Clear Sky Science · en
Cellular bioenergetic and migratory responses of human gingival fibroblasts to 940 nm diode laser photobiomodulation
Light to Help Mouth Wounds Heal
Anyone who has had a tooth pulled or gum surgery knows how uncomfortable healing in the mouth can be. The tissues are constantly stressed by chewing, talking, and bacteria, so anything that could safely speed repair is of great interest to dentists and patients alike. This study explored whether a common dental laser, used at very low power, can gently "coach" gum cells to work harder and move faster as they rebuild injured tissue, without burning or harming them.
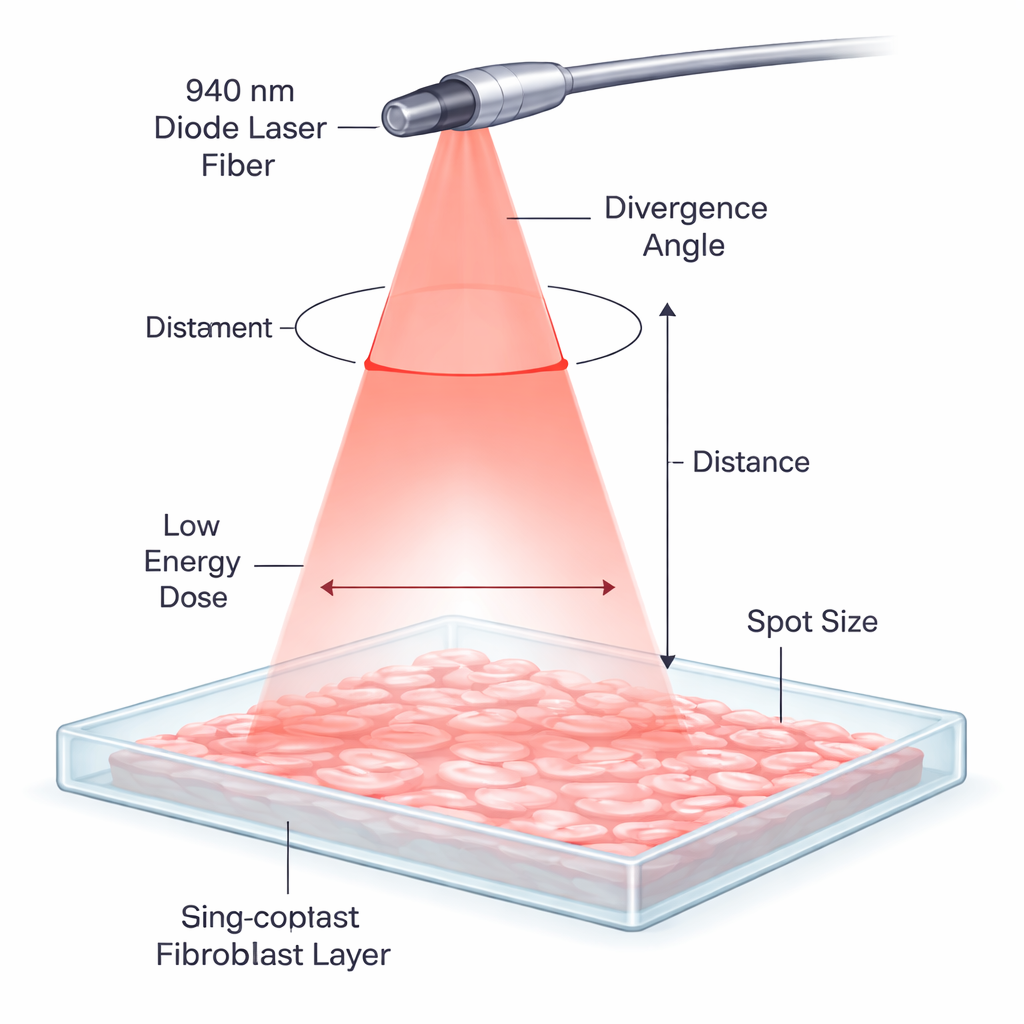
How a Gentle Laser Differs from a Cutting Laser
In many dental offices, diode lasers are routinely used to cut or reshape soft tissue by generating heat. Here, the same type of 940 nanometer laser was dialed down and used in a very different way. Instead of touching and burning tissue, the light was delivered for just one second from a short distance, spreading out into a soft cone over a thin sheet of human gum cells grown in a dish. At these low doses, the aim is not to cut but to nudge the cells’ internal machinery, a process known as photobiomodulation, so that they repair and reorganize themselves more efficiently.
Testing Gum Cells’ Energy and Safety
The researchers focused on fibroblasts, the main workhorse cells that produce the fibers and matrix giving gum tissue its strength. Commercially sourced human gingival fibroblasts were grown as uniform layers and exposed to three different energy doses of the 940 nm laser, while a fourth group received no light at all. The team then measured several markers: how metabolically active the cells were, whether their outer membranes were damaged, how much cellular fuel (ATP) they produced, and whether they released nitric oxide, a molecule linked to inflammation. Across all laser doses, the cells showed no signs of leakage or injury and did not trigger an inflammatory signal, indicating that the brief light exposure was gentle and biologically compatible under the tested conditions.
