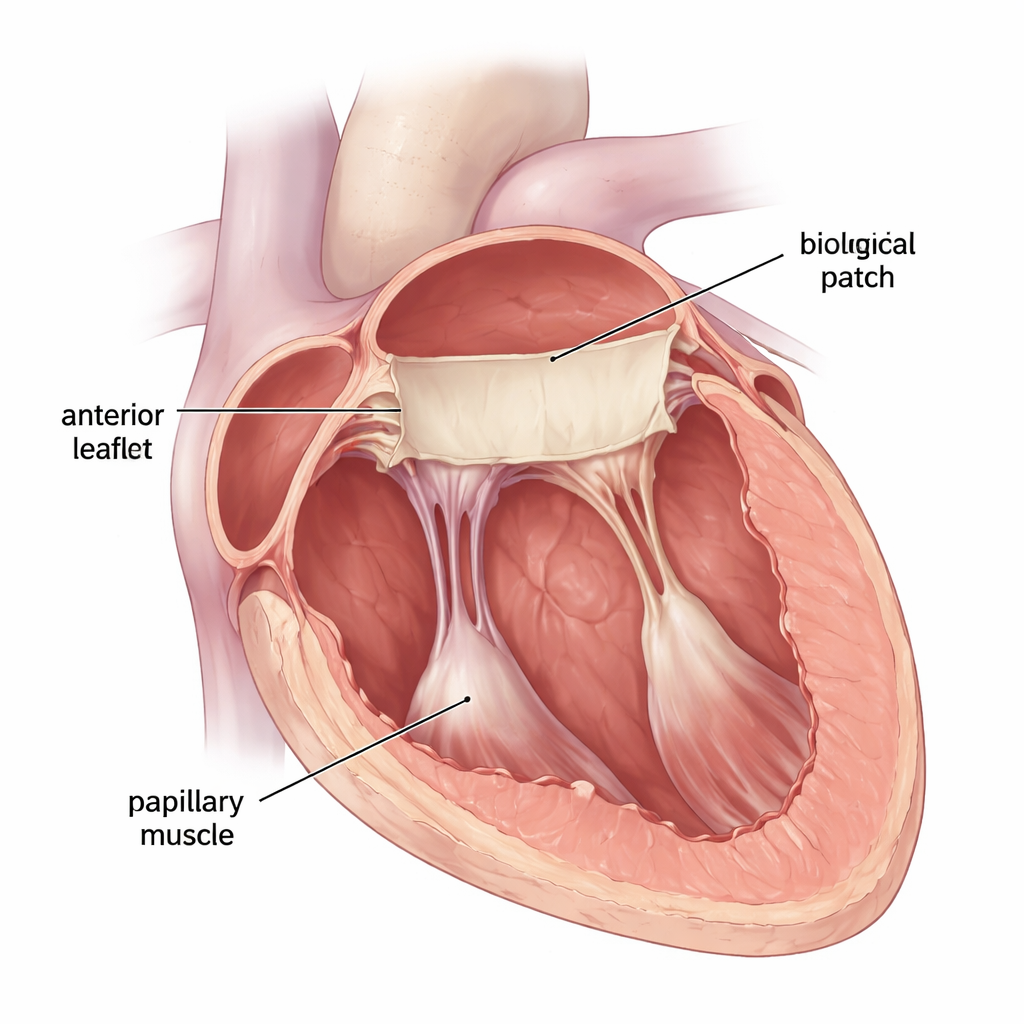
A new living patch for a worn-out heart flap
The researchers focused on the posterior leaflet, the back flap of the mitral valve, which often suffers the most from disease or calcification. Instead of removing the whole valve and sewing in an artificial replacement, they tested a custom‑shaped patch made from pig small intestine tissue, specially cleaned to leave only a supportive scaffold. This material, known as an extracellular matrix bioscaffold, has been used in other heart surgeries and can gradually be repopulated by the body’s own cells. The team used a stronger, “vacuum‑pressed” two‑layer version of this material, which had previously shown better tear resistance than an older freeze‑dried form. The goal was to see whether this patch could stand up to real heartbeats while replacing the entire posterior leaflet and its supporting cords.
Testing the patch in beating hearts
The study was carried out in seven healthy pigs, whose hearts are similar in size and shape to human hearts. In each animal, surgeons opened the heart, removed the native posterior leaflet and its supporting strings, and replaced them with a pre‑shaped bioscaffold patch anchored to the valve ring and to the papillary muscles in the ventricle. The front leaflet of the valve was left untouched. The pigs served as their own controls: measurements were taken before surgery and again after the repair, including ultrasound scans of the valve, pressure readings in the heart chambers, and precise tracking of valve-ring motion using tiny implanted sensors.
