Clear Sky Science · en
Disease-specific crosstalk of Alistipes with lipoprotein profiles in overweight individuals at high cardiometabolic risk
Why your gut bugs and blood fats matter
Many people know that high cholesterol can raise the risk of heart disease, but fewer realize that the tiny particles carrying fats in our blood – and even the microbes living in our gut – can also tilt the odds. This study looks at how a particular gut bacterium, called Alistipes, relates to detailed blood fat patterns in overweight people with either metabolic syndrome or the autoimmune disease lupus, and what that might mean for their heart risk.
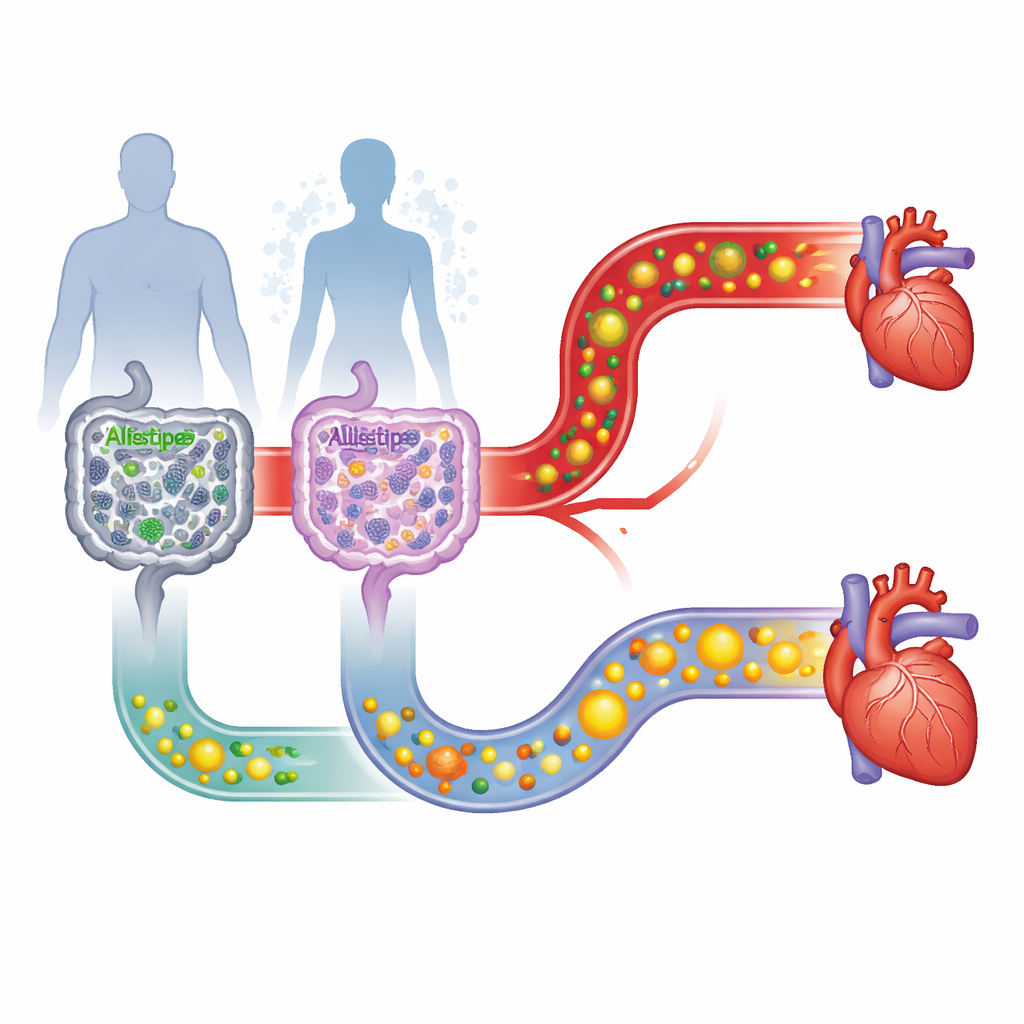
Two different illnesses, one shared heart concern
Metabolic syndrome is a cluster of problems – extra belly fat, high blood pressure, high blood sugar and abnormal cholesterol – that together greatly increase the chance of heart attack and diabetes. Lupus, in contrast, is an autoimmune disease in which the immune system attacks the body’s own tissues, causing widespread inflammation. Both groups of patients in this study were overweight and known to have higher than average cardiovascular risk, but for very different reasons. The researchers set out to compare these two conditions head‑to‑head, not only by standard medical measures, but also by looking closely at the structure of blood lipoproteins and the composition of gut bacteria.
Looking under the hood of blood fats
Rather than measuring only “good” and “bad” cholesterol, the team used a nuclear magnetic resonance technique to count lipoprotein particles of different sizes in the blood – including very small forms of LDL (“bad”) cholesterol that are thought to be especially damaging to arteries. They found that people with metabolic syndrome had a clearly more dangerous pattern: more particles rich in triglycerides, more intermediate and very‑low‑density lipoproteins, and a higher number of small, dense LDL particles. Their “good” HDL cholesterol was lower and shifted toward smaller, less protective forms. Patients with lupus, despite active inflammation, generally had fewer of these risky small particles and a somewhat more favorable lipoprotein profile.
