Clear Sky Science · en
Bilateral muscle activation in postparalytic facial synkinesis: a cross-sectional high-resolution surface electromyography study
When a Smile Closes an Eye
Most of us take it for granted that we can smile, blink, or puff our cheeks without thinking. For people who have had severe facial paralysis, however, everyday expressions can become tangled: smiling may make an eye squeeze shut, or closing the eyes can pull up a corner of the mouth. This study investigates how and why these “crossed‑wires” movements occur, not just in one muscle or one side of the face, but across the entire facial system.
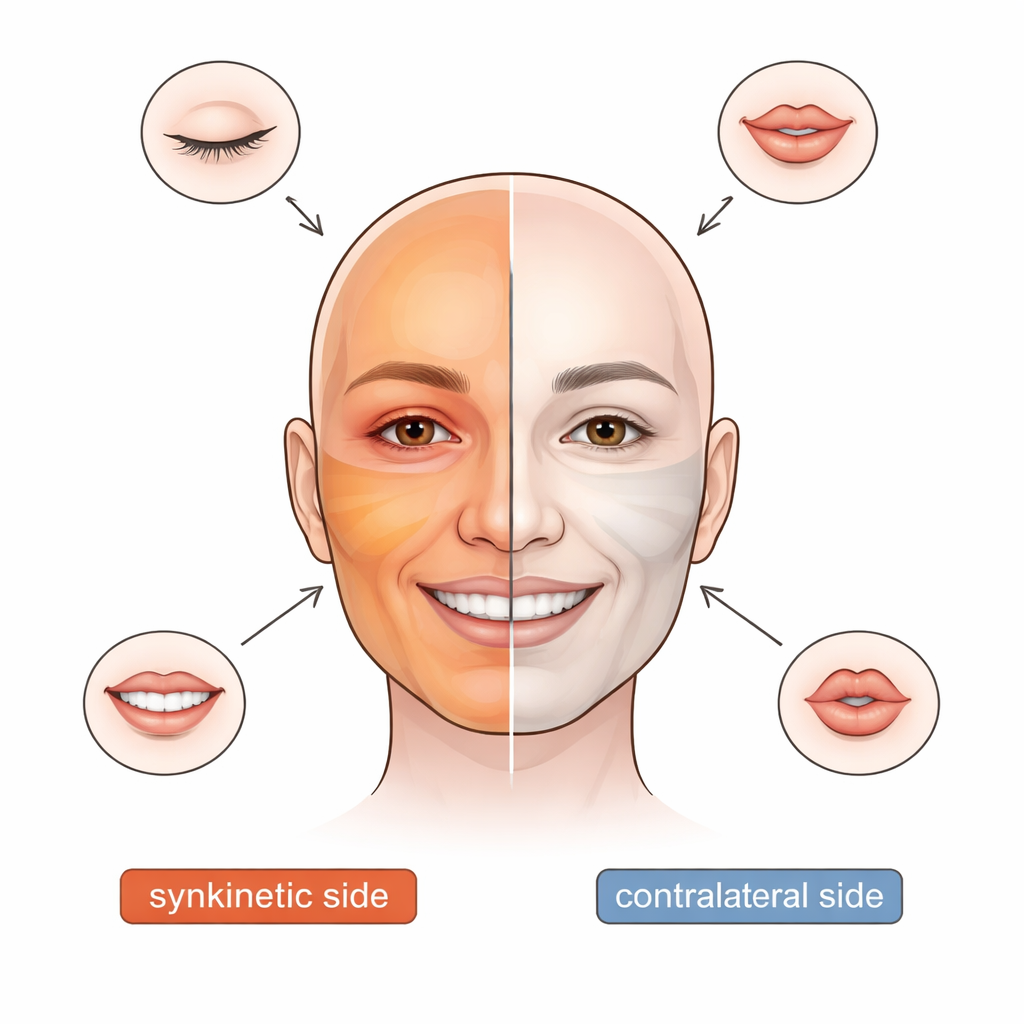
A Hidden Cost of Recovering from Facial Paralysis
After a serious injury to the facial nerve, some patients develop facial synkinesis, a condition in which attempts at a normal facial movement trigger unwanted contractions elsewhere. This can interfere with eating, speaking, or showing emotion and often leads to embarrassment or social withdrawal. Doctors know that nerve fibers can regrow in the wrong pathways, but until now most tests have focused on one or two muscles at a time, or on only one side of the face. The authors of this study suspected that the problem is much broader: that facial synkinesis affects nearly every facial muscle and even changes how the supposedly “normal” side of the face works.
Wiring Up the Face in High Detail
To explore this, researchers in Germany used high‑resolution surface electromyography, a technique that records tiny electrical signals from muscles through small skin electrodes. They placed 58 electrodes in two carefully planned patterns across the faces of 36 adults with facial synkinesis and 36 healthy volunteers. Participants performed 11 standardized tasks—such as resting, gently and tightly closing the eyes, smiling with lips closed or open, puckering, blowing up the cheeks, and snarling—while sitting calmly and following the same video instructions. For each task, the team measured how strongly each region of the face activated and compared three situations: the side with synkinesis, the opposite side in the same patient, and the faces of healthy people.
