Clear Sky Science · en
Therapeutic effects of vitamin D and intermittent fasting on metabolic associated steatotic liver disease in rats
Why this matters for everyday health
Many people carry extra fat in their liver without knowing it. This silent condition, now called metabolic associated steatotic liver disease (MASLD), is tightly linked to obesity and type 2 diabetes and can progress to liver scarring and failure. Because there is still no approved drug treatment, scientists are intensely interested in safe lifestyle approaches. This study in rats tested two simple, widely discussed options—vitamin D and intermittent fasting—to see how well they protect the liver from a fatty, sugar‑rich diet and to understand what is happening inside liver cells.
Setting up a real-world problem in the lab
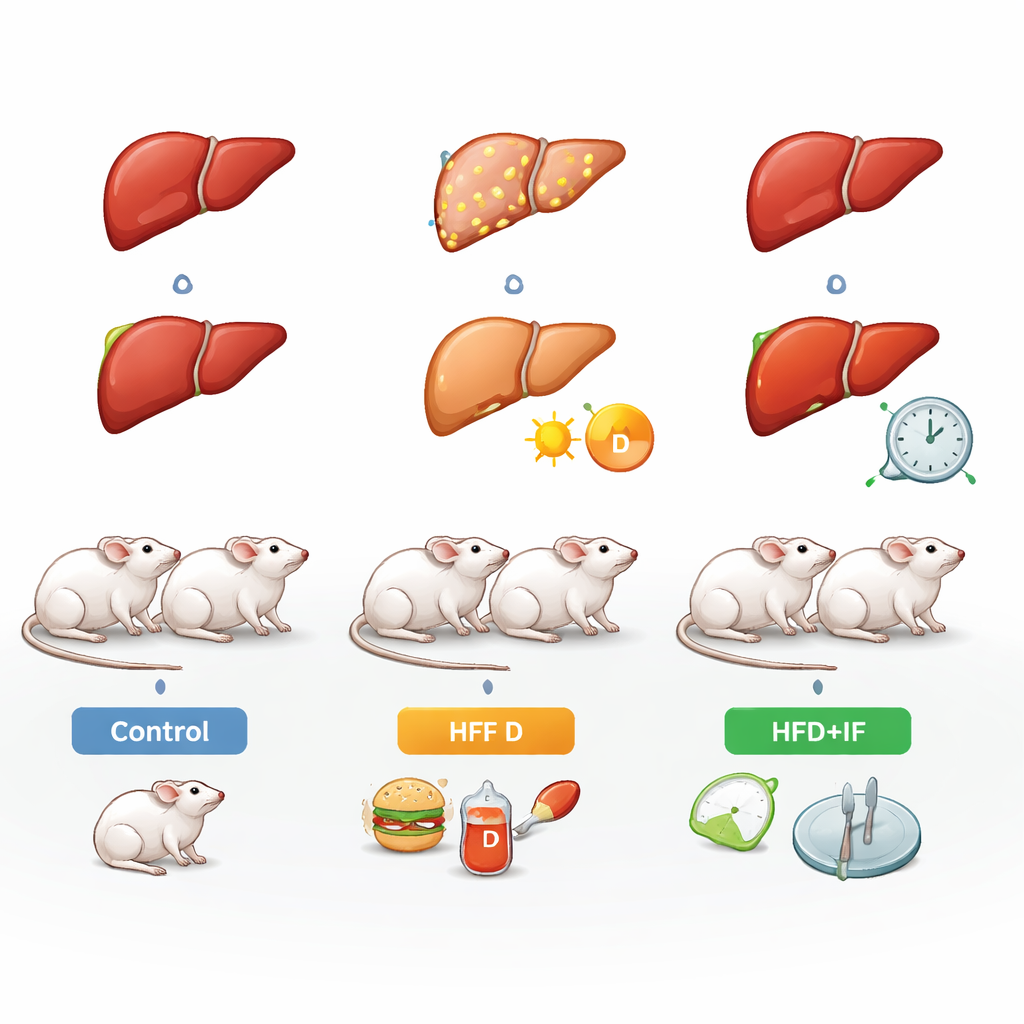
The researchers used 24 male rats and fed most of them a diet loaded with fat and fructose, mimicking the calorie‑dense foods and sugary drinks common in human diets. One group stayed on a normal diet as a healthy control. A second group received the high‑fat, high‑fructose diet alone, which reliably produced features of MASLD: weight gain, high blood fats, poor blood sugar control, and signs of liver damage. Two additional groups also started on the unhealthy diet but were later treated either with vitamin D injections or an intermittent fasting schedule that alternated 24 hours of feeding with 24 hours of fasting. This setup allowed a head‑to‑head comparison of how each strategy helped an already stressed liver recover.
What happened to weight, sugar, and blood fats
As expected, rats on the high‑fat, high‑fructose diet gained more weight and developed high levels of cholesterol, triglycerides, and “bad” LDL cholesterol, along with higher liver enzymes that signal injury. Both vitamin D and intermittent fasting reversed many of these changes. Blood sugar levels dropped by roughly half compared with untreated diseased rats, and insulin levels moved back toward normal, suggesting better control of blood sugar. Blood fats improved as well: triglycerides and LDL fell by about a third to a half, while “good” HDL cholesterol rose modestly. Intermittent fasting generally produced slightly stronger improvements in weight and cholesterol than vitamin D, hinting that regularly giving the body a break from calories may be especially powerful for metabolic health.
