Clear Sky Science · en
The associations of maternal liver biomarkers in different trimesters with birth weight outcomes
Why Liver Health in Pregnancy Matters
Most parents-to-be focus on ultrasound pictures and due dates, but what is happening in a mother’s liver during pregnancy may quietly influence how big or small her baby is at birth. This study followed more than twelve thousand pregnant women in China to see whether routine blood tests of liver function, taken at different stages of pregnancy, were linked with having babies who were unusually small or unusually large for their gestational age.
Following Mothers and Babies Over Time
Researchers drew on a long-running pregnancy cohort at Zhoushan Maternal and Child Care Hospital. They included women carrying a single baby, without major chronic diseases or serious liver problems, who had at least one liver function test and delivered after 32 weeks of pregnancy. Liver enzymes—ALT, AST, GGT and ALP, which are standard markers of how well the liver and related systems are working—were measured in the first trimester (weeks 9–13), second trimester (22–26 weeks) and third trimester (32–36 weeks). The team then linked these laboratory results to official birth records to see which babies were low birth weight or small for their gestational age, and which were very large or classified as macrosomic.
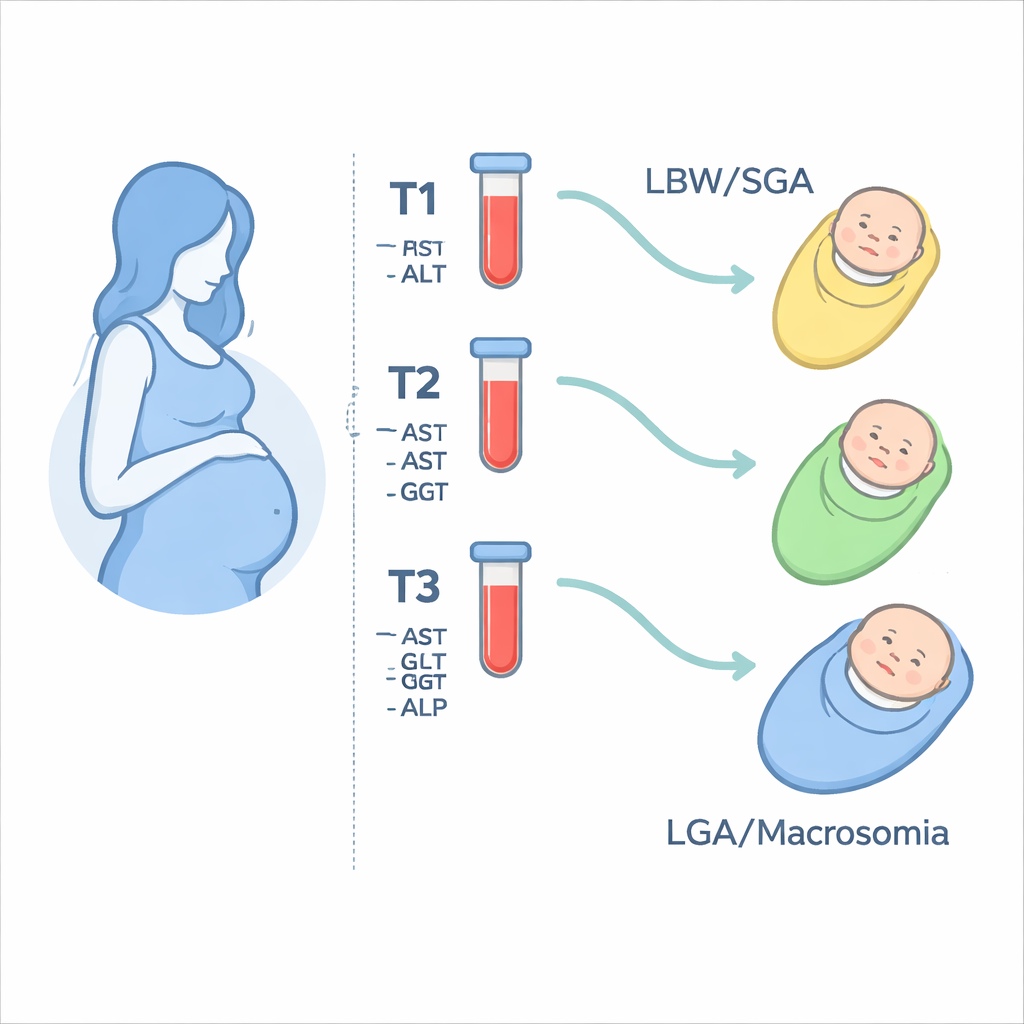
Different Enzymes, Different Growth Patterns
Among 12,728 mother–infant pairs, about 8% of babies were small and another 8% were very large. When the researchers compared mothers’ enzyme levels with birth weights, they found that the timing and type of liver marker mattered. Higher-than-usual levels of three enzymes—ALT, AST and GGT—during the mid-pregnancy window were linked with lighter babies and a greater risk of low birth weight or being small for gestational age. These links were not seen early in pregnancy, and they weakened by the third trimester, suggesting that the mid-pregnancy period may be especially sensitive for how the maternal liver and placenta support fetal growth.
