Clear Sky Science · en
FracDet-v11: a multi-scale attention and wavelet-enhanced network for real-time pediatric wrist fracture detection
Why tiny wrist cracks matter
When a child falls and lands on an outstretched hand, doctors usually rely on quick X-ray checks to decide whether a bone is broken. Yet children’s wrist fractures can be extremely hard to spot: tiny cracks hide among growing bones, and even experienced clinicians can miss them. This study introduces FracDet‑v11, a specialized artificial intelligence (AI) system designed to read pediatric wrist X‑rays in real time and help catch subtle fractures and other abnormalities that might otherwise slip through.
Hidden injuries in a busy emergency room
Painful wrists are one of the most common reasons children and teenagers visit emergency departments. The small bones near the hand are packed tightly together, and in young patients the growth plates—where bones are still developing—can mimic or mask fractures on X‑rays. In crowded hospitals, X‑ray images are often interpreted by surgeons or junior doctors rather than specialist radiologists, and published studies suggest that up to one in four emergency fractures may be missed. The authors argue that an accurate, fast, and reliable AI assistant could reduce these oversights, especially in regions facing a shortage of radiology experts.
Teaching AI what a broken wrist looks like
To train and test their system, the researchers used GRAZPEDWRI‑DX, a large public collection of over 20,000 wrist X‑rays from more than 6,000 children treated in Austria. Each image carries detailed markings made and checked by teams of radiologists, flagging fractures and other visible signs such as bone deformities, metal implants, or soft‑tissue changes. The authors divided this dataset so that images from the same child never appear in both training and testing, ensuring the AI is judged on entirely new patients. They also adjusted brightness and contrast of training images to mimic real‑world variation in X‑ray quality. A second dataset from Bangladesh, called FracAtlas, provided an extra test of whether the system can cope with different ages, scanners, and patient populations. 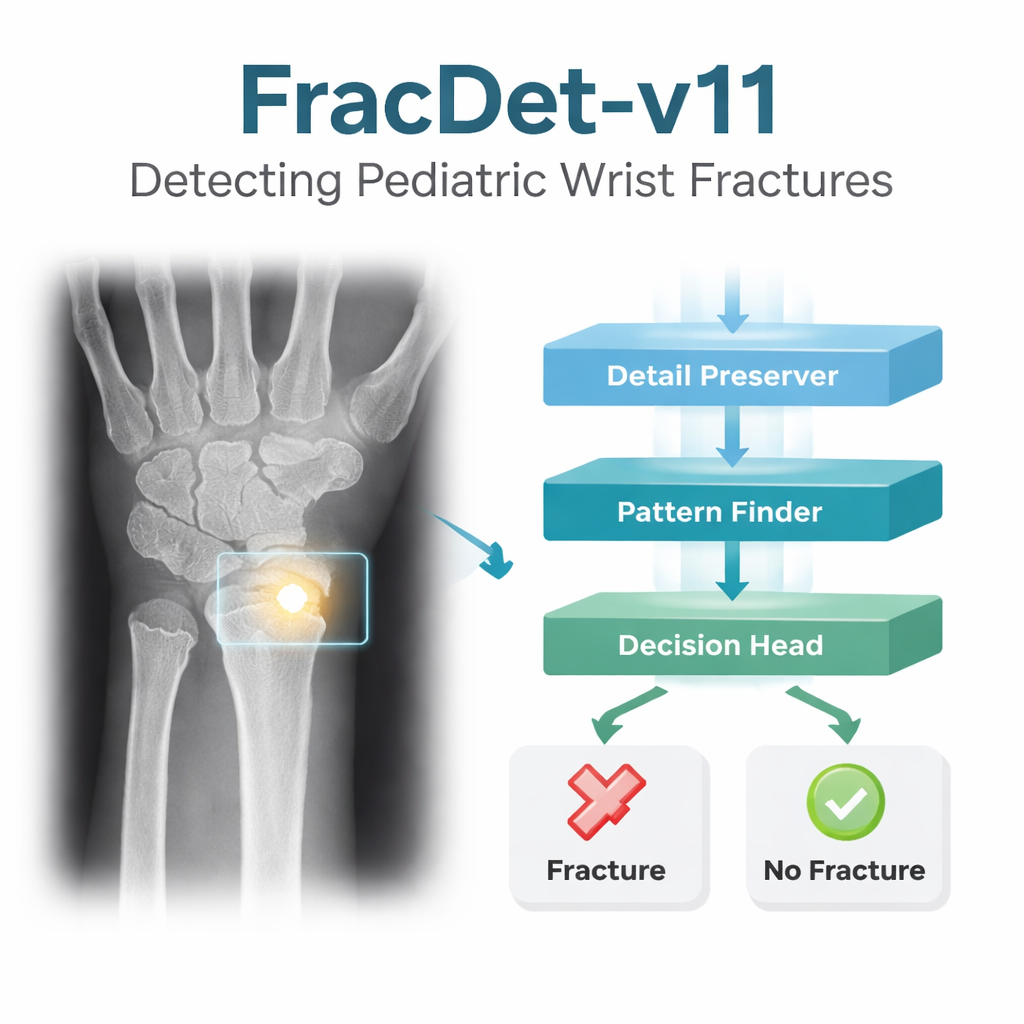
How FracDet‑v11 sees more than a standard algorithm
FracDet‑v11 builds on a popular real‑time object‑detection family known as YOLO, but reshapes it for medical use. First, the authors redesign the early layers that shrink and summarize images, replacing simple blurring and pooling steps with a wavelet‑based method that keeps delicate edges and textures—exactly the kind that outline fine fracture lines. They add modules that look at patterns at multiple sizes at