Facial Movements as a Whole‑Face Event
The recordings showed that even in healthy people, a single facial expression is rarely the work of just one muscle. Most tasks activated almost all facial regions to some degree, though the muscles primarily responsible for the intended movement—such as those around the eyes during eye closure or around the mouth during puckering—were the most active. In contrast, patients with synkinesis showed a strikingly different pattern. On the affected side, the intended muscles often worked less than in healthy volunteers, while distant areas that should have stayed relatively quiet switched on strongly. For example, closing the eyes forcefully not only activated the eyelid muscles but also caused exaggerated activity around the mouth and chin. Similar “off‑target” activation appeared across many movements.
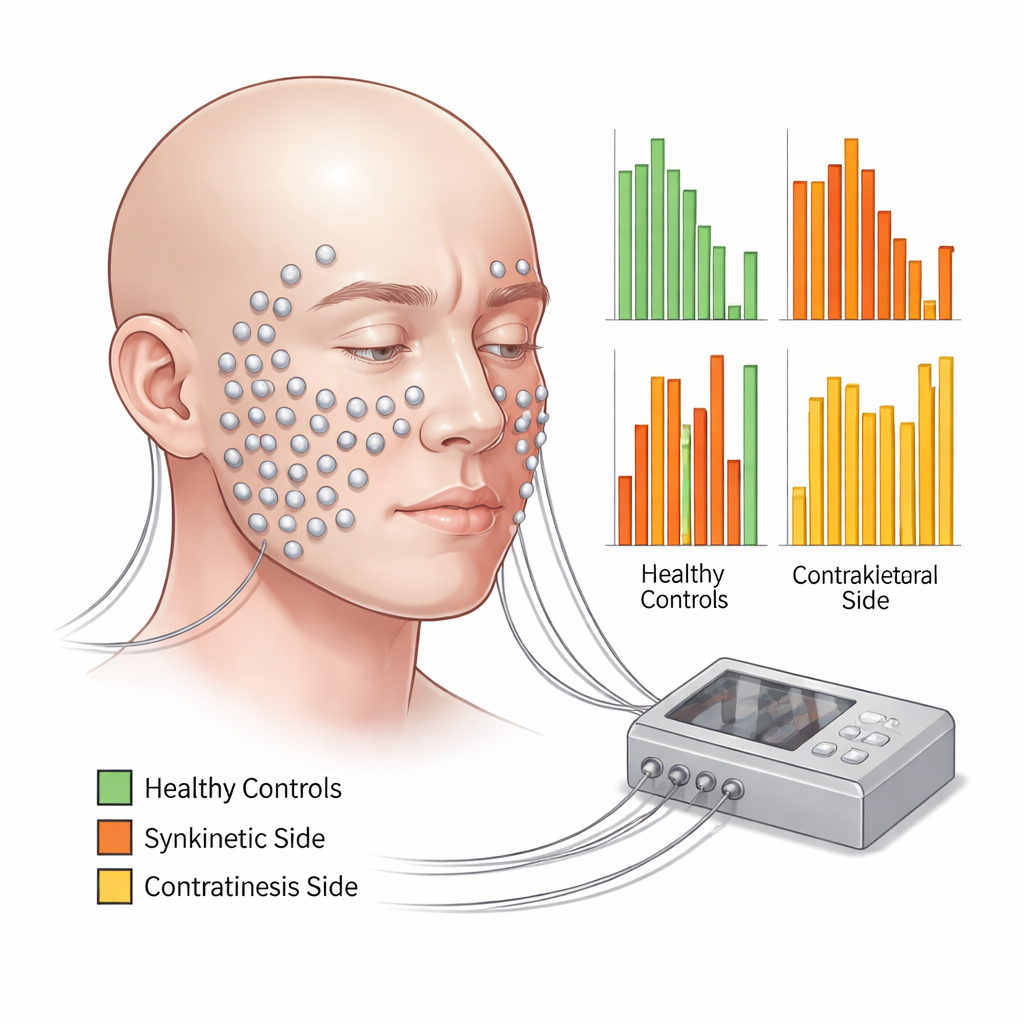
The “Good” Side Is Not Truly Normal
Surprisingly, the opposite side of the face in these patients also behaved differently from healthy faces. Its activation patterns were neither fully normal nor simply a copy of the synkinetic side. Depending on the task and region, the contralateral side sometimes resembled healthy controls, sometimes mimicked the abnormal side, and often showed values in between. This suggests that the brain and facial nerves may be trying to preserve overall symmetry by adjusting both sides together, even if that means spreading inefficient or unintended activity. The authors argue that the face, in effect, becomes a single, mis‑coordinated network rather than a damaged half paired with an untouched half.
Rethinking Treatment for a Network Disorder
By revealing that facial synkinesis involves widespread, bilateral mis‑coordination, this work challenges the idea that therapy should focus only on a few visibly overactive muscles. The detailed muscle maps produced by high‑resolution electromyography could eventually help clinicians tailor botulinum toxin injections, surgery, and biofeedback training more precisely, including on the “good” side of the face. For patients, the takeaway is that their symptoms stem from a whole‑face wiring problem, not a personal failure to control their expressions—and that future treatments may increasingly target the entire facial network to restore more natural, comfortable movement.
Citation: Funk, P.F., Schneider, R., Schramm, M. et al. Bilateral muscle activation in postparalytic facial synkinesis: a cross-sectional high-resolution surface electromyography study. Sci Rep 16, 2057 (2026). https://doi.org/10.1038/s41598-026-36015-1
Keywords: facial synkinesis, facial paralysis, facial muscles, electromyography, facial nerve