Clear Sky Science · en
The ansa cervicalis and superior cervical ganglion contribute to the fiber composition of the human hypoglossal nerve and its branches
Why a tongue nerve matters to everyday life
The nerve that moves your tongue does far more than help you stick it out at the doctor. Called the hypoglossal nerve, it is crucial for speaking, chewing, swallowing, and keeping your airway open while you sleep. Doctors are already using electrical stimulation of this nerve to treat obstructive sleep apnea, a common disorder in which the tongue collapses backward and blocks breathing. Yet, despite this clinical importance, scientists have long assumed that the hypoglossal nerve carries only movement signals. This study reveals that, in humans, it is actually a mixed cable carrying not just motor commands, but also sensory and autonomic (sympathetic) information.
Rethinking a “pure motor” tongue nerve
Textbooks traditionally describe the hypoglossal nerve as a simple output line from the brain to the tongue muscles. Animal experiments, however, hinted at a richer picture: signals could be recorded in the nerve when the tongue was touched or stretched, and cutting the nerve damaged tiny stretch receptors in tongue muscles. That suggested sensory fibers, carrying information back to the brain, run within the same nerve. Other studies found unmyelinated fibers with chemical markers typical of sympathetic nerves, which belong to the body’s automatic control system and regulate functions such as blood flow. Until now, no one had mapped where these different fibers enter the human hypoglossal nerve and where they are likely headed.
Tracing fibers along the nerve’s full journey
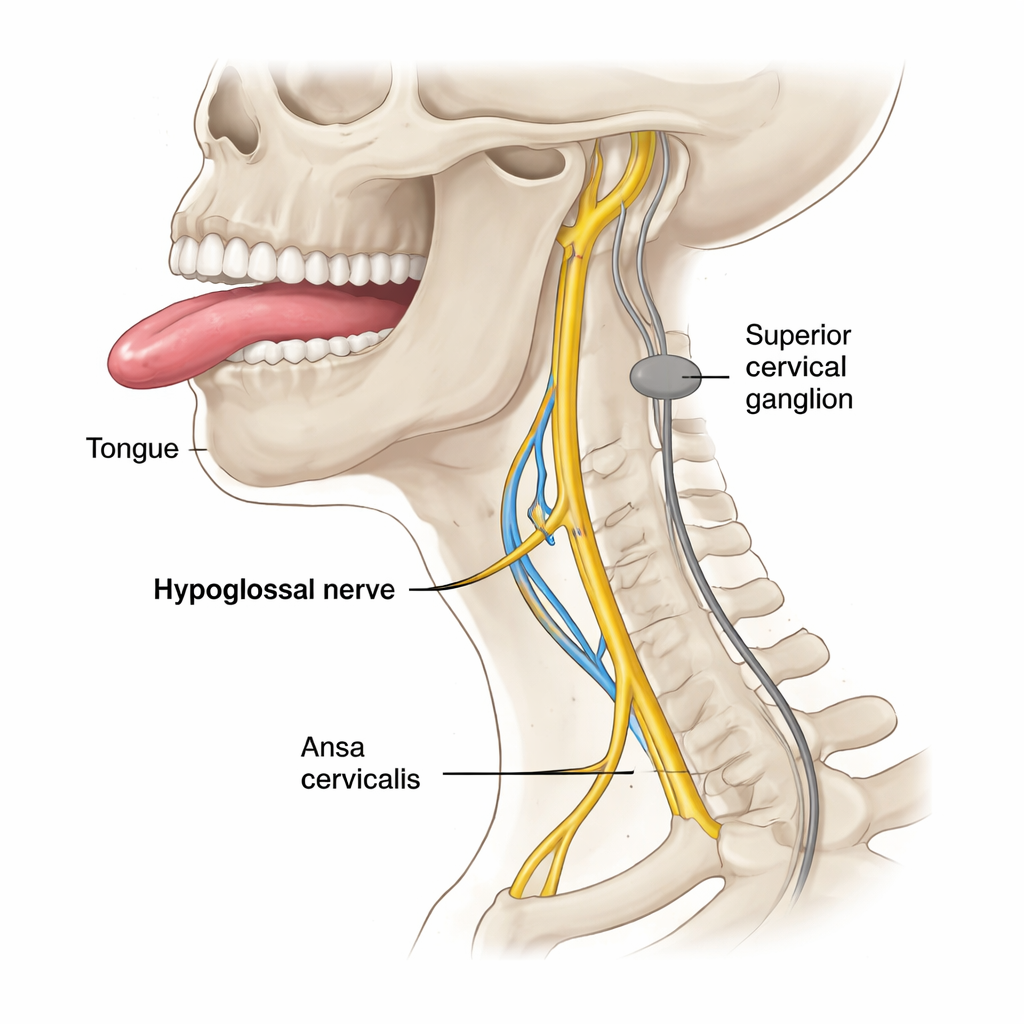
The researchers examined both hypoglossal nerves from six human donors, carefully dissecting the nerve from its roots in the brainstem all the way to where it branches inside the tongue. They focused on five key positions, from inside the skull to just before the nerve enters tongue tissue. Using multicolor immunofluorescence microscopy—essentially tagging different nerve fiber types with glowing markers—they could tell motor fibers apart from sensory fibers and from sympathetic fibers. They then counted thousands of individual fibers at each position to see how the mix changed along the nerve’s course, paying special attention to a looping neck nerve called the ansa cervicalis and a nearby structure of the autonomic system, the superior cervical ganglion.
