Clear Sky Science · en
Near-source wastewater surveillance as a non-invasive tool for disease detection in prisons
Why Sewage Can Reveal Hidden Health Risks
During the COVID-19 pandemic, prisons turned into hotspots for infection, yet testing everyone inside was difficult, costly, and often mistrusted. This study explores a surprisingly simple idea: by testing the wastewater flowing out of prisons, we can track outbreaks without swabbing every person. The researchers show how sewage can act like a collective health check, revealing when a virus is spreading behind bars and how closely prison outbreaks are tied to infections in the surrounding community.
Prisons as Invisible Epicenters
People in prison face far higher risks of illness than the general public, not only from COVID-19 but from many infectious diseases. Overcrowding, poor ventilation, limited healthcare, and high rates of underlying health problems create ideal conditions for viruses to spread. At the same time, prisons are not sealed off from the outside world: staff go home every day, prisoners attend court or hospital appointments, and some are regularly released or transferred. These constant movements mean that a virus can move both into and out of prisons, yet traditional testing often misses the full extent of the problem because it depends on individuals coming forward, agreeing to tests, and having access to healthcare.
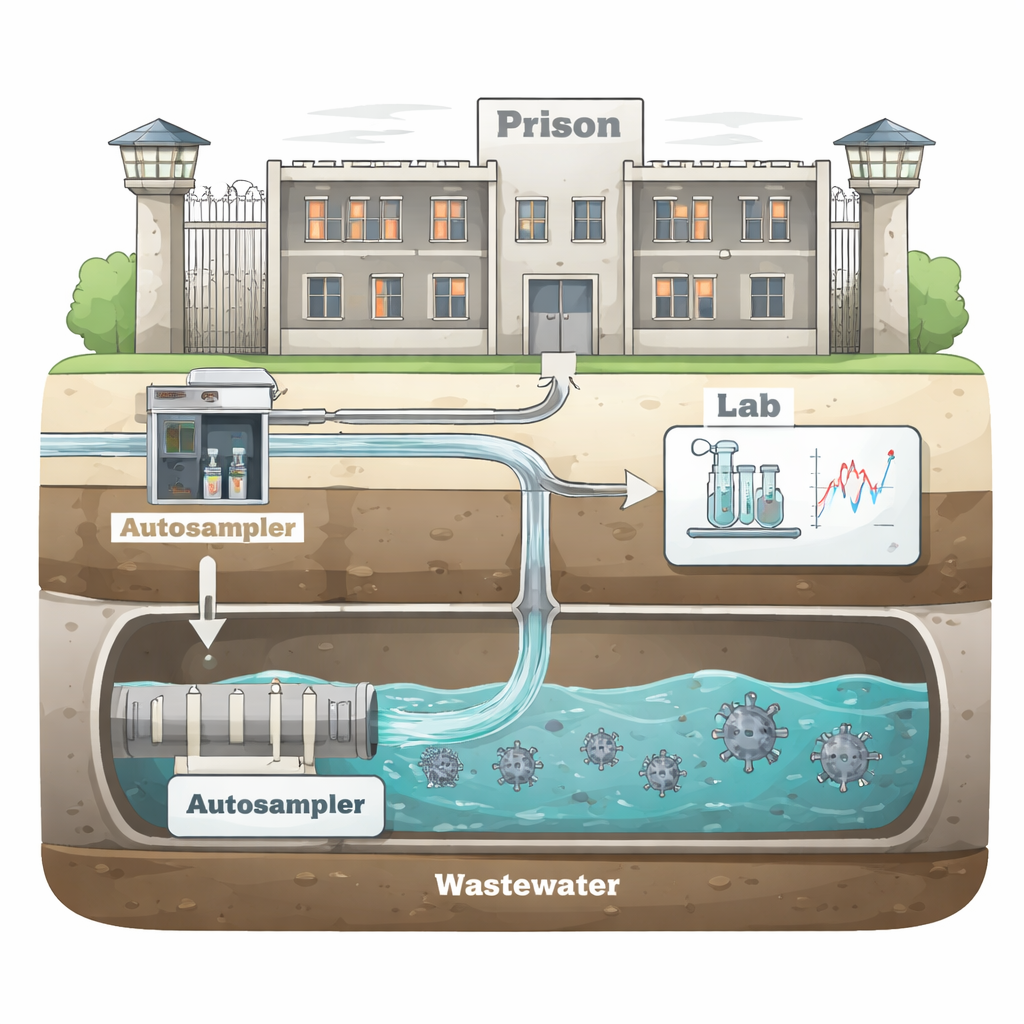
Listening to the Sewage
Wastewater-based epidemiology takes advantage of the fact that people infected with a virus shed tiny fragments of its genetic material in their urine and feces. By collecting sewage from a single pipe that serves a whole facility, scientists can estimate how much virus is present in the entire population. In this study, the team collected 680 wastewater samples from 14 prisons in England and Wales over six months in 2021. Using sensitive laboratory tests, they measured levels of SARS‑CoV‑2, the virus that causes COVID‑19, and compared these data with official case counts from each prison and from nearby towns and cities.