More Cellular “Fuel” and a Sweet Spot for Motion
Although the cells remained healthy in every group, their energy output changed in a dose- and time-dependent way. At moderate light levels, fibroblasts ramped up production of ATP, the universal energy currency of cells, by as much as about one quarter over untreated cells after 24 hours. Their overall metabolic activity also rose modestly, especially at the highest dose. To see whether this extra energy translated into better repair behavior, the scientists created a straight “scratch” in the cell layer and used digital holographic imaging to watch how quickly cells crawled in to close the gap. They found that a lower laser dose slightly increased migration speed and led to the fastest closure, while the highest dose actually slowed movement and delayed closure, even though energy levels were still elevated. This pattern, where a little stimulation helps but too much starts to hinder, is known as a biphasic response.
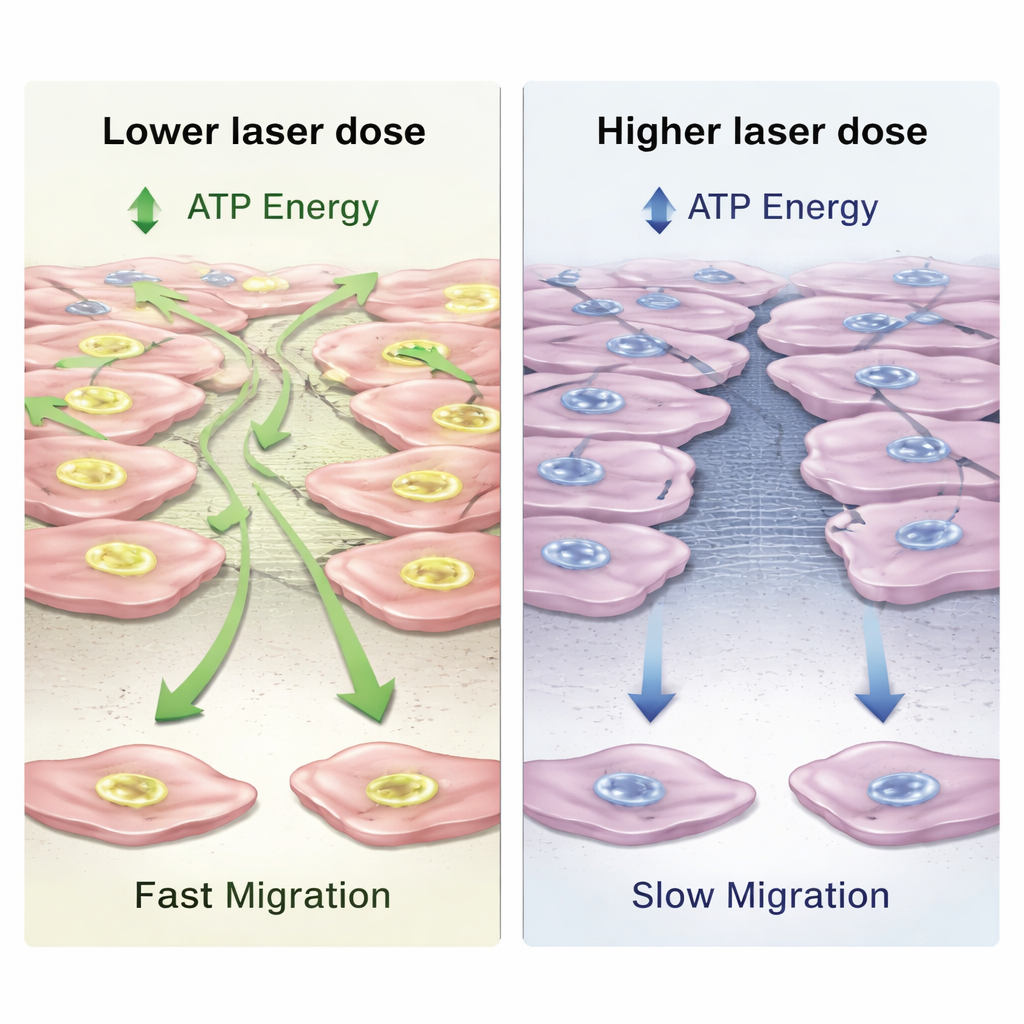
What This Could Mean for Dental Healing
Because these experiments were done in a simplified dish model, they cannot fully capture the complexity of a healing wound in a living mouth, where blood flow, immune cells, and bacteria all play major roles. Still, the results map out a promising window of light doses in which a 940 nm dental laser can boost gum cell energy and guide their movement without causing harm or inflammation. The work also shows that fine-tuning the dose matters: the conditions that maximized cellular fuel were not exactly the same as those that produced the quickest closure of the artificial wound.
Takeaway for Patients and Clinicians
For non-specialists, the key message is that low-level laser light, carefully controlled, may one day help gums heal faster and more predictably after procedures such as grafts, implants, or extractions. In this study, very brief, non-contact exposure to a 940 nm diode laser encouraged cultured gum cells to stay healthy, make more energy, and—in the right dose range—crawl more quickly to seal a wound-like gap. These settings are not yet ready to be applied directly in the clinic, but they provide a scientific foundation for future animal and human studies aimed at turning an everyday dental laser into a precise tool for enhancing natural tissue repair rather than simply cutting.
Citation: Mizrahi, I.K., Neculau, C., Balasea, B.V. et al. Cellular bioenergetic and migratory responses of human gingival fibroblasts to 940 nm diode laser photobiomodulation. Sci Rep 16, 5972 (2026). https://doi.org/10.1038/s41598-026-35824-8
Keywords: gum wound healing, low-level laser therapy, oral surgery recovery, photobiomodulation, gingival fibroblasts