Clear Sky Science · en
Fine particulate matter exacerbates childhood asthma via DNMT3A-mediated modulation of GPX4 DNA methylation
Why dirty air matters for kids’ lungs
City smog is more than just an eyesore; it can send children with asthma to the emergency room. This study asks a pressing question for families living in polluted areas: how do tiny air particles called PM2.5 actually make asthma attacks worse? By tracing what happens from the air outside to the cells lining a child’s airways, the researchers uncover a hidden chain of events inside lung cells that links pollution to inflammation and airway damage.
Tiny particles, big trouble
PM2.5 refers to airborne particles so small that they can slip deep into the lungs. Doctors have long known that days with high PM2.5 levels often coincide with flare-ups of asthma symptoms—more coughing, wheezing, and trouble breathing. Yet the biological steps connecting dirty air to these attacks have been murky. This work focuses on children’s asthma, using both animal models and samples from young patients to show that PM2.5 does more than irritate the lungs on the surface; it appears to trigger a particular form of cell damage that ramps up inflammation.
A special kind of cell damage inside the airways
The team homed in on a recently recognized type of cell death called ferroptosis, which is driven by iron and uncontrolled fat oxidation in cell membranes. They exposed mice and human bronchial cells to cockroach allergen—a common asthma trigger—and PM2.5. In mice, PM2.5 exposure led to more inflammatory cells crowding around the airways, thicker mucus, and higher levels of inflammatory molecules IL-6 and IL-8 in lung tissue. When the researchers gave a drug that blocks ferroptosis, these harmful changes were largely reduced, suggesting that this specific kind of cell damage is a key step in pollution-worsened asthma.
The body’s built-in shield and how pollution turns it down
Cells have defenses against this destructive oxidation, and one of the most important defenders is a protein called GPX4. In healthy airway cells, GPX4 helps neutralize harmful oxygen byproducts before they can shred cell membranes. In this study, PM2.5 exposure lowered GPX4 levels in both mouse lungs and human airway cells. As GPX4 dropped, cells showed more reactive oxygen species, more membrane damage, and a loss of healthy mitochondrial function—all hallmarks of ferroptosis. When the scientists artificially boosted GPX4 in the cells, much of the oxidative stress, cell injury, and IL-6/IL-8 release was reversed, underscoring GPX4’s role as a crucial shield.
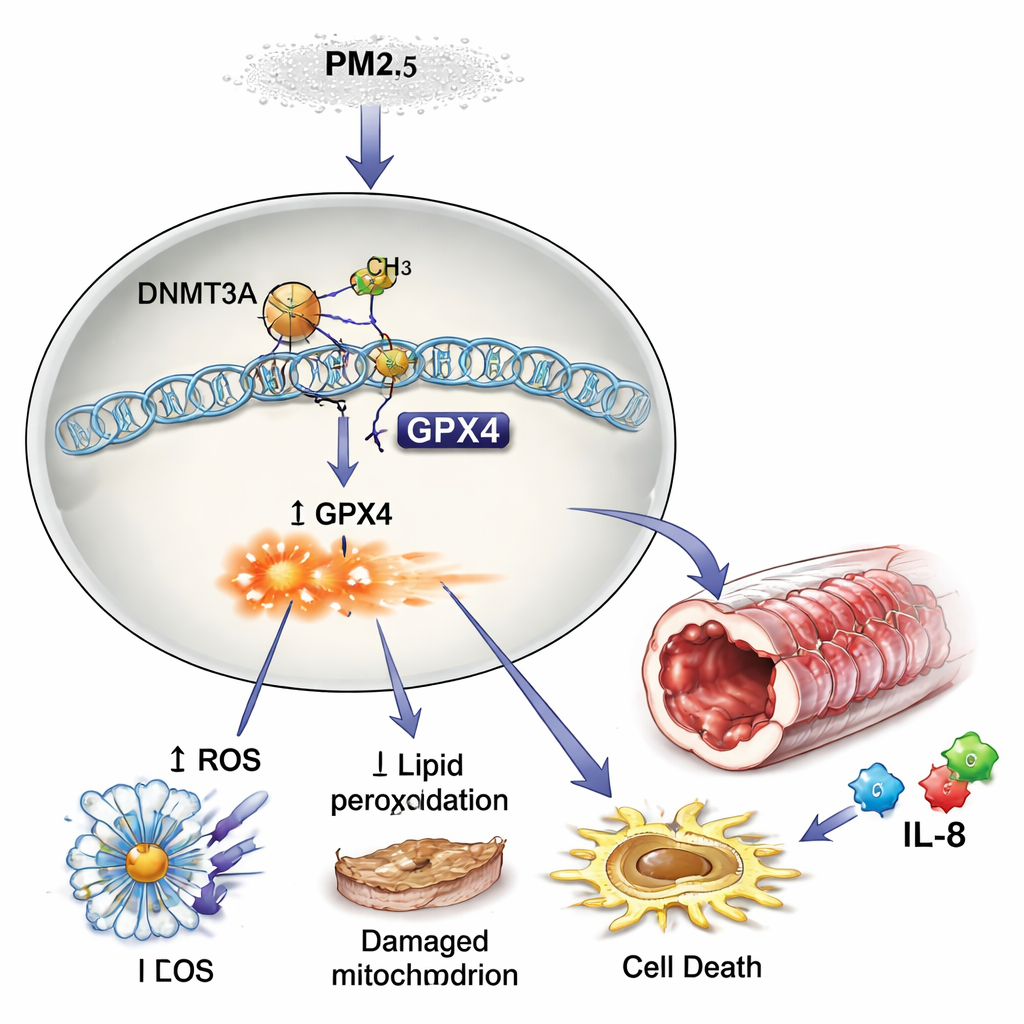
Pollution rewires gene switches through chemical tags
Why did GPX4 levels fall after PM2.5 exposure? The answer lay in epigenetics—chemical tags that act like dimmer switches on genes. The researchers found that PM2.5 increased the activity of an enzyme called DNMT3A, which adds methyl groups to DNA. These tags accumulated in the control region of the GPX4 gene, effectively turning the gene down. Blocking DNMT3A prevented this extra methylation and restored GPX4 expression, showing that PM2.5 “reprograms” airway cells by tightening this genetic dimmer switch. In blood cells from children with asthma, those with more severe disease had higher GPX4 methylation, lower GPX4 protein, and higher IL-6/IL-8 levels, mirroring the lab findings.
What this means for protecting children
For non-specialists, the message is that tiny pollution particles don’t just irritate the lungs; they silently alter how key protective genes work in airway cells. PM2.5 boosts DNMT3A, which adds chemical tags that mute the GPX4 “shield” gene. With this shield weakened, cells are more likely to undergo ferroptosis and release inflammatory molecules that tighten and clog children’s airways, worsening asthma. These discoveries not only reinforce the importance of clean air policies and indoor air protection but also point toward future medicines that might protect or restore GPX4’s function—ideally delivered directly to the lungs—to help children breathe more easily in polluted environments.
Citation: Wu, X., Dai, L., Li, R. et al. Fine particulate matter exacerbates childhood asthma via DNMT3A-mediated modulation of GPX4 DNA methylation. Sci Rep 16, 5566 (2026). https://doi.org/10.1038/s41598-026-35962-z
Keywords: air pollution, childhood asthma, PM2.5, epigenetics, lung inflammation