Clear Sky Science · en
Effects of local anesthetics on yield and differentiation of synovial mesenchymal stem cells
Why numbing shots matter for joint repair
Doctors are increasingly exploring ways to repair worn or injured knees using a patient’s own stem cells taken from the joint lining. To collect this tissue comfortably, they rely on numbing shots such as lidocaine or ropivacaine. But some lab studies have suggested these drugs can damage stem cells. This paper asks a simple but important question: do the numbing medicines used during real-world knee procedures actually harm the stem cells needed for future joint repair?
A rich stem cell source inside the knee
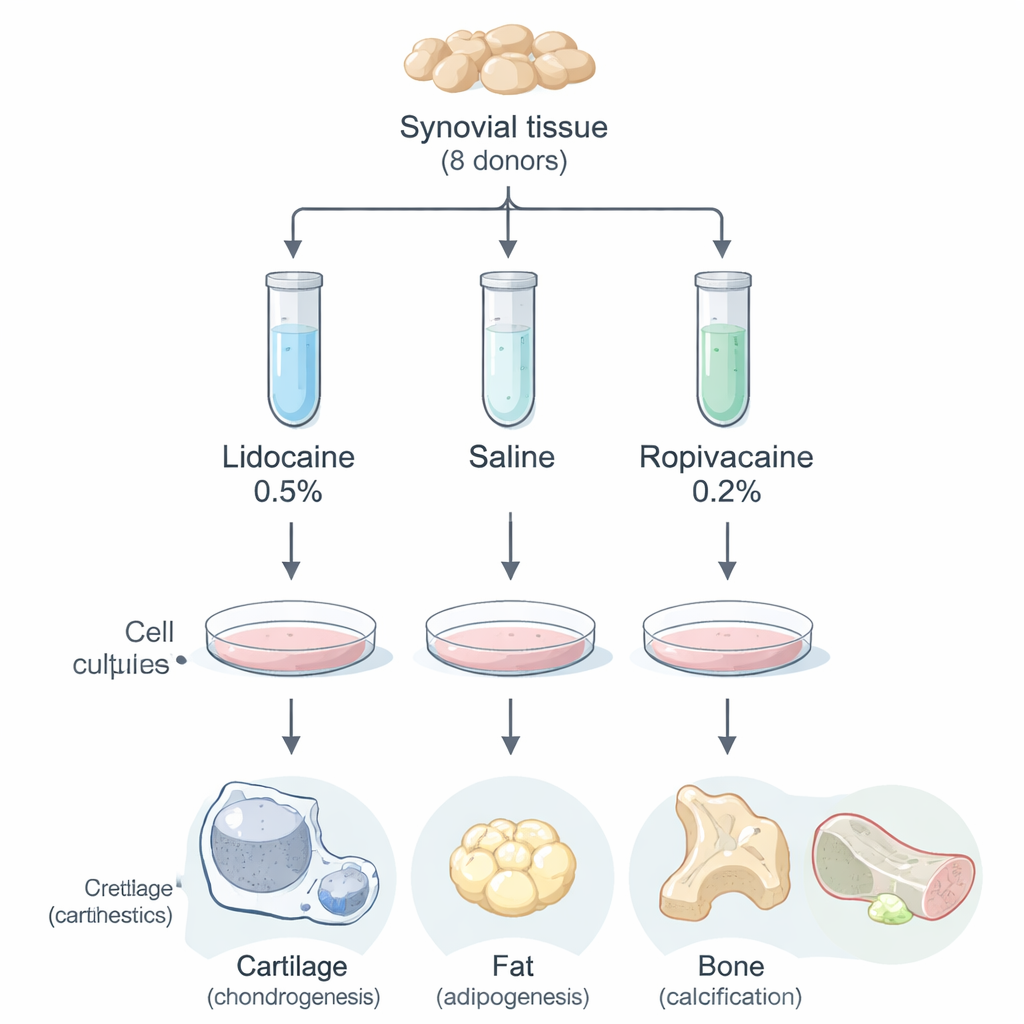
The inner lining of the knee joint, called the synovium, contains a special population of cells known as synovial mesenchymal stem cells. These cells can multiply and develop into cartilage, fat, and bone-like tissue, making them prime candidates for repairing damaged cartilage or meniscus and easing osteoarthritis. Traditionally, synovial tissue has been collected during arthroscopic surgery, which is invasive and costly. Newer ultrasound-guided needle techniques promise simpler, clinic-based harvesting, but they depend heavily on local anesthetics to control pain. Because earlier work on other types of stem cells hinted that these drugs can be toxic in a dish, clinicians have been unsure how safe they are for synovial stem cell–based therapies.
Putting numbing drugs to a realistic test
The researchers obtained small samples of knee synovium from eight older adults undergoing knee replacement for osteoarthritis. Each person’s tissue was minced and split into three equal portions. One was soaked in saline (salt water), one in a standard strength of lidocaine, and one in ropivacaine, for 20 minutes at body temperature—conditions meant to mirror the brief exposure that occurs when a doctor injects anesthetic into the joint before collecting tissue. After this short treatment, the tissue was washed, digested to release its cells, and the resulting cells were grown in culture dishes.
