Clear Sky Science · en
Selection of joint replacement methods based on AI cartilage model
Smarter Choices for Aching Knees
For many older adults, knee pain from arthritis can turn everyday tasks—like climbing stairs or walking to the store—into painful challenges. Surgeons can replace damaged parts of the knee in different ways, but choosing the right type of surgery is not always straightforward. This study explores how an artificial intelligence (AI) model built from MRI scans of knee cartilage can help doctors decide between two common operations and, in turn, improve patients’ recovery and quality of life.
Two Different Ways to Fix a Worn-Out Knee
When knee cartilage wears down, surgeons usually consider two main options. Total knee arthroplasty (TKA) replaces the entire knee joint surface, while unicompartmental knee arthroplasty (UKA) replaces only the damaged section—often the inner (medial) side—leaving healthy areas intact. TKA is more extensive but can better correct severe deformity and widespread damage. UKA is more limited but usually involves a smaller incision, less bone removal, and a more “natural” feeling knee. The challenge is identifying which patients truly need a full replacement and which can safely benefit from the smaller operation.
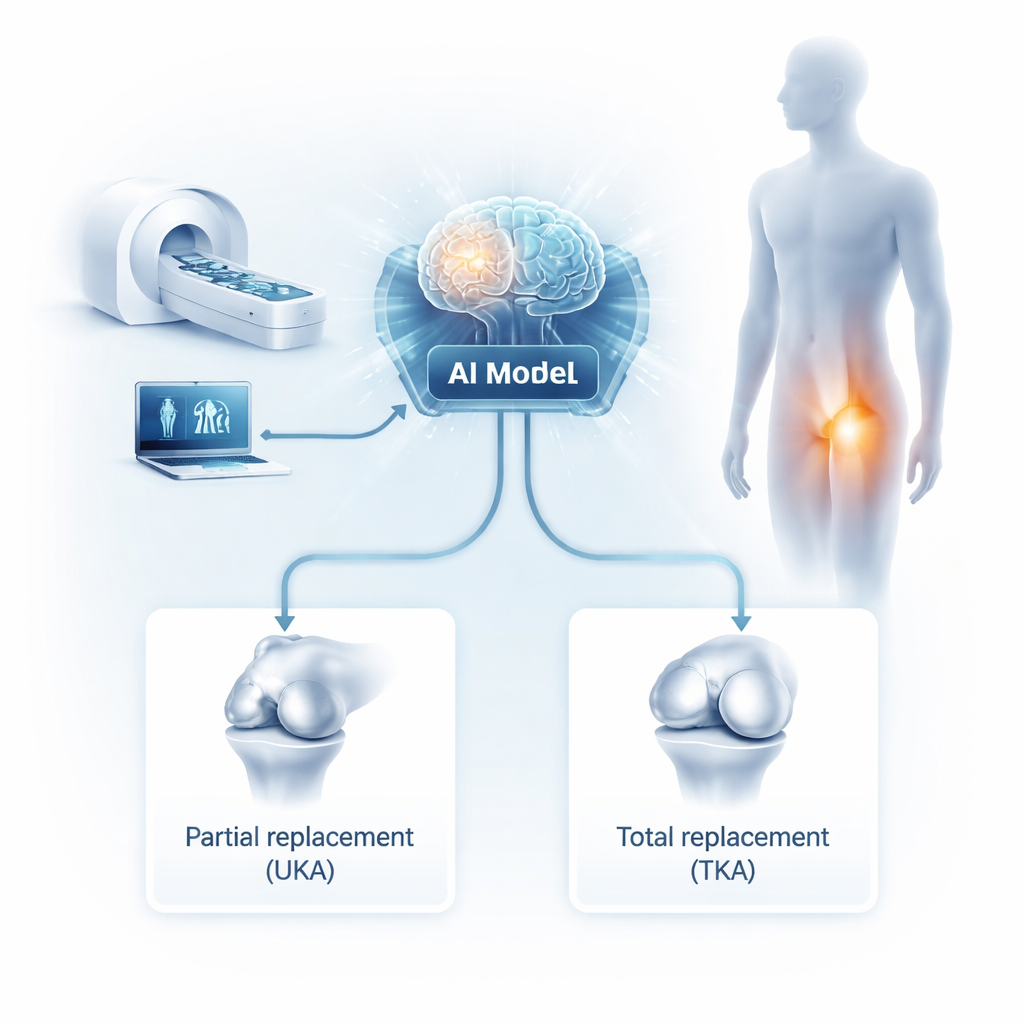
How AI Reads Cartilage Damage
In this study, 80 patients with advanced knee osteoarthritis underwent high-resolution MRI scans of the affected knee. These images were processed by an AI-based reconstruction system that built a three-dimensional model of 15 structures, including bones, cartilage, and key ligaments. The AI model could clearly show where cartilage was completely missing—a sign of severe damage. If the damage was limited to the inner side of the knee, surgeons chose the partial replacement (UKA). If severe damage extended to the outer side or the kneecap area, surgeons opted for a total replacement (TKA). In other words, the AI model acted as an objective “map” of damage to guide which operation best matched each patient’s knee.
