Clear Sky Science · en
Risk of total hip arthroplasty following lumbar fusion surgery in a nationwide cohort study
Why back surgery can matter for your hips
Lumbar fusion surgery is often performed to relieve stubborn lower back pain and stabilize an aging spine. But what happens to the hips when part of the spine is locked in place with screws and rods? This nationwide Korean study followed thousands of people for up to a decade and found that certain types of lumbar fusion, especially when extended down to the pelvis, are linked to a higher chance of later needing a total hip replacement. The work helps patients and surgeons weigh long-term trade-offs of major back surgery and highlights who may need extra monitoring afterward.
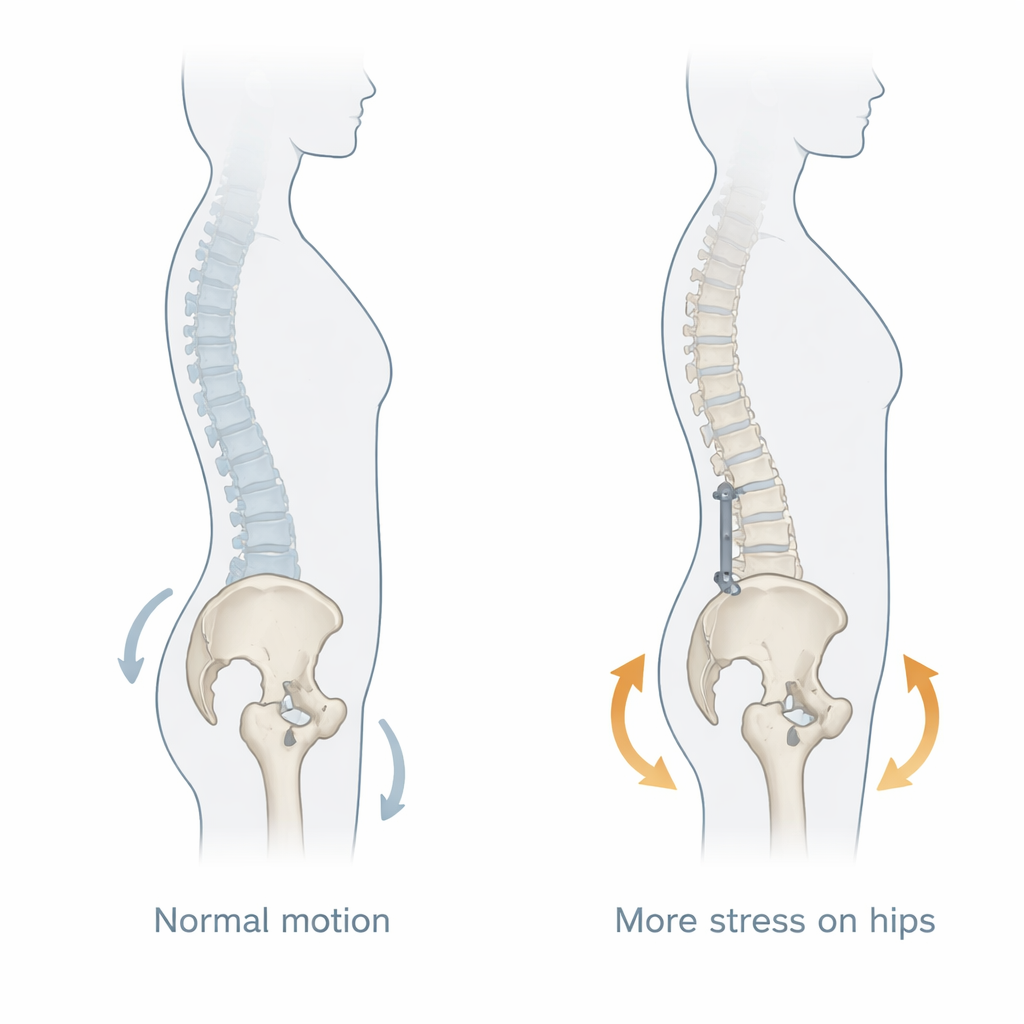
How the spine and hips work together
The spine, pelvis, and hips form an interconnected system that keeps us upright and balanced. When we move from standing to sitting, the pelvis normally tilts backward, subtly changing the socket position of the hip joint and spreading out mechanical forces. This motion acts like a built-in shock absorber. Lumbar fusion surgery stabilizes the lower back by permanently joining vertebrae with bone and hardware. When the fusion extends to the sacrum or pelvis, it limits the pelvis’s ability to tilt. As a result, the hips must bend and rotate more to achieve the same everyday movements, concentrating stress on the hip joint surfaces over many years.
A large real-world look at surgery and hip replacement
To test whether this altered mechanics actually translates into more hip damage, the researchers used South Korea’s National Health Insurance data, which covers almost the entire population. They identified adults who had lumbar fusion surgery with deformity correction or sacropelvic fixation between 2005 and 2013, then matched each of them with ten people of similar age, sex, and screening year who did not have fusion surgery. Everyone was followed for up to nine years after an initial three-year “washout” period, during which prior hip or knee replacements and certain other conditions were excluded. The main outcome was whether people went on to receive a first total hip replacement; total knee replacement was also tracked for comparison.