The gut community tells a different story
The scientists also analyzed stool samples using genetic sequencing to see which bacteria were present. Overall, people with lupus had lower microbial diversity and a distinct mix of species compared with those with metabolic syndrome. Using machine‑learning tools, the team highlighted certain bacterial groups that best distinguished between the two diseases. Among them, Alistipes stood out as particularly important. Differences in its abundance helped the computer model tell which patients had metabolic syndrome and which had lupus, suggesting this genus sits at a crossroads between gut health, metabolism and inflammation.
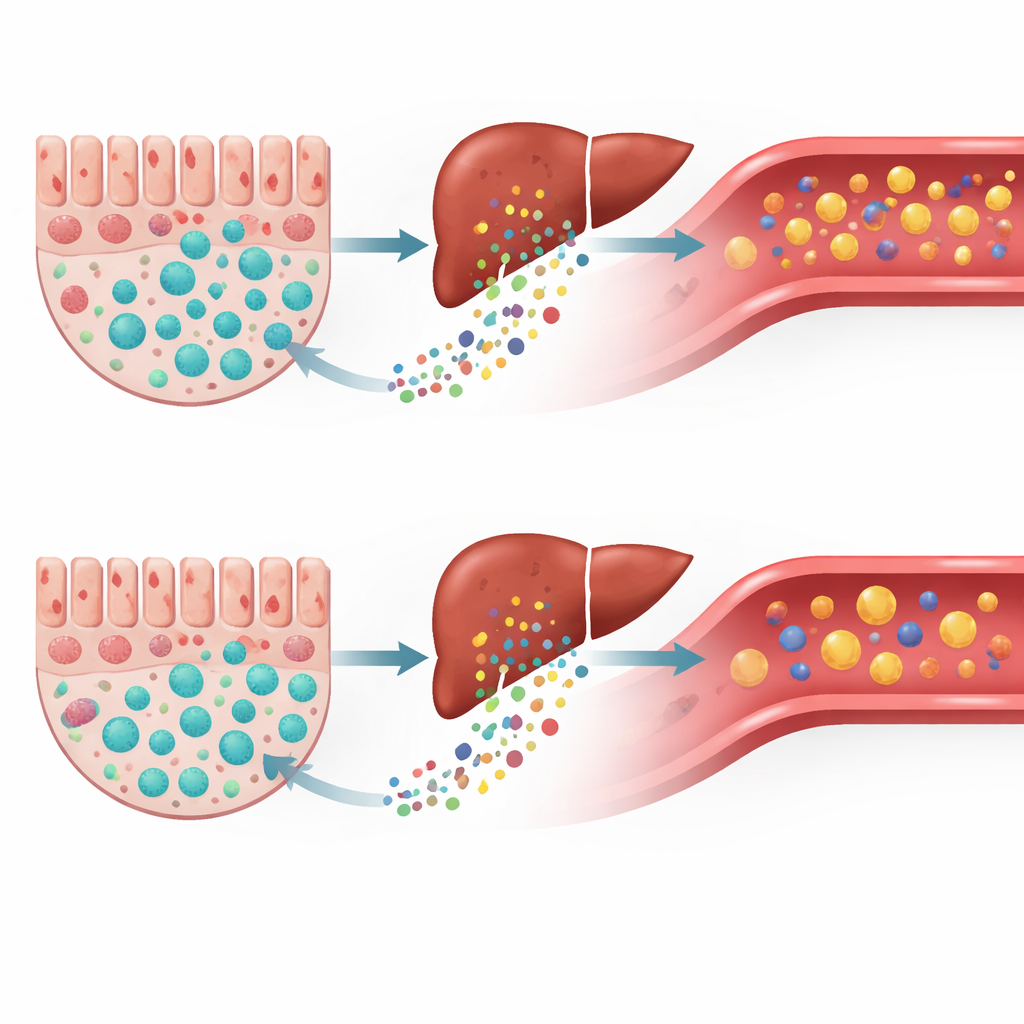
A single bacterium, opposite links to risky particles
The most intriguing finding came when the researchers connected gut data with blood fat data. They examined how the amount of Alistipes related to the number of small LDL particles, while accounting for age, sex, overall cholesterol and diet quality. In people with metabolic syndrome, higher levels of Alistipes went hand‑in‑hand with more small, dense LDL particles – the type most strongly tied to artery clogging. In people with lupus, however, higher Alistipes tended to be linked with slightly fewer small LDL particles. In other words, the same bacterium appeared to push blood fats in a harmful direction in one disease but not in the other.
What this means for future care
To a lay reader, the main message is that heart risk is shaped by more than just cholesterol numbers, and that the same gut microbe can behave differently depending on the illness background. Overweight patients with metabolic syndrome in this study carried more of the small, artery‑penetrating LDL particles, and their levels were closely tied to Alistipes. Lupus patients, while still at increased cardiovascular risk, showed a milder lipoprotein pattern and a different gut microbial landscape. These findings do not prove cause and effect, but they support the idea that future prevention and treatment strategies – from drugs to diet to microbiome‑targeted therapies – may need to be tailored not only to blood tests, but also to the specific disease context and the individual’s gut ecosystem.
Citation: Cuevas-Sierra, A., Higuera-Gómez, A., de Cuevillas, B. et al. Disease-specific crosstalk of Alistipes with lipoprotein profiles in overweight individuals at high cardiometabolic risk. Sci Rep 16, 8998 (2026). https://doi.org/10.1038/s41598-026-36024-0
Keywords: gut microbiome, metabolic syndrome, systemic lupus erythematosus, small dense LDL, cardiovascular risk