Comparing Pain Relief and Daily Function
After surgery, the researchers followed patients for a year, tracking pain scores, knee function, stiffness, and walking ability at 1, 3, 6, and 12 months. Both groups improved a lot compared with their pre-surgery state: pain dropped, movement increased, and daily tasks became easier. However, patients who had the partial replacement generally recovered faster at the beginning. At one month, they had higher knee function scores and reported less pain than those who had a total replacement. These early gains likely reflect the smaller surgical trauma and the preservation of more normal joint structures in UKA. By six to twelve months, though, overall pain and function were similar between the two groups, showing that both operations can deliver strong long-term benefits when well chosen.
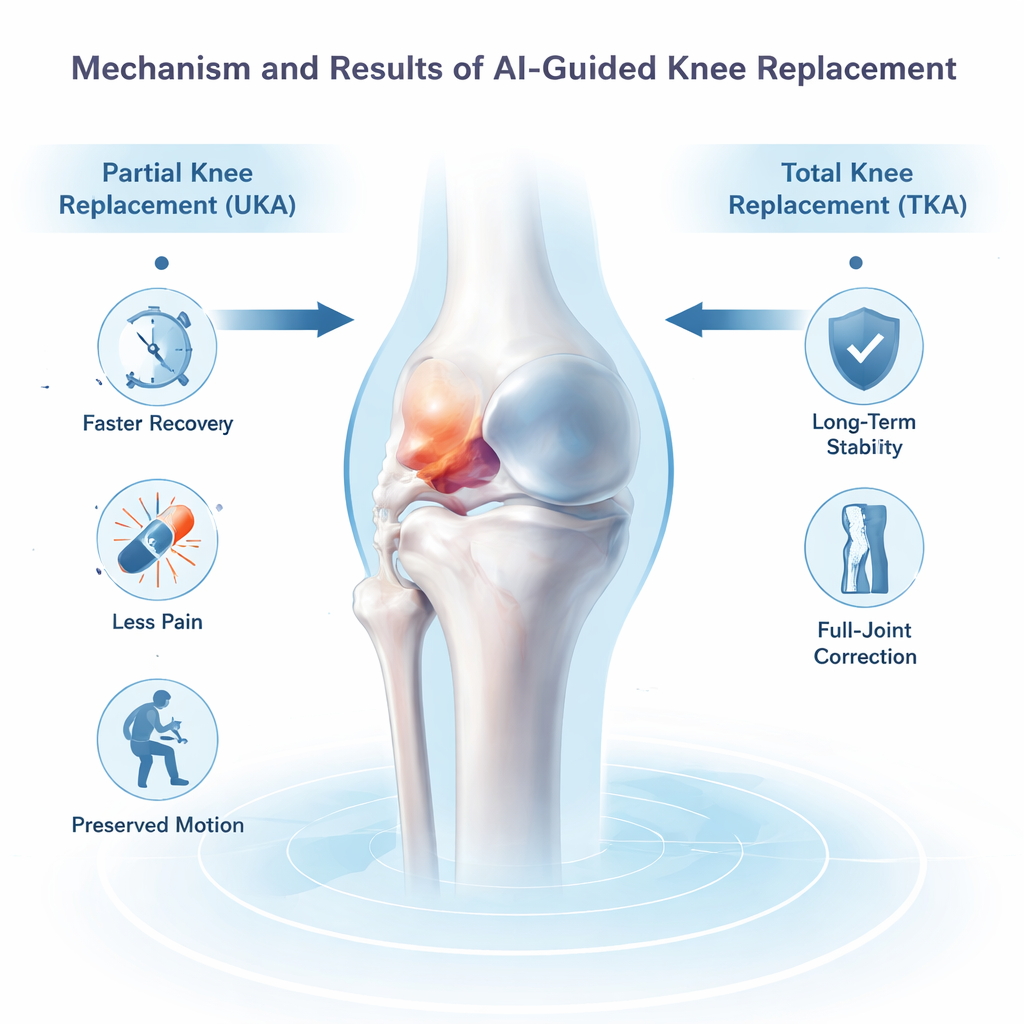
Alignment, Motion, and Long-Term Stability
The study also looked at how well each procedure straightened the leg and restored knee motion. Total knee replacement achieved a larger correction in the angle of the leg from hip to ankle, making it especially useful for patients with more severe deformity. Partial replacement changed this angle less, which fits its role in treating localized damage in an otherwise reasonably aligned knee. In terms of bending and straightening the knee, both groups improved, but UKA patients started with better motion and kept an edge after a year. The authors note that TKA may offer more stable alignment over time for knees with widespread damage, while UKA can deliver a more natural-feeling joint for carefully selected patients.
What This Means for Patients with Knee Arthritis
For people living with severe knee arthritis, the main question is not just “Do I need surgery?” but “Which surgery is right for my knee?” This research suggests that AI-built 3D cartilage models from MRI scans can help answer that question more precisely. By clearly showing where cartilage is missing, the AI tool helps surgeons avoid doing a full replacement when a partial one would suffice, potentially giving patients faster early recovery and less pain. At the same time, it flags knees with more extensive damage that truly need a total replacement to achieve better long-term stability. Although the study has limits, such as a modest sample size and differences in age between groups, it points toward a future in which personalized, image-guided decisions can make knee replacement safer, less invasive, and better matched to each patient’s needs.
Citation: Zhang, W., Gao, H., Zhao, B. et al. Selection of joint replacement methods based on AI cartilage model. Sci Rep 16, 5709 (2026). https://doi.org/10.1038/s41598-026-36186-x
Keywords: knee osteoarthritis, AI medical imaging, knee replacement surgery, cartilage damage, joint preservation