Clear Sky Science · en
Pravastatin combined with fibrin sealant-embedded BMSCs enhances recovery in steroid-induced avascular necrosis of the femoral head
Why Hip Bone Death Matters
When people take high doses of steroid medicines for long periods, a hidden side effect can quietly destroy the ball of the hip joint, a condition called avascular necrosis of the femoral head. As the blood supply fails, bone cells die, the joint collapses, and many patients eventually need a hip replacement in midlife. This study in rabbits explores a way to protect and rebuild the damaged bone using a combination of a common cholesterol‑lowering drug and living stem cells delivered in a biological glue. 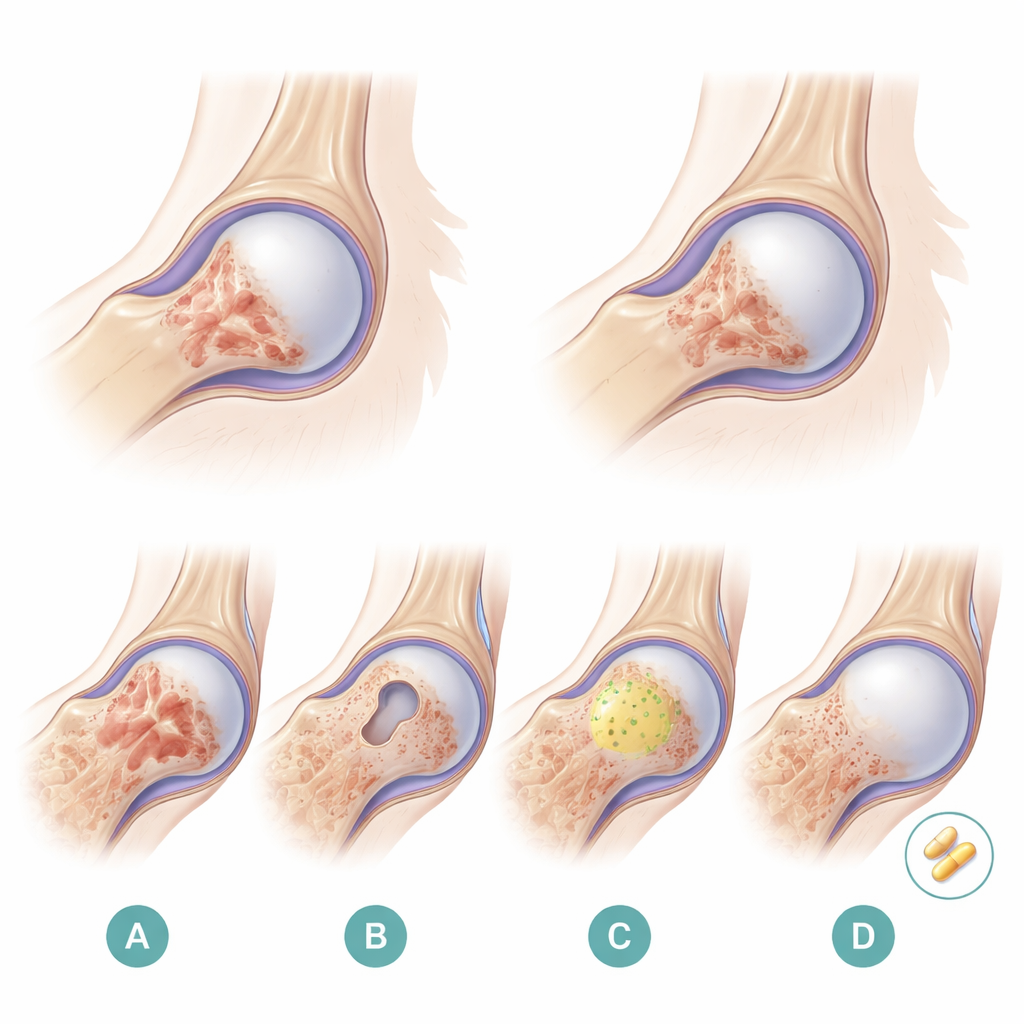
The Problem with Steroids and Hip Bones
Steroid drugs are powerful tools against inflammation and immune disease, but they also disrupt fat handling in the body. In the femoral head—the rounded “ball” at the top of the thigh bone—excess fat can clog tiny blood vessels, raise pressure inside the bone, and starve bone cells of oxygen. Over time, this leads to areas of dead bone that weaken the structure and can make the hip collapse. At early stages, surgeons sometimes drill a channel into the bone (core decompression) to relieve pressure and improve blood flow, but by itself this procedure often does not rebuild strong, healthy bone.
A Three‑Part Repair Strategy
The researchers tested four options in 48 rabbits with early steroid‑induced hip damage. One group was left alone as a control. A second group received only core decompression. A third group got decompression plus bone marrow mesenchymal stem cells, which are versatile cells from the marrow that can turn into bone and blood‑vessel‑forming cells. These stem cells were mixed into fibrin sealant, a surgical “biological glue” that forms a soft, three‑dimensional scaffold inside the drilled channel. The fourth group received the same stem‑cell‑in‑glue treatment plus daily doses of pravastatin, a statin drug widely used to lower cholesterol. The team followed blood fat levels and examined the hips using MRI scans, visual inspection, microscope slides, and staining for VEGF, a signal that encourages new blood vessels to grow.