Checking survival, growth, and identity
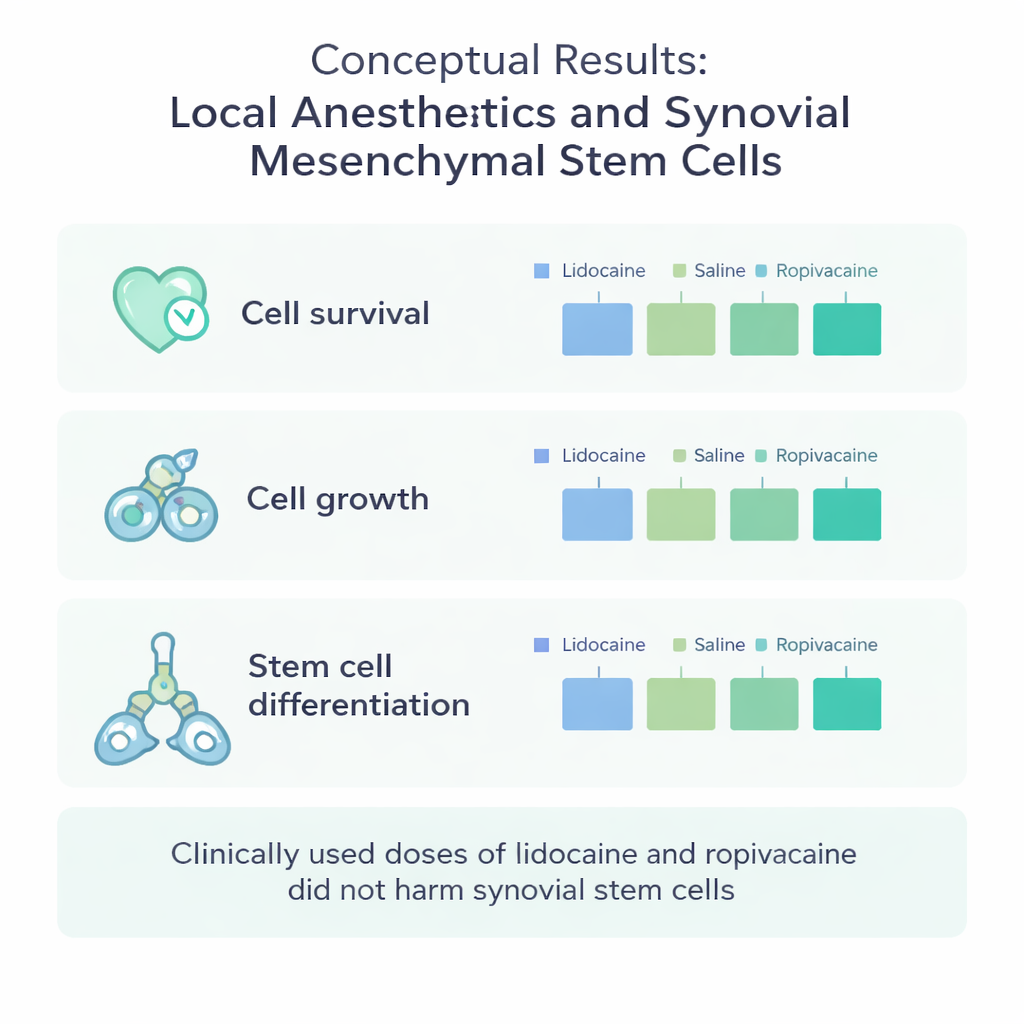
Right after the tissue was digested, the team counted how many nucleated cells were recovered per gram of synovium and how many of those cells were alive. They then grew the cells for 14 days and again measured how many stem cells could be expanded from each gram of starting tissue. Across all donors, cell survival, initial cell yield, and later expansion varied from person to person, but there were no consistent differences between saline, lidocaine, and ropivacaine. Under the microscope, the cells from all three groups showed the same typical spindle-shaped appearance, and a detailed marker analysis confirmed they still looked like bona fide mesenchymal stem cells, not blood or immune cells.
Do the cells still do their repair jobs?
Beyond simply surviving, stem cells must retain their ability to turn into different tissue types. The researchers therefore tested three key directions: cartilage, fat, and calcified tissue. When pushed toward cartilage, cells from all treatment groups formed round pellets that produced similar amounts of cartilage-like matrix, judged by pellet weight and dye staining. When driven toward fat, comparable fractions of cell colonies filled with oily droplets and took up a red stain. Likewise, when nudged toward calcified tissue, the area stained by a mineral-binding dye was similar in all groups. For each of these outcomes, some donors produced more or less tissue than others, but anesthetic exposure itself made no meaningful difference.
What this means for future joint therapies
In plain terms, this study shows that a brief, clinically realistic exposure of knee lining tissue to lidocaine or ropivacaine does not measurably harm the stem cells later harvested from that tissue. The cells survive, multiply, and retain their ability to become cartilage, fat, and calcified tissue just as well as cells from tissue exposed only to saline. For patients and clinicians, this supports the use of familiar numbing shots during ultrasound-guided synovial tissue collection, without fearing they will undercut the very stem cells needed for regenerative treatments of cartilage damage or osteoarthritis.
Citation: Kitamura, T., Endo, K., Ozeki, N. et al. Effects of local anesthetics on yield and differentiation of synovial mesenchymal stem cells. Sci Rep 16, 5557 (2026). https://doi.org/10.1038/s41598-026-36025-z
Keywords: synovial stem cells, local anesthetics, knee osteoarthritis, cartilage repair, regenerative medicine