When Normal-Range Changes Still Matter
The study did more than take one snapshot; it tracked how enzyme levels changed from early to late pregnancy. An increase in GGT across pregnancy, even when values stayed within usual clinical limits, was tied to a higher chance of having a small baby. At the other end of the spectrum, women with high levels of ALP and a high AST-to-ALT ratio in late pregnancy tended to have heavier babies and were more likely to deliver infants classified as macrosomic or large for gestational age. The combination of already higher early-pregnancy AST/ALT and a further rise over time strengthened this connection to large babies.
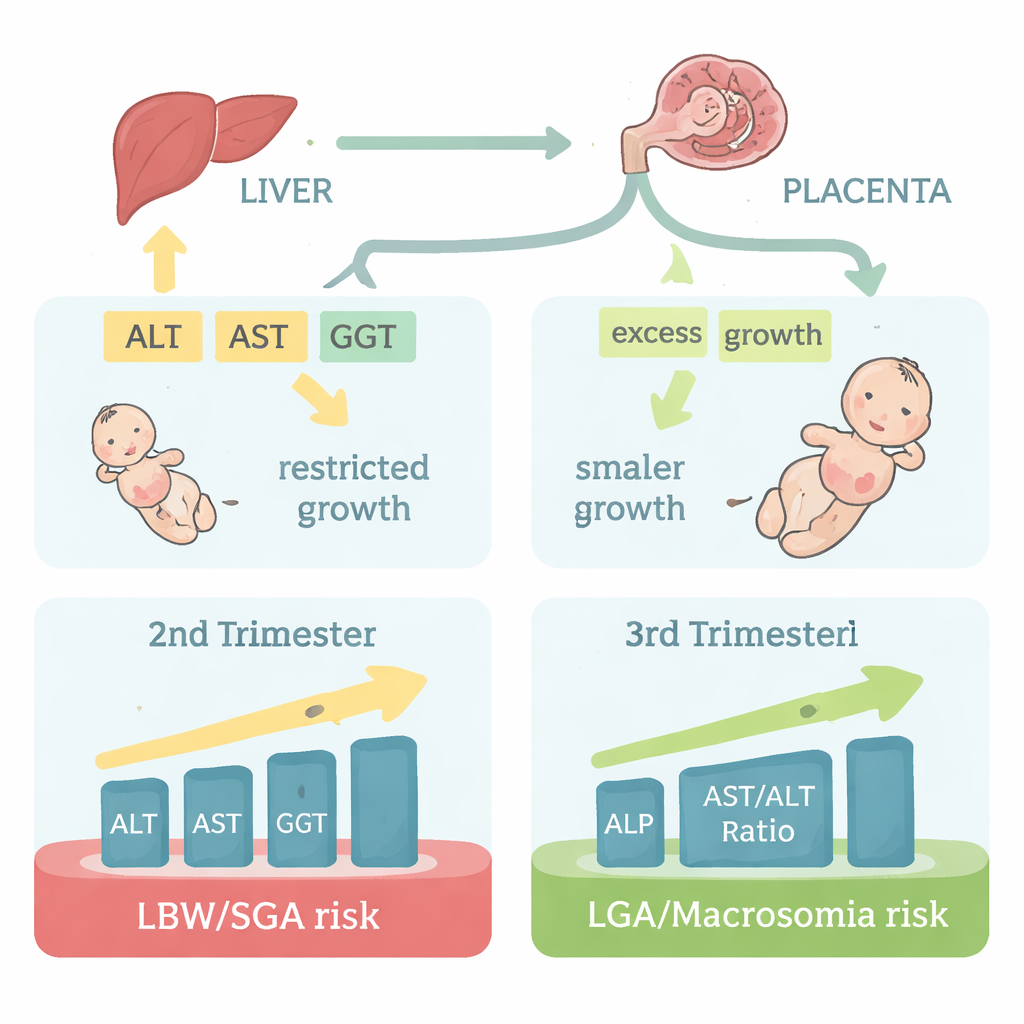
Possible Biological Explanations
Why might these routine blood markers relate to fetal size? The authors point to subtle inflammation and blood vessel dysfunction. Mildly elevated ALT, AST and GGT can signal low-grade liver stress and metabolic strain, which may damage the lining of blood vessels and interfere with how the placenta remodels and delivers oxygen and nutrients to the fetus. This could restrict growth and lead to smaller babies. ALP, by contrast, largely comes from the placenta in late pregnancy and reflects how actively it is transporting nutrients. Under conditions such as high blood sugar or oxidative stress, the placenta may respond by ramping up ALP production, a sign of a “reactive” state that may favor excess nutrient transfer and larger infants.
What This Means for Expectant Families
For parents, the takeaway is not that every small shift in a liver test is cause for alarm, but that these familiar blood tests may carry more information about fetal growth than previously appreciated. In generally healthy pregnancies, mid-pregnancy increases in certain liver enzymes were linked to smaller babies, while high placental-related enzymes late in pregnancy were tied to larger babies. The authors suggest that tracking patterns in liver markers over time could help doctors identify pregnancies that might benefit from closer monitoring, lifestyle counseling or other early interventions to support healthy birth weight. More research is needed to confirm these signals and to determine exactly when and how to act on them in everyday prenatal care.
Citation: Zhang, L., Qiu, Y., Ainiwan, D. et al. The associations of maternal liver biomarkers in different trimesters with birth weight outcomes. Sci Rep 16, 5575 (2026). https://doi.org/10.1038/s41598-026-36050-y
Keywords: pregnancy, liver enzymes, birth weight, fetal growth, placenta