Spotting Outbreaks Earlier and More Fairly
The sewage signals closely matched known COVID‑19 outbreaks inside the prisons. Almost half of all samples contained viral RNA, and weeks with higher concentrations in wastewater tended to align with weeks of higher case numbers among prisoners and staff. In some facilities, spikes in the sewer even prompted targeted mass testing, which uncovered many more infections than routine symptom-led testing had found—suggesting that regular clinical testing had missed a large share of cases. When the researchers adjusted the official counts to account for this under-detection, the link between wastewater levels and case numbers became even stronger. This shows that sewage monitoring can provide a more complete, less biased picture of infection, capturing people who are untested, asymptomatic, or reluctant to be swabbed.
Tracing the Flow Between Prisons and Communities
Beyond detecting outbreaks inside prison walls, the study also examined how prison sewage trends lined up with virus levels in nearby municipal wastewater systems. At some sites, the prison signal rose before the community’s, suggesting that outbreaks behind bars might serve as an early warning for the surrounding area. At others, community infections appeared to seed outbreaks in the prison, with the sewage signal inside lagging behind. These lead–lag patterns differed by prison type: some high-security and training prisons tended to follow community trends, while certain local and women’s prisons often led them. The researchers also found that each prison’s wastewater had its own chemical fingerprint, reflecting unique routines, populations, and plumbing, reinforcing the idea that every institution works as a distinct surveillance unit.
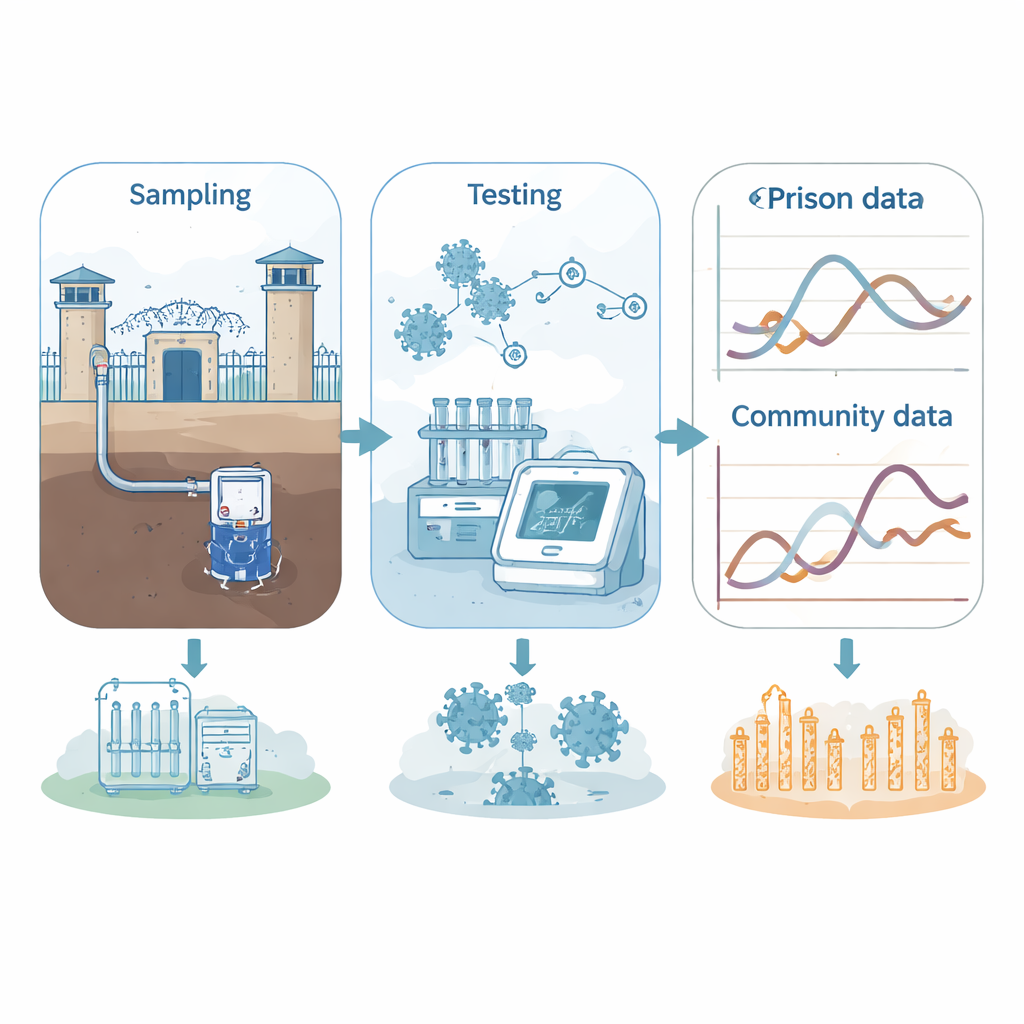
What This Means for Protecting People’s Health
For people living and working in prisons—and for the communities connected to them—this work shows that regularly testing wastewater can be a powerful, non-invasive tool for guarding public health. It can alert authorities to rising infections earlier than clinical testing alone, help track new virus variants, and guide where scarce testing and isolation resources should be focused. Because it does not depend on individual consent or access to care, it can also help reduce health inequalities in places where people are often overlooked. The authors argue that near-source wastewater monitoring should become a routine part of health security in prisons and other crowded, high-risk settings such as barracks, dormitories, and care homes, turning what we flush away into a vital source of early warning.
Citation: O’Mara, O., Hassard, F., Jobling, K. et al. Near-source wastewater surveillance as a non-invasive tool for disease detection in prisons. Sci Rep 16, 6815 (2026). https://doi.org/10.1038/s41598-026-35801-1
Keywords: wastewater surveillance, prison health, COVID-19, disease outbreaks, public health monitoring