Clear Sky Science · en
SULT1E1 exerts a protective role in COPD by inhibiting the AKT pathway: an in vivo and in vitro study
Why a Lung Enzyme Matters to Everyday Breathing
Chronic obstructive pulmonary disease (COPD) is one of the world’s leading causes of death, yet doctors still lack tools to stop it early or reverse its damage. This study shines a light on an unexpected player in COPD: a small enzyme called SULT1E1 that helps process hormones and chemicals in the body. By following this enzyme from big data to patient blood samples, animal lungs, and cultured cells, the researchers uncover evidence that SULT1E1 acts as a kind of built‑in shield for the airways—and that losing it may help drive COPD forward.
A Fresh Look at a Familiar Lung Disease
COPD is not a single illness but a cluster of chronic lung problems, including chronic bronchitis and emphysema, usually triggered by long‑term exposure to smoke or polluted air. Over time, the airways become inflamed, scarred, and clogged with mucus, leaving people breathless with even mild exertion. Current treatments mainly ease symptoms; they do little to halt the slow, irreversible damage to lung tissue. That is why scientists are searching for new molecular clues—proteins or pathways that not only mark disease severity but might also be targeted to protect or repair the lungs.
Following an Enzyme Across Datasets and Patients
The researchers began by mining four large public gene‑expression datasets of human lung tissue, comparing samples from people with COPD to those from individuals without the disease. Among hundreds of genes that differed, SULT1E1 stood out as sharply reduced in COPD lungs. This enzyme normally helps deactivate estrogen and other hormones and participates in the safe handling of drugs and foreign chemicals. Network and pathway analyses showed that SULT1E1 is linked to many metabolic and hormone‑related proteins, suggesting that changes in its level could ripple across multiple systems relevant to lung health.
To check whether this pattern holds beyond computer screens, the team measured SULT1E1 in real patients. In blood samples from 92 people with COPD and 40 healthy volunteers, both the protein level in serum and the gene activity in immune cells were significantly lower in the COPD group. Importantly, those with the lowest SULT1E1 tended to have the worst lung function, as measured by standard breathing tests (FEV1% and the FEV1/FVC ratio). This tight link hints that SULT1E1 could serve as a simple blood‑based marker of how far COPD has progressed.
Proof from Animal Lungs and Lab‑Grown Cells
The story did not stop at blood tests. In a rat model exposed to irritants that mimic human COPD, the animals developed classic lung damage under the microscope, and their lung tissue also showed a marked drop in SULT1E1 protein. To understand what this enzyme actually does in airway cells, the scientists turned to a human bronchial cell line grown in dishes. When they dialed down SULT1E1, the cells multiplied faster, resisted programmed cell death, and began to adopt features associated with tissue scarring and stiffening—a process called epithelial‑mesenchymal transition, or EMT. When they boosted SULT1E1, all of these changes reversed: growth slowed, cell death returned toward normal, and EMT markers declined.