How different fiber types join and travel
Inside the skull, all hypoglossal fibers were motor, confirming the classic view at the nerve’s origin. But just after the nerve left the skull, small numbers of sensory and sympathetic fibers appeared. Their numbers rose dramatically where the hypoglossal nerve temporarily runs together with the C1 branch of the ansa cervicalis, and then even more just after this branch leaves again. At that point, only about two-thirds of the fibers were motor; the rest were sensory or sympathetic. The pattern suggests that these non-motor fibers “hop on” to the hypoglossal nerve via the ansa cervicalis, likely carrying signals from and to the superior cervical ganglion and spinal sensory ganglia. Most of these fibers appear to travel outward toward the tongue, while a smaller share runs back toward the skull, probably joining a meningeal branch that supplies the brain’s coverings.
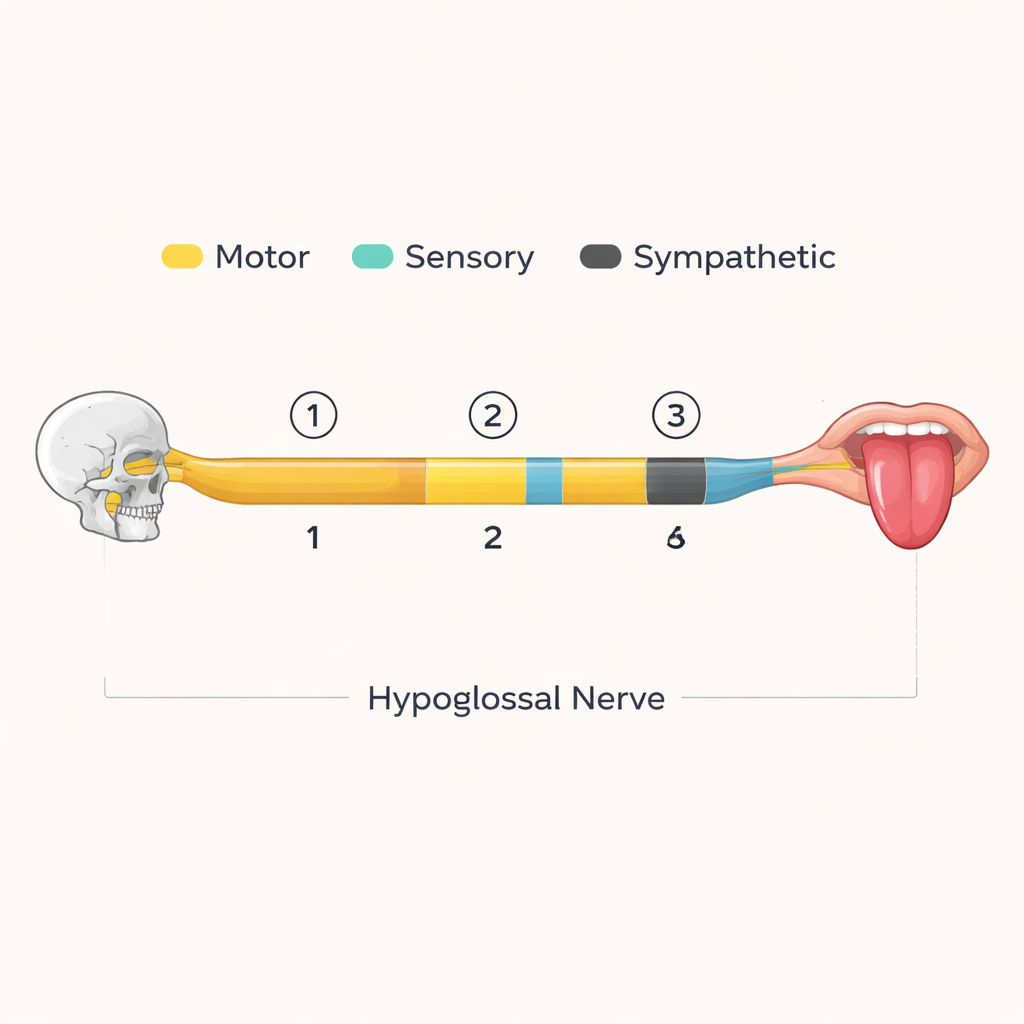
What this means for the tongue and beyond
The presence of sensory fibers within the human hypoglossal nerve implies that the brain receives detailed feedback about tongue position and stretch through the same pathway that drives muscle contraction. Large sensory fibers may connect to known muscle spindles in the tongue, while smaller ones may serve other stretch or pressure receptors. The dense sympathetic component suggests an additional, previously underappreciated route by which the autonomic nervous system can influence the tongue—possibly fine-tuning blood flow or other functions alongside the usual vessel-bound pathways. Together, these findings portray the tongue not just as a set of muscles, but as a richly monitored and automatically regulated organ.
Implications for sleep apnea and nerve injury
Because hypoglossal nerve stimulators are typically implanted on the neck portion of the nerve, they almost certainly act on this mixed bundle of motor, sensory, and sympathetic fibers. That raises the possibility—still theoretical—that such devices could influence sensation or automatic control in the tongue, not just movement. Likewise, injuries to the nerve outside the skull may disrupt more than speech and swallowing; they could also alter tongue feeling and its autonomic regulation. For patients and clinicians, the key message is that the hypoglossal nerve is a complex, multi-channel conduit. Understanding its full fiber composition and pathways should help refine treatments for sleep apnea and other conditions affecting the tongue and upper airway.
Citation: Didava, G., Petersen, A., Carrero-Rojas, G. et al. The ansa cervicalis and superior cervical ganglion contribute to the fiber composition of the human hypoglossal nerve and its branches. Sci Rep 16, 5889 (2026). https://doi.org/10.1038/s41598-026-35792-z
Keywords: hypoglossal nerve, tongue innervation, sleep apnea, sensory nerves, autonomic nervous system