Clear Sky Science · en
Immune regulation and lymphangiogenesis by lymphatic endothelial cells in the decidua in severe preeclampsia
Why this matters for mothers and babies
Preeclampsia is a dangerous pregnancy complication that raises blood pressure and can threaten the lives of both mother and baby. Doctors have long known that faulty blood vessels in the placenta play a role, but this study looks at a more hidden player: the tiny lymphatic vessels and their lining cells in the womb. These vessels help move immune cells and keep the mother's immune system from overreacting to the baby. Understanding how they go wrong in severe preeclampsia could open new paths to safer pregnancies and better treatments.
A hidden drainage system in the womb
During pregnancy, the baby’s placenta attaches to the mother’s uterus in a tissue layer called the decidua. Here, blood vessels bring oxygen and nutrients, but lymphatic vessels form a second, quieter network. They act as a drainage and trafficking system for immune cells, carrying them to places where they can be educated to tolerate the fetus rather than attack it. The team first confirmed that these lymphatic vessels exist only on the mother’s side of the interface, in the decidua, and not in the fetal membranes. They isolated and grew the lining cells of these vessels, called decidual lymphatic endothelial cells, from women with severe preeclampsia and from women with healthy pregnancies, carefully proving that the cells were of maternal origin.
When vessel builders lose their tools
Next, the researchers examined the genetic activity of these cells. They found sweeping changes in cells from preeclamptic pregnancies: thousands of genes were more active or less active than in cells from normal pregnancies. Many of the most strongly reduced genes are normally needed to build and maintain lymphatic vessels and to guide immune cells into and through them. In laboratory tests, the preeclampsia cells were sluggish builders. Compared with normal cells, they migrated more slowly, stuck less firmly to their surroundings, formed fewer tube-like structures, and produced shorter sprouts in three-dimensional growth assays. Together, these defects suggest that in severe preeclampsia the maternal lymphatic network near the placenta is not only reduced in number but also functionally weakened.
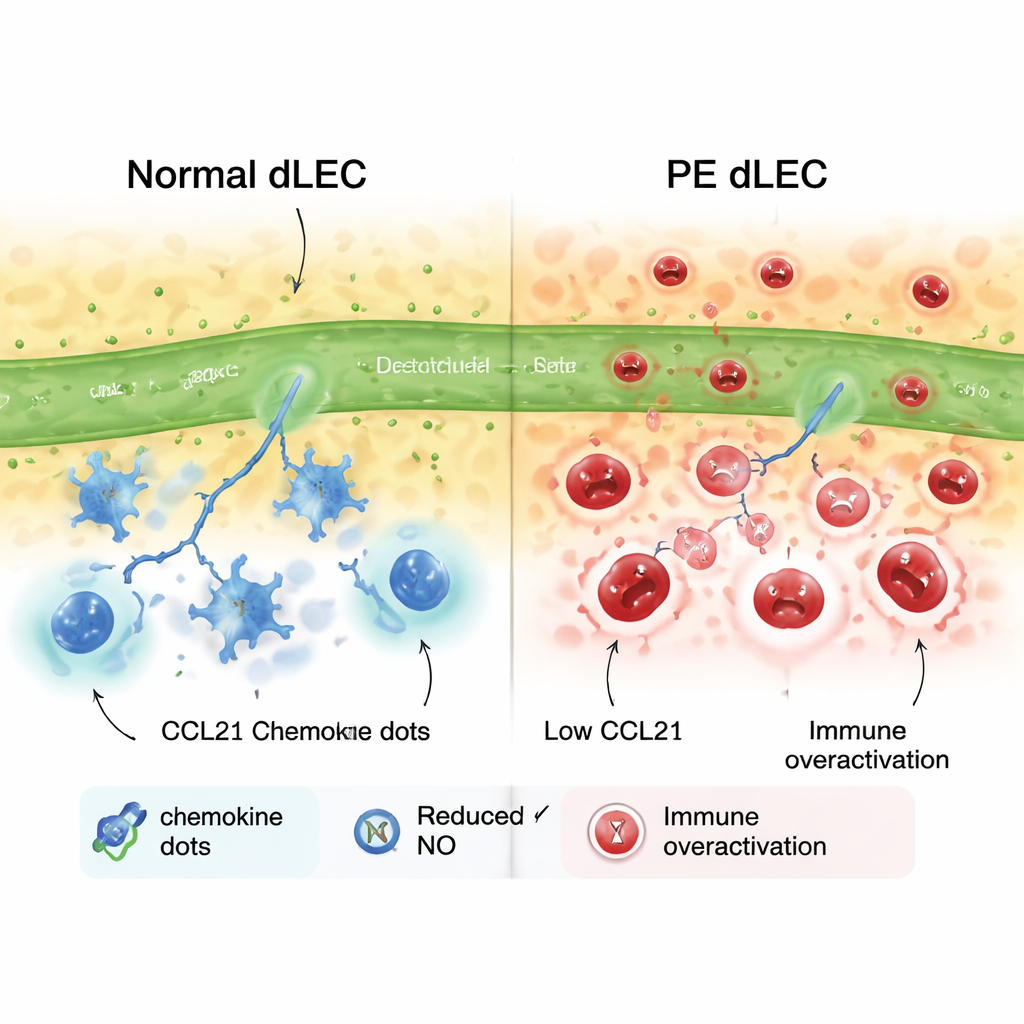
Immune traffic jams at the maternal–fetal border
The lymphatic lining cells also act as traffic controllers for the immune system. They make chemical signals that attract dendritic cells, a type of immune cell that carries messages to lymph nodes and helps educate T cells to tolerate the fetus. One such signal, called CCL21, was markedly lower in cells from preeclamptic pregnancies. In migration experiments, dendritic cells moved, stuck, and passed through the preeclampsia-derived cells much less efficiently than through normal cells. When the researchers added back CCL21, dendritic cell movements recovered. This points to a scenario in which faulty lymphatic cells create an immune “traffic jam,” reducing proper antigen presentation and disturbing the delicate balance between protective and harmful immune responses in pregnancy.
Loss of a natural brake on aggressive immune cells
Beyond guiding cell traffic, healthy lymphatic cells produce nitric oxide, a small molecule that helps control vessel function and also acts as a brake on aggressive T cells. The study showed that although the main nitric oxide–producing enzymes themselves were present at similar levels in both groups, key helper proteins that activate this pathway were reduced in preeclampsia cells. As a result, signaling through the nitric oxide pathway was weaker, and overall nitric oxide production dropped. With less of this calming signal, cytotoxic T cells in the decidua are more likely to become overactive, adding fuel to the inflammation and vascular stress already linked to preeclampsia.
A new angle on a complex disorder
Taken together, the findings paint a picture of severe preeclampsia as not only a disease of blood vessels and blood pressure, but also a disease of the maternal lymphatic system at the site where mother and baby meet. The lymphatic lining cells in the decidua lose their ability to form healthy vessels, to guide dendritic cells, and to produce enough nitric oxide to restrain harmful T-cell responses. This combination may tip the local environment toward inflammation and poor placental function. While more work is needed before new therapies can be safely developed, targeting these lymphatic and immune pathways could one day help prevent or treat preeclampsia without endangering the fetus.
Citation: Kim, S., Lee, Y., Kwon, JY. et al. Immune regulation and lymphangiogenesis by lymphatic endothelial cells in the decidua in severe preeclampsia. Sci Rep 16, 5181 (2026). https://doi.org/10.1038/s41598-026-35667-3
Keywords: preeclampsia, placenta, lymphatic vessels, immune tolerance, pregnancy complications