Clear Sky Science · en
Variations in the perceived value of anti-SARS-CoV-2 therapeutics based on physicians’ clinical backgrounds
Why the Price of COVID Pills Still Matters
The global COVID-19 crisis may no longer dominate headlines, but for older adults and people with serious health problems, the virus can still be deadly. Pills that fight the virus early can keep high-risk patients out of the hospital. In Japan, however, patients must now pay part of the cost of these medicines, and that price tag is changing how doctors think and act. This study asks a simple but important question: when COVID drugs are expensive, do doctors hold back on prescribing them—and does it depend on where and what they practice?
From Free Treatment to Shared Costs
At the height of the pandemic in Japan, antiviral drugs for COVID-19 were fully covered by public funds, so patients paid nothing at the pharmacy. That changed in late 2023 and 2024, when the country shifted to a standard cost-sharing system. Now, most patients must pay 10–30 percent of the bill, which translates to about 100–200 US dollars per course of the main COVID antivirals. By comparison, a full course of flu antivirals usually costs around 33 dollars or less. 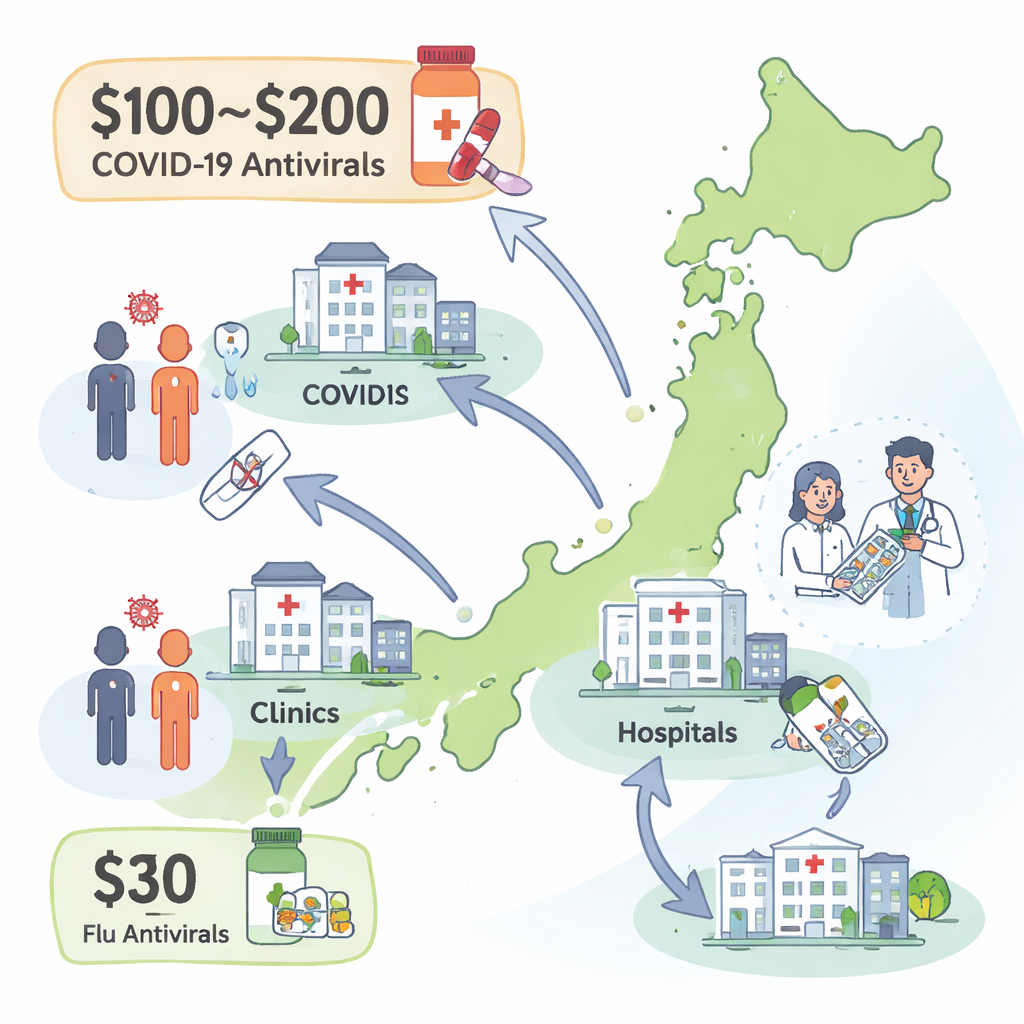
A Nationwide Look at Doctors’ Choices
The researchers carried out a large web-based survey of 1,500 physicians across Japan who care for COVID-19 patients. Many were general practitioners, lung specialists, or ear, nose, and throat doctors—fields that often see people with respiratory infections. Doctors answered questions about how they would treat 16 made-up cases of mild COVID-19 before and after watching an educational film about antiviral benefits. In addition, they were asked two key questions: do they ever avoid prescribing antivirals because of cost, and what do they believe is a “reasonable” price for a full treatment course? Response options ranged from 33 dollars or less up to 101 dollars or more.
High Costs, Reluctant Prescribing
The results revealed a clear tension between what doctors think antivirals should cost and what they actually cost. Nearly four out of five physicians said they had held back from prescribing COVID-19 antivirals in daily practice because of the price. About two thirds felt that 33 dollars or less would be an appropriate cost for one course of treatment—far below current levels. 
Where a Doctor Works Shapes How They Prescribe
To tease apart the roles of age, specialty, and workplace, the researchers used a statistical model that looked at all these factors together. They found that workplace setting—not specialty or age—was the only factor that independently predicted whether doctors avoided prescribing because of cost. Clinic-based physicians were significantly more likely to say they held back on antivirals than hospital-based physicians. This suggests that cost sensitivity is closely tied to the everyday reality of clinics, where doctors may see patients who are more affected by out-of-pocket expenses and may rarely encounter life-threatening COVID-19.
What This Means for Patients
For high-risk people with mild COVID-19, the first stop is often a neighborhood clinic. If clinic doctors are reluctant to prescribe antivirals because of cost, treatment may be delayed or never started, potentially raising the risk of severe illness. The study’s authors argue that encouraging appropriate antiviral use in clinics is crucial. They suggest better communication and sharing of clinical experience between hospitals and clinics, as well as ongoing medical education, to narrow the gap in prescribing patterns. In plain terms, the paper concludes that when lifesaving drugs are priced above what most doctors and patients feel is reasonable, important treatments may be used too little—especially where patients most commonly seek first-line care.
Citation: Hagiwara, A., Komiya, K., Shindo, Y. et al. Variations in the perceived value of anti-SARS-CoV-2 therapeutics based on physicians’ clinical backgrounds. Sci Rep 16, 5705 (2026). https://doi.org/10.1038/s41598-026-35878-8
Keywords: COVID-19 antivirals, drug costs, physician prescribing, primary care clinics, health policy Japan