What the Experiments Revealed
Over 12 weeks, blood tests showed that rabbits given pravastatin had steadily falling cholesterol and triglyceride levels, while levels rose in all other groups. Imaging and tissue analysis told a similar story inside the bone. In the untreated rabbits, MRI scans became more chaotic and eventually showed collapse of the femoral head. Under the microscope these animals had many swollen fat cells, thin and broken bone struts, and numerous empty spaces where bone cells had died. Core decompression alone gave only modest improvement. Adding stem cells in fibrin sealant reduced the extent of dead bone and modestly increased new bone formation. The best results, however, were seen in the group that received both pravastatin and the stem‑cell‑in‑glue transplant. Their MRI scans showed fewer abnormal signal bands and no collapse; their femoral heads kept a near‑normal shape. Microscope slides revealed fewer fat cells, thicker and more numerous bone trabeculae, and far fewer empty bone spaces. VEGF staining was also strongest in this group, indicating a richer network of new blood vessels feeding the healing bone. 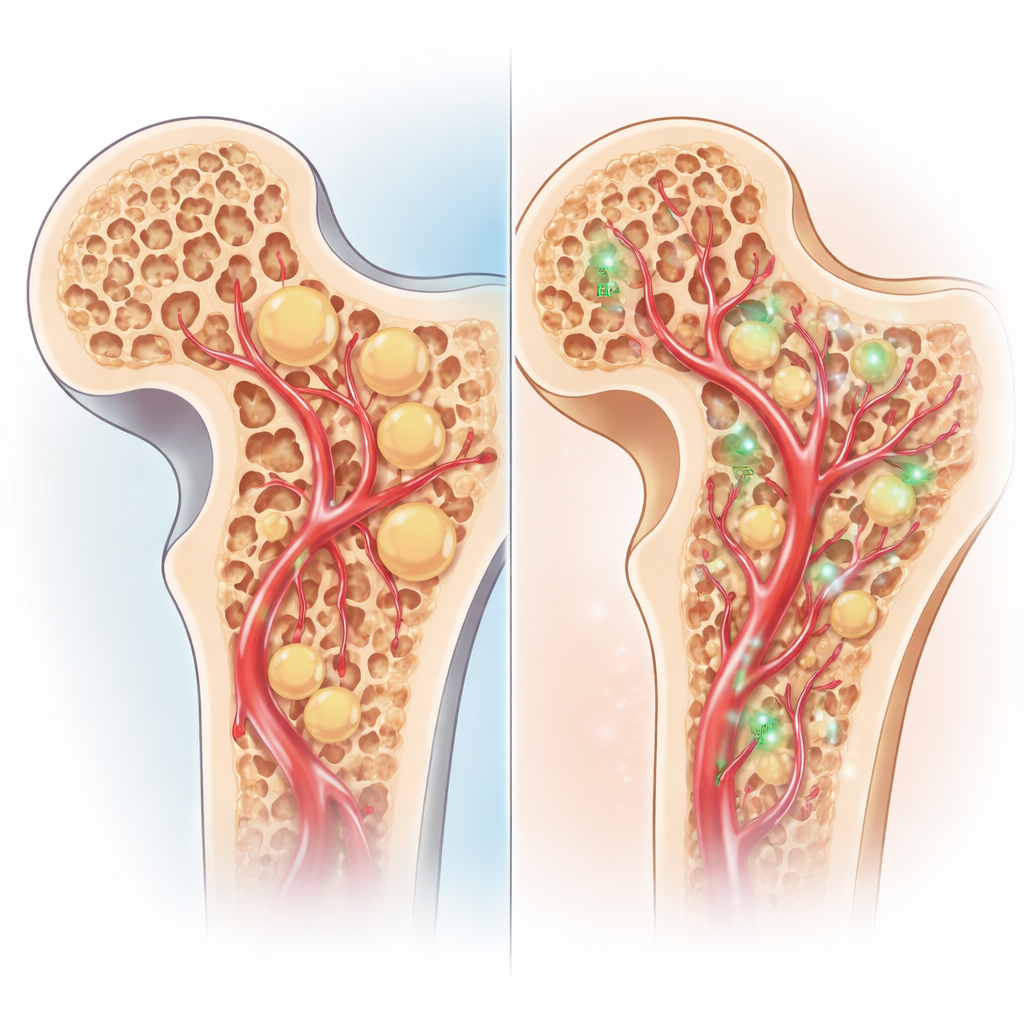
How the Combination May Work
This three‑part treatment appears to help from the inside out. Pravastatin tackles the root metabolic problem by lowering blood fats, which may reduce fat clots and pressure in the bone’s tiny vessels. At the same time, core decompression opens a path for better circulation and space for new tissue. Into this space, the fibrin sealant holds stem cells in place like a sponge, preventing them from washing away and giving them a structure to grow on. These cells can turn into bone‑forming cells and also release factors such as VEGF that call in new blood vessels. Together, these effects replace fatty, dying bone with stronger, better‑supplied tissue, at least in this animal model.
What It Could Mean for Patients
For people who must use steroids and face the risk of hip bone death, the study suggests that combining a familiar cholesterol drug with stem cells and a simple surgical glue could one day delay or even prevent the need for hip replacement—if started early enough. The work was done in rabbits and followed for only three months, so clinical trials and longer‑term studies are still needed. But the results offer a hopeful glimpse of a future in which doctors not only relieve pressure in the bone, but also correct blood fat problems and actively rebuild the joint using living repair cells.
Citation: Yang, Q., Yang, Y., Li, B. et al. Pravastatin combined with fibrin sealant-embedded BMSCs enhances recovery in steroid-induced avascular necrosis of the femoral head. Sci Rep 16, 5074 (2026). https://doi.org/10.1038/s41598-026-35663-7
Keywords: hip osteonecrosis, steroid side effects, stem cell therapy, pravastatin, bone regeneration