Clear Sky Science · en
Differential brain reorganization in chronic cervical spinal cord injury and its relation to motor versus sensory impairments: a preliminary investigation
Why this matters for people living with paralysis
When the spinal cord is injured in the neck, messages between the brain and the body are disrupted, often leaving people with weakness, loss of feeling, and long-term dependence on others. Yet the brain does not simply shut down; it reorganizes. This study uses advanced MRI scans to ask a practical question with big implications: do problems with movement and problems with sensation after chronic cervical spinal cord injury come from different patterns of brain change—and could understanding those patterns point to more personalized rehabilitation?
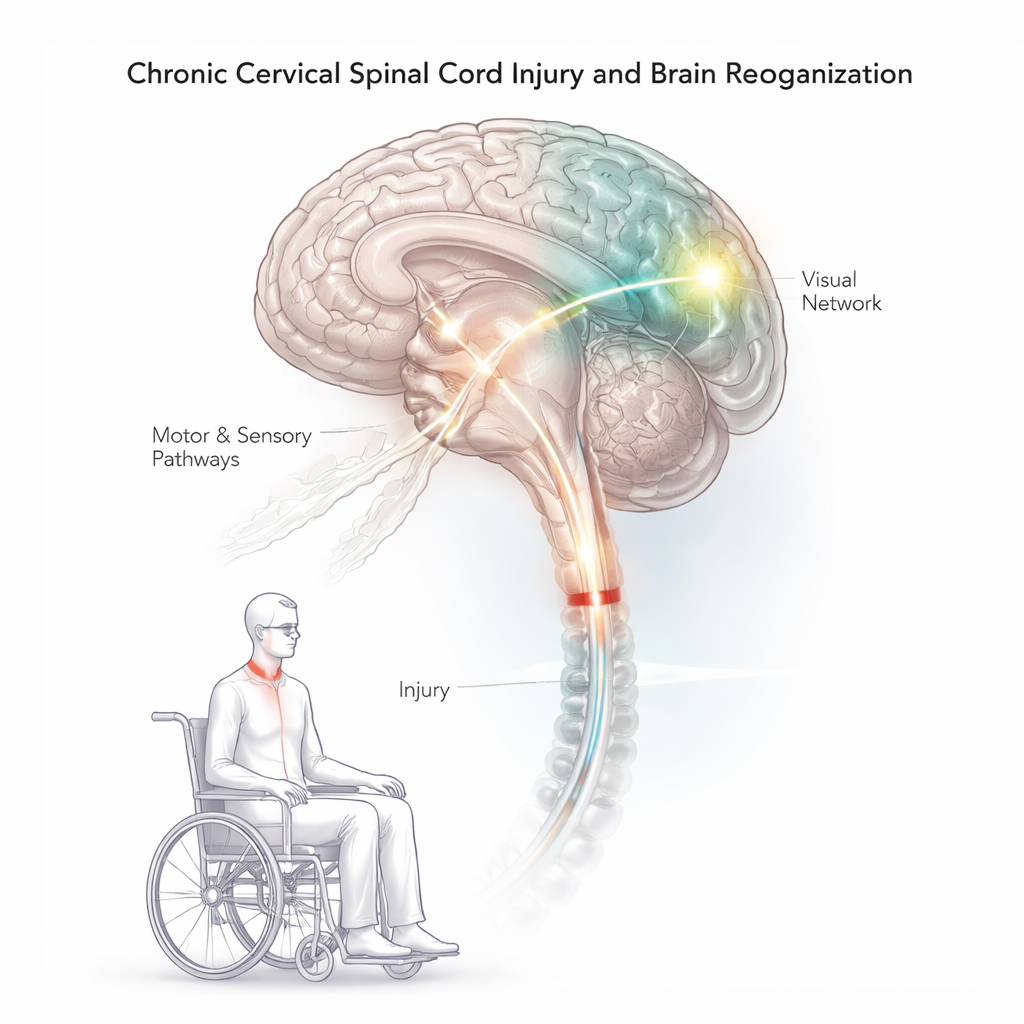
Looking inside the brains of people with spinal cord injury
The researchers studied 12 adults with chronic traumatic spinal cord injuries in the neck region and compared them with 12 similar adults without injury. All participants underwent detailed brain scans while resting in the MRI scanner. The team measured brain structure (cortical thickness and gray matter volume) and how different brain regions “talk” to each other at rest, a measure called resting-state functional connectivity. For the spinal cord injury group, arm and hand function was carefully tested with a clinical tool known as GRASSP, which separately scores strength, touch and feeling, and how well a person can grasp and manipulate objects.
How the injured brain’s communication network changes
Compared with uninjured volunteers, people with chronic cervical spinal cord injury showed widespread changes in how brain areas communicate. Connections between key movement and touch regions in the brain (sensorimotor areas) and many other areas—including frontal regions involved in planning and attention, and back-of-the-brain regions involved in vision and spatial awareness—were often weaker. However, some connections became stronger. For example, certain sensory regions showed increased communication with deep brain structures and the cerebellum, which helps coordinate movement and balance. These mixed patterns suggest the brain is both losing some normal pathways and strengthening alternative routes.