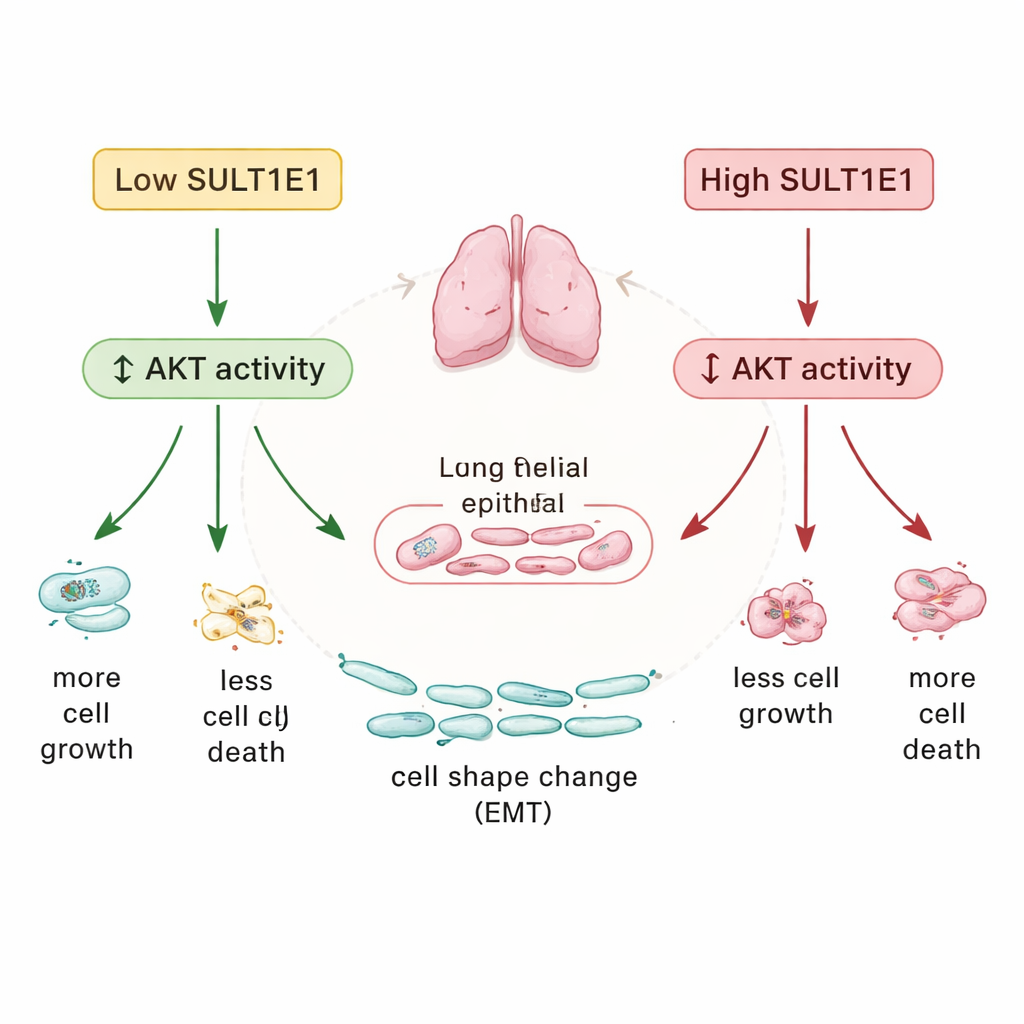
The Signal Switch That Links the Pieces
Digging deeper, the team traced these effects to a central signaling route inside cells known as the AKT pathway, which helps control growth, survival, and stress responses. In lung cells lacking SULT1E1, AKT was more strongly switched on; with extra SULT1E1, AKT activity dropped. In other words, SULT1E1 appears to act as a natural brake on AKT signaling. When that brake fails in COPD, the result is a shift toward excessive cell growth, reduced cell turnover, and structural changes in the airway lining—all hallmarks of the disease. The researchers speculate that this may partly stem from altered handling of estrogen, which can itself feed into AKT activation, though other, non‑hormonal roles for SULT1E1 are also possible.
What This Could Mean for People with COPD
Taken together, the findings portray SULT1E1 as a quiet guardian of the lungs: when present at healthy levels, it keeps key growth and survival signals in check, helping maintain a stable airway lining. In COPD, that guardian is lost or weakened, and the AKT pathway runs too hot, encouraging overgrowth and scarring of airway cells. For patients, this work offers two main prospects. First, SULT1E1 in the blood could become a convenient marker to gauge disease severity or track response to treatment. Second, medicines that raise SULT1E1 activity—or mimic its calming effect on AKT—might one day form a new class of targeted therapies aimed not just at easing symptoms, but at slowing the underlying damage that makes breathing such a struggle.
Citation: Song, W., Zhang, W., Wang, F. et al. SULT1E1 exerts a protective role in COPD by inhibiting the AKT pathway: an in vivo and in vitro study. Sci Rep 16, 6238 (2026). https://doi.org/10.1038/s41598-026-35997-2
Keywords: COPD, SULT1E1, lung inflammation, AKT signaling, biomarker