Clear Sky Science · en
Impact of iron chelation therapy on thyroid function in beta-thalassemia major patients from Pakistan
Why this matters for families and patients
For thousands of children and young adults living with transfusion-dependent beta-thalassemia, regular blood transfusions are lifesaving—but they come with a hidden cost: excess iron slowly builds up in the body and can silently damage vital organs. This study from Pakistan asks a simple but crucial question for these patients and their families: can medicines that remove extra iron also protect the tiny thyroid gland in the neck, which controls energy, growth, and overall well-being?
Too much iron, too much strain on the body
People with transfusion-dependent beta-thalassemia need frequent blood transfusions because their bodies cannot make healthy hemoglobin on their own. Over time, each unit of blood adds more iron than the body can naturally get rid of. This iron settles in organs such as the liver, heart, kidneys, and hormone-producing glands—including the thyroid. When the thyroid is overloaded with iron, it may stop making enough hormones, leading to hypothyroidism. This condition can cause tiredness, weight gain, feeling cold, poor growth in children, and other long-term health problems that further burden patients who are already medically fragile.
How the study was carried out
Researchers in Mardan, Pakistan, studied 200 patients with beta-thalassemia major who regularly received blood transfusions. Half of them had been taking iron-removing medicines, known as iron chelation therapy, for at least six months. These drugs—deferasirox, deferoxamine, and deferiprone—bind excess iron so the body can excrete it. The other half of the patients had not yet received any chelation treatment. The team collected detailed medical histories and blood samples, measuring thyroid hormones (free T3 and free T4), thyroid-stimulating hormone (TSH), iron stores in the body (serum ferritin), and markers of liver and kidney health. They then compared the results between patients who were on chelation and those who were not.
Clear differences in thyroid health
The contrast between the two groups was striking. Patients receiving iron chelation had thyroid hormone levels mostly within the normal range and TSH values close to what is expected in healthy individuals. In the group without chelation, thyroid hormones were much lower and TSH levels were more than three times higher, a pattern strongly pointing to underactive thyroid glands. When the researchers looked at thyroid status as simple categories, nearly nine out of ten patients without chelation showed some degree of hypothyroidism, while almost eight out of ten patients on chelation had normal thyroid function. Among the chelating drugs, deferasirox stood out as being linked to the lowest TSH levels, suggesting better protection of the thyroid.
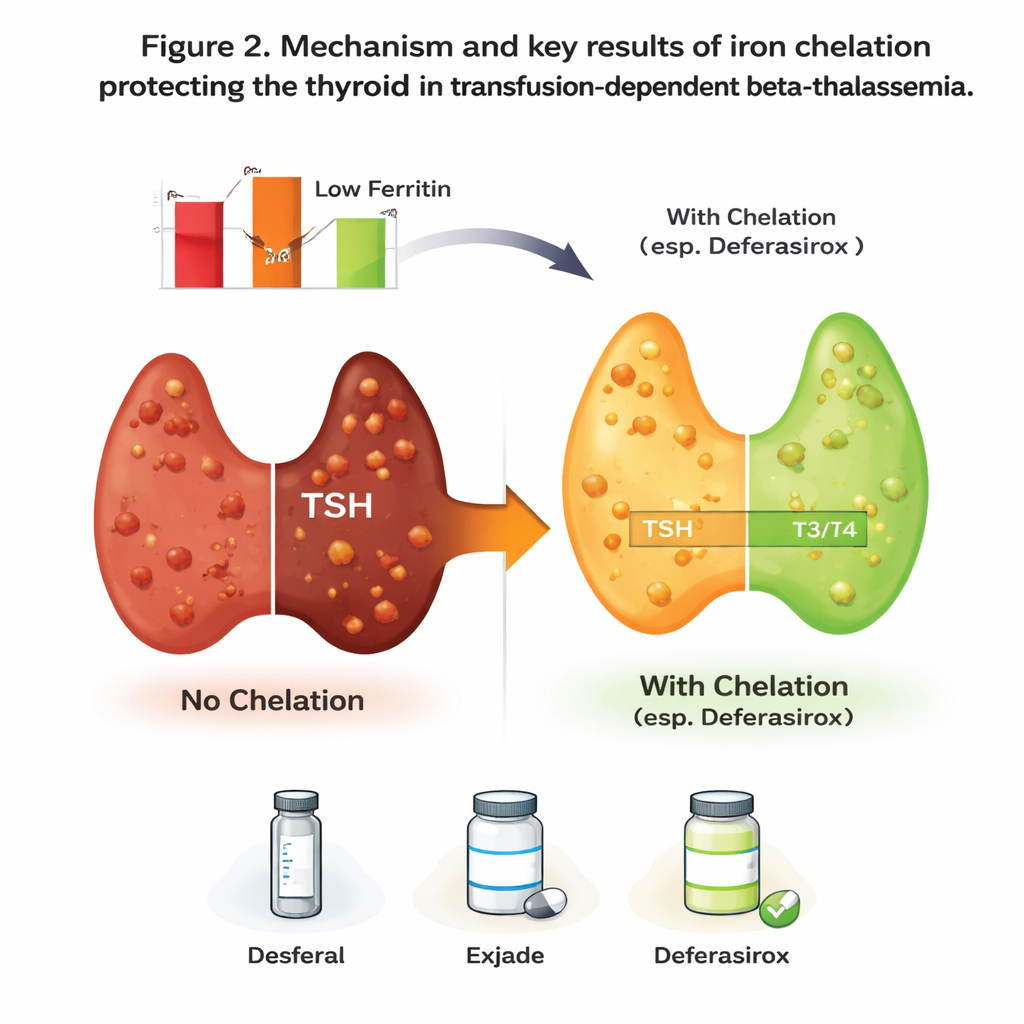
Iron levels as a key warning signal
Beyond comparing groups, the study examined how tightly iron levels were connected to thyroid problems. Serum ferritin, a common blood test that reflects the body’s iron load, showed a very strong relationship with TSH: the higher the ferritin, the higher the TSH, and the greater the chance of thyroid trouble. Even after taking into account age, sex, type of chelation drug, and transfusion frequency, ferritin remained the only independent predictor of TSH. In simple terms, this means that the amount of stored iron appears to be the main driver of thyroid strain. Importantly, patients on chelation not only had better thyroid results but also healthier liver and kidney tests, underscoring that controlling iron benefits the whole body.
What this means for care and daily life
For families and clinicians managing beta-thalassemia, these findings deliver a practical message: sticking with effective iron-removing treatment, particularly deferasirox when appropriate, may greatly lower the risk of thyroid damage and other organ complications. Regular checks of ferritin levels and routine thyroid screening can catch trouble early, before symptoms become severe. While this study cannot prove cause and effect because it captured a single moment in time, it strongly supports making iron control and thyroid monitoring central parts of long-term thalassemia care—especially in countries like Pakistan, where the disease is common and medical resources are limited.
Citation: Shah, A.W.A., Shams, S., Khan, M.J. et al. Impact of iron chelation therapy on thyroid function in beta-thalassemia major patients from Pakistan. Sci Rep 16, 7533 (2026). https://doi.org/10.1038/s41598-026-36200-2
Keywords: beta thalassemia, iron overload, iron chelation therapy, thyroid function, hypothyroidism