Clear Sky Science · en
A survey of physicians perceptions of disability outcomes after hypothetical traumatic brain injury
Why this matters for patients and families
When someone suffers a serious head injury, families are suddenly asked to make life-and-death decisions without knowing what the future will really look like. This study explores how doctors themselves judge different levels of disability after traumatic brain injury—whether they see certain outcomes as a life worth living or as worse than death. Understanding these beliefs matters, because doctors’ expectations can strongly shape what treatments are offered, continued, or stopped.
Different paths after a serious head injury
Traumatic brain injury (TBI) affects more than 50 million people worldwide each year and can leave survivors with anything from subtle memory problems to profound physical and mental disability. To describe these outcomes, researchers often use the Glasgow Outcome Scale-Extended (GOSE), which ranges from death to a return to normal life. In this study, the authors focused on seven possible states one year after a hypothetical TBI, from being in a vegetative state to enjoying a good recovery with few or no problems. They wanted to know how doctors value each of these states in terms of quality of life.
Asking doctors to make a difficult choice
The researchers surveyed 646 board-certified physicians in fields such as neurology, neurosurgery, intensive care, and rehabilitation at major trauma centers across the United States. Of these, 528 completed all of the questions and were included in the analysis. Using a method called the “standard gamble,” each doctor repeatedly chose between two options: living in a specific GOSE state for the rest of one’s life, or taking a risky treatment with a chance of perfect health but also a chance of immediate death. By adjusting the odds until the doctor was unsure which option to pick, the researchers could turn that judgment into a number between –1 and 1, where 1 means perfect health, 0 means death, and negative numbers mean “worse than death.”
How physicians rated life with disability
Doctors generally gave lower quality-of-life scores to more severe disability. Strikingly, they rated two of the worst states—vegetative state (GOSE 2) and lower severe disability (GOSE 3)—as worse than death, with negative scores. They also did not see every step along the scale as equally different. The sharpest drop came between lower moderate disability (GOSE 5), where a person cannot fully return to work or social life, and upper severe disability (GOSE 4), where a person needs regular help from others. That steep fall suggests doctors place particular weight on how dependent a person is on caregivers, even if the person is awake and interacting.
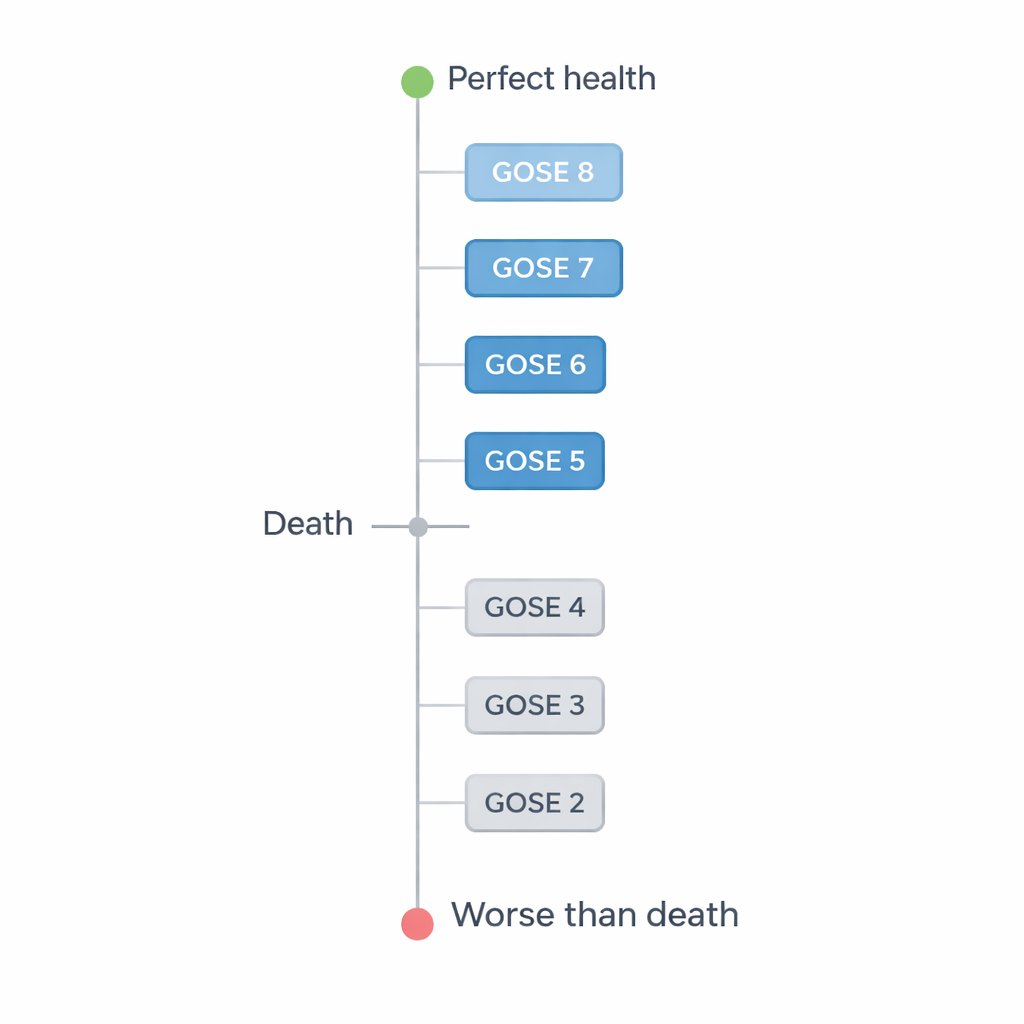
Doctors versus patients and families
To understand how unique these views are, the authors compared their results to earlier studies of healthy volunteers, people living with serious TBI, and their caregivers. Those earlier groups also saw deep disability as very challenging, but patients and families tended to rate severe disability states more positively than doctors did. They often saw less difference between several levels of disability, perhaps because they had adapted to new limitations over time. Healthy volunteers, by contrast, looked more like the physicians, often judging the most disabled states as worse than death. The new findings suggest that doctors may share this more pessimistic outlook and may underestimate how acceptable some outcomes feel to people actually living with them.
What this means for real-world decisions
In the hospital, choices about continuing or stopping life-sustaining treatment after TBI are often made under intense pressure. Because families rely heavily on physicians’ guidance, the doctors’ private beliefs about disability can shift the balance toward or away from aggressive care. This study shows that doctors, on average, value life with moderate or severe disability less than many patients and caregivers do. The authors argue that recognizing these biases is essential for truly shared decision-making. By talking more openly about values, listening carefully to what patients and families consider a life worth living, and using better prediction tools, clinicians can move closer to care plans that match each patient’s own goals and sense of dignity.
Citation: Weppner, J., Yim, I. & Martinez, M. A survey of physicians perceptions of disability outcomes after hypothetical traumatic brain injury. Sci Rep 16, 4978 (2026). https://doi.org/10.1038/s41598-026-35727-8
Keywords: traumatic brain injury, disability, physician decision-making, quality of life, prognosis