Different brain patterns for movement versus sensation problems
By relating MRI findings to GRASSP scores, the team found that movement and sensory impairments were tied to different communication patterns. Individuals who retained better arm strength and hand use tended to show stronger connections between sensorimotor areas and visual and visuospatial regions, as well as with some deep structures such as the pallidum and nucleus accumbens. In contrast, better sensory scores were linked to a different set of changes—for instance, altered connectivity between primary motor areas and the thalamus, a major relay station, and between primary sensory areas and specific visual and association regions. In short, people who moved better and people who felt better were relying on partly distinct rewired networks.
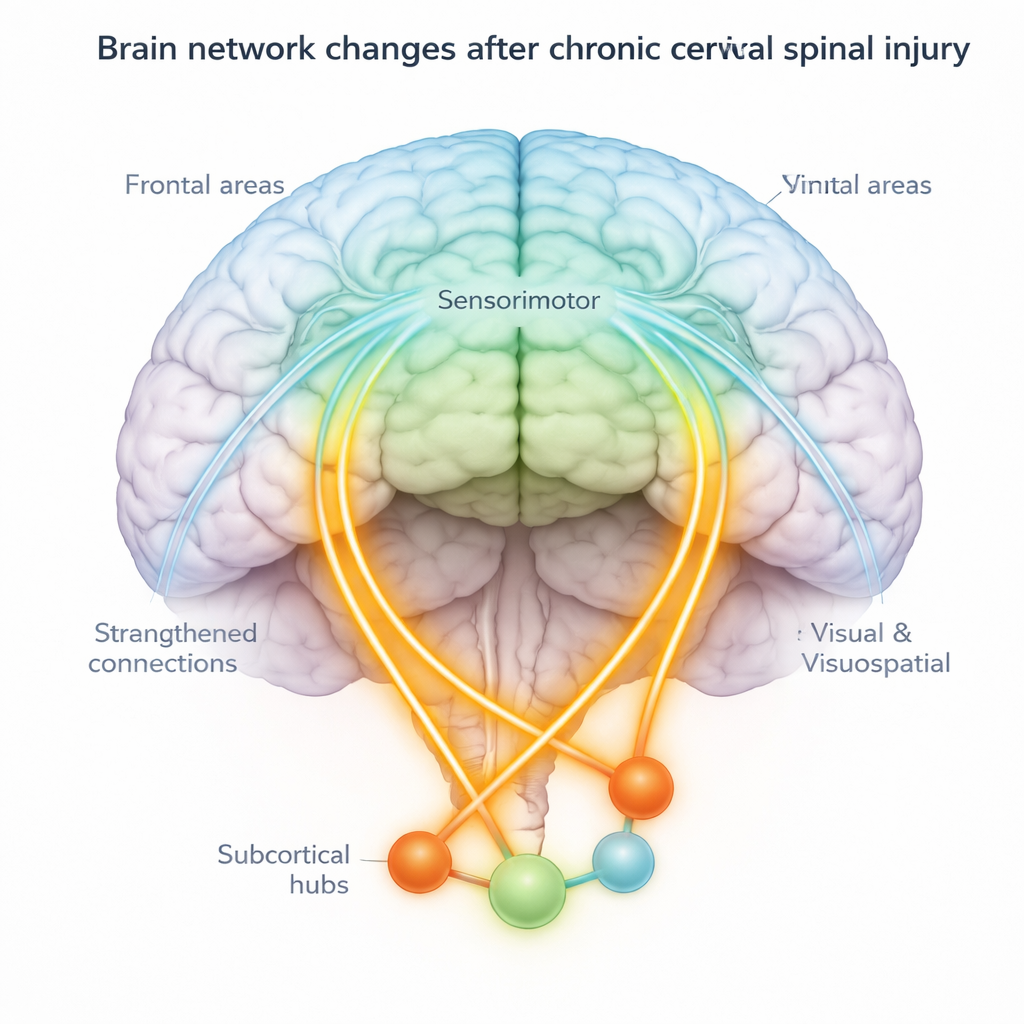
Physical changes in brain tissue go along with network shifts
Functional changes were mirrored by structural ones. The spinal cord injury group showed thinning of some motor and frontal areas and parts of the parietal and visual cortices, which may reflect loss of input and disuse over years. At the same time, some deep structures—including the thalamus, putamen, and parts of the cerebellum—were larger in volume, hinting at long-term remodeling. Notably, some regions that changed in connectivity, such as the thalamus and putamen, also showed these tissue differences, strengthening the idea that anatomy and communication are jointly reshaped after injury.
What this means for future therapies
For a layperson, the central message is that the brain’s response to spinal cord injury is not one-size-fits-all. Long after the initial trauma, the brain reorganizes in different ways depending on whether movement or sensation is more affected. Visual and visuospatial areas—traditionally thought of as "seeing" regions—emerge as key partners helping the brain compensate, especially in people who regain better hand strength and function. This suggests that therapies that actively engage vision and spatial processing, such as virtual reality, visually guided training, or brain stimulation targeting these networks, may enhance recovery. Multimodal MRI, as used here, could help match the right combination of interventions to each person’s unique pattern of brain reorganization.
Citation: Brihmat, N., Saleh, S., Zhang, F. et al. Differential brain reorganization in chronic cervical spinal cord injury and its relation to motor versus sensory impairments: a preliminary investigation. Sci Rep 16, 7108 (2026). https://doi.org/10.1038/s41598-026-36187-w
Keywords: spinal cord injury, brain plasticity, functional connectivity, visuospatial networks, motor and sensory function