Clear Sky Science · en
Dietary patterns and emotion dysregulation in borderline personality disorder and eating disorders as a shared mechanism underlying symptom severity
Why Food and Feelings Matter
Most of us know that what we eat affects our waistline and heart health, but this study asks a deeper question: can our daily food choices also shape how we handle intense emotions and, in turn, the severity of serious mental health problems like borderline personality disorder and eating disorders? By looking closely at women in psychiatric treatment, the researchers explore whether diet quality, emotional self-control, and psychiatric symptoms are linked in a common chain.
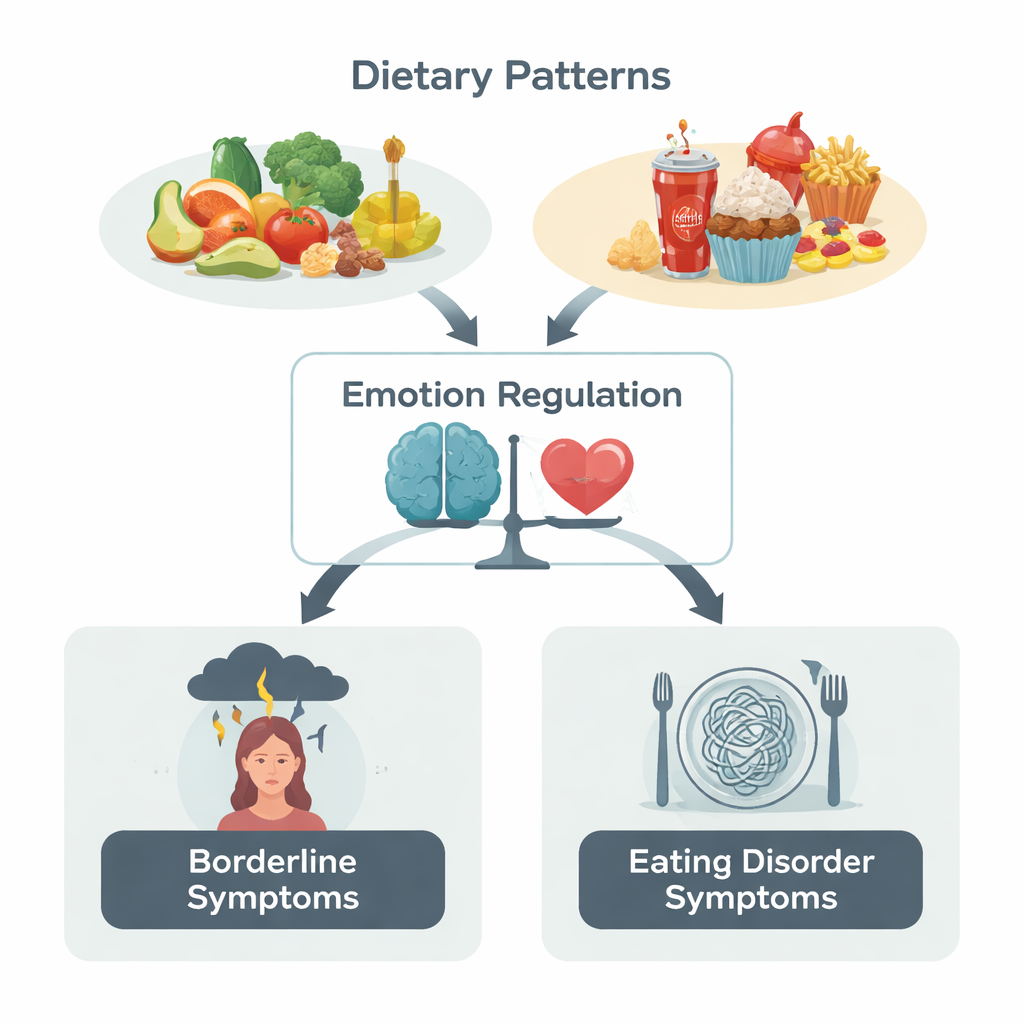
Who Was Studied and What Was Measured
The research followed 136 women in Poland, aged 18 to 50, divided into four groups: those with borderline personality disorder (BPD), those with eating disorders (including anorexia, bulimia, and binge-eating disorder), those with both BPD and an eating disorder, and healthy comparison volunteers. All participants completed a detailed food questionnaire covering how often they ate various foods over the past year. From this, the researchers built simple scores indicating how closely each woman’s diet resembled a Mediterranean-style pattern (rich in fruits, vegetables, whole grains, fish, and healthy fats) and how often she ate foods rich in omega‑3 fatty acids, such as fish, nuts, seeds, and certain vegetable oils.
How Emotions and Symptoms Were Tracked
To understand emotional functioning, the team used a standard questionnaire that measures “emotion dysregulation”—in everyday terms, difficulty understanding, accepting, and managing strong feelings and impulses. Higher scores mean greater struggles with emotions. The women also filled out tools that rate the current severity of BPD symptoms, disordered eating behaviors, anxiety, and depression. This allowed the researchers to see not just who had which diagnosis, but how severe their day‑to‑day problems were across a spectrum of emotional and behavioral symptoms.
Clear Differences in Everyday Eating Habits
Dietary patterns differed noticeably between the groups. Compared with healthy women, patients with BPD—especially those with both BPD and an eating disorder—tended to eat fewer foods that fit a Mediterranean diet and fewer sources of omega‑3 fats, including fish, legumes, nuts, and seeds. Women with BPD also reported drinking more sugar‑sweetened and energy drinks and, in some cases, eating more butter and cream. Those with eating disorders generally consumed less cheese, red meat, and alcohol than healthy controls, reflecting a more restrictive style of eating rather than a clearly healthier pattern. Overall, the picture that emerged was not one of extreme junk‑food indulgence in the patient groups, but of diets that lacked protective, nutrient‑dense foods.