once and emphasize informative regions while downplaying background clutter, such as overlapping soft tissue. A redesigned middle “neck” of the network fuses information from different resolution levels using lighter, more efficient convolution blocks, so the model can still run quickly. Finally, at the decision stage, the team swaps in a more flexible type of convolution that can bend its sampling grid to follow irregular crack paths, and a new loss function that pushes the model to focus especially on hard, low‑contrast examples instead of easy, obvious ones. 
How well does it actually perform?
On the pediatric GRAZPEDWRI‑DX test set, FracDet‑v11 spotted abnormalities with a precision of about 74% and correctly covered them with bounding boxes 65% of the time under a common scoring rule (mAP50). This clearly beat the standard YOLOv11s baseline model and other popular detectors, while using fewer parameters and less computation—important for real‑time use on hospital hardware. In carefully controlled ablation tests, the authors showed that each design choice—wavelet‑based downsampling, attention modules, streamlined feature fusion, deformable convolutions, and the new loss—added a measurable boost. When the model was applied, without redesign, to the more varied FracAtlas collection (which includes adults as well), it still outperformed all comparison methods, suggesting that it can generalize beyond the children’s training data.
What this means for patients and clinicians
The authors emphasize that FracDet‑v11 is not meant to replace radiologists but to act as a second pair of eyes. In a busy emergency room, an automated system that rapidly highlights suspicious regions on a wrist X‑ray could help junior doctors avoid oversights, speed up triage, and ensure that children with subtle but clinically important fractures receive timely treatment. The work also underlines current limitations: the system still works only with 2D images, can be confused by normal growth plates, and inherits any uncertainty in the original expert labels. Even so, FracDet‑v11 demonstrates that carefully tailored AI can both sharpen the visibility of tiny injuries and remain fast enough for real‑world use, pointing toward a future in which fracture detection becomes more consistent and less dependent on the luck of who reads the X‑ray first.
Citation: Qiu, H., Liu, L., Hong, J. et al. FracDet-v11: a multi-scale attention and wavelet-enhanced network for real-time pediatric wrist fracture detection. Sci Rep 16, 5888 (2026). https://doi.org/10.1038/s41598-026-35827-5
Keywords: pediatric wrist fractures, X-ray imaging, deep learning detection, emergency radiology, computer-aided diagnosis