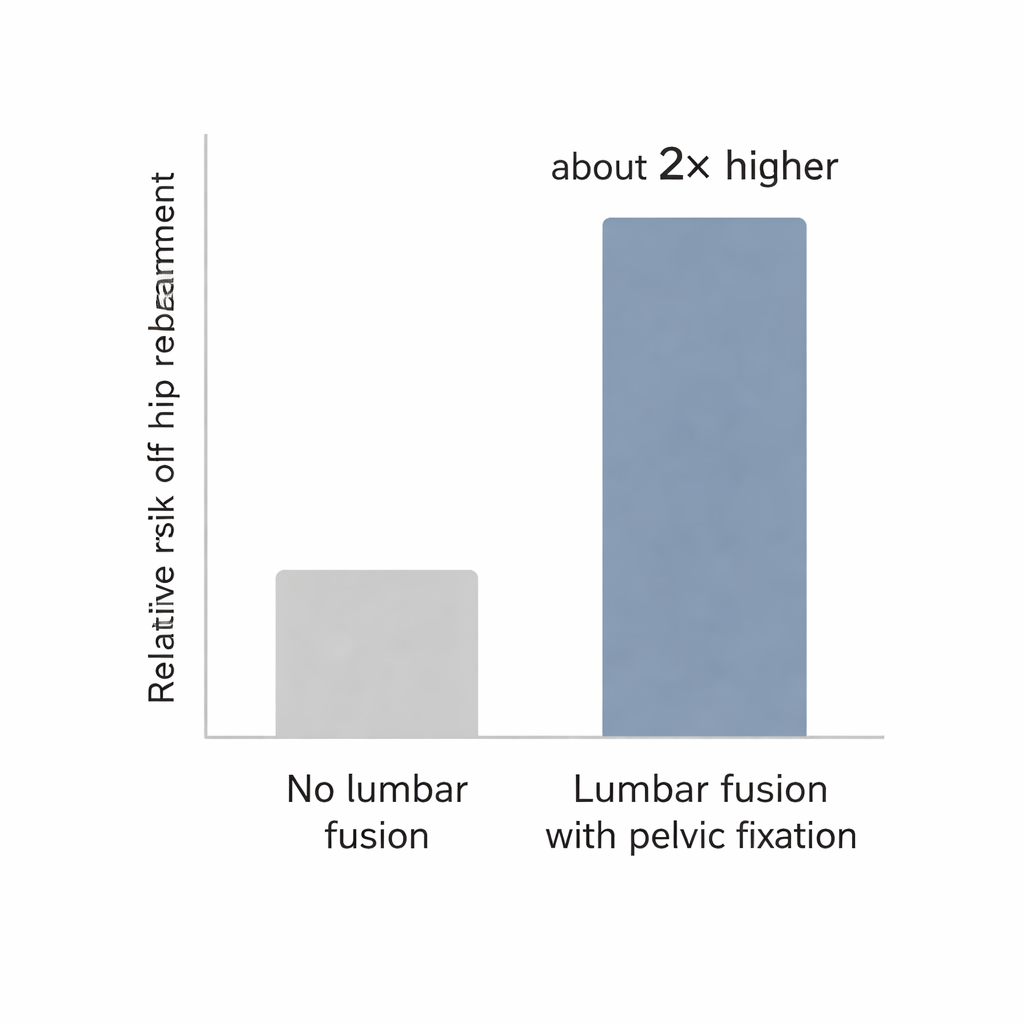
What the study found about long-term risk
Among 558 patients who had lumbar fusion with deformity correction or pelvic fixation and 5,580 matched controls, hip replacements occurred noticeably more often in the surgery group. Their crude rate of total hip arthroplasty was about 6.7 per 1,000 person-years, compared with 2.8 in controls. After adjusting for factors like age, sex, smoking, body mass index, cholesterol, alcohol use, and income, the fusion group still had a little more than double the risk of hip replacement. The increase was driven mainly by people aged 60 and older, and was especially pronounced in women and in those with higher body weight or higher income. In contrast, knee replacement did not rise significantly after this type of fusion, suggesting that the hip — directly linked to the stiffened pelvis — bears the brunt of the extra load.
Why some people are more vulnerable
The authors argue that the combination of a rigid spine-pelvis unit and normal aging makes the hip more fragile. Older adults already face thinning cartilage, weaker muscles, and less stable gait. Locking the lower spine and pelvis together removes an important motion buffer, so forces that would once have been shared by the back and pelvis are shifted into the hip joint. Extra body weight further amplifies these compressive forces. Women, who tend to have higher rates of osteoarthritis and different bone and cartilage patterns, appeared particularly affected. Higher-income patients showed more hip replacements, which may reflect better access to surgery and greater willingness to opt for joint replacement once symptoms become limiting.
What this means for patients and surgeons
For people considering lumbar fusion, this study does not argue against surgery when it is truly needed, but it does underline a cost that may show up years later. Fusions that include the sacrum or pelvis seem to carry a meaningful long-term increase in hip replacement risk, while the knee appears less vulnerable. The findings support closer follow-up of hip pain and function in older, female, and heavier patients after fusion, and they encourage surgeons to consider hip mechanics when deciding how far to extend spinal hardware. For lay readers, the main message is that the spine and hips form a single mechanical chain: when one link is made rigid to solve a problem, another link may wear out faster and deserve ongoing care.
Citation: Bae, Y., Lee, S.W., Seo, S. et al. Risk of total hip arthroplasty following lumbar fusion surgery in a nationwide cohort study. Sci Rep 16, 5670 (2026). https://doi.org/10.1038/s41598-026-35894-8
Keywords: lumbar fusion surgery, hip replacement, spine and hip mechanics, joint degeneration, osteoarthritis risk