Clear Sky Science · en
Comparison of epidural space contrast flow and clinical outcomes in parasagittal versus transforaminal epidural steroid injection
Why back and leg pain injections matter
Lumbosacral radicular pain—often felt as sharp, shooting pain from the lower back into the leg—is a common reason people struggle to work, sleep, or even walk comfortably. Many patients try epidural steroid injections when pills and physical therapy are not enough. But there is more than one way to place the needle, and doctors still debate which route is both safest and most effective. This study directly compares two popular techniques to see whether a newer, simpler approach can match the performance of a more targeted but technically demanding one.
Two different paths to the same target
Both injection methods in this trial deliver steroid medicine into the epidural space, a thin envelope around the spinal nerves. In the parasagittal interlaminar (PIL) approach, the needle is guided in from the middle of the back but slightly off to one side, between the bony arches of the spine. In the transforaminal (TF) approach, the needle enters from the side and aims directly toward the nerve root as it exits the spine. The TF path is often considered more precise, but it is technically trickier and can involve more X-ray guidance. The question the researchers asked was whether using a larger volume of medicine through the simpler PIL route could reach the painful area as well as the TF route does with a smaller volume.
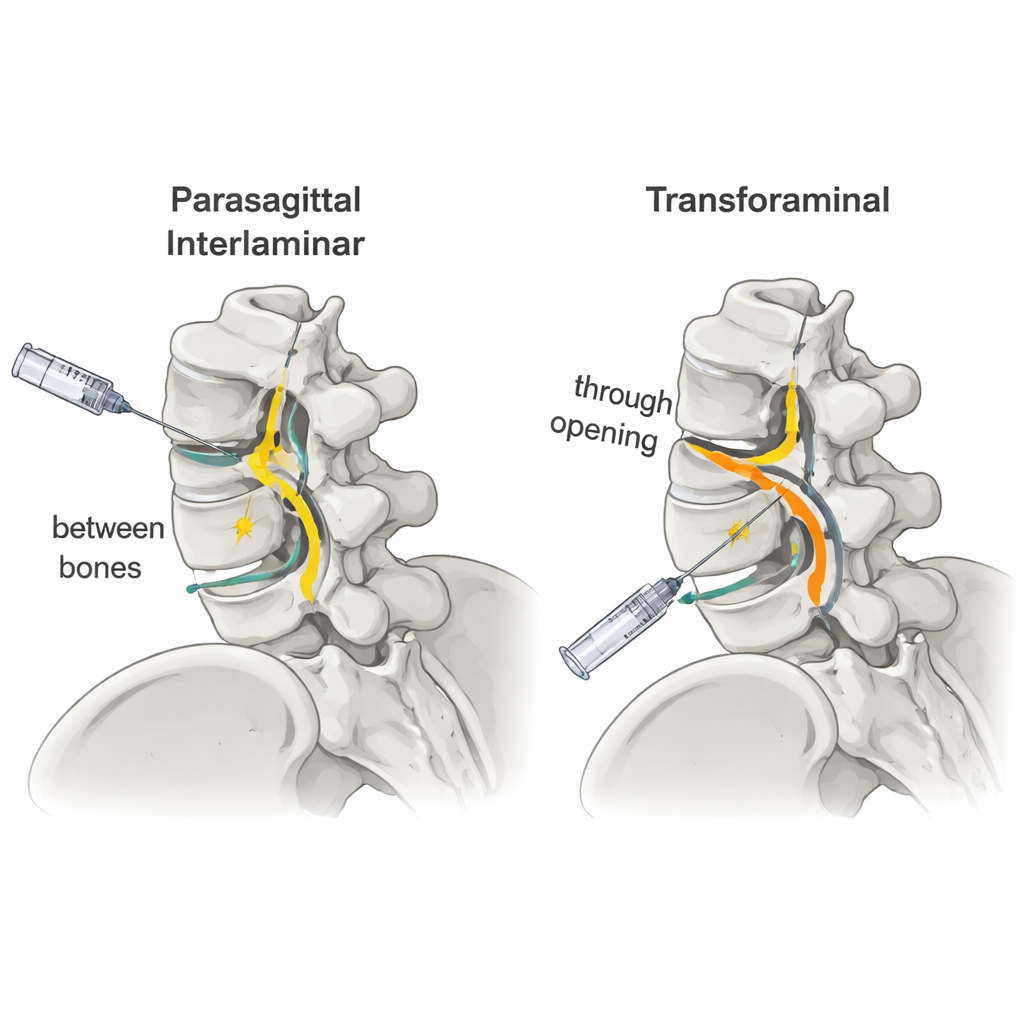
How the study was done
The researchers enrolled 79 adults aged 20 to 80 with one-sided leg pain caused by a damaged lower-back disc, confirmed by MRI scans. People with previous spine surgery, major medical problems, or recent similar injections were excluded. Participants were randomly assigned to receive either a high-volume PIL injection or a standard-volume TF injection, all performed by the same experienced pain specialist using live X-ray (fluoroscopy) to guide the needle. A contrast dye was first injected and imaged to see how far the fluid spread around the nerves, especially toward the front of the spine where disc-related inflammation is thought to be strongest. Patients’ pain scores, satisfaction, and quality of life were then tracked over six months by an observer who did not know which technique each person had received.
Pain relief and daily life results
Both groups experienced clear reductions in pain that were large enough to be meaningful in everyday life, with about 50 to 60 percent average pain relief in the first weeks and benefits that remained close to 50 percent at six months. People in the PIL and TF groups reported similar improvements in their ability to carry out daily tasks such as walking, sitting, and lifting, as measured by a standard low-back disability questionnaire. Satisfaction scores and patients’ own ratings of how much better they felt also did not differ between the techniques at any time point. In other words, from the patient’s perspective—pain, function, and overall impression—both routes worked about the same.
What the X-rays revealed inside the spine
The contrast dye images showed that, in both techniques, the injected fluid reached the front (anterior) part of the epidural space and spread upward and downward across more than two spinal levels. This suggests that a generous-volume PIL injection can reach the same inflamed region near the disc and nerve roots that the more targeted TF injection aims for. One subtle difference was that the PIL approach tended to spread farther downward along the spine, which may be helpful when several levels are irritated. Importantly, the TF procedures required roughly twice as many X-ray images as the PIL procedures, implying greater radiation exposure for both patients and staff. No complications were reported in either group during the study.
What this means for people with sciatica-like pain
This trial indicates that, for patients with leg pain from lower-back disc problems, a high-volume parasagittal interlaminar epidural steroid injection can provide pain relief, functional improvement, and nerve coverage comparable to the more intricate transforaminal route. Because the PIL method achieved this with fewer X-ray shots and is technically simpler, it may offer a safer and more practical option in many everyday clinical settings, especially for people who may need repeated injections. The authors recommend larger and longer studies, including more precise radiation measurements, but their findings support the idea that when it comes to these injections, a carefully performed “simpler path” can work just as well as the more complex one.
Citation: Khojasteh, N., Majedi, H., Meibodi, A.E. et al. Comparison of epidural space contrast flow and clinical outcomes in parasagittal versus transforaminal epidural steroid injection. Sci Rep 16, 7127 (2026). https://doi.org/10.1038/s41598-026-36056-6
Keywords: low back pain, sciatica, epidural steroid injection, spinal injections, radicular pain