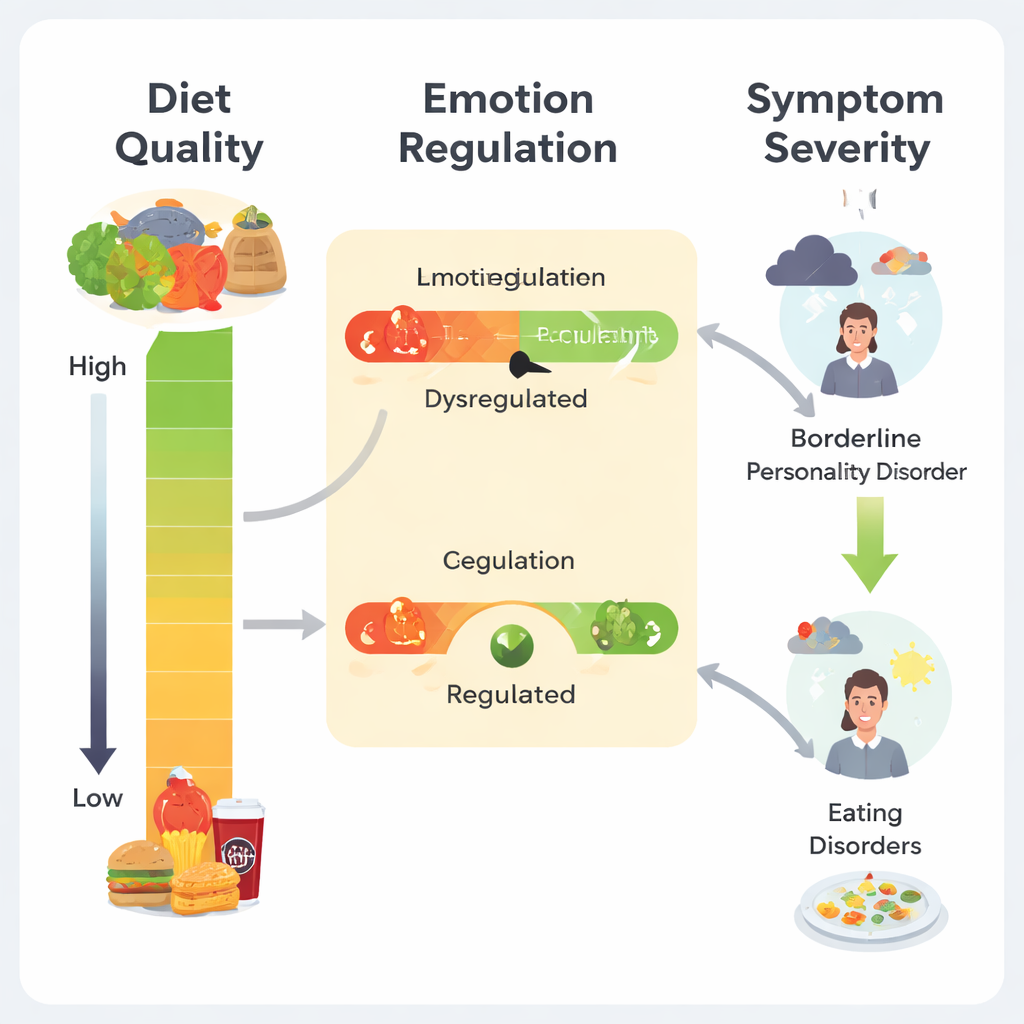
A Chain from Diet to Emotions to Symptoms
The heart of the study lies in how these pieces fit together. Women who more often ate Mediterranean‑style foods and omega‑3‑rich items tended to report fewer problems regulating their emotions and, in turn, less severe symptoms of both BPD and eating disorders. When the researchers used statistical models to test this chain, they found that emotion dysregulation largely “carried” the effect of diet quality on symptom severity. In other words, a healthier diet was linked to milder psychiatric symptoms mainly because it was associated with better emotional self‑control. For eating disorders, this indirect pathway appeared in all women, but an additional direct link between omega‑3 intake and symptom severity showed up only in those with a diagnosed eating disorder, hinting at a stronger biological or behavioral tie in this group.
What This Means for Real Life
For a layperson, the takeaway is both simple and cautious: while this study cannot prove cause and effect, it suggests that regularly eating nutrient‑rich foods—especially those typical of the Mediterranean diet and rich in omega‑3 fats—may support healthier emotional responses, which are central to conditions like BPD and eating disorders. In turn, better emotion regulation might help reduce the intensity of self‑destructive behaviors and extreme eating patterns. The findings do not replace established psychotherapies or medications, and the study’s design cannot show whether diet changes alone can improve symptoms. But they highlight diet as a promising, practical piece of a broader treatment puzzle, and they encourage future trials to test whether targeted nutritional interventions can meaningfully ease emotional suffering in these complex disorders.
Citation: Kot, E., Skimina, E., Pietras, T. et al. Dietary patterns and emotion dysregulation in borderline personality disorder and eating disorders as a shared mechanism underlying symptom severity. Sci Rep 16, 6010 (2026). https://doi.org/10.1038/s41598-026-36068-2
Keywords: borderline personality disorder, eating disorders, emotion regulation, Mediterranean diet, omega-3 fatty acids