Signs of calmer, cleaner livers
When the scientists examined the livers under the microscope, the differences were striking. Rats on the unhealthy diet alone had livers stuffed with fat droplets, distorted cell structure, and clusters of immune cells—hallmarks of fatty liver disease. In contrast, livers from vitamin D‑treated animals showed mostly normal tissue with only mild fat buildup, while those from the intermittent fasting group looked closest to healthy controls, with minimal fat and evidence of tissue repair. Chemical tests backed this up: markers of oxidative stress, which reflect damaging reactions between fats and oxygen, were much lower in treated animals, especially those that fasted. Levels of glutathione, one of the body’s key antioxidants, rebounded strongly in both groups.
Peeking inside liver cells
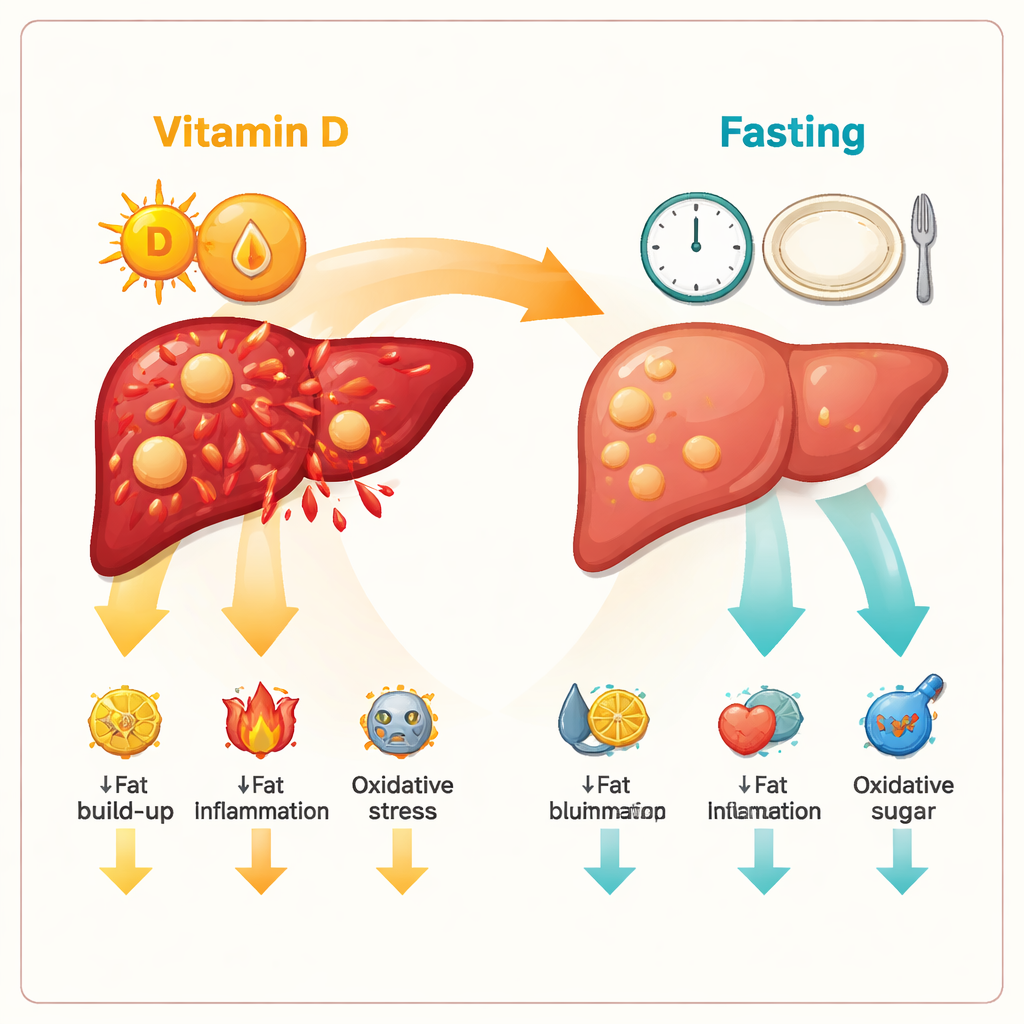
To understand how these improvements arose, the team measured several proteins that control fat handling and inflammation. In diseased rats, a protein that drives new fat production in the liver, called SREBP1, and a channel that brings glycerol into cells, AQP9, were both overactive, encouraging fat overload. Another set of molecules, TLR4 and NF‑κB, acted like fire alarms, switching on inflammatory signals. Both vitamin D and intermittent fasting turned these switches down: SREBP1 and AQP9 levels fell, and TLR4 and NF‑κB activity dropped back toward normal. This suggests that the treatments not only reduce fat storage but also quiet the chronic, smoldering inflammation that pushes simple fatty liver toward more dangerous stages.
What it could mean for people
In plain terms, this rat study shows that extra vitamin D and well‑planned periods without food can both help a fatty, overworked liver slim down, better control blood sugar, and cool off harmful inflammation. Intermittent fasting tended to have the strongest overall impact, but vitamin D also provided clear protection and may be easier to adopt for some people. While animal findings do not automatically translate to humans, they reinforce growing clinical evidence that sensible fasting routines and maintaining healthy vitamin D levels could be valuable, drug‑free tools to combat MASLD. The authors argue that these strategies deserve careful testing in long‑term human trials as part of a broader lifestyle approach to protecting liver health.
Citation: Youssef, O.M., Osman, A., Nour El-Deen, A.ES. et al. Therapeutic effects of vitamin D and intermittent fasting on metabolic associated steatotic liver disease in rats. Sci Rep 16, 4775 (2026). https://doi.org/10.1038/s41598-026-36143-8
Keywords: fatty liver, vitamin D, intermittent fasting, liver inflammation, metabolic health