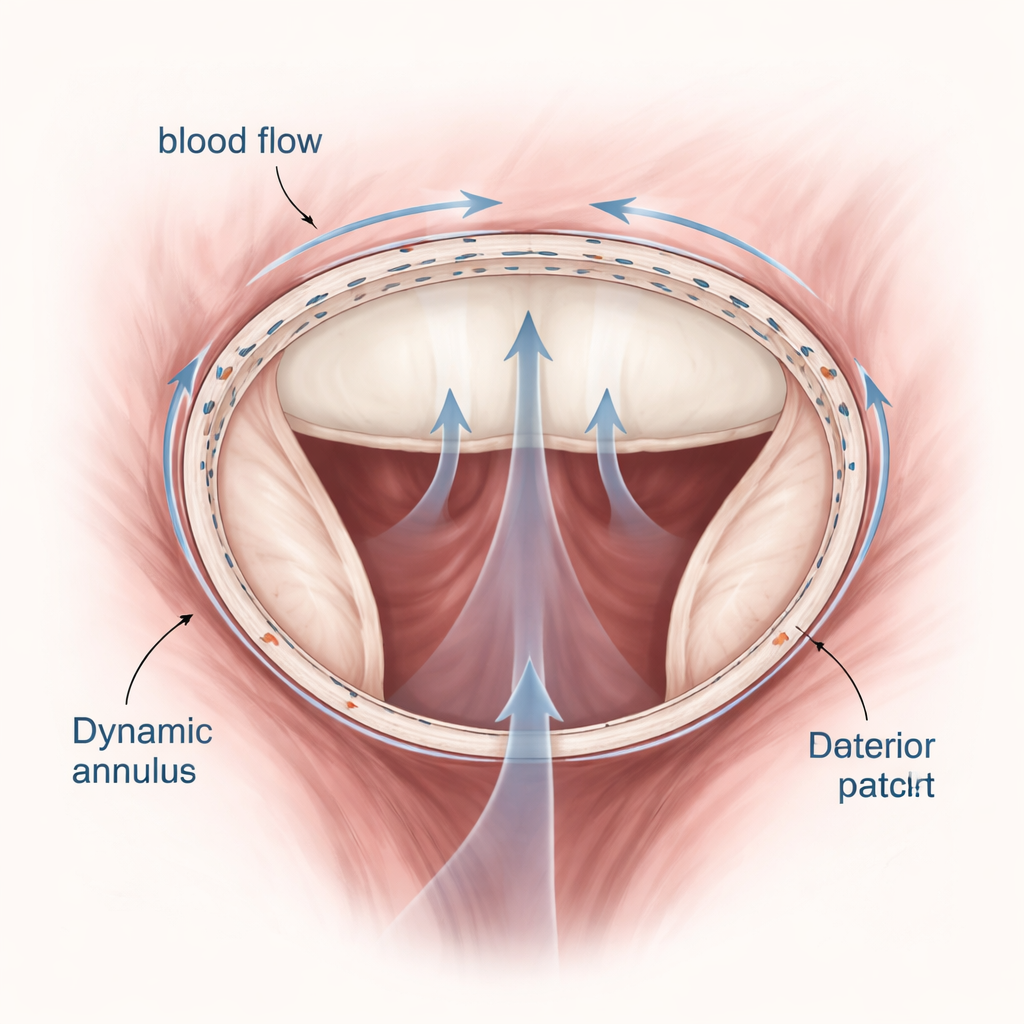
How well did the rebuilt valve work?
After the operation, the reconstructed valves functioned effectively in all animals. Pressures in the left atrium and across the valve stayed essentially unchanged, showing no signs of new leakage or narrowing. Ultrasound images confirmed that blood flowed smoothly through the valve and that the front leaflet moved normally. The patch itself provided a slightly longer back leaflet and a larger contact zone where the two leaflets meet, which can help prevent leakage. Measurements from the implanted sensors showed that the overall size and motion of the valve ring and the deeper supporting structures remained close to natural behavior, meaning the patch did not disrupt the heart’s normal pumping mechanics.
Subtle shape changes and remaining challenges
Although the main function was preserved, the new design was not perfect. The back leaflet made from the patch tended to bend slightly toward the atrium during heartbeat, likely because it had more tissue and fewer supporting cords than a native leaflet. The back portion of the valve ring also widened instead of tightening slightly during contraction, creating a kind of ballooning effect. These shape changes did not cause immediate problems in this short‑term experiment, but they could alter blood flow patterns or stress on the patch over time. The study also could not assess longer‑term issues such as clot formation, tissue overgrowth, or how well the scaffold becomes integrated with the heart’s own cells.
What this means for future heart repairs
For patients whose posterior mitral leaflet is too damaged for conventional repair, this study suggests that a carefully tailored biological patch could someday offer an alternative to full valve replacement. In pig hearts, the new two‑layer vacuum‑pressed scaffold allowed surgeons to rebuild the entire back leaflet while keeping normal pressures, smooth blood flow, and natural motion of the deeper heart structures—at least in the short term. However, because the experiments were done in healthy animals and observed only shortly after surgery, further work in long‑term and disease‑based models is needed. If future studies confirm its durability and safety, this kind of living scaffold patch could expand the options for gentle, tissue‑preserving heart valve surgery.
Citation: Jedrzejczyk, J.H., Andersen, F.T., Kaspersen, A.E. et al. Functional competency of a novel 2-ply vacuum-pressed biological scaffold for entire posterior mitral valve reconstruction. Sci Rep 16, 5233 (2026). https://doi.org/10.1038/s41598-026-36236-4
Keywords: mitral valve repair, biological scaffold, heart valve surgery, extracellular matrix patch, porcine model